A stroke from cracking his neck to relieve the tension was the last thing Mac expected. At 24 years old and a trained EMT he knew immediately that he was experiencing a stroke.
Highlights:
01:57 Introduction
02:57 Neck Cracking And Stroke
09:11 Misdiagnosis
17:15 Initial Rehabilitation
21:35 Parent Concerns
25:21 Realizing The Effects of Stroke
33:01 Losing The Ability
42:29 Seven Stages of Grief
54:16 What Caregivers Have To Deal With
1:01:14 Kintsugi
1:09:59 The Intubated State
Transcription:
Bill Gasiamis 0:00
Hey, Mack, you know, mom just said that you didn’t know that you couldn’t walk? When you found out what was that, like?
Mac Brand 0:08
That was such a harsh learning experience because it wasn’t so much that I didn’t really think about, like, I couldn’t walk, it was more like I remember how easy it was to kind of even move or do stuff.
Mac Brand 0:21
But then I’d be like, a lot of confusion as to essentially why things were so difficult. It was all learning. And just, I mean, like, I was in a fairly delusional state too where it was just like I kind of was expecting that I would just kind of get to leave the hospital too.
Mac Brand 0:39
Like, once I got the tube out and everything, I remember being ecstatic about that, because I could finally talk I didn’t realize how much I wanted to talk after like a week or two. And everything I was saying was delusional and didn’t make sense when I was just excited about it.
Colleen Brand 0:57
This is the recovery after stroke podcast. With Bill Gasiamis, helping you navigate recovery after stroke.
Bill Gasiamis 1:11
Hello, and welcome to another episode of the recovery after stroke podcast. Recently, Spotify released a new feature which allows you to narrate your favorite show, in the same way that the apple podcast app allows it.
Bill Gasiamis 1:26
If you think the show deserves it, I’d love it. If you left us a five-star review. This will help the show rank better on search engines and help newly diagnosed stroke survivors find the show better.
Bill Gasiamis 1:37
And it could make a massive difference in their recovery. So go to your favorite podcast app, whether it’s Spotify, Apple, whatever it is, and share what the podcast means for you. It really will make a huge difference to how people find the podcast and how they have a better stroke recovery.
Introduction

Bill Gasiamis 1:57
Now, this is episode 190. And my guests today are Mac and Colleen brand who I reached out to after seeing a photo that Colleen posted of the scar on the back of Mac’s head, which she upgraded in the tradition of the ancient Japanese art of Kintsugi by painting a gold to enhance it and embrace its imperfections by highlighting it.
Bill Gasiamis 2:24
Now Mac was an EMT age just 24 when he had an ischemic stroke that he caused by cracking his neck to relieve tension. Colleen and Mac brand. Welcome to the podcast.
Colleen Brand 2:37
Thank you.
Bill Gasiamis 2:40
Guys, thanks for reaching out and connecting. I have done a little bit of pre-reading of Mac stuff. And I’ve seen the video the unfixed media video, tell me Mac a little bit about what happened to you.
Neck Cracking And Stroke
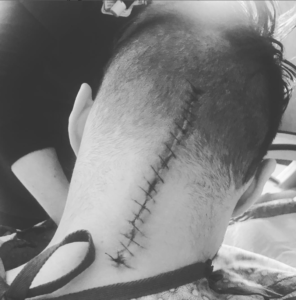
Mac Brand 2:57
So, I think it was it was a long time ago. Well, not that long ago, it was 2018. I remember I got back from really, I think I got back just from vacation. And I was sitting at home one day and I cracked my neck which I guess which ended up causing me to have a stroke or something.
Mac Brand 3:27
I mean, not something. It caused me to have a stroke. So then I walked to the hospital and I woke up like, you know, a week or two later and suffering the effects of the stroke, which was a cerebral brainstem stroke.
Mac Brand 3:50
I when I first woke up, I had, you know, partial paralysis on my left side. Now it’s more just kind of incoordination and stuff like that. Yeah, so that’s the like real summary version of it.
Mac Brand 4:07
Which was just from manipulating my neck, I was able to, I guess shed the inner lining of some sort of veins in your vertebrae, and I’m not sure shoot it up to my brain. It was a kind of experience.
Bill Gasiamis 4:29
I’m curious. You seem not to be completely aware of what happened is that because of a memory issue, or you haven’t really been told or haven’t paid attention?
Mac Brand 4:39
So I know it’s mostly a memory issue right now just because I’ve been told over and over again, honestly, what it is but what happened but it’s a it is more of a memory issue. It’s kind of one of those Yeah, that’s one of the things
Bill Gasiamis 5:03
Colleen, give us your version of that story.
Colleen Brand 5:06
Yeah, it’s interesting listening to Mac because I don’t know whether his memory comes in ebbs and flows. But anyway, he had just come back from being in San Francisco visiting us where we live in San Francisco, he had just gotten back and to Colorado.
Colleen Brand 5:33
And he had cracked his neck like he does, he does that left-right motion and cracks his neck when he has a headache and relieve some pressure. And that caused a blood clot, that action caused a blood clot, which caused him to have the stroke symptoms.
Colleen Brand 5:56
And I wouldn’t have recognized that but because Mac had EMT training. He, knew stroke symptoms. So he identified it himself really quickly. And he knew that it was going he had about 15 minutes before he’s going to collapse.
Colleen Brand 6:19
But he didn’t call 911. I think his logic was already going because he was so dizzy. He went, Okay, I’m a couple blocks from the small community hospital, I’m gonna walk there.
Colleen Brand 6:33
And he was starting to walk there. And that’s when he collapsed. But he knew enough he was able to do 911 before he hit the pavement, and then that’s where he was found. And then that’s where we went through the sequence of Boy, I wish I knew then what I know now about strokes. Because boy, would we have handled it differently.
Bill Gasiamis 7:08
That’s a very common story. everybody’s the same on the same. How do you suppose to know about strokes? If you’re not familiar with somebody who’s had a stroke, and you’re really aware of what happened and how it went down?
Bill Gasiamis 7:22
I mean, you just won’t know. How are you going to know about anything broken toes, damaged knees, you’re not going to know unless it happens to you. And that’s the scary thing. But was Mac alone at the time?
Colleen Brand 7:40
Mac was by himself.
Mac Brand 7:41
I was alone. And so I remember the term it was I had a vertebral artery dissection. That’s just what happened to me, which is kind of like a walking urban legend thing to where it’s like you cracked your neck and you get that?
Mac Brand 7:59
Yeah, I was alone. At the time. I didn’t really recognize that was a stroke until I started feeling paralysis actually, when I was walking there to the hospital it was only about three or four blocks away.
Mac Brand 8:10
And then when the ambulance came, they started running stroke protocols on me and I was like, that’s not right. I’m 24 and I’m just dizzy. You know, it was one of those things where it just kind of kept getting, it started out as just being dizzy.
Mac Brand 8:27
It felt like I described it as like, you know, when you get too drunk and you’re just kind of like spinning so I thought originally I had food poisoning because it’s like, what do you mean I’m having a stroke?
Mac Brand 8:42
But, you know, I eventually learned, waking up I was I had gone to the hospital when I had appendicitis I literally walked in there like pop my appendix out so I kind of figured do the same deal, I woke up a couple of weeks later and was not the same deal at all you know?
Bill Gasiamis 9:02
Yeah. And in those two weeks Colleen what’s the family doing because Max was out of it. What are you guys trying to do?
Colleen Brand 9:11
So the smaller hospital really botched things up. They actually did not treat him for any stroke protocol. So that was a huge delay. These are the delays that it’s so great to get people that everyone should have better stroke information so that they’re empowered understand how critical time.
Misdiagnosis of Mac Brand
Colleen Brand 9:11
Again we don’t know this walk until we walk it right? And so you don’t realize how critical that first 72 ours is. And so they actually dismiss Mac, because he had smoked some weed before he had cracked his neck.
Colleen Brand 10:13
And so they dismissed him as just being a young stoned man. And so when he was walking out of the hospital, he collapsed in the hospital. And that’s when they brought him back. But they still didn’t follow any stroke protocol.
Colleen Brand 10:32
And he’s by himself with no one to advocate for him at that time, there was a tremendous amount of time lost, then they finally got him to the next level Hospital, which didn’t have any type of a stroke department or neurology department that they brought in a neurologist who was a very unqualified individual.
Colleen Brand 11:06
And but he really wanted to hang on to Mack, he didn’t want to take him over to the better hospital at Ann Schultz, which had a proper neurology department, which is what Mac was needing. And he really wanted, I’m assuming that was for the revenue.
Colleen Brand 11:23
He really wanted to, because it wasn’t because of his abilities. So he actually drilled into Max had to try to relieve some pressure. And it was not even in the right spot we found out later. So it was for naught. And so we wasted another night there.
Colleen Brand 11:44
And quite honestly, we, at that point, we started to educate ourselves and make phone calls. And we found out about Ann Schultz. And they wouldn’t release him. And so we had to work on it ourselves to demand that he gets released.
Colleen Brand 12:02
And Mac went unconscious very, very quickly. And but fortunately, at the very same time, the the helicopter team was landing at the hospital. And honestly, these people were right out of a movie.
Colleen Brand 12:20
They’re such heroes in their work. They dismissed that hospital team. Mac was already intubated and passed out at an unconscious at that point. And I watched them literally unplug and redo everything, dismissed those people.
Colleen Brand 12:38
And they took him over and got him airlifted to Ann Schultz, which they told us immediately to drive there. And, you know, we signed the paperwork. And as soon as he landed, they had him going into surgery. And they saved his life.
Bill Gasiamis 12:56
So they drilled into his head to relieve pressure.
Colleen Brand 13:02
Yeah.
Bill Gasiamis 13:02
Was there a bleed in the brain?
Colleen Brand 13:05
Yeah, we had a brain bleed that wouldn’t stop.
Bill Gasiamis 13:09
Okay, so he had a brain bleed and a clot?
Colleen Brand 13:14
Yeah.
Mac Brand 13:14
Yeah, it wasn’t necessarily a clot. I think I remember them describing that as the inner lining of my artery that essentially was shed when I cracked my neck. And it kind of shed itself so it wasn’t like I had a clot that got dislodged it was actually a part of the artery an interior lining or something.
Bill Gasiamis 13:42
But at the same time, there was a bleed Mac? Was there some blood bleeding into the brain?
Mac Brand 13:48
Yeah, I believe so. I mean, yeah, at that point, also, like, I remember, I was either unconscious or my brain was swollen. I wasn’t really aware of anything until probably even like a month after, you know.
Colleen Brand 14:02
No, he wasn’t I don’t even think that he came out of being in this induced coma state for several weeks. And when he first did like I drew him this picture. I don’t know if you can see it.
Colleen Brand 14:27
But basically it was trying to get him to understand do not freak out because you’re intubated. And so we wanted, because I kept thinking about, Oh, my God that has got to be so fearful when you start to become alert from that coma state, and you’re intubated.
Colleen Brand 14:55
I can’t even imagine what the panic one would feel. So we were really, really surrounding him and trying to figure out the best way so that we can stay calm when he came to that you are, you’re intubate you can’t speak.
Colleen Brand 15:17
You’re not going to breathe on your own. I don’t know what a person is going through when they transition from that point to the other. But that was a huge concern for us. Of how do we keep him from being panicked?
Bill Gasiamis 15:36
Mac, do you recall what that was like when you woke up in that state?
Mac Brand 15:43
So it’s, yeah, I do actually. Well, like, it’s really interesting, because I didn’t know I was going to wake up in that state. It’s kind of like blinking. And then, you know, one second here, there.
Mac Brand 15:55
And also, at the time, you have to remember my left side I had center paralysis, and my left side was paralyzed. But my right side was actually just as strong as it was before. So they had to kind of restrain it, when I was getting up to make sure I couldn’t move around.
Mac Brand 16:14
And my brain was still swollen, and when you’re intubated you’re on a lot of like fentanyl and stuff, so I spent, like the first probably week or two fairly delirious under those circumstances.
Mac Brand 16:28
And honestly, I kind of remember it, almost humorously, because they’re some of the things they had to put like a pizza, like an oven mitt on my hand to make sure I couldn’t grab stuff with my good hand.
Mac Brand 16:40
And because I was essentially like, you know, a toddler almost. You don’t want to grab on the tubing or anything like that. So I had this pizza mitt. And I remember thinking, like, Oh, God, I’m in a Pizza Hut, like, you know, like, just not being able to connect the dots even to what is happening. It’s just, I mean, yeah, I honestly, I look back at it almost humorously, but it was pretty traumatizing for everyone.
Mac Brand’s Initial Rehabilitation
Bill Gasiamis 17:16
Absolutely, I can imagine, man. So when you finally got out of the hospital, I imagine you went to rehabilitation, what did you have to rehabilitate.
Mac Brand 17:27
So, I spent one month in inpatient rehab. And then essentially, like, kind of have to test out to make sure you can shower on your own you can do and cook on your own, you’re not going to be a danger.
Mac Brand 17:40
So I did that. A lot of my rehabilitation was essentially strength training. Because the left side of my body fatigues twice as fast as the right side. So a lot of times, it’s just things like, it’s a lot of just walking and, you know, getting that muscle memory to kind of work and retrigger and rewiring that neuroplasticity around those damaged parts of your brain.
Mac Brand 18:10
So it’s like, you know, you lose parts. But the nice thing about having a stroke when you’re 24 Is that your brain will kind of remap itself around that damaged parts. So it’s like, yeah, I might not be able to open a key with my left hand anymore, or whatever.
Mac Brand 18:26
Or hold a spoon with it. But it’s like, I couldn’t really do that with my left hand either way, things like typing. Like, it’s just one of those things where it’s like, yeah, fine motor skills and muscle memory are super important for getting that stuff back and just kind of triggering that neuroplasticity to help rewire your brain around what’s been damaged.
Bill Gasiamis 18:44
And you had to learn how to walk again?
Mac Brand 18:46
Oh, yeah, I spent a long time learning how to walk. I was, you know, I still have my cane with me for when I get tired. I have a lot of neurological fatigue associated with it. So it’s like, I look really good for probably about 30 minutes, and then I get real limpy or I need my cane.
Mac Brand 19:07
So I still get a lot of neurological fatigue. And it’s like, oh, there’s the stroke, you know. So it’s one of those things where it doesn’t really get away for me, while I can kind of like compound the time where I’m, you know, where I’m strong and kind of, you know, mobile and doing my stuff. It’s always kind of one of those things where it’s like you kind of hit a wall at a certain point in the day and it’s like, okay, now I’m, you know, kind of back at it.
Bill Gasiamis 19:35
Yeah, we went and saw Batman with my wife last night. And we got the eight o’clock session, not realizing that it’s a three-hour movie. So sitting down in the chair watching that was pretty cool movie but then you get tired and then by 11, 11:30 we had to walk back to the car quite a distance and the left side is numb the knee is not supported 100%.
Bill Gasiamis 20:07
The hamstring is feeling a little bit weird. And the quadricep is feeling a little bit weird. And it’s like, okay, I’m really tired. Now I can tell that I’m tired, and I need to go to bed and sleep immediately.
Bill Gasiamis 20:20
So I get what you’re saying it does take some time to get beyond the neurological fatigue, where you feel like, I know I’m tired. But I can still sit through the movie, for example. But there was a time where I couldn’t, I would never take an eight o’clock session to go watch a movie. Because I wouldn’t be able to get through it. And then I would feel terrible the next day.
Mac Brand 20:49
Yeah, I’m kind of like, right in that space. I feel like I’ve been doing really well with a lot of my mobility exercises, I feel like have been really helpful with just kind of making me not feel like I’m, you know, almost lopsided, or whatever, you know, with my strength. But yeah, sitting through, I noticed my fatigue hits really hard, where I just even paying attention or focus on like, a movie for three hours. Sounds like a task.
Bill Gasiamis 21:22
Yeah, yeah. It used to be for me as well does gets better. But I think you’re still in the early days of recovery. You might sound like you’ve been doing it for a while. But stroke recovery takes a long time. And so you’re still in the early days.
Parent Concerns
Bill Gasiamis 21:35
Colleen, what’s it like sitting on the other side, watching your son in hospital, being really unwell, and then not being able to use his left side?
Colleen Brand 21:49
In all honesty, because we came so close to losing him. I was so grateful for him being with us. And then that roller coaster of you know, will his brain start bleeding again, because that kept happening.
Colleen Brand 22:17
And there were so many times I’ve never prayed so hard in my life. And just every little thing you’re like, just get us there. We didn’t know when they could finally take out the tube. We didn’t know if his chest would collapse. We didn’t know if he was going to be able to breathe on his own.
Colleen Brand 22:46
We didn’t know if he was going to be able to swallow. And we didn’t know if he would be able to walk again. You’re there’s so many things you don’t know you really do take every moment of that that you get to go forward, it feels like a miracle.
Colleen Brand 23:08
And you’re so grateful. I felt that we had incredible doctors, we had incredible care at Ann Shultz. And we are so thankful that Mac got those breaks to be able to swallow and did not have to go through a tracheotomy.
Colleen Brand 23:32
When they finally were able to have him start to even sit up. He didn’t know he couldn’t walk. There was a lot of things that he didn’t know. And it was probably better he didn’t know because it’s just so much you’re going through.
Colleen Brand 23:59
But yeah, to not lose him, that he would just have the opportunity to get better, was all the miracle I could ask. And then everything else that we got afterwards was just an absolute gift.
Intro 24:19
If you’ve had a stroke, and you’re in recovery, you’ll know what a scary and confusing time it can be. You’re likely to have a lot of questions going through your mind. Like how long will it take to recover? Will I actually recover? What things should I avoid in case I make matters worse.
Intro 24:36
Doctors will explain things that obviously you’ve never had a stroke before. You probably don’t know what questions to ask. If this is you, you may be missing out on doing things that could help speed up your recovery. If you’re finding yourself in that situation.
Intro 24:51
Stop worrying and head to recoveryafterstroke.com where you can download a guide that will help you it’s called Seven Questions to Ask Your Doctor About Your Stroke. These seven questions are the ones Bill wished he’d asked when he was recovering from a stroke.
Intro 25:07
They’ll not only help you better understand your condition, they’ll help you take a more active role in your recovery, head to the website. Now, recoveryafterstroke.com and download the guide, it’s free.
Mac Brand Realizing The Effects of Stroke

Bill Gasiamis 25:21
Hey, Mac you know, mom just said, that you didn’t know that you couldn’t walk? When you found out what was that like?
Mac Brand 25:31
That was pretty. I mean, like, it was all such a harsh learning experience, because it wasn’t so much that I didn’t really think about, like, I couldn’t walk, it was more like, I remembered how easy it was to kind of even move or do stuff.
Mac Brand 25:50
But then I’d be like just a lot of confusion as to essentially why things were so difficult. But yeah, I remember just like, it was all learning. And I mean, like, I was in a fairly delusional state to where it was just like, I kind of was expecting that I would just kind of get to leave the hospital.
Mac Brand 25:55
Once I got the tube out and everything I remember being ecstatic about that, because I could finally talk, I didn’t realize how much I wanted to talk after, like a week or two. And everything I was saying was delusional and didn’t make sense when I was just excited about it.
Mac Brand 26:38
But I was fully expecting to go home and be like, okay, you know, but then I spent another month in inpatient rehab and stuff like that. And it was a slow, painful process to kind of reassess and be like, okay.
Mac Brand 26:53
But it was definitely helpful with me coming to like reality. Just like about what had happened. Because there was a long time where I honestly couldn’t even comprehend it.
Bill Gasiamis 27:11
Yeah, yeah. You probably had a couple of reasons why couldn’t comprehend the first you were on medication. Second, you’ve had a stroke. So it’s difficult sometimes to comprehend things.
Bill Gasiamis 27:23
And, I remember trying to walk the first time after I had the brain surgery, and I got out of the bed on the left side, and there was a nurse who was going to help me go to the, to the toilet.
Bill Gasiamis 27:41
And she said, you know, just step out, place your arm around my shoulder, and I’ll support you, she was half my size, and a bit shorter than me. So I’ve got out, I’ve placed my left leg on the ground. And because my left I couldn’t feel my left leg, it just collapsed.
Bill Gasiamis 27:58
So I’m out of brain surgery. Fresh scar on my head, literally just a few hours out of brain surgery. And then I went on my ass on the ground screaming because I fell out of the bed and the nurse wasn’t able to support my weight.
Bill Gasiamis 28:14
That’s when I found out I couldn’t walk. And then it was ok getting back into bed and book him into rehabilitation because they hadn’t assessed me yet. They just assumed that I came out, okay, because I moved my toes and moved my fingers and it was pretty rough.
Bill Gasiamis 28:32
So I know the feeling. I totally get it. You know mom, he looks pretty cool. He looks okay, he looks pretty normal. Everything’s okay. Is it sometimes difficult to connect the dots that he looks great. But he’s not the same inside like his ability to do the things that he normally did is not there. It’s not the same as it was. Is it hard to connect those dots sometimes do you look at him and go but you look great?
Colleen Brand 29:12
I don’t because I stayed with him in the hospital on that journey. So being able to experience it along with him. I knew we protected a lot of information from him. And mom’s know, you know, we know so I know all the differences of Mac before and after.
Colleen Brand 29:54
I do like even with his walking now. He has to walk at one pace. And I’m learning things all the time. We were out taking a walk the other day. And he was like, that’s when I found out that, oh, you can only walk at one pace.
Colleen Brand 30:13
He told me he can’t go slower, he can’t go faster. Because that’s the rhythm that he has taught himself to move. And so Okay, no problem. Now, I know this piece of information. And so I adjust my behavior accordingly. It’s a lot of eyes and ears, and less mouth.
Bill Gasiamis 30:40
Really learning how to interact with him. That’s awesome. I mean, I remember going for a walk with my son in one of the local malls. And he’s just taken off and he’s left me behind.
Bill Gasiamis 30:51
And he’s not paying attention to me behind. And I said you gotta come back, and he was like, ah, what happened? I can’t walk that fast anymore. I’m gonna walk slower. But we worked it out. I did get faster with time. Mac, what were you doing as a 24-year-old? What was your daily life like, where you at work?
Mac Brand 31:14
I was in my undergraduate, I was working two jobs. You know, I was in a full-time, you know, relationship so I was out in Colorado working on my undergraduate in criminal justice, criminal forensics, and working at a plasma donation center with my day job.
Mac Brand 31:40
And then I also did like, P.I work on the side, like kind of as a resume builder, too, which was an interesting gig. So I was working, I was doing a lot, honestly. And then I was probably about like, I would say, a junior year, like kind of in my undergrad.
Mac Brand 31:40
So it was about one or two years away. Took me another two years to finish it after the stroke, because I had the stroke actually, during my finals too. I failed my finals, I had like, B’s or something in those classes.
Mac Brand 32:08
But because I failed my finals, I had to redo my finals in the hospital. And I was like, I can barely read. So I just kept retaking those classes and just kept retrying. So it kind of spread it out a little bit.
Mac Brand 32:39
But I got the undergraduate done, at least I’m working on my Master’s right now, which is really cool. But yeah, it was definitely a big, huge bump in the road. I am stoked, though, that. I mean, if you’re gonna have a stroke, it might as well be at 24 when you’re still on your parents health insurance, you know, so that’s not the worst thing.
Mac Brand Losing His Abilities

Colleen Brand 33:01
I was a miracle. Yeah it was a miracle that we checked that box, it truly was. But MAC’s, a big dude. He’s about six, three. He’s always been naturally strong without ever lifting a weight. It’s just how he was drawn.
Colleen Brand 33:35
And so he’s always relied on that physical strength for a lot of work and jobs. And just one of those things, it’s like, it’s what you can do. And that’s gone. And so, that’s another adjustment.
Colleen Brand 33:56
It’s fine, you know, you adjust, but it’s just it’s another adjustment. And it’s another frustration for him. You know, when you’re used to having a certain physical ability. And now that one’s off the table too.
Colleen Brand 34:12
And as you know, it takes a great deal of effort of daily discipline, it’s a lot of discipline to maintain. What the corrections and the games you’ve been able to have, you have to work hard to maintain that.
Bill Gasiamis 34:34
Yeah, yep. It’s a different kind of work and because yeah, MAC one side is going yeah, well, let’s keep doing this. And the other side’s going no, I’ve had enough. And it’s a real mental battle because you actually physically have had enough you actually totally drained on one side.
Bill Gasiamis 34:55
But the other side’s quite fine and you got to find the balance right? You can to work out how to continue or why you should not continue, and for me, it was not continue. It’s like stop and rest because you are really tired even though your right side is okay and wants to keep going. That’s not the right thing to do right now the left side is really tired, that means the brain is fatigued. Mac do you relate?
Mac Brand 35:25
Yeah definitely, like essentially, almost exactly like, you know, because if I push my fatigue side or any of my fatigue, it’s going to fatigue my brain, which literally just drags everything out and makes it so much harder to recover when I get that, you know, neurological brain fatigue.
Mac Brand 35:44
So it’s like, you really do have to rest and listen to that side. It’s a real weird dichotomy, especially because it’s like, my left side is my non-primary side. So you know, because I’m right handed. So it’s weird to listen to the side, I almost never really cared about.
Colleen Brand 36:04
Yeah. And Mac was also, you know, far more social. And that also changes after a stroke, which is very difficult, in my opinion, for a very young person, to have these extreme social limitations.
Colleen Brand 36:25
At a time in life when you actually are at such a desire to be, you know, out and about and where things are happening. And that’s no longer tolerable or enjoyable.
Mac Brand 36:44
Once I kind of was ready to get out and about COVID hit and that was a prime too it was like, literally once I was like, you know, done with my outpatient rehab and was kind of seeing people again, it was like, okay, and now we got the mystery disease. Okay, cool it’s a weird one.
Bill Gasiamis 37:06
I remember feeling the same. When COVID hit for me, it was like eight years after the first time I ended up in hospital, it was 8 years. So it still felt like I was in the same kind of fog, as I was back then it used to go, Well, you couldn’t go anywhere, you couldn’t see anybody.
Bill Gasiamis 37:29
You couldn’t go and eat out, you couldn’t do anything. It felt exactly like it did when I had the stroke, and was isolated for quite some time and couldn’t get out and about and I needed to go through this thing to recover, etc.
Bill Gasiamis 37:44
But then I got annoyed being out and about because the overwhelm from noises from all the things that were happening from sometimes even the the sun and looking at, like there was a lot of overwhelm of my brain. Is that what you also experienced? Did you have that kind of neurological overwhelm? And you couldn’t cope?
Mac Brand 38:08
Yeah, I definitely, especially like, before I learned, you know, skills, and learn more about myself, like with my memory and ways to help with just like, essentially, like scheduling and keeping track of things like, I felt overwhelmed.
Mac Brand 38:30
All that like, almost all the time, like, you know, I go outside and then I go be overwhelmed. And just by I remember, the snow was a big deal, because I lived in Colorado at the time, too, because I wanted to be close to answering the doctors who perform the surgeries on me.
Mac Brand 38:47
But yeah, I remember being like, you know, the snow is so bright and everywhere you look is so bright, and it would be just hard to just sit there and kind of like, look at my own feet and just like be afraid of ice and lurching around is all one of those things that was very overwhelming.
Colleen Brand 39:03
Mack wanted to go on what I was calling a memory towards thinking that that was going to be this miracle. As soon as she saw these places from his past, things would click or people.
Colleen Brand 39:20
And so we went to Michigan where he had spent a lot of time as a child. We had a summer place up there. And we went up there and it was very disappointing for him because memories were not coming back.
Colleen Brand 39:39
And then the same thing in San Francisco, where we had moved when he was 12. He lost his dad passed from a heart attack when he was 12. And so we moved from DC to San Francisco just for a change and so he was hoping that go into these places would spark instantly a memory.
Colleen Brand 40:03
And they didn’t and that was something that it took the wind out of his sails a little bit. And it may with other stroke victims as well, where you’re thinking, Oh, when I see these things that were in my past, it will click.
Colleen Brand 40:22
And then it doesn’t. And that to me is like another. There’s a lot of things I feel people that have had experienced strokes have to say goodbye to. And I think that’s something that needs to be understood and felt on their journey.
Bill Gasiamis 40:48
Yeah, there’s a lot of loss. There’s a lot of grieving. And people struggle with it, because it’s happening at the same time as their recovery. And the recovery is really difficult and really hard. And they are physically exhausted and they’re emotionally exhausted.
Bill Gasiamis 41:06
And then they’re grieving this loss of their previous life, or their previous limbs or whatever it is that they’ve lost, and they’re trying to get it back. And it’s really hard. Did you relate to that Mac? Is grief, something that you experienced?
Mac Brand 41:23
Oh, yeah, absolutely. I, because I thought it was kind of going to be easy, honestly, like, you know, like, things would kind of click, and I had the story of my life down. But it was one of those things where it was like, I didn’t really have the memories in my head, but it was like, okay, like, this is, this is who I was.
Mac Brand 41:46
So I really did have, and you know, I can get back to this. So it was one of those things where it was like, things are going to be different now forever. So when I kind of had to do that I did go through, I approach that as a typical grieving process.
Mac Brand 42:00
And so when you lose someone, so I essentially pretend to be, you know, this guy that I knew, and, you know, basically, love that I wanted to be is no longer here. So you kind of have to bury it and be like, Okay, this is new. Now. I’m new, this is fine. So there was a big, coming to terms and it felt like a literal grieving process for bypass.
Seven Stages of Grief
Bill Gasiamis 42:29
Yes the seven stages of grief, are shock and denial. Pain and guilt, anger and bargaining. If I just get this back, you know, it’ll be okay. Depression, any of that stuff? Did you get?
Mac Brand 42:50
I definitely went through all like, you know, the whole rounds of it. For sure. Definitely. I know, I experienced generalized depression, especially like one year, and general a lot of generalized anxiety to just kind of being that it was new, but yeah, a lot of depression.
Mac Brand 43:11
With it being, you know, essentially, saying goodbye to that person. And the fact that it wasn’t going to be easy, you know, that was a hard thing was things are kind of, you know, when I had my, all my other surgeries, you know, easy, whatever, you know, this was one of the things where I was like, this is never going to be easy, like, you know, ever.
Bill Gasiamis 43:37
But what does it taught you about yourself?
Mac Brand 43:39
Oh, I mean, it taught me everything. It taught me, you know, essentially, it gave me a really fundamental understanding of life with just that we assign meaning, we create meaning in our life, my ultimate understanding is that life is essentially meaningless.
Mac Brand 44:05
Unless if you create it, unless, where you create it, you know, and I just want to kind of, I kind of looked at as just, the only thing I can do is just try to make things better, if not for me than other people, just wherever I can.
Mac Brand 44:22
You know, I wanted to just perceive the world as what I can put into it, and not what I want to put into it, but literally just measuring physical positive impacts that I can do to just make things better, I guess.
Bill Gasiamis 44:39
In the stages of grief, right? That’s called the upward turn what you just described. Is stage five, right. So you’re heading up. And then the next stage is reconstruction and working through.
Bill Gasiamis 44:52
And then the next stage is acceptance and hope. I mean, you can see you’ve gone through all of that and you’re at that upward turn and now you’re looking out for ways to support other people, you’re reconstructing everything your life, you’ve got back to studies.
Bill Gasiamis 45:07
And now there’s acceptance of that. And also, you’ve got hope for the future. And you’re looking forward as to how your life’s gonna turn out. Mom has done a pretty good job with you, after losing your dad at the age of 12. Would you agree? Has she been a pretty good mom?
Mac Brand 45:26
Oh, yeah, absolutely. I mean, like, me, my brother, and my mom has been, you know, the real real unit for such a long time after the loss of our dad, it was one of those things where it was like, you know, you’re either going to learn from it and get through it, or it’s going to destroy you.
Mac Brand 45:45
And hopefully, eventually, you learnt from it. But at the end of the day, my mom has been someone who has been the most support, like, in my life that I’ve known, you know, it’s like, it’s one of those things where it’s like, I don’t think I could have gotten to where I am without that support.
Mac Brand 46:02
And honestly, like, you know, it’s like, there’s obviously very, there was very frustrating times for me, and it’s all very much a learning experience. And I’m sure it was frustrating for her too. But at the end of the day, that basis and understanding of unconditional love that there is no condition that is going to remove that support, or that basis for support is important.
Mac Brand 46:02
Colleen it sounds like you actually laid a really amazing foundation from that time when you lost your husband. It sounds like you laid a really amazing foundation and example of how to get through really difficult and tough times. How hard was it to raise two kids on your own when, when your husband passed away?
Colleen Brand 46:51
Oh, you mess up a lot. It’s very, very difficult. I never planned on being a single parent. I think most people don’t go looking to be a single parent, but boy, it gave me a lot of empathy. You can’t do it all, and you often end up doing your job and then parenting, you end up doing both not well.
Colleen Brand 47:27
And you’re just as honest as possible. Sadly, with kids that probably you’d like to not have to be that honest with them at those young ages. But basically, you have to be that honest with them to survive, because we all have to push through it.
Colleen Brand 47:53
So you’ve got to really put everything out on the table of like, you know and fortunately I had raised I have two stepsons. So I already knew what was coming down the path with teenagers. So I took that experience and it was like all that stuff that your older brothers did. You can’t do that.
Mac Brand 48:22
Yeah, especially because she’s gonna be alone.
Colleen Brand 48:25
No one’s allowed to burn down the house. We have one house if it goes we’re toast people understand. So there was a lot of that was what I mean by reality. I was like, Y’all have to learn to clip coupons and get to the grocery store. Do your laundry like they really stepped up guess what y’all just had to grow up a little fast.
Colleen Brand 48:50
So let’s go because they stepped up too we did it together is what I liked to think and it wasn’t easy. It wasn’t ideal for any of us. I mean, for God’s sake, they’re young boys. They’ve lost their father a mom can’t at least this mom, I can’t do all the jobs. You know, so I can do the best I can.
Colleen Brand 49:17
But I kept waiting for that. That Disney moment of this coach that was gonna walk in the door or this male figure that was going to happen. Just like not coming okay. But whatever there’s a lot to be grateful for in there.
Colleen Brand 49:36
Both he and his brother, they’re really good humans. They’re good people. They they got it. They had the common sense to realize that. Yeah, we can’t do a bunch of stupid stuff. because we just can’t, you know, do we can do marginally stupid what we can’t do extremely stupid.
Bill Gasiamis 50:09
I reckon Mac probably achieved doing some stupid stuff though.
Colleen Brand 50:15
Of course they do.
Mac Brand 50:17
We were growing up in the city too we’re having a lot of fun.
Bill Gasiamis 50:24
Brilliant. Brilliant. So now you’ve gone through that with your husband. And now you’re going through this thing with your son, especially in the early days. Did you think you might lose him? Did you have that fear?
Colleen Brand 50:37
Oh, no, that’s when I knew. If Mac didn’t make it. That was the first time in my life that I went. I’m not making it either. I’ve always been a person that was like, oh, no, we’re gonna find a way.
Colleen Brand 51:02
But that night, I was like, yeah, not gonna make it. Yeah, I finally found what was going to chop me off at the knees.
Bill Gasiamis 51:15
Wow, that would have been hard. I’m glad we’re not talking about it.
Colleen Brand 51:22
And again, it gives you incredible empathy for parents that have had that ultimate loss, your heart goes out to them at the deepest level.
Bill Gasiamis 51:39
It sounds like, you’re really well connected, you got a great relationship. But did it get shitty at some times after the stroke after the recovery? Mac he seems like he’s a really nice guy. But did you lose it a few times Mac? Were you terrible to be around?
Mac Brand 51:58
There was a lot especially because in the stages, like when I was in the hospital, and you know, going through that grief and going through like I wasn’t in it a place in my mind where I was as emotionally mature. Like, I don’t like to say I had the mind of a child, but I had the impulse control of a child.
Mac Brand 52:21
So there is like, my emotions were almost very new to me too you know, like swallowing and eating were you know, at the same time, so there are times where I was almost like a baby in bed, like, and I’m six foot three very grown man, and there’s a lot of times where I’m sure I was a little bit that, you know, maybe frustrated or short.
Mac Brand 52:52
And that’s a product that’s something I noticed with brain fatigue, when it happens faster, I tend to get a little bit more shorter tends to be a little bit more of a problem with my increased anxiety and lack of like, kind of control and just kind of like, you know, stuff like that.
Mac Brand 53:11
But yeah, definitely, it was all a learning experience. It’s all just like, you know, I’m sure I wasn’t a peach in bed. But I remember you know, in the hospital, but I do remember times when I was intubated.
Mac Brand 53:27
This is gonna sound really strange. But when I was intubated and I had the oven mitt on, I thought that I was going to be able to escape the hospital somehow. Coz I thought I could walk like my car was in the parking lot that I could just drive away.
Mac Brand 53:48
So I was being really nice to the nurses trying to I guess, trick them and getting me to like leave the hospital it just totally a strange thinking. So I would like pat them on the back and stuff.
Mac Brand 54:02
When I was intubated like to say thank you and things like that. It was very, funny. But the nurses really liked me because I was very nice. But at the same time, I was like I’m going to escape with their help.
What Caregivers Have To Deal With
Colleen Brand 54:19
I am a very fortunate person that I have another partner his name’s Alex. So I was so fortunate to have had love twice. And he has also been a great stepfather to both Mac and Bo we’re so fortunate to have him in our lives to help tremendously. So we’re very lucky that you know, we have him as well.
Colleen Brand 55:05
Which is, yeah, it’s a tremendous help because that male influence is really needed. My, my voice is not always the best one to hear and it’s also, um a safe place for Mac to vent. And I want to be that safe place for him to vent.
Colleen Brand 55:28
And that’s a good thing, you know, that if you’re gonna get upset at your situation or something, get upset with me, you know, because I get it, I know where that’s coming from. That’s not personal.
Bill Gasiamis 55:42
Yeah. That’s such a good thing that you’ve got there Colleen because my wife, she a little bit of abuse, you know, verbal abuse, because I was a mess. And I didn’t know what I was doing. And I was misbehaving.
Bill Gasiamis 55:59
And at the same time, I couldn’t explain myself because they could see me, but then I looked normal, but then I couldn’t explain how I was feeling on the inside. And they didn’t get it.
Bill Gasiamis 56:13
And then she took it personally, because I’d never really gone out of my way to mistreat her like that, of course, we mistreated each other from times in our marriage, but I never gone out of my way to do it.
Bill Gasiamis 56:26
Whereas I was now getting triggered by the smallest thing like parking in the wrong car space, or something like that would trigger me. Go nuts. And she, she used to take it personally.
Bill Gasiamis 56:40
And then to undo that, for me, it was really, really difficult because of course, I appreciated her. She was my everything. And I loved the fact that I was supported by her. But then I was also the guy giving her a real hard time.
Bill Gasiamis 56:57
And then I was trying to undo the pain and suffering that I’d caused her on top of all the other pain and suffering she’s already going through. It was such a difficult time. I mean, the only thing I could do was try and get somebody to intervene for me.
Bill Gasiamis 57:13
So I went to counseling, and I took her with me to counseling a few times, just so I could get somebody else to kind of explain things on my behalf or to try and make her feel better about things. Because I didn’t know what I was doing.
Colleen Brand 57:29
I can only begin to imagine how much frustration Mac had to be going through. And you’ve got I call it kick the dog, you’ve got to be able to kick the dog somewhere. And totally fine having it come towards me because I know exactly what that is.
Colleen Brand 57:58
And I can I know exactly where that’s coming from. And you got to get that out. You can’t. Keeping that in is the worst thing you can do. You got to get it out you’ve got to let those explosions come out.
Colleen Brand 58:16
And you can’t keep suppressing everything for God’s sake, look at what you’re going through. You know, you are really like a baby relearning everything. And how many times is a baby cry?
Colleen Brand 58:30
You know, so it was very easy for me to put it in that category of well, there’s Mac at 2 my God, that two year old Mac was a nightmare. I mean, I can’t tell you but then I could pick him up and leave. You know, with him screaming.
Bill Gasiamis 58:48
At six foot three.
Mac Brand 58:54
My time in the hospital being a very big guy, and you just can’t even really fit in the bed and they’d have to bring the one bigger guy from upstairs to come and carry me around to the bathroom or whatever.
Bill Gasiamis 59:08
That’s another logistical thing that you don’t experience as a What will people under six foot you know, everything’s kind of made for people under six foot roughly. Above that, it’s a bit harder.
Mac Brand 59:21
Yeah, that was that was interesting. I’m so lucky that you know, I did end up at the Ann Shultz hospital because that was such a great place. Like, you know, all the people there were so awesome.
Colleen Brand 59:36
They were all just, I mean, they were really like what you see out of a movie, you know of a hospital movie.
Colleen Brand 59:44
All the good stuff.
Mac Brand 59:48
It’s a teaching hospital, so they all look good too. And they’re all your young.
Colleen Brand 59:53
The doctor that saved him. He had just gotten to that hospital. He had been a Navy SEAL bomb diver gentleman then went to neurology school and then you know became this great brains surgeon I mean, just you have these people of the highest caliber in their skill set and in their moral character. And they were incredibly uplifting to be around also, I can’t say enough about just how noble these people are. They’re truly incredible heroes.
Bill Gasiamis 1:00:38
I appreciate my doctors, too. I mean, I can’t believe there’s people out there that just decide that they’re going to do a job that helps other people to the extent that we get our help. It’s like, it’s just nuts. It never occurred to me. So I assumed that there weren’t other people out there.
Bill Gasiamis 1:00:57
But they really are. And many of us wouldn’t be here without them. You’re really creative. Colleen, I saw a post of yours on Instagram. And I thought, oh my gosh, I need to speak to these people. I need to speak to you immediately and have you on the podcast.
Kintsugi Mac Brand
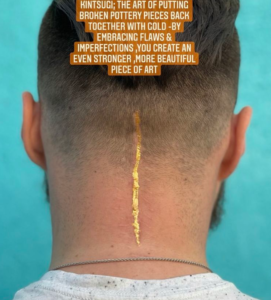
Bill Gasiamis 1:01:14
And it was the post where you’ve got a photo of Mac’s head. And it’s the scar down the back of his head towards his neck, the middle of his head. And you’ve put the gold leaf on the back of that. Tell me a little bit about what inspired you to upgrade his scar to gold?
Colleen Brand 1:01:36
Gosh, that is Mac you have to look up what that is. I always forget what it’s called. Thank you. Thank you that is Kintsugi which is to me that is perfect. I wish that everybody that has a scar that wanted to have it embedded with gold that we could do that. Because that to me perfectly explains the scars.
Mac Brand 1:02:07
I really like my scars. Honestly, I think they’re cool. The back of my head was awesome.
Colleen Brand 1:02:13
Yeah, that, to me is everything. And that’s your new journey. And you know, let it be filled with gold, it be that the perfect imperfection that it is and defining that new journey in in such a beautiful way that it is repaired with these precious materials.
Colleen Brand 1:02:42
And then I just thought that was the perfect, metaphor for that the scars that one has from these life altering experiences.
Bill Gasiamis 1:02:55
It really is the perfect metaphor. I saw that and exactly knew about I know about Kintsugi a lot of stroke survivors actually know about Kintsugi. But to see that done the way that you did, it was just phenomenal.
Bill Gasiamis 1:03:10
And hopefully what I can get from you is the photo. So I can include it in the episode so I can show people what we’re talking about. Mac, I love my scar as well. The problem is that it’s disappearing, and I can brag about it. It’s getting better, and it’s getting covered by hair so you can barely see it. It’s pretty cool. You tell me about how you like to show off your scar.
Mac Brand 1:03:37
Oh, I mean, I literally just cut all my hair off because I’m regrowing. But I got the one. I mean, this is where they put one of the drain tubes right here, I liked that one.
Colleen Brand 1:03:52
Yeah. It had to be redone. Yeah, that was cool.
Mac Brand 1:03:57
And then my back was the crazy one, which I noticed is like, I don’t know if they’ll ever really how that one. I don’t know if that one’s ever gonna really run away. really toned down. I feel like that one’s intense.
Bill Gasiamis 1:04:10
They settle down they do and disappointingly more importantly, Yeah, mine was about the same as yours is now for a few years and then it kind of got flatter and flatter and better and better.
Bill Gasiamis 1:04:24
And now other people can see it when I shave because I usually keep my head quite short as well. And other people see it and they can tell yeah, like I can’t feel it anymore. It’s gone. And it’s a bit annoying.
Bill Gasiamis 1:04:44
I was the same I’m not sure what it is about it but I was quite excited by the fact that it was visible and that I was never afraid for people to see it and wonder and ask me about it was all good.
Colleen Brand 1:04:57
These are your battle wounds.
Mac Brand 1:05:01
Other people like with the same scar will be like, Hey, I got to and take off their hat and show me it’s always really, it’s really funny like with that scar in particular, I feel like people are like, Oh, I like that.
Bill Gasiamis 1:05:12
It’s a community. I agree with Colleen as well. That it’s our battle scars, it just shows. We’ve been through life. You know, that’s what’s happening to us. It’s we’re living it, we’re experiencing life.
Colleen Brand 1:05:29
Yeah, it’s so great that I’m so grateful that we’re getting to talk to you. Because we do need to share these stories. And we do need to help people that have had strokes, how that you know, this community to move forward and to have more information and to share the stories and then for people to understand prevention and then if you have want to be empowered with the knowledge of what to do, where you have to get to.
Bill Gasiamis 1:06:11
Yeah, and that there’s a brighter side. Think about it, you know, Mac went through a hard time four years ago. Now he’s getting better. We’ve, we’ve turned the corner, you know, we’ve done shock and denial, we’ve done pain and guilt, we’ve done anger and bargaining, we’ve done depression.
Bill Gasiamis 1:06:26
And we might go back there from time to time as well. And that’s okay, too, right. And now we’re at the upward turn and reconstruction is happening and acceptance in the hope is coming, and it’s happening.
Bill Gasiamis 1:06:38
So this is what I love about the podcast is I get to share the it was really shit at the beginning. And now look how we’re moving forward. And we’re overcoming stuff, problems, challenges.
Mac Brand 1:06:48
You know, I wouldn’t give it up for anything, honestly. Like, I like, my stroke, and you know, so it’s a part of me, same with my dad passing when I was young, they’re all things that, you know, have taught me more at the end of the day and made me stronger.
Bill Gasiamis 1:07:12
Yeah. Mac, your mum sent me a PDF of I no longer dream. Oh, yeah. Tell me about putting your thoughts into words? How does that help your recovery? And why was it important to do that?
Mac Brand 1:07:31
Well, that was kind of like cathartic writing with, I wanted it to be similar to kind of the Dante’s trilogy, where you start out in the inferno purgatorio and paradisumo. By starting off, in trying to describe all the confusion, and coming into being and being, you know, not really understanding what’s happening.
Mac Brand 1:08:03
There was a long period, I know, you know, six months after, where I was kind of like, just, you know, maybe going to outpatient rehab, and just kind of floating and not really feeling like myself, or having really any grounding to the world around me. And then it’s like, you know, I come out here.
Mac Brand 1:08:20
And finally, it’s like, I feel like I have grounding. Like, it’s kind of one of those things where it felt good to write down a journey, you know, and bring it to a point where, like, even if things aren’t perfect, there never will be, Nothing’s ever perfect, it’s fine. You know, everything is what you make. And at the end of the day, it’s like, everything’s better.
Bill Gasiamis 1:08:46
Are you hoping to do more with it at this stage? Or is it just for you.
Mac Brand 1:08:51
I have it sent to like an editor right now. So I have someone editing it, maybe I’ll send it out to see if someone will publish it or something. If not, I might just make it a book and sit on my shelf one day and look through it, I just, I’m always kind of fearful that my plateau so to speak, will end earlier.
Mac Brand 1:09:21
Which I don’t think it will. But it’s kind of one of those fears in the back of my head. So I always want to have these things like writings and you know, art and stuff like that, that kind of remind me of those periods of my life. So I don’t feel like if I do forget it ever, I can always go back and look at these things that I’ve done and be like, Okay, this is where I was, you know, and this is what I was doing.
Mac Brand 1:09:43
So that’s kind of where I’m at with it where it’s like, if it doesn’t become something that’s fine, It’s something to me, and that’s all that matters. And if it does, and if it helps someone or someone finds value in it, that’s fantastic too.
Bill Gasiamis 1:09:56
Yeah, that’s perfect.
The Intubated State
Colleen Brand 1:09:59
When I had one person read it, who works with a lot of people in Walter Reed, and what she liked about it was that, we really don’t understand the perspective of someone that is in a state of intubation.
Colleen Brand 1:10:21
And that they do have awareness? And what is that awareness. So she really liked it as having an awareness of what somebody is going through that is in that state of intubation.
Colleen Brand 1:10:42
Because it is an unknown, and we’re assuming that, oh, there’s nothing but there’s very much going on. And perhaps the experience could be different for the patient, perhaps we could dim the lights, perhaps we could bring in soothing music, perhaps we could be a little bit more gentle and comforting.
Colleen Brand 1:11:05
Perhaps we could perform Reiki perhaps, you know, some other types of things to to soothe the soul and spirit in a more gentle way. Because it’s so horribly clinical, we think that there’s nothing going on there.
Colleen Brand 1:11:22
And that’s wrong. There is much going on. And I think that if some more holistic things could be come in, or even an awareness of Dimming the lights, and what can be experienced. That was what she brought in. And I was like, that is lovely, and very important. That does have value.
Bill Gasiamis 1:11:47
I completely agree with you guys. Absolutely. Look. Thank you so much for agreeing to be on the podcast when I reached out. Mac, thanks so much for sharing your story in the way that you have.
Bill Gasiamis 1:12:01
You guys are doing great, you guys are doing an amazing job of, you know, getting back to life and recovering from trauma and from overcoming your pain and your suffering. And it’s a great example. And I’m glad that we get to share that with other people and just give them a sense of how some other people like you guys are doing it.
Bill Gasiamis 1:12:24
And then there’s 180 or so other episodes where it’s exactly that’s what we’ve done. We’ve given examples of how other people have gone through their own recovery. And it’s not all been pretty, you know, there’s been shitty times and terrible times and hard times.
Bill Gasiamis 1:12:43
But a lot of people are seeming to find the way through the fog and get better at living their life the way that they intended to live their life before stroke happened to them. So really appreciate you guys sharing your story.
Mac Brand 1:13:02
Thank you so much for talking to us.
Colleen Brand 1:13:05
Thank you. It’s nice to not be alone. That’s for sure.
Bill Gasiamis 1:13:10
Yeah, by all means you’re definitely not alone. Mac if you ever need to reach out, please feel free to Instagram is full of people that are recovering from stroke. Hashtag stroke survivor is huge. There’s so many amazing people there. And they’re all willing to share.
Bill Gasiamis 1:13:27
They’re all willing to help others, which is bizarre, strange and amazing to me at all at the same time. So and you guys fit the bill, you guys are exactly the same as them. You know, you want to connect with people.
Bill Gasiamis 1:13:39
You want to feel less alone and you want to share and help others, man, I can’t ask for more from my guests on the podcast. That’s exactly what I want to do. So thank you for helping me do that as well.
Colleen Brand 1:13:55
Thank you so much. We appreciate you.
Bill Gasiamis 1:13:58
Thanks for joining us on today’s episode. I hope you enjoyed the conversation and got something positive from it. Please comment, like and share. If you’re watching on YouTube. Click the like button, leave a comment, subscribe. Tap the notification bell so that you can get notified of new episodes as they become available.
Bill Gasiamis 1:14:18
And just let me know what you’re thinking. I look forward to people’s comments and I love responding to them. And it will also help each episode rank better. And therefore it will make it easier for other stroke survivors to find the episodes and maybe that will help them have a better stroke recovery. Thanks again.
Intro 1:14:36
Importantly, we present many podcasts designed to give you an insight and understanding into the experiences of other individuals. The opinions and treatment protocols discussed during any podcast are the individual’s own experience and we do not necessarily share the same opinion nor do we recommend any treatment protocol discussed.
Intro 1:14:53
All content on this website at any length blog, podcast or video material control this website or content is created didn’t produce for informational purposes only and is largely based on the personal experience of Bill Gasiamis.
Intro 1:15:06
The content is intended to complement your medical treatment and support healing. It is not intended to be a substitute for professional medical advice and should not be relied on as health advice.
Intro 1:15:15
The information is general and may not be suitable for your personal injuries, circumstances or health objectives. Do not use our content as a standalone resource to diagnose treat, cure or prevent any disease for therapeutic purposes or as a substitute for the advice of a health professional.
Intro 1:15:30
Never delay seeking advice or disregard the advice of a medical professional your doctor or your rehabilitation program based on our content if you have any questions or concerns about your health or medical condition, please seek guidance from a doctor or other medical professional.
Intro 1:15:44
If you are experiencing a health emergency or think you might be, call 000 if in Australia or your local emergency number immediately for emergency assistance or go to the nearest hospital emergency department.
Intro 1:15:55
Medical information changes constantly. While we aim to provide current quality information in our content. We did not provide any guarantees and assume no legal liability or responsibility for the accuracy, currency or completeness of the content.
Intro 1:16:08
If you choose to rely on any information within our content, you do so solely at your own risk. We are careful with links we provide however third party links from our website are followed at your own risk and we are not responsible for any information you find there.







