After a hemorrhagic stroke caused by a ruptured AVM at age 33, Blair Ames turned to blogging to discuss his stroke recovery experiences.
Highlights:
01:00 Introduction
04:43 Stroke at the age of 33
08:54 The stroke symptoms
14:38 When the gravity of the situation hits you
18:45 The Emotional Rollercoaster of Stroke Recovery
24:43 Dealing with new emotional states
27:42 Setting a stroke recovery deadline
31:59 The importance of sleep in stroke recovery
44:06 Managing time for stroke recovery
49:35 Avoiding alcohol after a stroke
1:02:14 The current status of the AVM
1:09:02 The possibility of another AVM bleed
1:17:49 Blair’s advice to stroke survivors
Transcript:
Blair Ames 0:00
I mean, for me, the emotional aspect of recovery has certainly been the biggest challenge. The physical aspects for me, I felt like it kind of came naturally. I’ve always enjoyed physical activity, working out. So I was never worried about being able to kind of rebuild myself. But for me, stroke recovery has kind of been everything I never would have expected it to be, in terms of the emotional and psychological aspect of it. That it’s been a significant challenge for sure.
Intro 0:47
This is the recovery after stroke podcast. With Bill Gasiamis, helping you navigate recovery after stroke.
Introduction

Bill Gasiamis 1:00
Hello, and welcome to episode 249 of the recovery after stroke podcast. My guest today is Blair Ames, a guest who was really grateful to be able to join me on the podcast, because Blair experienced a bleed on the brain at age 33, due to an arteriovenous malformation.
Bill Gasiamis 1:21
And he discovered the podcast early on. And he reached out a number of times to speak with me to be on the show. But we were never able to make it happen, because he was never able to fill up to the conversation and to be on a zoom call.
Bill Gasiamis 1:40
But now he is. And that is an amazing thing. I am so grateful that somebody who has been on this journey for a couple of years is now good enough, well enough, comfortable enough to finally get back in touch and say, Hey, are we going to do this?
Bill Gasiamis 1:57
Let’s do this podcast interview. So I’m grateful. And this is what stroke recovery is it is tough, and it’s difficult. But with time things do improve, and things get better. So that’s enough from me, and I hope you enjoy this interview. Blair Ames, welcome to the podcast.
Blair Ames 2:23
Thanks for having me.
Bill Gasiamis 2:24
It took a while. But we got here. We were trying to get this organized for quite some time. Stroke recovery goes like that it takes a while to get over the line sometimes.
Blair Ames 2:38
Yeah, Bill, your podcast when I first returned home from the hospital and rehab center, your podcast was one of the first resources I found to really learn more about stroke recovery. And I remember reaching out to you multiple times just exchanging emails, exchanging notes. And it’s kind of surreal to be talking to you now. But it’s a pleasure. I’m looking forward to it.
Bill Gasiamis 3:01
It’s a pleasure here mate. I’m glad when I come across a stroke survivor who’s got a struggle and not realizing at the beginning that you’re in the beginning of this whole saga. And what that needs to do is probably get you over the line with you know, rest recuperation, working out this new version of yourself, you know, there’s so many things to consider.
Bill Gasiamis 3:27
And reaching out is a quick thing. Like it’s clearly okay, you know what, this guy knows what’s happening, let me reach out to him and then I’ll get some solutions to some problems, who knows what, but then sometimes that’s not the first thing you need to be doing.
Bill Gasiamis 3:42
The first thing you need to be doing is taking care of yourself and finding a way to deal with everything and get better and be healthier. And it happens a lot. A lot of stroke survivors will reach out to me and then I’ll hear from them a year later. And they’ll be telling me how far along they are compared to when they first reached out.
Bill Gasiamis 4:02
And that’s the real exciting part. It’s that I get to see people actually get to overcome a lot of the challenges. And even in the state that they arrived at 12 months later, they’re still talking to me about how much better it is and how much more energetic they are and how now they’re able to actually be available to be on the podcast and they’re gonna make it through a whole episode rather than fall asleep or something. And that’s so heartwarming and that’s just brilliant. So I’m just as excited that you’re here as you are. So tell me a little bit about what happened to you.
Stroke at the age of 33
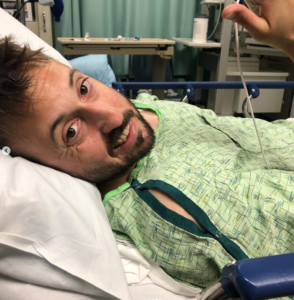
Blair Ames 4:43
Of course. So I am now as of today just past the 23 month mark. I at age 33 I was in the middle of the gym, working out. started to feel a little funky, I ended up going outside thinking I just needed a breath of fresh air to relax. And over the course of, you know, 10 to 20 minutes after I left the gym, I was standing by my car and I collapsed.
Blair Ames 5:16
Thankfully, there was a number of people nearby who were able to come over, help get me comfortable, call 911. And I was rushed to a hospital. And that’s where I learned what a stroke was, what an AVM was, where my AVM was all those details. So I was certainly one of those people before stroke. I had no idea what a stroke was. I had no idea what an AVM was.
Bill Gasiamis 5:48
So I looked at your scan, because you’ve got it on your blog website, what is it strokerecoveryrehab.com. That’s it. Yep. And that image looks very similar to my image. So I had an AVM that bled, it was near the cerebellum, nice and deep they called it.
Bill Gasiamis 6:14
And you wouldn’t believe it. So a friend of mine who helped me get through that time in 2012, was a radiographer who put me in touch with some awesome neurosurgeons and all those things, used to give me some feedback on the scans, and all that kind of stuff a little bit more detailed feedback than what you would get from your doctor, you know, because he was the one actually doing the scans.
Bill Gasiamis 6:41
His daughter, who’s 17, literally a month ago, had an AVM that bled. And it looks almost identical to the image that you’ve got there, and my image, this is becoming a little bit annoyingly common. And it’s supposed to be rare. Right? So before you went to the gym, did you notice anything in the weeks months leading up to it that perhaps something was about to? Well, in hindsight that something was brewing?
Blair Ames 7:23
No, absolutely nothing at all. It was, a very normal Saturday morning for me. When I started feeling funky in the gym. Like many other people, I just chalked it or like many other people would I just chalked it up to you know, we had a late night the night before, maybe had a few too many, was very hot out. I had no idea that there was anything bubbling under the surface.
Bill Gasiamis 7:51
It sounds like you read straight out of the rulebook, how to reflect back on why you’re having a stroke it’s like, I had too much to drink or I was at the football and I was screaming too much or so many excuses that are not relevant. But we chalk it up to anything that our mind tells us might be appropriate, just so that we can somehow get through.
Bill Gasiamis 8:21
I must add as we continue that my friend’s daughter went from ICU to back on her feet within a month. So it’s extremely a good outcome. So for anyone who was going to be concerned about that, thank you for your concern. And I just wanted to get that out of the way now.
Blair Ames 8:40
That’s great to hear.
Bill Gasiamis 8:41
Yeah, it’s really good. So you’re in the gym. And now what happens? How do you get help? How do you move through that phase?
The stroke symptoms
Blair Ames 8:54
Yeah, of course, I was about halfway through a workout. And one of the first things I started to notice was my vision was a little blurry. So I thought perhaps I had put my contacts in the wrong eyes. That’s what I use. You were just saying, you know, we kind of chalk it up to two other events.
Blair Ames 9:14
But then as I went to pick up a dumbbell, my left hand, my fingers wouldn’t grasp the dumbbell. I couldn’t, you know, I couldn’t grip the dumbbell. So at that point, I was like, you know, I need to go outside, take a break. And I kind of stumbled on my way out, I kind of tripped over my my gym bag.
Blair Ames 9:39
But I did did make it outside to my car. And while I was in my car, I was texting my girlfriend at the time who’s now my fiancee. I was texting her and just letting her know that I was feeling a little off and I was like, Hey, you might need to come get me I might need some water.
Blair Ames 10:03
And over the course of maybe just five or 10 minutes sitting in the driver’s seat, I really started to feel just very discombobulated, I struggled, even just leaning the seat back to lay down and relax. And so I texted her and I was like, my mood shifted from, you might need to come get me to, I would like you to come here now please, like pretty soon because I feel pretty funky.
Blair Ames 10:31
And then as I mentioned, once I had got out of the driver’s seat to just lay down in the backseat. And as I opened up that rear door, that’s when I just collapsed to the ground. And that’s when there were some nearby people who were able to rush over and, you know, thankfully keep me comfortable and call an ambulance.
Bill Gasiamis 10:54
So left side deficits, you collapsed, because you couldn’t feel one side of the body or were you dizzy? What happened that made you collapse?
Blair Ames 11:05
To be honest, I don’t it just, it all happened so fast. You know, I opened up the rear door, I just wanted to lay down in the back seat thinking I could just you know, relax all these weird feelings away. And I assume my left side kind of, I guess just gave out at that point, maybe
Bill Gasiamis 11:25
Relax all those weird feelings away?
Blair Ames 11:29
I was going to try.
Bill Gasiamis 11:30
I love it. I was in my car the third time it bled. And I thought I’d walk around the outside of the car. And that will make my symptoms go away. But alas, it did not work. It worked for a moment. And then when I got back into the car, I realized this is pretty bad. So she was with you by now. And then how did you guys respond to your collapsing? What happened then?
Blair Ames 11:57
Oh, yeah, it was actually great timing on her part. She got there as the ambulance got there. And you know, I was very lucky to have her by my side this whole time. She was she was there as because we had we had originally gone to a local regional hospital.
Blair Ames 12:16
And I needed to be airlifted to Johns Hopkins in Baltimore, which is about three hours away from where we are on the eastern shore. And no, she was she was great. She was there with me the entire time. And I think for her and my family as they traveled down from Philadelphia to be at the hospital in Baltimore. You know, I think it was honestly probably a little bit harder on them than it was for me because I was so naive to what was going on.
Blair Ames 12:54
I was in the ambulance. I was just worried that, you know, this is gonna be really expensive. And this is really annoying. Am I going to have to come back to the gym tomorrow to finish this workout? Or am I going to do a different workout? So for me, I was very just kind of annoyed by what was happening to me. I was never really worried about what was happening to me. And I guess I think it’s just because I was so naive to the seriousness of it.
Bill Gasiamis 13:29
Yeah. So your parents coming down? How far are they traveling?
Blair Ames 13:34
Philadelphia to Baltimore about two and a half, three hours depending on traffic.
Bill Gasiamis 13:38
Yeah. Okay. So it’s a reasonably quick trip. But nonetheless, it’s a hike. They’ve got to get there. They just know there’s something wrong. They don’t know what’s wrong. They’re probably at their wit’s end. It’d be a hard drive. For sure. Your girlfriend at the time is how is she coping with all of this? She’s being the middle person between you and your parents? How’s she doing?
Blair Ames 14:03
You know, she was great for me just to have her there with me the entire time. So I’m not alone in those hospital rooms as I’m waiting for the helicopter crew to get there. But I know it was it was certainly hard on her. She had an interesting story that she told me after the fact but there was one point where I had been wheeled back for my initial CT scan.
When the gravity of the situation hits you
Blair Ames 14:38
And the nurse was coming by and she had asked the nurse, you know, is the is he going to be okay? And she told me that the nurse didn’t give her an answer. The nurse just handed her a box of tissues. And that was it. So when I heard that story, after probably many months later, that really kind of just triggered how serious you know, this situation was. And like I said at the time, I was completely oblivious.
Bill Gasiamis 15:13
Yeah. You know, that seriousness when it finally hits home. How does it impact your emotions and your mental health? Because I’ve had a lot of people that I’ve spoken to clients, and also, podcast guests who have told me that there was a realization that there was kind of like a line in the sand moment when they realized that they could have not been around.
Bill Gasiamis 15:43
And sometimes you hear about people who almost had a car crash and make it sound like they had a car crash. And it’s like, they go nuts, and they lose it at the other driver. And my whole theory on that is, when that happens to me in the car, the whole theory is, well, we didn’t collide, right? So everything that you are talking about didn’t happen.
Bill Gasiamis 16:08
So we had the best outcome, and nothing went wrong, because we didn’t collide. But then the other person is treating it as if they collided, right? So stroke survivors have this thing where some people imagine themselves having died, and that they’re not around anymore. And the gravity of that is really a lot to bear.
Bill Gasiamis 16:35
What kind of guy are you? Are you the guy that goes up? I got away with it. Like I say, like, I tend to sort of say, well dodged the bullet. And then other people go, Oh, my gosh, I don’t know what that means that I’m I’m here, but I should not be or may not be, may not have been or may not be in the future. It’s the first time they really get a sense of mortality. What happened? How did you cope with that?
Blair Ames 17:04
Yeah, you know, I would say, certainly, I’m not the kind of person I’m not the kind of individual who had a stroke. And it’s like, you know that old version of me died that day. That’s a little too dark for me to say something like that. I think it’s maybe more important to think about how you’re just evolving, you’re not so much, you know, lamenting how that old version of you is gone, you’re just evolving into a different person. But overall.
Intro 17:42
If you’ve had a stroke, and you’re in recovery, you’ll know what a scary and confusing time it can be, you’re likely to have a lot of questions going through your mind. Like, how long will it take to recover? Will I actually recover? What things should I avoid in case I make matters worse.
Intro 17:59
Doctors will explain things that obviously, you’ve never had a stroke before, you probably don’t know what questions to ask. If this is you, you may be missing out on doing things that could help speed up your recovery. If you’re finding yourself in that situation, stop worrying, and head to recoveryafterstroke.com where you can download a guide that will help you.
Intro 18:22
It’s called seven questions to ask your doctor about your stroke. These seven questions are the ones Bill wished he’d asked when he was recovering from a stroke, they’ll not only help you better understand your condition, they’ll help you take a more active role in your recovery, head to the website now, recoveryafterstroke.com and download the guide. It’s free.
The Emotional Rollercoaster of Stroke Recovery

Blair Ames 18:42
I mean, for me, the emotional aspect of recovery has certainly been the biggest challenge. The physical aspects for me, I felt like it kind of came naturally. I’ve always enjoyed physical activity working out. So I was never worried about being able to to kind of rebuild myself. But for me, Stroke recovery has kind of been everything I never would have expected it to be in terms of the emotional and psychological aspect of it. It’s been a significant challenge for sure.
Bill Gasiamis 19:29
Okay. I find this as well. So people come along and they say, you know, I need some help with my recovery. I want to get beyond my stroke deficits and all that type of thing. And they see the obvious physical deficits as the thing that steps in the way of their recovery.
Bill Gasiamis 19:50
And then it’s a real difficult conversation to have with somebody to sort of suggest that the deficit that you’re dealing with, I’ve got nothing to do with your stroke recovery, they’ve just got to do with one aspect of your physical of the way you physically move around the world.
Bill Gasiamis 20:10
How you respond to that emotionally, and how you respond to that mentally, is what exactly what you said is where the challenge is. And if you’re somebody whose life before stroke, was, “I avoid problems, and I don’t tackle my challenges, and I live in fear, and I’m emotionally unintelligent, so I have low emotional intelligence”, then what that’s going to do is that’s just gonna rear its ugly head when it comes to overcoming a dramatic life event.
Bill Gasiamis 20:41
And what you’re often dealing with is you’re not dealing with the stroke recovery, you have to unpack and undo and resolve all the past life events that are stacked up. And then once you kind of get through those, you can learn about how to go through potentially walking with a deficit, or not being able to use one of your arms or a more dramatic deficit than that. So does that resonate with you? Is that how your experience about the past came into play now into this after stroke version of you?
Blair Ames 21:26
I feel like for me, I was, you know, I was somebody that before stroke, I was very lucky. I certainly, wouldn’t say I faced a ton of adversity in life, until stroke, you know, outside of, you know, any standard education, work problems that are now just pale in comparison to having a stroke.
Blair Ames 21:47
So, for me, I think as soon as I had a stroke, I had recognized that, you know, I had been very lucky up into this point, in terms of having no other significant health problems. So I think I wanted to embrace, you know, the challenge of stroke recovery.
Blair Ames 22:08
And even with that, you know, there certainly have been points over the past two years, where that’s, it’s a difficult burden to carry. Especially when, you physically look fine, everything’s good. People think you’re, “better”. And you’re kind of, you know, every minute of every day is still affected by stroke, in a sense, and how you go about things. So no, carrying that burden of stroke and stroke recovery, especially as you get back into work life, you know, get back into all of your personal commitments. It’s, certainly a challenge to balance all those things, of course.
Bill Gasiamis 23:00
yeah. So this just occurred to me that perhaps for me, because I have a similar approach to the way or have a similar kind of way that I’ve got the stroke in that the things that I thought were problems weren’t really problems, I made them big problems. And then I had the stroke, and then I was very easily able to assess or what was a serious problem before the stroke, which really wasn’t.
Bill Gasiamis 23:29
And now what really is something that I’ve got to take seriously, and I’ve got to step up to. Before I used to complain about problems and not really do anything about them, because I could complain about them and get it off my chest for a little bit of then feel okay, and then just move on with the rest of my day.
Bill Gasiamis 23:46
What just occurred to me was, that perhaps for me, what it was, was new, emotional states I had never experienced before and new mental states I’d never experienced before. And that inability to know how to react or respond to that made it very difficult because that meant I had to stay in those new emotional states negative mostly, and then negative mental health space for a bit longer than I was comfortable with.
Bill Gasiamis 24:20
And then it’s like, Okay, remember the ones where you used to be able to just push them aside and pretend that they weren’t there. This is not going to allow you to do that. You’ve got to tackle this. And you’ve got to resolve it. And I don’t know how long that journey is going to take. Because I don’t know how long the stroke incident is going to continue for.
Dealing with new emotional states
Bill Gasiamis 24:43
And for me, it continued for nearly three years before I had surgery to remove the AVM and then I had to deal with not being able to walk again and all the stuff that the surgery caused, and then living with all the deficits that I live with every day, which is the left side numbness, the pins and needles, the proprioception issues, and the fact that everyone thinks I’m perfectly okay. Because I look okay. So, any of that sound familiar? Is that kind of where you’re at? Or are you somewhere else?
Blair Ames 25:20
Literally everything you just said sounds familiar. No, I agree with everything you just said. 100% when you were discussing the emotional states and how they’re new emotional states that you hadn’t dealt with before, I think for me, I’ve definitely noticed I’m more irritable than I was before.
Blair Ames 25:53
In the hospital, my mother, my sister, Mallory my fiance, they all told me to a tee that I was being mean, I was being rude. And at the time, I wasn’t doing anything like that intentionally. So that was something that I struggled with. And as I continued in recovery, up until now, about two years post, I still find myself getting easily frustrated over things.
Blair Ames 26:28
Whether it be a work assignment, or if just, you know, kind of, I’m not feeling too great a day, and we had some plans. And now I have to manage that. I do find myself getting easily frustrated to this day. And that’s something I’m working through for sure.
Bill Gasiamis 26:46
Are you comparing the old Blair and going oh, man, this used to be easy, why can I do this? How are you getting frustrated? Is it at yourself? The situation? How specifically?
Blair Ames 27:00
Oh, yeah, a good question. I don’t, I don’t think it’s because I compare myself to the way that I used to do things. I think I’m just annoyed by the current situation. And that it’s, you know, I’m two years after stroke, and I’m still, you know, still not back to where I feel I need to be. So it’s more of just an you know, it’s I’m tired of dealing with this day by day type frustration. So I most most days are okay, at this point. But there certainly are some moments where you know, those post stroke feelings kind of rear their ugly heads for sure. Yeah.
Setting a stroke recovery deadline
Bill Gasiamis 27:42
Yeah. So did you perhaps have a timeline or a deadline that you thought this was going to be all resolved by and you haven’t reached it? And that’s part of the thing that’s getting in your way, about how you feel about the whole thing?
Blair Ames 28:00
No, I certainly learned early on that setting, arbitrate deadlines in recovery is a bad idea. I think for me, as I progressed pretty quickly, in those initial weeks and months. Like by the end of that first year, I had assumed alright, we’ll be back to normal by four months by five months by six months.
Blair Ames 28:27
And then once you hit those, those checkpoints, and you realize how far you feel you still have to go? Yes, it’s hard. It’s devastating to deal with. So no, I’ve kind of given up on setting deadlines. I prefer to just set monthly goals of something I feel like I can accomplish over the next 30 days. That makes me feel like I’m still moving forward in stroke recovery. So no, I agree. setting deadlines is not an optimal way to go.
Bill Gasiamis 29:04
Yeah. So how far have you come tell me about what you were faced with? What the deficits were and then how far you’ve come? And, of course, those deficits are not just the physical ones that could be fatigue and other things.
Blair Ames 29:19
Yeah, of course, well, in the hospital, I was told I was completely paralyzed on the left side, ended up staying in the hospital for about a week and a half to two weeks, and then went to an inpatient rehab center about same timeline. A week and a half, two weeks.
Blair Ames 29:41
I left the inpatient rehab center, I was able to walk out on my own with the assistance of a walker. So the physical deficits I do regret in those early weeks. I never let anybody take any photos Those are videos of me because I was just incredibly embarrassed that, you know, I was using a walker, that when I, when they would get me out of bed, I would kind of collapse on to the physical therapist or the occupational therapist.
Blair Ames 30:16
And then some of the other machines that they put you on to help you learn to walk again, I was really embarrassed by that, you know, somebody in my early 30s. And here I am, you know, I can’t get out of bed on my own. In terms of other deficits, once I returned home, you know, certainly vision has been a bit of a struggle for me, extended computer time at work.
Blair Ames 30:47
I definitely, you know, try and take breaks get outside. But that’s still you know, a bit of a nuisance here and there. Obviously, just riding in cars and being dizzy was a real struggle at the beginning. And then I’ve really struggled with with sleeping after stroke, it took me the better part of a year to realize that there was a consistent problem here.
Blair Ames 31:16
But I woke up at about 1:30 in the morning, pretty consistently, and then struggled to get back to sleep after my stroke, so that the not sleeping was a big was a big problem, which obviously contributed to that post stroke fatigue feeling. But yeah, I don’t I’m not sure I had any unique post-stroke deficits. It was all kind of what I’ve heard other stroke survivors talk about.
Bill Gasiamis 31:48
You know, this sleep thing. So does that mean that you’re getting less than five or six hours sleep at night at the beginning?
The importance of sleep in stroke recovery
Blair Ames 31:59
It must have because, it was so frustrating, because I would have no problem falling asleep. And I’ve recognized early on how important sleep is going to be to recovery. So you know, I’m trying to fall asleep between 10 or 11. And I would have no problem falling asleep whatsoever.
Blair Ames 32:21
And in the middle of the night I wake up, be wide awake, we use the restroom, and then not be able to fall back asleep. And it’s like, let me look at my phone. And it’s 1:30 again. So for me, after that Some nights I would fall back asleep other nights, I would really struggle to fall back asleep. So in those early months I was I’d say I definitely getting less than five to six hours most nights.
Bill Gasiamis 32:50
Okay, here comes the diagnosis from our first meeting ever and my professional opinion as a stroke survivor. So what I learned about sleep because I suffered a little bit about sleep. And this is just food for thought for people to hear about. And maybe it is for them, maybe it’s not, and I’m not a doctor and don’t take any of my advice.
Bill Gasiamis 33:11
But what it could be it could be the adrenal situation, adrenal glands, it could be something to do with the pituitary gland, it could be to do with the thyroid. If you’re waking up in the middle of the night, at the same time, it’s potentially an excessive amount of the stress hormone cortisol occurring at that time and interrupting with your sleep cycle.
Bill Gasiamis 33:38
So cortisol is part of the sleep cycle. And it usually comes at sunrise, it usually decreases melatonin. And then as melatonin decreases, cortisol increases. And then what happens is, you start to get awake in bed, and then a couple of hours later, an hour and a half later, the cortisol drops off, and you just go into your regular day.
Bill Gasiamis 34:03
Now, additional cortisol spikes happen when you have a coffee. They also happen when you go for a drive to work and there’s traffic and somebody cut you off. And then when you get to work and your inbox is full, but cortisol, because of the adrenal glands happening in the middle of the night, is what causes people waking is part of what causes the people waking.
Bill Gasiamis 34:30
Now what we do is we get into our heads and then at that moment, when you get into your head and look at your phone, you’ve completed the circuit to stay awake. And what’s really necessary to do is to walk out of your bedroom and not look at the phone if you can, perhaps read a book or do something but outside of the bedroom so that your bedroom becomes a place of just sleep and not awake time.
Bill Gasiamis 34:57
So that you start to kind of habituate your already, so that as you walk into your bedroom, and as you’re in the bedroom, you’re only in the bedroom for sleep time, not tossing around time and not wondering why the hell am I awake again time and all that kind of stuff, right?
Bill Gasiamis 35:15
So just a few little bits and pieces of stuff that is coming back for me because I also experienced that. And even a couple of nights ago, I woke up at 2:30. And my regular routine when I wake up is I wake up because I’m thirsty. But then, of course, while I’m awake, and I’m thirsty, and I have a drink while most I go to the toilet, and then come back and then fall asleep.
Bill Gasiamis 35:42
And usually, that works. But this time, I wake up at 230. And I couldn’t go back to sleep. So I stayed out of my room for a while, then I went back into the room, and then I fell asleep at around five o’clock. And then I woke up at seven with the alarm. So it’s not uncommon for it to continue to occur from time to time, and I’ve kind of taken it as well, if it’s happening today. I’m just going to have to deal with it today.
Bill Gasiamis 36:14
And I’ll be better tomorrow. And I always tell myself, I’m going to this is a loss for me tonight, I’m going to give you the win. And tomorrow, I’m going to catch up. And usually that meant that last night I went to bed at around 9:30. And this morning, I woke up really well at around 6:30.
Bill Gasiamis 36:36
So you kind of give yourself the opportunity to catch up later rather than over, over, kind of think about it or get concerned about it or frustrated about it. But it does. I know I know that it’s hard because it means that that day, you’re going to be less than an optimum state.
Bill Gasiamis 36:55
And I definitely used to suffer that day. Quite a lot. So what do you do? What did you do to sort of start to get back into the routine? Did you notice that your sleep improved gradually on its own? Did you need some help with that? How did you get better at that?
Blair Ames 37:18
I’ve experimented with a ton of different just lifestyle adjustments supplements over the past two years. Because like I said, for me, it took me the better part of about a year and a half to actually realize something was wrong. Because for the most part like when you wake up in the middle of the night, like you said sometimes you’ll just get a drink of water go to the bathroom and then you can’t fall back asleep and that you know that that happens that’s normal.
Blair Ames 37:53
Sometimes it was you know an excuse of there was a loud noise outside there were neighbors were loud. excuse of you know, we stayed out too late. I was on my phone too late, I had trouble falling asleep. So I’m you know, I’m a real psycho and I write down what time I go to bed every night and what time I wake up. So I was looking for patterns to see what was going on here.
Blair Ames 38:21
And like you had alluded to, it’s very easy to put too much pressure on yourself to fall back asleep. And then that prevents you from falling back asleep. So I totally agree with your your proposal of you know, sometimes you’d have to get out of your bedroom for a little bit.
Blair Ames 38:40
So certainly for me when I do have a rough night of sleep I do try and go to our spare bedroom or just lay down on the couch for a little bit to try and sleep somewhere else. But some of the most effective practices that I’ve used over the past two years, one of my absolute favorites is drinking tart cherry juice. I found that to be Helpful.
Blair Ames 39:11
How is that helpful man? Please.
Blair Ames 39:16
Oh I enjoy the taste. So I enjoy drinking tart cherry juice a couple hours before bed.
Bill Gasiamis 39:25
You’ve said the word tart. And I had the experience of the tart thing that happens in the back of your mouth when you eat something tart. So that’s why I had to ask that question I’ve reacted immediately.
Blair Ames 39:38
I know not everybody enjoys the taste of cherry juice. I’ve enjoyed it. It was interesting tart cherry juice is a big one. Taking l’theanine was a big supplement for me. And then also trying to get outside as the sunsets. That’s another big one. And then the last one, which was a really basic, simple one is just taking a hot shower, you know about an hour and a half before bed. So I try as as often as I can to combine those four practices together. And for me, as of today, I’m sleeping better now than I did before my stroke. And those nights where I wake up at 1:30 are very few and far between.
Bill Gasiamis 40:39
That’s good. That little trick of seeing the sunset, that’s great, because that does start to bring on the melatonin and start to decrease your cortisol levels. So that’s really good. switching off lights, if you can, that are above your head helps and just put on really warm lamps in the corners of the rooms that you’re going to be spending some time in.


Bill Gasiamis 41:03
Also little bits of things that might help. A really good book that I’ve recommended to a lot of people is a book called The Sleep book, How to sleep well, every night by Dr. Guy Meadows. And he’s from an organization that he calls the sleep school.
Bill Gasiamis 41:19
And I’ve read a couple of books about sleep. And one of the best ones that I read about sleep, which was good to give you an insight in what sleep is and how sleep works. And all that kind of stuff was, of course now just escaped my mind as I started, Why We Sleep by Matthew Walker.
Bill Gasiamis 41:46
It’s a great book in that it gives you a great insight into what sleep is. Scientifically, it has been a little bit poo pooed by his peers, because they question his scientific method. But if you’re interested in sleep, ideas, and how sleep works, and all that kind of stuff, it’s still a really great book.
Bill Gasiamis 42:13
Because if you’re like me who’s not scientific, you don’t really mind how he tells the story, and why he tells the story. So I got so much out of that book, that was such a great book. But then, for tips and tricks that will support sleep, this book by Guy meadows, is a really good read.
Bill Gasiamis 42:37
It’s easy, it’s short, it’s not too overly scientific. But it is based in a scientific method, because what he because he’s the sleep guru or sleep guy, you know, or he has the sleep school. They have a lot of data. And they have a lot of evidence to show the things that are proven to work that support the sleep cycle. So anyone listening wants to just go and check out the sleep book by Dr. Guy Meadows. And then Matthew Walker’s book was a game changer for me.
Blair Ames 43:16
Thank you for that. I love a good book recommendation.
Bill Gasiamis 43:19
Yeah, you’re welcome. Just another version of Matthew Walker’s book. In a more succinct, more nuanced kind of approach towards sleep. It’s just very, to the point, you know, there’s not a lot of filler, you know, not that Matthew Walker’s book is like that.
Bill Gasiamis 43:41
I really, I gotta say, well, Matthew Walker’s book was the first one I read. That just changed my idea about what I was trying to do and how I was trying to go about sleep and why I was sleeping and all that stuff. You know. So guy Meadows is the is that this is what we know works for people kind of book.
Blair Ames 44:04
That’s great. I’ll put that one on my list. Thank you.
Managing time for stroke recovery

Bill Gasiamis 44:06
Yeah, check it out. So it’s only been two years in my estimate, on your overcoming your challenges. So which means that you’ve come a long way, and you’ve got a long way to go. Right? And I only say it’s only been nearly two years, because I just mentioned my challenges, and it’s been 11 years.
Bill Gasiamis 44:29
So it’s not like you haven’t come a long way already you have and if you’re the type of person who is curious as you are, and has put some time and effort into discovering what’s going to help you and support you and you continue doing that. By the time we get to 10 or 11 years, you’re going to have this nailed down and you’re going to have a routine that works for you.
Bill Gasiamis 45:00
You’re gonna have a clear in your mind and in the way that you go about life, and that’s going to make your life a lot easier. So last night, for example, it was a Friday night for us. And we usually do something on a Friday night, we go somewhere, you know, we go out, we catch up with some friends, whatever.
Bill Gasiamis 45:18
And for me, if I had done that, today would have been a really difficult day for me, it would have been tiresome, I wouldn’t been able to be productive. I certainly wouldn’t have enjoyed being on the podcast, even though for my guests, I always turn up and I try and do my best.
Bill Gasiamis 45:35
So I’m at that stage where all of those things that I’ve learned about how I need to act/behave, or prepare. They’re almost non negotiable. If I didn’t go to bed at 9:30, on a Friday, today wouldn’t have been a good day. So it’s not a sacrifice anymore.
Bill Gasiamis 45:59
It’s not like I’m missing out on anything that I used to feel like I was missing out on now what I’m doing is going, I need to be good on Saturday, because I don’t want to spend the whole day on the couch doing nothing and being unproductive.
Bill Gasiamis 46:13
So as you move into your recovery, and you start getting better at it, and by the way, you’re going to continue to recover, you’re going to continue to feel better, you’re going to continue to dial in all those little things that are challenging you.
Bill Gasiamis 46:29
What will happen is you’ll feel really good about where things are at regardless of whether or not you have a deficit and a bad day, one in every 10 days, it won’t really bother you. How do you feel about the future? Going forward? What is your Have you contemplated at all?
Blair Ames 46:52
Yeah, well, no, certainly, Bill, I appreciate your your kind words and encouragement. You know, I’ve certainly enjoyed your podcasts over the years for that just to to learn about how you’re going to progress over the years. I mean, I think I certainly recognize I’m still very early on in this process only being two years. I’m certainly hopeful that, you know, I’ll continue to get better and perhaps, you know, obviously have days where the stroke doesn’t affect me as much as it does today.
Blair Ames 47:29
I guess for me, I feel like I’m at that point in recovery, where Like, I’m back to doing everything that I need to do. And it’s really just a matter of, of managing everything kind of like you were discussing where you know, you have to go to bed around a decent hour on Friday, or else you know, Saturday, you won’t be very lively. When you said that I I agree with that wholeheartedly, and I saw myself in your habits, I feel the same way.
Bill Gasiamis 48:03
Yeah, that’s what I found. And that’s what I encourage people to think about is to think about how with time and studying and becoming more educated about what they need, they will be able to create a routine for them, that works really well.
Bill Gasiamis 48:20
And that means they’re going to enjoy a lot of their life. Rather than pushing through for the sake of old habits and old behaviors and old patterns for other people and then suffering through the rest of the next week. And the next weekend or whatever. And I just can’t do that, I don’t drink any more when I go out. And if I do I have one drink and then people who drink with who I used to drink with will say, you know, they’ll say well, just one, you know, that’s it.
Bill Gasiamis 48:57
You only gonna have one, can we have another one? Or can we keep drinking or whatever. And it’s like, I can’t do that. I’m not going to do that. And I know that you need to or you want to, but I’m not that way anymore. I can’t do what I used to do with you for you or whatever. How do you feel your relationships are changing and evolving as you navigate being out and about with people? Has that been different?
Avoiding alcohol after a stroke

Blair Ames 49:35
Yeah, man, this our conversation, I’ve really enjoyed it thus far, because so many of the things you’ve said, have rang so true to me. And as you were just discussing, you know, I don’t drink that much myself anymore. I’m like you if I go out I might have a drink here or there. But most nights I really just don’t.
Blair Ames 49:59
Don’t really You have the desire to have a drink anymore. And I’ve certainly gotten the comments over the past two years of, you know, why aren’t you any fun anymore? Why don’t you just have a couple of drinks? Why doesn’t Blair loosen up and have a couple of drinks?
Blair Ames 50:18
You know, when are we going to be able to do the things that we used to do type comments? And it’s certainly been tough at times. But for me in terms of having a drink of, you know, I could take it or leave it. And I think people are maybe starting to understand I don’t have a desire to drink a lot anymore. But certainly over the past two years, it’s been a bit of a learning curve for sure.
Bill Gasiamis 50:52
Yeah. It’s interesting with people who drink they need somebody to drink with. It’s so weird. I don’t get that. What if I’m just drinking sparkling water? Or a soda water next to you in a glass that appears like an alcohol class? Can I do that? Even that’s not enough? It’s kind of like, I need to be under the influence of alcohol so that you feel good about yourself being under the influence of alcohol? Like I’ve got to make it normal for you. I’ve got to normalize it. It’s really strange.
Blair Ames 51:30
No, I 100% I agree with you. And for me, I guess I’m glad I got my my drinking habits out of the way when I was in my 20s. I enjoyed it plenty, then, because I’m not really interested in all that anymore. But as I’ve transitioned to, to not drinking as much over these past two years, I’ve certainly realized what you have where it’s almost as if in terms of alcohol, it’s like, if you don’t drink, there’s something wrong with you.
Blair Ames 52:03
Whereas if you drink it’s, you know, is what you’re supposed to do. So that’s been an interesting realization for me is when you’re at an event, or you’re out and people see your you’re not having a drink, it’s do they assume something’s wrong with you.
Bill Gasiamis 52:21
And not that something wrong with you, which there actually is not like, they assume you have a medical issue, they assume you have a personality issue, isn’t it? Exactly, yes. That’s interesting. I’ve never thought about it like that before. But that’s exactly what they do. They make your personality, not the right kind, and not the right type, because you’re not drinking.
Bill Gasiamis 52:46
And the fact that you really actually have something wrong with you, is not relevant to their reasoning. And to their problem with you not drinking, they can’t come to terms with that. And maybe you’re also because you don’t look like you’ve had a stroke, so to speak, you’re also giving false signals as to, perhaps their eyes, so that they don’t grasp the concept of why he looks great, you know, and he talks about all this stuff, but I can’t see it. So you know, maybe he’s just become boring. Who knows?
Blair Ames 53:28
For sure, it’s, you know, if I go out here and there, I might feel the need to have a drink. But like I said, it’s just not really something that appeals to me anymore. Because I know it doesn’t really, it doesn’t help me feel any better. So I’ve, I’ve kind of lost interest in in that regard.
Bill Gasiamis 53:47
Yeah. And it says a lot about relationships that we’ve formed, that were formed, around drinking, and how shallow that relationship might be. And the depth of the relationships that we need to help get us through this time and to actually going to have decent, long term relationships with our family members or our friends.
Bill Gasiamis 54:16
It says a lot about perhaps also where they’re at in their life, and how their inflexible in flexibility is impacting the relationship in that they only relate to you as a person who is somebody who behaves a certain way who is more fun to be around or whatever it is. And that’s interesting that they’re in flexibility is turned into your your problem it’s made, you know, it’s kind of outsourced to you and that’s how I felt.
Bill Gasiamis 54:50
It’s like, I’m not telling you not to drink, man. I’m just telling you that I’m not drinking you know, leave me alone. I can’t do think and feel like I’m having another stroke again. I’m going to show if you understand what that means, I can’t do it. So you go for it. Or power to you, but just leave me out of it’s not a lot to ask. It’s such a simple thing to ask.
Blair Ames 55:16
No, exactly. It’s just like, you know, people still, if I ever hear a comment like that, normally I don’t pay much attention to it anymore. I’m very happy drinking my water, or whatever else it may be.
Bill Gasiamis 55:27
Yeah. So Mallory, your girlfriend at the time became your fiancee? How long after the stroke did she become the fiancee? And did you pop the question?
Blair Ames 55:42
Oh, yes, I see. I’m glad you asked that. So we had been dating. How many years we have been dating maybe three years, two and a half, three years at the time of my stroke. And I was actually, I had already been shopping for an engagement ring. I had the ring picked out. And on the day of my stroke that Saturday, I was supposed to call the jeweler to schedule an appointment for the next week to go pick out you know, the center stone.
Blair Ames 56:17
So of course, I didn’t get a chance to call him that day. I think I ended up calling him from the hospital a couple days later. And I was just like, hey, Sergio, you’ll never guess what happened, I guess I’ll see you in a couple of weeks. So I ended up going to see him. We’ve got the ring probably six to eight weeks after my stroke. And then I proposed to Mallory in September of that year, so about four months after the stroke. So we are four months delayed.
Bill Gasiamis 56:55
Yeah, that’s okay. She said yes. And was that a relief to you? Had you created any stories or any thoughts in your head about how that might go? Because of the stroke, because sometimes after these incidences, relationships change. I’m not questioning Mallory, or any anything like that. I’m just curious about what was going on in your head?
Blair Ames 57:26
No, of course. Well, I know she’ll appreciate you asking that. But she’s always been 100% supportive of me. And and I think, you know, our relationship over the past two years, was challenged because of the stroke for sure. But I think you could also argue that it’s been improved, because of the stroke now that we’ve gone through this together. And I mean, for me, I was just very disappointed that I hadn’t proposed to her sooner as I had a stroke, and as I was recovering.
Blair Ames 58:08
Because it just, there was a point in recovery. Where as we discussed earlier, it kind of dawned on me how close I was to not making it. And I think in the worst case scenario, if that would have happened. And I didn’t have the chance to propose to her. That thought devastated me. So after the stroke, and as I recovered, it was it became more and more of a point of I have to do this sooner rather than later.
Bill Gasiamis 58:49
Yeah, right. That was a little regret kind of looking around was it.
Blair Ames 58:56
Yeah, just as you look back on your older self, and it’s like, what was Why did I not do this sooner? You know, why did I almost not make it to this point of being able to do this?
Bill Gasiamis 59:09
And out of curiosity, why do you think you delayed that event?
Blair Ames 59:15
It was actually, my sister was getting married around that time, I was shopping for a ring. So that was part of it. Just that, you know, we were going through that with her. I don’t know, maybe it was just, I just was little too immature to get married.
Blair Ames 59:34
You know, I need to mature a little bit as I got through my early 30s. But I don’t know it was something I had been thinking about for a while and I just never really you know, I’ve been thinking about a ring. I just kind of never pulled the trigger, so to speak.
Bill Gasiamis 59:51
Yeah. Yeah. Well, look, it’s not uncommon people question that all the time that they should I should and I will To say, it’s pretty standard, you know, that’s nothing to be to feel bad about, but I get the part of oh my gosh, I almost never got the opportunity to and then that wouldn’t have been nice, at least then you would have had expressed your deepest desires.
Bill Gasiamis 1:00:20
And you would have been able to give that person the opportunity to know what your deepest desires were. And I think there’s an there’s a level of in a relationship is there’s there’s something really, really deep and meaningful, not just about the fact that you’re living together, but the fact that you’re prepared to ask such a serious question.
Bill Gasiamis 1:00:46
Which is, this is how I think of you like this, I don’t just think of you as somebody who we live together, and we’ve spent three years together, I think of you like this, I think that’s a really kind of deep, you know, emotional message that you’re sending to that person and to have the opportunity potentially go would have would have been a thing that wasn’t able for Mallory to experience.
Bill Gasiamis 1:01:23
And then I think that’s kind of where the both the for you, you’re kind of lost would have been in that phase. But also, she would have the loss of not experiencing the deep meaning of what it means for you to ask her the type of question that you were really hoping to ask.
Blair Ames 1:01:48
Yeah, and as we were discussing earlier, just about when the severity of the situation hit me, that was certainly part of that experience for me, you know, just realizing kind of what’s, what would have been left undone, so to speak. That was really eye opening as I progressed to recovery in those initial weeks and initial months.
The current status of the AVM
Bill Gasiamis 1:02:14
So how did they resolve this AVM in your head? What did they do to resolve it? What’s stage is it at now?
Blair Ames 1:02:24
Yeah, well, I guess it’d be appropriate to say I still have it. It was in the right basal ganglia. And it was just since it’s, it’s really right there in the center of my brain. It wasn’t it was to it was unsafe to operate on it. So I’ve been undergoing radiation treatments. And I’ve had one or two thus far, and it’s been all the progress from the doctors has been positive. They they said on this on the CT scans on the MRIs, it’s closing up. So in the coming years, I will continue to go through all the MRIs, the CT scans, the angiograms, and hopefully, radiation treatment will resolve my view.
Bill Gasiamis 1:03:17
So is that radiation treatment, what they commonly refer to as gamma knife?
Blair Ames 1:03:24
I believe that’s correct. Yeah. I think mine’s I think what the device I was under was called the CyberKnife. But yeah, I think that’s correct.
Bill Gasiamis 1:03:30
Right, right. How does it feel when you go through that procedure when they zap your brain with radiation
Blair Ames 1:03:38
I have the helmet right here that holds your head down on the table.
Bill Gasiamis 1:03:47
Lift it up for us in the middle of the screen. And for everyone listening who wants to see it, I’ll post a picture of it in the show notes. And then if you go to the YouTube video, you’ll be able to see it as well. I’m definitely going to use that as the thumbnail of this podcast for sure.
Bill Gasiamis 1:04:07
And we’re gonna get you to pose with it later, before we end the show so people can see it straight away. So So what they do is they lay you down and then they put that amazing helmet on your head and what does that meant to do?
Blair Ames 1:04:25
This is just meant to hold your head in place to make the best of my understanding is to hold your head in place so they do not zap the wrong parts of your brain. And the you know, the the the radiation treatment itself may have been about an hour, hour, hour and a half for me and it’s certainly certainly wasn’t painful in the moment.
Blair Ames 1:04:53
You know, the after effects. You definitely feel it that day in terms of just the fatigue But it’s very, very difficult to get into a car afterwards. Very easy to just get dizzy standing up too quickly. So the the procedure itself, thankfully, is is painless. It’s the the after effects in the in the days and weeks afterwards that can be a little difficult. But for me I, I was pretty much fully recovered after a few days, I reported back to my neurosurgeon that I didn’t need any additional medication painkillers, anything like that I was able to bounce back pretty quickly.
Bill Gasiamis 1:05:40
And the second time, what’s more familiar? Does that make it easier? Does you get through it a lot better?
Blair Ames 1:05:48
Yeah, no, I just got going through the process, you know, multiple times and being there in the facility kind of knowing what the steps are. It was the honestly the hardest part for me, was the first time I had requested a certain Pandora station be put on my headphones during the procedure.
Blair Ames 1:06:09
And unfortunately, they ended up choosing like a Mexican pop station. So I was hoping for a different form of music. But I ended up laying there for the better part of an hour. Listening to like I said, sounded like Mexican pop music, I wasn’t quite sure what what it was, it was like Mexican salsa or something that made it uncomfortable.
Bill Gasiamis 1:06:39
They might have done it on purpose. I love that idea that the music made it uncomfortable. But it’s really important, isn’t it because it helps you focus concentrate, and get distracted from what’s going on around you. I remember going into the MRI, and then listening to, again, the local radio station, which was terrible. And you had to be in there for 30 or 40 minutes.
Bill Gasiamis 1:07:05
And just hoping that it was over. And then as I got to understand that I could request my own music, I took a guided meditation in with me. And that guided meditation, it lasted for the duration of the MRI. So not only was I meditating, putting myself into this space of feeling really calm and comfortable and all that kind of stuff.
Bill Gasiamis 1:07:29
The procedure just felt like minutes instead of 40 of them, you know, just felt like a couple of minutes. But everyone’s got, I reckon an experience with an MRI or gamma knife or something like that, where they have to remain still for a long period of time. And choice of music is far from optimal.
Blair Ames 1:07:53
That’s a great, great idea from you to use a meditation, I had never thought of that before. I was just thinking what is my favorite type of music that I would like to listen to for this, I’d never thought of taking a meditation in there.
Bill Gasiamis 1:08:04
Yeah, because and then the meditation, what it also does is hopefully it calms the body relaxes the muscles, it decreases the cortisol levels, it settles your heartbeat, it settles your blood pressure, it does all of that stuff. So it kind of creates, it puts you into an optimum state so that you can be the best kind of patient for them on the day. So it helps with their procedure, I feel.
Bill Gasiamis 1:08:32
So that was my thinking behind it, as well as the fact that I love meditations. And if, if I’m on a meditation and it kind of puts me to sleep, well, then that’s better than being anxious and annoyed and frustrated at what’s happening with your head locked into the device that they lock it into. So you don’t move. But that’s good man, that you’re you’re progressing through that resolution as well.
The possibility of another AVM bleed
Bill Gasiamis 1:09:02
So to put this thing to bed, so to speak, has it been on your mind that they hadn’t removed that it was still there. And that it was hard to remove. Did you think about the fact that there was a possibility? Did they tell you that there might be a possibility that it re bleeds? How did you handle that part?
Blair Ames 1:09:25
Yeah, no, that’s that’s a good question. Um, for me, I was always advised that there was a very small chance that it would bleed again. You know, I don’t quite remember exactly the percentage they gave me. But I was always struck by as I researched AVMs myself and continued talking to doctors in the subsequent weeks and months after my stroke.
Blair Ames 1:09:55
That generally it seems like the the biggest precursor to an AVM rupturing is a previous rupture. So that was always a little unsettling. But over the past two years, it’s really it’s not something I generally think about. It doesn’t affect how I go about doing anything. I think I certainly hope I’m not in this situation. But if it were to ever happen again, I’m sure I would react a little differently this time around. But in terms of thinking about it on a day to day basis, I never really think about it.
Bill Gasiamis 1:10:40
Yeah, I like to think that you’re a smart guy, and that you would respond differently, I definitely responded differently. Every time I had a bleed, I was better and better and better. So mine bled three times. That’s why it lasted the whole process to surgery almost took three years, because they were hoping that wouldn’t bleed again. And they told me the same thing.
Bill Gasiamis 1:11:05
And I went about my life as normally as I could dealing with the deficits and the fatigue, and all that kind of stuff. But I still went about life. And I didn’t think about it on the daily. I’ve kind of mentioned that a few times. But my my motto in life is expect the best prepare for the worst. So I had contingency plans in place.
Bill Gasiamis 1:11:28
But I wasn’t going to go about being anxious about the fact that this thing would play it again, you know, we were we were just going to be proactive. If it did, we were going to do the right things and get help immediately. So that’s what we did. And and the third time when eventually, they bled the third time and they decided to take it out. It wasn’t me who said let’s get this thing out.
Bill Gasiamis 1:11:55
My surgeon said, it’s time to get it out. We need to get it out. We don’t want it to continue bleeding, it’s not likely that it’s going to stop bleeding. It seems like it’s one of the rarer ones that is that might continue to bleed. And that’s putting you at greater risk than surgeries. So we should go there, we should definitely get it done. Are you up for it? And I said, Well, yeah, I’m up for it.
Bill Gasiamis 1:12:19
Let’s resolve it one way or another. And that’s what we did. I like hearing your story, because you go about things in a very seems like a very calm, gentle way. You’re progressing really nicely. You know, you’ve overcome a lot of the hurdles, you’re aware of what some of the hurdles are, which is a really good thing, when you become aware that stroke recovery is not just about the physical recovery, it’s also about the mental and the emotional recovery.
Bill Gasiamis 1:12:54
That’s a big game changer, man, that is making your stroke recovery far better than it would have been. And that’s also allowing you to deal with all the stuff that arises between you and Mallory in your relationship. Because you’re realizing they’re part of my response, my lack of emotional awareness, perhaps, or my emerging emotional awareness or my awareness that now that it’s happened, I have reacted, but now that it’s happened, I’m aware of it so I can resolve it with you.
Bill Gasiamis 1:13:39
I can tell you that I’m sorry, because I wasn’t intended to behave that way or whatever. And I’m doing better. And that is taking out the stress in the relationship. And that creates a bit of space for recovery. And that makes her feel about the things that you guys are going through better. So you’re just doing great things. And that’s what I said at the beginning of the podcast episode.
Bill Gasiamis 1:14:04
It’s like, it’s so good to have you here after us being in conversation on and off for the last couple of years. And then finally, to get you here, it’s like, wow, man, that is brilliant. Firstly, I’m grateful that you found me when you did and that the podcast gave you hope. And now, I’m certainly grateful that you’ve recovered to a point where you felt like you could be my guest and we could learn from each other.
Blair Ames 1:14:34
Yeah, Bill, I appreciate those kind words for sure. And you know, as I mentioned earlier, your podcast and those early days. We know when I was too tired to really get off the couch, you know, just pretty much worked through some rehab stuff and then sat on the couch all day before I was back at work. Certainly your podcast was one of the most popular things I watched on YouTube in those days. So I guess I like to think Maybe I picked up some of my perspective, from you and from I learned a lot from you.
Bill Gasiamis 1:15:06
They’re beautiful. And all those awesome guests that have come on before you as well to be a guest on my podcast is such an amazing thing for people to just say that they want to be on my podcast is just oh my gosh, like, it’s just the most amazing thing for me that somebody wants to be on my podcast, I love it. So thank you. As we kind of wrap this up, I was just curious about what you feel stroke has taught you.
Blair Ames 1:15:33
You know, I think as I mentioned earlier, stroke recovery is everything that I didn’t expect it to be. You know, in those early days in the hospital, I was just running through my mind all of the physical exercises, I could do all of the things I could do to get physically better.
Blair Ames 1:16:05
And then once I got out of the rehab center, and once I was home, just working through everything and realizing that, you know, my emotions were were sky high some days, and then in the bottom of the valley the next day, riding that roller coaster.
Blair Ames 1:16:27
I think stroke probably taught me a ton in terms of just how do we maintain our well being is not all about working out. It’s, you know, you know, it’s not all about being active. That’s That’s an incredible, credibly important part of it. But I’ve certainly learned the importance of sleep. I’ve I’ve as I had already pretty much dialed in my nutrition before I was big on nutrition before the stroke.
Blair Ames 1:17:00
But I’ve certainly made some changes in that regard. And then just overall, you know, how do you improve your mental well being, I think I’ve really realized the importance of meditation. I’m very grateful that I had started a meditation practice before stroke, because that was something that I leaned on heavily over these past two years.
Blair Ames 1:17:24
So I think stroke has really opened my eyes to some things that before the stroke I just never would have even thought to pursue. It’s taught me a lot about how I can physically improve my well being, you know, outside of the gym, and I’m grateful for those opportunities.
Blair’s advice to stroke survivors
Bill Gasiamis 1:17:49
Brilliant. As we get to the final question, I’d like to ask you, there’s people that are listening now that are waiting in the same stage of recovery that you were two years ago. They’ve just found the podcast. And they’re trying to get as much information as they can out of us so that they can be guided on their own recovery. What would you tell somebody who might be listening? Who’s at early stages of recovery? What are some of the things that you’d like to impart on them that they should know? Maybe one thing doesn’t have to be lots.
Blair Ames 1:18:29
No, of course. And that’s something I thought about a lot in terms of what would if I could go back and talk to myself in those early days, you know, what would I tell myself, because I hate to sound like a broken record. But as I mentioned, it’s like I was just so naive to what I was getting into.
Blair Ames 1:18:49
You know, I was so focused on physically getting better. And I had no idea about the physical and mental challenges that were coming down the road. And I was really never someone that resonated with the stay positive mantra. That was something that was just “Thanks, I appreciate your advice”.
Blair Ames 1:19:13
But I think if I could give somebody advice, who is in my situation, I would tell them to just embrace those challenges, embrace those early days of recovery. Because I think when you’re really struggling, is when you really find the opportunities to find innovative solutions. And instead of, you know, being upset about the situation, just embrace the challenge. And, and, and be ready to learn a lot and be ready to to improve over time.
Bill Gasiamis 1:20:00
Beautiful Man. Blair, thank you so much for being on the podcast.
Blair Ames 1:20:06
Hey, Bill, thank you. I really appreciate your time.
Bill Gasiamis 1:20:08
Well, thanks for joining us on today’s episode, you can see now why I was so grateful to have Blair on the show. He has come a long way in his stroke recovery journey, but he’s got some way to go. And he’s been able to learn a lot about what this journey the road that this journey has put him on, he’s learned about himself, he’s learned about things that he never expected, he’s grown as a result, and his recovery continues to occur.
Bill Gasiamis 1:20:42
And he continues to evolve, which is just amazing. To learn more about my guests, including links to their social media and other pages, and to download a full transcript of the entire interview, please go to recovery after stroke.com/episodes.
Bill Gasiamis 1:20:57
If you would like to try the course five foods to avoid after stroke, go to recovery after stroke.com/courses If you’d like to support this podcast, and now I’m going to explain why you must support this podcast by giving it a five star reviews because people like Blair, who have been listening for two years, get to feel a lot better about the way that their recovery is coming along, and then get to finally be at that point where they can get on the podcast.
Bill Gasiamis 1:21:24
That’s exactly what the podcast is meant to do. Paint that picture is give hope is show people that there is light at the end of the tunnel. And therefore I would love it if you left the show a review so that more people like Blair, who are at the beginning of their journey can find the podcast and as a result of that hopefully make a difference to their recovery.
Bill Gasiamis 1:21:51
It’s also something that helps the caregivers of the stroke survivors because a lot of caregivers reached out to me to tell me that the show has been really helpful. So any positive feedback on Spotify or on iTunes will really have any positive feedback on YouTube will really help and be really appreciated.
Bill Gasiamis 1:22:12
And it’s just going to make it easier for people like you and me to get what they are missing, which is what I was missing. When I was going on this journey. There was no podcasts in 2012, about the possibilities that I was going to get better after stroke. So it was a lot lonelier back then.
Bill Gasiamis 1:22:31
And I’m hoping that this podcast makes it less lonely for you. So that’s my request from you and then come and join me on the show. Come and be a guest on my show that interviews are not scripted, you don’t have to plan for them. All you need to do to qualify as be a stroke survivor, a caregiver of a stroke survivor or somebody who works in the field of helping stroke survivors.
Bill Gasiamis 1:22:57
So go to recoveryafterstroke.com/contact fill out the contact form. And as soon as I receive your request, I’ll respond with more details on how you can choose a time that works for you and me. We’re going to meet over zoom, the interview will be recorded it will go on YouTube, it’ll go on iTunes, Spotify, and everywhere else. And hopefully your interview with me will make a difference to some other people. So thanks again for being here and listening. I really appreciate you and see you on the next episode.
Intro 1:23:28
Importantly, we present many podcasts designed to give you an insight and understanding into the experiences of other individuals opinions and treatment protocols disgusting any podcast or the individual’s own experience and we do not necessarily share the same opinion nor do we recommend any treatment protocol discussed all content on this website at any length blog, podcast or video material controlled this website or content is created and produced for informational purposes only and is largely based on the personal experience of Bill Gasiamis.
Intro 1:23:58
The content is intended to complement your medical treatment and support healing. It is not intended to be a substitute for professional medical advice and should not be relied on as health advice the information is general and may not be suitable for your personal injuries, circumstances or health objectives. Do not use our content as a standalone resource to diagnose treat, cure or prevent any disease for therapeutic purposes or as a substitute for the advice of a health professional.
Intro 1:24:23
Never delay seeking advice or disregard the advice of a medical professional your doctor or your rehabilitation program based on our content if you have any questions or concerns about your health or medical condition please seek guidance from a doctor or other medical professional if you are experiencing a health emergency or think you might be.
Intro 1:24:39
Call 000 if in Australia or your local emergency number immediately for emergency assistance or go to the nearest hospital emergency department. Medical information changes constantly. While we aim to provide current quality information in our content. We did not provide any guarantees and assume no legal liability or responsibility for the accuracy, currency or completeness of the content.
Intro 1:25:00
If you choose to rely on any information within our content you do so solely at your own risk we are careful with links we provide however third party links from our website are followed at your own risk and we are not responsible for any information you find there







