Bryan Caldwell was 34 and seemingly healthy and well until high blood pressure caused a stroke that would allow doctors to also discover that he had total kidney failure.
Highlights:
01:55 Introduction
02:52 High Blood Pressure & Stroke
13:56 Initial Deficits
16:27 Make Your Own Destiny
18:44 Pseudobulbar Affect (PBA)
24:32 Stepping Up As A Caregiver
31:25 Diet After A Kidney Failure
37:58 Second Chances
49:47 Reaching Out
57:45 Parenting At a Young Age
Transcription:
Bryan Caldwell 0:00
You know, I’m not going to accept what I’ve been handed. Like, these aren’t the cards I’ve been dealt. You know, it’s it’s basically like, almost like fate or my own destiny, I need to figure out my own destiny if I want to be successful in whatever it’s going to be then I need to do it. I don’t need to give myself excuses.
Intro 0:24
This is the recovery after stroke podcast, with Bill Gasiamis, helping you navigate recovery after stroke.
Bill Gasiamis 0:37
Hello, and welcome to another episode of the Recovery After Stroke Podcast. I’m Bill Gasiamis. And recently, Spotify released a new feature that allows people to now rate their favorite shows similarly, or in a similar way to the way the apple podcast app allows it.
Bill Gasiamis 0:54
So even if you’re not somebody who uses Spotify to listen to your music or your podcasts, if you do go across to Spotify, you can leave the show a five-star review just go to Spotify search for recovery after stroke, the podcast will come up and then you can leave, hopefully, a five star review if you think the show deserves it.
Bill Gasiamis 1:15
Now, this has been happening more and more in the last few months as I’ve been asking people to do it. And I’m noticing that the number of downloads per month is starting to increase.
Bill Gasiamis 1:25
The show has surpassed 5000 downloads a month. And that is an amazing, amazing thing. Considering that when it first started, it was lucky to get maybe three or four downloads a week.
Bill Gasiamis 1:39
So please feel free to go across to your favorite podcast app. Even if it’s not the Spotify one, leave the show review. Tell people what you think of it. It’ll help the podcast rank higher and it’ll help the podcast be found by more stroke survivors and their caregivers.
Introduction

Bill Gasiamis 1:55
And hopefully, it’ll make their life a little easier and feel less alone. So I’d really appreciate if you did that now. Today’s episode is episode 189. And my guest today is Brian Caldwell, who at the age of 35 is right now currently recovering from a hemorrhagic and ischemic stroke as well as total kidney failure.
Bill Gasiamis 2:20
Likely the symptoms of undiagnosed high blood pressure. Also joining us was Brian’s partner Brittany, who had to step in to being a caregiver as well as a mum. And despite all of their challenges, these two are super positive.
Bill Gasiamis 2:36
They’re a delight to interview and I had such an amazing time getting to know them a little. I hope you enjoy this episode. Brian Caldwell, welcome to the podcast.
Bryan Caldwell 2:46
Thanks for having me.
Bill Gasiamis 2:47
Pleasure, man. Thanks for being here. Tell me a little bit about what happened.
High Blood Pressure & Stroke
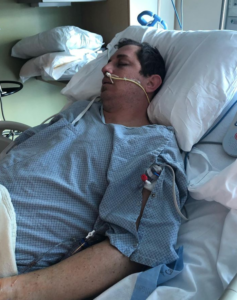
Bryan Caldwell 2:52
Well, let’s see how it started out. I have no symptoms. I had some cramps in my leg. But I had a feeling it was from like low potassium or something like that. So I was taking a potassium supplement but it wasn’t doing anything, I kept having cramps.
Bryan Caldwell 3:12
So that’s the only symptom I had. So one day, I was having a Zoom meeting like we’re having for a new job I was about to start. And basically my wife was on the stairs right next to where I was having a Zoom meeting like we are on the computer here.
Bryan Caldwell 3:30
And I was just sitting there and I basically got the job and she was being nosy listening on the stairs saying, okay, babe did you get it? and I yelled babe and then as I said babe, put my head down, passed out, and that was it.
Bryan Caldwell 3:47
And then I remember bits and pieces. Like, I wasn’t completely incoherent, except for like the last three weeks that as I passed out beyond that, but she basically kind of stepped in, learned all about stroke, and it was caused by high blood pressure of my diabetes. And then I don’t know if you want to jump in and kind of tell him most of the story here.
Bill Gasiamis 4:12
Hey, who’s that?
Bryan Caldwell 4:15
This is Brittany.
Bill Gasiamis 4:16
Hi, Brittany, how are you? Come a bit closer.
Brittany 4:19
He’s taken up the whole screen.
Bill Gasiamis 4:22
Yeah. Shove over Bryan.
Brittany 4:24
Yeah. So when we had gone to the hospital, he actually had a bleed in his brain in his brainstem. And he was transported to the nearby stroke center. And they told me basically, how long have you known that his kidneys weren’t functioning?
Brittany 4:42
I was like, I have no idea. And they said we can’t even push contrast through because his kidneys aren’t working at all. And so I was like, Huh, well, that’s news to me. So they were on with and neurologists down in Salt Lake City, which is the main city and Utah, and they have a specialized neurology center over there.
Brittany 5:04
And so they wanted him to get transferred. So it took him about two hours to get transferred down to Salt Lake. And by the time he got over there, he was totally out of it. He was like, slurring his words. So it was like the stroke was progressing.
Brittany 5:21
He had more like drooping on his left side. And then at that point I had walked in because I thought, okay, he’s gonna go from one hospital to the next. They’re just going to, you know, do workup, see what they can do for him.
Brittany 5:34
But by the time I got there, they said, Hey, we need to intubate him, like, he can’t swallow. He’s not, you know, projecting his airway. So we need to do what we can. So I said, okay, like, is he gonna make it out of this, like, what’s gonna happen?
Brittany 5:49
And they said, We don’t know. We can’t give you any definite answer. And I’m like, okay. So they basically pushed me out, of course, it’s healthcare. So they, you know, come to me, they want my card, they want my information.
Brittany 6:00
So they want to make sure I can pay. And I actually called my boss who has a large family of doctors. And I said, Hey, this is the situation. This is what’s going on. And so he got his sister on the phone, who owns her own Medical Clinic in Arizona.
Brittany 6:18
And she was like, ask them how big the bleed was. Ask them what kind of stroke it was, what it was caused from. So I basically have went right upstairs. And I was like, are you the nurse? Yes. And I said, Okay, how big was the bleed?
Brittany 6:31
And she’s like, looking at me, and so she goes, well, it was only a couple millimeters. And I said, Okay, well, what kind of stroke was it? And so she said, Well, it’s a pontine hemorrhage, but we’re still trying to decide specifically what it is.
Brittany 6:44
Because they were trying to say it was a I think caucus malformation, which they said could be something that he’s had since he was very little.
Bill Gasiamis 6:53
A cavernous malformation?
Brittany 6:55
That one, yeah, cavernous malformation. So it was either that or he had, what it more so seemed like over time, when we were kind of figuring things out was that he had a lot of clots in his body from kidney failure, which he could have had the clot in his brainstem for a period of time.
Brittany 7:17
And then his kidneys weren’t functioning. So obviously, the blood pressure wasn’t functioning as well, which caused essentially the clot to rupture in his brain and caused the bleed in his brainstem. So that’s kind of the roundabout of what happened initially.
Bill Gasiamis 7:37
Wow, that’s crazy. Bryan, did you know you had high blood pressure? First question.
Bryan Caldwell 7:44
I had been diagnosed years ago, but it was never like an ongoing issue. Like I was never fully diagnosed with hypertension.
Bill Gasiamis 7:53
Okay, so no medication.
Bryan Caldwell 7:55
I was taking some medication, but was unaware that I was supposed to take it consistently.
Bill Gasiamis 8:03
Okay, and then second question is, you had no idea you had kidney failure. And is that common is that what happens?
Bryan Caldwell 8:11
It’s not very common, but I didn’t have very, in my younger years, I wasn’t very controlled. Like, my blood sugar was out of control. My eating habits were out of control.
Bryan Caldwell 8:23
My exercise was off and on. I was fairly active. I mean, I played hockey. I was the coach of my son’s hockey team, right before I had my stroke. So I was active, but I wasn’t very consistent as I should have been. Now it’s different. You know, with my stroke, it’s like, you know, it’s a wake up call. I’m very active just about every day now.
Bill Gasiamis 8:47
But were you really, really bad? Or are you just a regular person because nobody’s perfect with their diet. Nobody avoids, you know, sugary drinks. Nobody avoids fast food. Most people do all that kind of stuff. Were you like out of control with that stuff? Or were you just a regular guy?
Bryan Caldwell 9:08
I’d say when I was younger, I was probably more out of control. I’d say between the ages of 18 and 25. I was basically an alcoholic with my friends basically just love to have a good time with my friends.
Bryan Caldwell 9:21
So I think that’s what caused my high blood pressure and then as undiagnosed over the years and basically when I got older is when it kind of, you know kicked my body’s butt.
Bill Gasiamis 9:32
Yeah, right. Okay, so what’s it like Brittany when somebody’s talking one second, they’ve just got the job and then they pass out? What happened to you like, how did you cope with it?
Brittany 9:46
So I was being the nosy person that I am. I was kind of right beside him right up the stairs because I wanted to know what happened. We talk about it all the time. It’s like the perfect storm. Everything happened in a perfect way.
Brittany 10:05
And I still almost don’t believe it because he wanted to go to the desert that weekend. And he was supposed to be driving home that day. And I told him no, like, you know, you need to get a job. He needs to do this. Like then he called me a penny pincher or something.
Brittany 10:22
And I said, You’re lucky I’m a penny pincher, I saved your life. Like you could have been on the road in the middle of nowhere and have your stroke. And then I usually at that time, I was on calls back to back to back at work, and I would shut my office door, put my headphones on and not hear anything that was going on.
Brittany 10:40
So when he was on the phone, it was like that 30-minute break of me not being on meetings. And he yelled, and I thought, okay, maybe he just wants to tell me you know what happened, how it went.
Brittany 10:52
And then I said, what? And then he didn’t answer. So I was like, okay, whatever. So I went downstairs and he had like, his head slumped over on the desk. And he was like, kind of like slouching over his whole left side, couldn’t move.
Brittany 11:06
And I was just like, what’s going on? And he was like, Call 911, Call 911. That’s the only thing he could get out. So to me, I’m sitting on the phone with 911. They’re asking me about his blood sugar. I’m like, It’s not his blood sugar. He’s not high. He’s not low. Like he’s having signs of a stroke.
Brittany 11:22
And I would hope that’s not what it is. But I’m pretty sure that’s what it is. And so when the ambulance came, the fire department, the sheriff, they all looked at him and they were like, he’s too young, he’s not having a stroke.
Brittany 11:35
And so he actually thought his sugar was going low. So he was chugging Snapple. And when he was chugging Snapple, it ended up that his sugar when the paramedics got here, his sugar with well over 500, so he wasn’t low.
Bryan Caldwell 11:53
Sugary drinks check.
Brittany 11:56
But then on top of that, his blood pressure was like around 230, 240.
Bill Gasiamis 12:01
Wow.
Brittany 12:01
So it was just like all at once. And then they basically took them out, they took them over to the hospital. And it was kind of like this instant shock what is going on, it happens to be the day where our son was home from school on top of that.
Brittany 12:17
So I’m trying to round up a dog and a seven-year-old, I’m trying to tell him to go upstairs because I didn’t want him to see what was going on. But I couldn’t really control that make sure he didn’t fall over and hit his face or injure or anything else.
Brittany 12:28
So I had to let things kind of play out. And then at that point, it’s like, how do you explain to a seven-year-old that, hey, he left, he’s in the hospital, and he’s gonna be there for a little while.
Brittany 12:39
So it was definitely tough. Like, I didn’t have time to clean the floors, because he when he had the stroke, it affected his swallowing. So he stopped swallowing. So all he was doing was drooling everywhere.
Brittany 12:55
And of course it was Snapple drool so it smelled like Snapple every time I walked in the house, and it was like, I would just look at that area where he was sitting. It’s like, it’s just a bad dream.
Brittany 13:06
I’m just gonna wake up from it like this isn’t happening. And then it was like, every day, it was the same thing over and over and over because he was in the hospital for almost three months.
Bill Gasiamis 13:15
Traumatic.
Brittany 13:17
Yeah, definitely.
Bill Gasiamis 13:19
What happens, Brian? You go to hospital, you get told all these things went wrong with you? What are you thinking, man?
Bryan Caldwell 13:27
At that point, I don’t even think I control of my thoughts. I was so incoherent for a good three weeks. And I was doing hemo dialysis, which is, you know, my different levels were so out of control that they’re trying to get my toxicity back under control.
Bryan Caldwell 13:44
And you know, different levels are throwing my brain off. And I can’t think clearly. So I’m basically just sitting there, letting them do whatever they want to do and just going with the flow.
Initial Deficits After High Blood Pressure & Stroke

Bill Gasiamis 13:55
Wow. And then when they stabilized your kidneys and the dialysis started to work and all that kind of stuff, then did you have some deficits on your left side that you had to deal with and recover from what were they?
Bryan Caldwell 14:12
Oh, definitely, I had my full left side paralysis all the way down to my leg. But luckily, within a few days, Brittany was stretching my leg pretty often. And that actually helped a lot. So my leg function came back pretty I mean, took a few weeks of rehab to get it back.
Bryan Caldwell 14:34
But my arm was completely useless. But, you know, months go by and I’ve got some movement and you know, I’m able to still do some things like it’s fairly functionable just can’t like grip some things and you know, I have full function, full mobility, but I’m working on that the strength and stuff like that to try and get it back every day.
Bill Gasiamis 14:56
You were 34 when it happened. So, how old are you now?
Bryan Caldwell 15:03
35.
Bill Gasiamis 15:04
Okay, so it was not not that long ago was any 12 or so months ago?
Bryan Caldwell 15:08
Just last February.
Bill Gasiamis 15:11
Wow. So it’s pretty short amount of time. So you’ve gone from being relatively healthy feeling, okay, really capable of going out to the desert, do whatever you’re going to do there.
Bill Gasiamis 15:22
Up until that day and then you’re this completely different person from that day on, you’ve got the job. Clearly you didn’t go back to work. Brittany’s nagging didn’t get you back to work it got you a job but not back to work.
Bryan Caldwell 15:39
I call her my sugar mama now.
Bill Gasiamis 15:41
You’re living off her the good life, right?
Bryan Caldwell 15:45
I would say pretty close.
Bill Gasiamis 15:46
I know. You’re lucky boy. I did the same thing right? I lived off my wife for quite a few years, on and off. And it was interesting and challenging and confronting and difficult. What’s it been like for you to kind of be unable to get back to some of the things that you were doing before stroke?
Bryan Caldwell 16:14
So as I got out or back home to kind of recovering. Within the first month I was kind of focused on like, you know, when’s the depression going to kick in because I keep hearing about depression.
Make Your Own Destiny
Bryan Caldwell 16:27
And I watched a movie in the hospital called seven yards. It’s on Netflix. And it’s about a paraplegic. He, becomes paraplegic when he’s 19, I think, from a bad football hit. And, you know, I see that he’s got a much worse life than I do, you know, not being able to move anything.
Bryan Caldwell 16:47
So his goal was to walk seven yards down the aisle to get married. And that kind of gave me a motivation. Like, you know, I’m not going to accept what I’ve been handed. Like, these aren’t the cards I’ve been dealt.
Bryan Caldwell 17:01
You know, it’s basically almost like fate or my own destiny. I need to figure out my own destiny. If I want to be successful in whatever it’s going to be, then I need to do it. I don’t need to give myself excuses.
Bill Gasiamis 17:17
Wow. And are you driving?
Bryan Caldwell 17:21
Yeah, I started driving. Oh, my wife’s gone. Sorry, I started driving, I think November.
Bill Gasiamis 17:28
Okay. So that came back relatively quickly, they gave you permission to drive or you started driving?
Bryan Caldwell 17:36
Yeah, the funny thing was, I failed the first assessment with my occupational therapist. It basically wasn’t really my fault, it was more of a bad timing issue. Like they had canceled the appointment on me. And I was upset. And I said, You know what, I’m not gonna stand for this, like, give me another appointment as soon as possible.
Bryan Caldwell 17:56
And they were kind of upset that I did that, and basically failed me on the spot. So then I went to another lady that was nearby. And luckily, she actually grew up in my hometown in a different state.
Bryan Caldwell 18:07
So we actually got along really quick. So it was great. So at that point, I think I needed a little more time, it was like a month in between, and I probably needed that month in between just to, you know, gain a little more cognitive ability.
Bryan Caldwell 18:22
I never really lost my cognitive ability, but like, just like, you know, being able to multitask and keep my eyes open and focus on different things and notice the things around me really helped a lot with my driving. I still get nervous from time to time, but it’s a lot more easygoing than it used to be.
Pseudobulbar Affect (PBA)
Bill Gasiamis 18:44
Did it impact your emotions?
Bryan Caldwell 18:48
At first it did. But that was like a big focus of therapy at first was, you know, I had regular therapy like for my mind, so they would just, you know, console me all the time. Just reaffirm me like, Hey, you’re allowed to feel like this is what you’re going to feel like and pseudobulbar was like, played a major part, the beginning.
Bryan Caldwell 19:09
So I cried uncontrollably all the time towards everything. I mean, the littlest things. When I was sitting in my bedroom, the first I think, the first couple of days. My nurse was coming in to train my wife on dialysis. And I heard them talking about dialysis.
Bryan Caldwell 19:29
And I didn’t realize how far along I was, what stage I was in, but I had overheard, I was in stage five. And I was like, wow, that’s really hitting home. So I probably cried harder than I’ve ever cried in my life at that point.
Bryan Caldwell 19:44
And that, you know, shortly after I kind of got used to it and just can’t give myself excuses to feel bad for myself. I gotta push forward. I gotta try harder. I gotta, you know I just do things to make myself happier. So I kind of focused on my crying more. There’s times where like I wanted to cry. But I just held it in and said, Hey, you got this, just think about it a little harder.
Intro 20:15
If you’ve had a stroke, and you’re in recovery, you’ll know what a scary and confusing time it can be, you’re likely to have a lot of questions going through your mind. Like, how long will it take to recover? Will I actually recover? What things should I avoid? In case I make matters worse.
Intro 20:32
Doctors will explain things that obviously, you’ve never had a stroke before, you probably don’t know what questions to ask. If this is you, you may be missing out on doing things that could help speed up your recovery. If you’re finding yourself in that situation, stop worrying, and head to recoveryafterstroke.com where you can download a guide that will help you.
Intro 20:55
It’s called seven questions to ask your doctor about your stroke. These seven questions are the ones Bill wished he’d asked when he was recovering from a stroke, they’ll not only help you better understand your condition, they’ll help you take a more active role in your recovery. Head to the website now, recoveryafterstroke.com and download the guide. It’s free.
Bill Gasiamis 21:19
Hmm, that’s interesting. So what about your identity guys, like your combined identity before it was, you know, healthy husband, healthy wife, healthy child healthy life? You know, everything was going good. But how did it change the way you guys interact as a family?
Bryan Caldwell 21:37
I think my son actually adjusted really well, like he’s still very worried when you know, little things happen. And he cries, I’m like hey dude, it’s okay. But, you know, what I struggle with sometimes is putting my socks on.
Bryan Caldwell 21:54
So every morning, he puts my socks on for me. So he loves to help out. And he does a really good job of assisting with different things. And he doesn’t really, I mean, a typical seven year old, of course, he’s going to complain about stuff.
Bryan Caldwell 22:06
But he loves to just, you know, whatever we’re doing wants to help out. He wants to be a big kid. So he’s done a really good job. I mean, Brittany, when I speak on behalf of her, she, you know, I would say that, we’ve only been married for three years.
Bryan Caldwell 22:23
But when we met five years ago, I wouldn’t say she was very responsible. But within this last year, she has become my rockstar. Like she has done everything, learned everything taken care of everything. I mean, I have nothing to worry about whenever she handles something.
Bill Gasiamis 22:41
All right, stop for a second. She was working telling you to go and get a job. You weren’t working. What do you mean, she wasn’t responsible?
Brittany 22:51
I wasn’t really working when we had first gone together years ago. And I kind of had to step outside of my comfort zone and go get a job, put my son in daycare, do things like that, that I didn’t really want to do.
Brittany 23:07
Like he handled everything like he did laundry, he would pay the bills. he mowed the lawn, like I suddenly became a gardener overnight, a bill payer, accounts payable, like all of the stuff that I didn’t want to do, and I had to do it.
Brittany 23:24
And then on top of that, it was like, all of these little things he didn’t take into account. Like I spent hours on the phone trying to figure out like disability, for example, and trying to get that process done. And that took six months alone or the transplant. It’s like I have a ginormous two inch binder of all of his stuff that he needs for transplant.
Brittany 23:46
And it’s like when he just he looks at it. He’s like, oh, where’s that? Oh, okay. So it’s all here. Like, we went to see his kidney doctor today. And she was like, Here, here’s his labs. I know you guys are probably the only ones that actually keep these cuz you’re actually responsible enough. So I’m like, I like to look at this stuff. It’s, interesting to me.
Bryan Caldwell 24:10
And she also praise Brittany because she was there since I think the first week? Second week?
Brittany 24:16
Probably like day three.
Bryan Caldwell 24:19
And she saw me when I was at my worst. And she’s a nice Indian lady. And she goes, You know, I’m so thankful that you are here we are about to pull the plug on you.
Stepping Up As A Caregiver
Bill Gasiamis 24:32
Britany so you had a massive change in mindset? Did you need such a drama to change your mindset and become quote unquote, more responsible? I mean, obviously, you need to help out or you need to step up, you know.
Bill Gasiamis 24:48
In sickness and in health and death do us part probably you said that when you guys got married, maybe. So like, what happened with your mindset? How did it shift like that? I know what caused it.
Brittany 25:06
I think I was just very focused into work. So I would, because I work from home, so I would work, you know, get on the computer, seven 8am. And there were nights where I wouldn’t get off till 8:30 9 o’clock 10 o’clock at night and he’s like.
Brittany 25:23
Get off the computer separate time separate, then I’m like, it’s so hard when my office is right next door in my mind is running a million miles an hour, but my priorities just weren’t in line with what they should have been. And so when there’s something drastic that’s happening in life, like this, it’s like, you know what work is going to be here tomorrow.
Brittany 25:41
And I’ve had that mindset to where the same work is going to be there. And if there’s something that needs to be done today, then I gotta get it done. If I have to take care of my son, because he’s sick, if I have to take him to doctor’s appointments, if I need to go to therapy, and luckily, I have a really good job to where my boss understands the situation that I’m in, and I don’t, you know, get a hard time from it.
Bill Gasiamis 26:01
Work never ends anyway. I mean, doesn’t matter how much work you do, it never ends, there’s always something to do tomorrow. That’s really cool, that you had the awareness to just realize that, okay, some priorities need to change, and work is going to be second fiddle to everything else that’s family-oriented.
Bill Gasiamis 26:23
And, look, that’s what most people do. That’s what my wife did. That’s, that’s what a lot of people do. But I get what you’re saying about the chores and all that sort of stuff. Now, you’ve got to step up, and you’ve got to take over the whole running of the family, which was what my wife did.
Bill Gasiamis 26:36
She became a caregiver, she became school mom, she became the main breadwinner, she became the person who had to look after her dad, because my mother-in-law passed away at the same time that I was unwell.
Bill Gasiamis 26:52
And it was she just had to put everything on hold and do all of her things without really anyone asking her. Was she okay with it? You know, Are you up for it? Is that what you want to do?
Bill Gasiamis 27:05
Of course, she said she wouldn’t want to do it. But she did it. She did what she felt like she had to do I was so lucky. Because I went through about three and a half, four years of bleed, a little better, another blade, a little better brain surgery.
Bill Gasiamis 27:23
So it was just ongoing this ongoing constant saga. So have you put some of the things you love to do on hold? Have you found some time for yourself to do the things that you’d love Britney? Where that all the rest of your life?
Brittany 27:42
I don’t know. I mean, at first, it was extremely hard. I felt like I would go to the hospital every single day and just be mentally drained by the time that I got back because all he did was just cry.
Brittany 27:55
And I know that he couldn’t help it. But he you know, I get there at 9am. And he’s like, help. They’re trying to kill me. And I’m like, No, they’re not, you know, if you’re just an ICU, you’re having delirium like hallucinations.
Bill Gasiamis 28:05
They’re trying to save you.
Brittany 28:07
Yeah. And on top of that, I would leave for 20 minutes, and he’d sit there and watch the clock. And literally watch it tick. And then I would come back, you were gone a really long time. I’m like no, I wasn’t, so I didn’t get a break the entire day.
Brittany 28:21
And then by the time we get back at night, it’s like, I had to explain what was going on with Logan, our son, and hey, he’s okay. He just can’t talk right now. And then I still had to work, you know, meanwhile, all of this, I still had to make sure our dog was getting taken care of the house was somewhat taken care of.
Brittany 28:41
So I think I pushed all of my feelings aside for a really long time. And then, on top of that, when he came home a couple months later, it was like, we went straight from this hospital adjustment to now we have to adjust with dialysis and doing dialysis every day. And what does that mean for us? And how is that going to change and we have so much more freedom than ever before.
Brittany 29:03
If we wanted to go for a drive and enjoy the beautiful scenery, we could just go and do that now. It’s like, hey, at 6:30 we need to go hook up to dialysis. And so it changed and it went from dialysis to doctor’s appointments to therapies to every single week, there was probably three or four specialty appointments on top of therapies that he had to go to.
Brittany 29:27
And it didn’t stop and I think it finally hit me like last October and I’m just like, I think I’m just at my like my brain I can’t take anymore because I just had taken care of everyone else for so long. That I just I felt like I just needed to break down over and over and over and over again because I hadn’t all year.
Bill Gasiamis 29:49
And did you?
Brittany 29:50
Oh yeah, plenty of times. So it was hard and then it was hard because I was doing that when he was trying to stay positive and focused on I was recovery. So it’s like now I feel like I’m being this negative person. But it just was like, it was a lot for me to kind of adjust and adjust with this new life.
Brittany 30:10
And how do we move forward? It’s so different. And I just remember, you know, there’s a lot of things that he doesn’t remember, because he wasn’t there for he was so incoherent. And I remember, you know, he was our son’s hockey coach. And the season was still ongoing when he went into the hospital. And every Friday was his hockey practice.
Brittany 30:29
And I said, Hey, let’s go to hockey. I’ll meet you there, I’ll take you. And he’s like, No, if he’s not going to be my coach out there, I don’t want to go. And I’m like, so it was really hard. He didn’t want to go for pretty much the rest of the season. And then when this season started, I was like, Hey, I think you should do it.
Brittany 30:46
He’d want you to do it. And so we had a big conversation with him. Like he may not ever be able to be your coach again, but just get out there and go have fun and he had fun when he did it. And he’s like, I’m glad I went ice skating again, or played ice hockey again.
Bill Gasiamis 30:59
Is that hard for you to listen to Bryan?
Bryan Caldwell 31:02
It’s hard to be a spectator to be honest. I like participating in basically everything. But when I just having to experience like the whole ordeal myself with her, it’s been an experience. So I’ve grown more no doubt. I’m sure she has also.
Diet After A Kidney Failure
Bill Gasiamis 31:25
It sounds like you both have adjusted grown, learn new things about yourself. You’ve changed your diet dramatically. I imagine. Brian has that right. So what are you not consuming these days? Or what are you consuming?
Bryan Caldwell 31:39
So what the dial says and diabetes and stuff like that, just watch my blood pressure. Make sure that’s okay and controlled. I watch potassium, sodium, carbohydrates, sugar, anything that tastes good, it’s out of my diet.
Brittany 31:57
He can’t eat cheese anymore.
Bryan Caldwell 31:59
No beans. But I cheat sometimes, like today, for instance, I got my levels and my blood checked and everything was great. And beyond good. So I said, You know what, let’s go have a cheeseburger today. So we went out, I didn’t eat the buns, which is all the carbs.
Bryan Caldwell 32:21
But I did splurge on French fries and cheese and stuff like that, which I never have, it doesn’t affect me that much. But every now and again, it’s like, you know, I’ve always lived by I don’t want to die unhappy, I want to, you know, experience some things that I enjoy.
Bryan Caldwell 32:40
So I’m not gonna just give up on things completely that I enjoyed before. So the little things in having a portion controlled, and, you know, taking them in seldomly, like, you know, here and there, not all the time.
Bryan Caldwell 33:00
Just, you know, give your body a break. So I for the most part 90% of time I take care of my body, in and out. No problem. And then when it comes time to cheat, you know, I don’t feel guilty.
Bill Gasiamis 33:11
Yeah, yeah, fair enough, man, I get that. So what about your sleep? Did you get any sort of changes in the way that you slept? Or are you sleeping? Okay? Has that become worse or better? Is it okay?
Bryan Caldwell 33:27
I’d say because of dialysis. The machine loves to be that me. If my line my dialysis line that gets cramped, so the fluid doesn’t flow so it just screams at me until I wake up and it’s loud.
Bryan Caldwell 33:41
So that wakes me up. You know, it depends if it’s a good night or bad night. If it’s a bad night it’ll wake me up five six times. If it’s a good night I’ll sleep all the way through so I usually I mean basically every night I wake up right when dialysis end so about 5:30 to 6:00.
Bryan Caldwell 33:58
And I get up and usually you know go right to the gym right to my workout and get things done before I take my son to school and usually if I don’t get it done before school, then I come home and do it that way. All right, pick Brittany Up we go both go to the gym together.
Bryan Caldwell 34:14
And you know we kind of have motivated each other for the most part. You know, I was working out for myself and then I got Brittany to work out for herself. And you know, I think my motivation probably rubbed off on her a little bit to kind of get herself in check and her health and check.
Bryan Caldwell 34:34
So she’s on a you know, a diet right now where she’s eating better and she has more energy and you know things are just properly flowing the way it should. And her mood is better my mood’s better. You know, it’s funny how the vibrations is go off one person just affect all the people around you.
Bill Gasiamis 34:55
Absolutely food is huge on that I mean increases your blood pressure eating kliesch, your blood sugar. And all those things increase your cortisol levels, your stress hormone, then you have a food coma crash, if you’ve eaten too many carbs, and then that’s no good for energy levels, and you can’t get stuff done.
Bill Gasiamis 35:14
I mean, food is probably one of the most critical things that people can do to manage their symptoms of stroke and feel better. The better you eat, the better it is, the less inflammation that occurs in the brain.
Bill Gasiamis 35:27
The better that neurons rewire, and re-fire to give you back movement, and all that kind of stuff. So it’s a massive part of the recovery. Of course, it’s a massive part of dialysis treatment as well. How often is dialysis? And how many hours does it take?
Bryan Caldwell 35:44
10 and a half hours every night?
Bill Gasiamis 35:46
And is there a way to make it five hours, say midday, and then five hours at midnight? Was there an option for that?
Bryan Caldwell 35:59
I think Brittany could talk on that. She knows she’s more educated than I am.
Brittany 36:03
I don’t think so because it runs cycles back to back to back. And so there’s four cycles, which totals the 10 hours. But I think it works out better, because he just, well, if he slept through the machine beeping, he would be able to sleep throughout the night, and then he’s free to do whatever he can.
Brittany 36:23
Versus going to a clinic three times a week or five hours. So that’s why I kind of made the decision for him when he was in the hospital that PD, which is peritoneal dialysis would be a better option for him because he needed to go to those therapies he needed to go to doctor’s appointments.
Brittany 36:40
And then to have to worry about going to dialysis three times a week, it just would have been really hard. On top of that he needs a transplant and hemodialysis was very hard on the heart. And so it could have affected him heart wise, and he’s already got on top of everything else a 40% blockage in one of his arteries in his heart. So we didn’t want to make anything worse.
Bill Gasiamis 37:04
Bryan, stop it with all the drama, please.
Bryan Caldwell 37:09
You know, everyone says that, you know, God was pretty hard on you, is he ever gonna give you a break?
Bill Gasiamis 37:13
I don’t think God’s got anything to do with it. I feel like you’re the guy that’s going have to take responsibility here. And sort yourself out.
Bryan Caldwell 37:25
That’s definitely true, I mean, I think that’s part of my recovery is having to realize that I didn’t take responsibility for basically my health, like, I’ve got myself here. This is definitely 100% preventable.
Bryan Caldwell 37:40
If I would have made better decisions when I was younger. But you know, as I got older and didn’t really watch my diet kind of ate whatever. I kept up on my insulin and my sugar, but I just ate whatever I wanted. It’s like, it wasn’t good for my health overall.
Second Chances

Bill Gasiamis 37:58
God, wants you here all the shit that you’ve done to your body, God’s going hang on a sec, your time is not up yet. Bryan, you know. There’s stuff to do. There are things you need to learn and discover and teach your son. And you know, and work out with your wife. And God’s going, you know, like, let’s go again, let’s have another trial, let’s sort it out.
Bryan Caldwell 38:20
It’s definitely changed my perspective on life. Like, I look at it, as you know, I’m not going to let this chance be the end of me, this is another chance of life that I get to pursue, I get to make the most of my journey.
Bryan Caldwell 38:38
You know, make the most of other people’s journey, which I’ve been told that my story is inspiring, and, you know, my recovery is much better than they expected. And, you know, it all comes from hard work really.
Bill Gasiamis 38:52
Yeah. Hard work. Definitely a lot of luck. Even though it seems like you’ve been unlucky, actually, you’ve been extremely lucky to still be here to within a year be on the podcast talking about it.
Bill Gasiamis 39:04
Like you’re looking healthy and fantastic. I know that you may not feel that way every day, but you’re looking great. And that’s a great start. You got a supportive wife who’s done everything and she’s just moved heaven and earth to make sure that you’re well and everything’s okay.
Bill Gasiamis 39:19
I mean, you’re lucky boy, you are such a lucky boy. I love that you’re here talking to me about it. And not only that, I mean, I know that some people have a worst time with a stroke and recovery and all that kind of stuff. But you know, if this happened 50 years ago, when our parents were growing up, they wouldn’t have survived it the people back then wouldn’t have been around would they?
Bryan Caldwell 39:46
I think my Millennialish mind kind of focuses on my stroke mind and it makes me look at things different.
Brittany 39:57
He’s stubborn, In other words, I’m not gonna be like this the rest of my life. And the funniest thing that I think is before his stroke, I would try to talk to him about his diabetes, or you know his insulin or get him to go to the doctors.
Brittany 40:14
And it was I know nothing about diabetes. I know nothing about anything that he’s going through. When he came home from a hospital, it was like, Hey, here’s your lunch, I’m giving your insulin, no questions about how much I was giving him, no questions about what I was giving him. And it’s like every single day is his levels were perfect.
Bill Gasiamis 40:34
Why don’t we listen to our spouses, though, it doesn’t matter who I spoke to, you know, we’d never listened to them. It’s like, Yeah, shut up, leave me alone, stop nagging. We don’t ever listen.
Bill Gasiamis 40:45
And usually our spouses are coming from a good place. They’re coming from a caring place. Maybe they don’t know exactly how to express it to show their caring concern for your health. And they kind of sound nagging and whinging and complaining. But why don’t we ever listen, Bryan?
Bryan Caldwell 41:04
I don’t have a perfect answer to that. But my answer for myself personally, is I looked at that she was younger than me, so she didn’t experience more than I did. And over time now, especially my perspectives change.
Bryan Caldwell 41:18
I mean, I see that she’s more responsible. She, took control, she stepped up to the plate. I mean, I can trust her with anything and everything now, before it was questionable.
Bill Gasiamis 41:33
How much younger?
Bryan Caldwell 41:35
She’s eight years younger.
Bill Gasiamis 41:36
Yeah, she’s eight years younger. Now she has to put up with all the sexy stuff in the bedroom, you know, the dialysis, the beeping and all that kind of stuff. Come on, man, you know, you could have done better.
Bill Gasiamis 41:49
You should have done better. What’s that? Like? Actually? How has it impacted intimacy and all that kind of stuff. If you don’t want to talk about it too much. You don’t have to.
Bryan Caldwell 41:58
I’m okay with opening up. She’s not so much opening up. But I’d say you know, it’s definitely affected both of us in a sense, but more her than myself. I’d say physically, it’s affected me a little bit.
Bryan Caldwell 42:13
But you know, I have my days where I tell her like, Hey, I’m having an on day. Like, let’s go. And she’s like, you know, all the typical excuses.
Bill Gasiamis 42:24
Headache.
Bryan Caldwell 42:26
Yeah, you know, I’m hungry. I didn’t eat today. I didn’t exercise. I work too hard, you know, all those. And for me, it’s like, Hey, this is once in a blue moon, I’m gonna feel like this. So let’s do it. But her on the other hand, it’s like, you know, she looked at me basically before, like, Hey, I’m a lot of fun. And that’s just the way I am.
Bryan Caldwell 42:51
And you know, I’m very bubbly and outgoing. And, I was very affectionate before, but she’s never been an affectionate person. So now that with my stroke, I’m actually a lot more affectionate. So I’m actually like, I’d say I always been saying, like, five years ago, I was like, you know, I’m the girl in the relationship.
Bryan Caldwell 43:12
I like to cuddle. I like to laugh. I like the hand holding. I like kisses. I like all that stuff. She hates it. You know, it’s like when I reached out to kiss her. She’s like, eww your breath stinks, like, stay away from me. And I’m like, come on, I just want a kiss and she’s like, no, get away.
Brittany 43:31
It was hard at first, because I always told him, he’s like a stage five clinger. Like I would go in my office to work. And I have a bed right behind me in my office, because it was like our guest room slash office. And he would come in here and fall asleep on the bed.
Brittany 43:51
And I would be on meetings, and he’s behind me snoring. And I’m like, get out of here. Like, give me space. Like, this is just different for me. When you didn’t have your stroke, you were at least out you’re working.
Brittany 44:03
You we’re outside working on your truck, you were just doing something. I’m like, you never leave like as wrong as that sounds. You’re always here. So and he’s like, wanting to cuddle and wanting like, just get away.
Bryan Caldwell 44:14
Like now it comes to the point where you know, I’m well enough to go and do stuff and I I try to stay out the house and keep busy and do different tasks. So now when I leave, she’s always calling me.
Bryan Caldwell 44:25
Where are you? When are you going to be home? I want you home. You know she does the complete opposite of what she was telling me. And just having a good time with it making sure she’s bugging me now because I bugged her so much before.
Bill Gasiamis 44:41
Yeah, I love it. So some of it. Actually, Brittany, you’re worried about him and thinking that maybe something’s gone wrong. If you haven’t heard from him for too long. Is it something like that?
Brittany 44:53
Yeah, I think and that’s what I was struggling with a lot when he first started driving in August is he would leave Even I’m like, where are you at? And they he wouldn’t answer. He had this he would take his phone everywhere he went, but he was horrible at answering his phone.
Brittany 45:08
And so I’m sitting there stressing out what if you have another stroke? What if something happened, his blood sugar is low. And so it was more of me worrying. And then it It freaked me out even more driving around with our seven-year-old, I don’t want something bad to happen.
Brittany 45:23
And then he feels he has to now take responsibility. And it just happened. We went to an event a couple of weeks ago, and his sugar was so low. I was like, hey, I’ll go get the truck, we can leave. And so I left our seven-year-old inside with him to watch him because I didn’t want to leave him there and have him pass out.
Brittany 45:44
And my seven year old is calling me on his watch because he has like a phone watch where he can call me and him and he’s like, but he handled it so well. I think you need to come in here right now. I’m like, Hey, I’m trying to find a parking spot. Just give me a few minutes.
Brittany 46:00
And he’s like he’s about to pass out. Can you please go get help, like the most calmest voice. And I’m like, okay, you know what, I don’t even care. I’m parking in Brazil. And they can tell me for all I care. So I ran back inside.
Brittany 46:12
And it was like I had gotten in I got the paramedics because I just needed like glucose tablets or something to get his sugar up. And I think he said at one point, it was like 37. So he was on the verge of passing out if he wasn’t trying to pass out. And so things like that just freaked me out and then having to put our son in that situation too. It’s tough.
Bill Gasiamis 46:33
That is tough. It’s tough for anybody, let alone a seven year old. Kids are resilient. They are troopers. They know how to help out when they become a teenager he’ll be a complete pain in the ass right?
Bill Gasiamis 46:47
But still, isn’t it amazing that a seven year old can instruct you give you all the information that you need. Update you let you know what’s happening. And just do it as if you know, it’s just part of his day like regular stuff. You know that to look out for this old bloke who can’t do anything for himself right now?
Brittany 47:09
Yeah. And he does that at first, it was a hey, let’s run to the store. Let’s go here. And he’s like, but what if his sugar goes low? Like, what if something happens to him? And I’m like, It’s fine, because I made him get a continuous glucose monitor. So the ducks calm. And I downloaded the app on my phone.
Brittany 47:28
Because he didn’t have that before the stroke. And I tried to get him to many, many times. He just didn’t do it. So I have the app on my phone. So anytime he’s going low, if he doesn’t text me back right away, if I’m like, Hey, are you eating something?
Brittany 47:41
Are you drinking something? I’ll call them call them call because I don’t want them to be sleeping to where he’s so low. He passes out. I don’t want to have to go through all of that again.
Bill Gasiamis 47:50
Yeah. And that gives you alerts as well, doesn’t it when it’s noticing too low or something’s up? Yeah, it does. Yeah, that’s a bit of relief. And yeah, I know, I was saying about checking in all the time. You know, that was one of the things that was happening in our house, people were wondering, all the time where I was what I was doing, am I okay.
Bill Gasiamis 48:13
Especially when my wife had to go back to work at some point and leave me at home alone. I had a couple of falls, which she found out about, you know, when she came home, because luckily, they weren’t too bad. But I did tell her that I fell. So then there was concerns about that. And there’s all sorts of concerns and things you need to take into consideration. Technology plays a big part in helping out doesn’t it?
Brittany 48:39
Yes, so I got a camera for our loft, and I got a camera for our living room for our son because he was doing a lot of very questionable things when we weren’t around. And he would sneak away when we were doing dialysis. And we would find stuff under the couch and you know, all of this random stuff.
Brittany 48:57
But I actually use it for him too. Because I’m like, Hey, is he okay? Like if I’m gone you know? Is he just sleeping on the couch? Like, that’s fine. And I actually plan to travel here pretty soon for work.
Brittany 49:11
And I think it’ll just make me feel a little bit better. I feel like a complete stalker, like, no question about it. But also I’m okay, because I know that if something does happen, I can easily see, hey, he’s on the ground. Let me call for help.
Bryan Caldwell 49:28
And the good thing is we have all these very supportive neighbors. So anything if I need anything, we can basically go to any direction and they’re there.
Bill Gasiamis 49:37
So community support is really high. And you guys have got good relationships with everybody?
Bryan Caldwell 49:45
Definitely.
Reaching Out – High Blood Pressure & Stroke
Bill Gasiamis 49:47
Yeah, that’s a relief. That’s such a good thing. A lot of people don’t have that either. It’s such a struggle for some people not to have support and not to have a community. What about stroke? Did you get curious about stroke? and needing to find stroke survivors I needed to learn from them. Who was it that reached out to me? I can’t remember.
Bryan Caldwell 50:06
That was me actually, I was at the gym, and I’m struggling with motivation and inspiration. So I was looking just on Apple podcasts. And yours was the first to pop up. So I listened to a bunch of different episodes. And I had reached out saying, you know, this is very interesting. I want to jump on there and tell my story.
Bill Gasiamis 50:25
Yeah, does it help to tell your story?
Bryan Caldwell 50:28
I would say, I just want to help others. It doesn’t help me necessarily, but I want to help others. I actually got bored within my first few months of being home. So I without it’s not current, but back in the day, I started charity. So I actually was able to give away about $6,000 to different people that are struggling financially.
Bill Gasiamis 50:56
Thats $6,000 that you needed for your self imagine and you were giving it away?
Bryan Caldwell 51:01
Luckily, we’re fairly well off. So we’re not too worried. But lots of people, you know, they have struggle paying co-pays. Like here in the States. I don’t know, do you have universal health care in Australia?
Bill Gasiamis 51:15
We do.
Bryan Caldwell 51:16
So we have to pay over here in the States. So a lot of people struggle with paying $20 $50. So you know, just like when I saw people like, I was in the stroke support group on Facebook, a couple of different ones. So I just saw like people here and they’re talking about, you know, I just can’t pay for my co-pays this month.
Bryan Caldwell 51:39
And, you know, things are so hard. And I just, you know, just I’ve reached out to a whole bunch of them. And some of them were reluctant to accept the money and say, Thank you so much. You’ve changed my life, and this and that. Some people thought it was a scam. So they called me a scammer. And I’m like, that’s fine. Call me whatever you want to call me. But you don’t get no money.
Brittany 52:00
So, it wasn’t our money. It was actually friends who wanted to just donate and help other people. And I thought it was actually pretty nice. Because when people would write back and it was like, you know, to still some people still will message him just from time to time and say, How are you doing? You know, so I think it’s just an interesting thing.
Bryan Caldwell 52:26
And he spoke about telling your brain positive things and your brain reacts in a positive manner. So that’s basically how I kind of approach things is, you know, stay in a positive direction, tell myself positive things. Don’t listen to my negative thoughts, because that gets me nowhere. And that’s a realistic thought.
Bill Gasiamis 52:49
I used to have them too. It’s okay to have them. Just don’t give them too much. airtime. That’s all.
Bryan Caldwell 52:55
Yeah, any power.
Bill Gasiamis 52:56
Yeah, Cory was in Episode 173. He’s a real cool dude. And he’s doing some really good work, trying to work out whether or not cannabis oil can be used to support people recovery, after stroke, and probably lots of other things.
Bill Gasiamis 53:13
And I’m not sure how he’s done it, but he’s actually doing proper studies where they’re researching, and they’re gonna have a proper study, and then a proper report after it. And it’s like, really awesome stuff. Cory is amazing. So he too, he’s kind of like, you know, he’s like the surfer dude.
Bryan Caldwell 53:31
It’s a good feeling. If you’re in touch with your your emotions. So with your stroke. So when you do nice things, it makes you feel a lot better internally.
Bill Gasiamis 53:46
It does. It makes a big difference to the other person as well. They get a real surprise and a shock and they feel like you know, wow, Humanities alright, someone did something nice for me.
Bill Gasiamis 53:56
And I didn’t need to pay it back or do anything for it. So Brittany, what’s it like for you now to remember how you kind of were before what what your thought pattern or process was like before?
Brittany 54:12
I just don’t think it’s the same at all. I think I’ve changed and probably in every way but not I would say not in a worse way. I think I’ve grown up and matured probably a lot more in a lot of different ways that I probably wouldn’t have this quick. And I just, I don’t know, it’s different.
Brittany 54:35
I mean, he talks about giving money away and I’m like, Well, who’s like a caregiver. I want to go on the caregiver group because there’s a lot of people struggling and I go on those groups and, you know, I’ll read their stories and then I’ll almost feel thankful that he yes, he had a stroke, but he’s still here because people will talk about how you know, their stroke survivor that they have to take care of will yell at them.
Brittany 55:00
And we’ll cuss at them. And we’ll throw things at them. And they’re abusive, and I don’t have to deal with that. So it’s unfortunate that he had a stroke. But he’s not nearly as severe as I would say a lot of other people that are out there. And I think he’s pretty fortunate for the circumstances that he was in altogether.
Brittany 55:22
And when he had gotten to the hospital, they had said that his kidney function was at 5%. So it’s almost as if it was like, probably a couple more months probably would have went by and he would have just passed in his sleep from kidney failure. So it’s unfortunate that he had a stroke, but it’s almost a good thing that he had a stroke.
Bill Gasiamis 55:41
Yes. Yeah. I hear you, it’s kind of like a blessing in disguise.
Brittany 55:46
Yeah.
Bryan Caldwell 55:47
It’s a wake up call for sure.
Bill Gasiamis 55:49
Yeah. Are you a better mum, because of all this stuff?
Brittany 55:54
I.
Bill Gasiamis 55:56
You’re a great mom. Don’t get me wrong. I’m not saying you weren’t. But are you a better mom, not better to your kid or, you know, changes clothes better.
Brittany 56:06
Like I said, Before, I just was so into work. I just didn’t want to deal with it. And now it’s like, let’s go do this. Let’s go take him here and just have fun or let’s sit there and play Uno, even though he gets mad and tries to steal the wildcards.
Bryan Caldwell 56:23
I think that’s where I still have my cognitive ability was, you know, I Ripper pretty hard for her like, you know, because she always says, Oh, you’re the cool parent. And and I’m just, you know, chopped, what he’s called chopped liver, chopped liver over here. So, so our son, Logan, Logan doesn’t even like to hang out.
Bryan Caldwell 56:44
And I’m like, That’s because you don’t do anything fun with them. You don’t participate. I’m like, go do stuff with them, you know, and she doesn’t now, she’s more aware than she used to be. So I think that he’s, you know, he tends to use us against each other at first.
Bryan Caldwell 57:01
So, you know, we figured that out, and you know, we’re working with each other rather than against each other now. So I think that she is, you know, that’s her growing in a way, like, you know, as you get older and figure things out, and realize that you could have been better than why you were, that’s her, you know, getting to age basically.
Bryan Caldwell 57:23
So I’m still saying, Hey, she’s 27. And still, there are moments where I’m like, you know, palm to the forehead, like, why are you acting like this? Then I remember, like, you know, just because of my stroke, and my perspectives a little bit different. You know, I probably realize I’m a little bit of a pain in the ass too, and she’s reacting to the way I’m acting.
Parenting At a Young Age

Bill Gasiamis 57:45
For sure. You are Bryan 100%. And when you’re 20, and you have a kid, or 20, I mean, your barely, you were just a kid not that long ago, like, you’ve got no idea I was a young dad, I was 22, when I had, my wife gave birth to our first son, I had no idea, I had no idea for good.
Bill Gasiamis 58:11
Man, the best part of the first 10 12 years, I had no idea what the hell I was doing. His younger brother is four years younger than him. And I was getting it wrong a lot of the time and ego was a big part in my life, you know, and it was the stroke that made me realize at 37 that I need to make some things good, I need to go back and repair some of the stupid things that I said, did, behave like.
Bill Gasiamis 58:36
And kind of let them know that I’m going to try and change and be a better version of a dad, I was a pretty good dad. But I just, I had didn’t have a lot of resources to handle complex situations.
Bill Gasiamis 58:52
So I used to default to the one dumb thing, which was yelling all the time and screaming and making them feel like they couldn’t speak up and give me their perspective was never a conversation a two-way conversation about what they thought and what I thought it was always about how I saw it, and what the rules were and how there was no getting around them and all that kind of stuff.
Bill Gasiamis 59:14
And I was just a bit of a tense hardass. And I sort of started to let them speak and pay attention. And it took a while to undo all the mess that I had made, you know, to make them feel comfortable with talking to make them feel comfortable with saying stuff that they knew I wasn’t going to like to hear and then to me not to respond and act like an idiot again, it was to stop them.
Bill Gasiamis 59:39
Just give them a space to express themselves, you know, and tell them and allow them to tell me when I was being stupid that hey, you are actually being stupid to me right now. You better stop that. I may actually take that as a really good thing that I’m being checked, my behavior is being checked by them.
Bill Gasiamis 1:00:02
Because I’m making them feel bad for some in a way that’s not productive or supportive of their growing and learning, because they’re teenagers, and they’re learning and they’re growing. And I wasn’t. I think that our path would have been completely different.
Bill Gasiamis 1:00:21
If I continued to be that kind of guy, they just would have been more disconnected from me and more and less likely to come to me when they needed help. And that really scared me, you know, I really wanted to make sure that I was going to be able to be there when they needed help, and they did something stupid as a teenager does.
Bill Gasiamis 1:00:39
You know? So, when you’re 20, and you have a kid, and you’re just a kid yourself, it takes a lot of growing up. There’s so much to learn at 20 between 20 and 30, there’s so much to learn, especially when you become a mum, that young. Brittany, do you relate to that? Does that kind of feel similar?
Brittany 1:00:59
Yeah, I think so. Like I was somewhere the other day. And I think the lady had asked me Do you have kids? And I’m like, Yeah, I’m gonna have an eight-year-old this year. And she was like, what? You look like you’re maybe 20.
Brittany 1:01:11
And I’m like, I know, I sometimes don’t believe that I have an eight-year-old either. So I was very young, very immature, naive. And I think just as I’ve grown as a person if there’s a lot that’s changed, whether that’s in our relationship and the relationship that I have with him.
Brittany 1:01:31
There’s things that I could see last year where it’s like, you know, he was going through a lot, and how do you not get mad at a kid for the things that they were doing? Because then I was also feeling bad at the same time, but then it just became a struggle, because you also have to be a parent.
Brittany 1:01:50
And tell them no, that’s not right. Like, there was one time, he went to the grocery store with him and just stole gum, because he just wanted gum. And we made him go back and return it to the manager, and he just bawled his eyes out. But it’s like, Hey, you’re you can’t do that. And you’re not going to just get away with it. Because we’re all going through a tough time right now. Otherwise, he’s gonna continue getting away with it.
Bill Gasiamis 1:02:14
Yeah, yeah, so when I’m not shaved say a few gray whiskers, but I don’t have any gray my hair. So when I shave, you know, people think I’m 47 People sometimes say to me, you look like you’re maybe in your late 30s, something like that. So I still, and then they say to me, How old is your son, I’ll say my oldest son’s 25.
Bill Gasiamis 1:02:36
And they’re like, Woah, you don’t look like you got a 25 year old that that’s a really lovely thing. It’s good that it was so difficult financially, when I had kids young, we did a tough for a good 1015 years. We didn’t go without, but it was really tough to cover all the bills and all that kind of stuff.
Bill Gasiamis 1:02:56
But now my kids, I’m 47. My kids are 25 and 21, the 25-year-old moved out less than a year ago. And the 21-year-old is looking at moving out already. Me and his mum their mums a few years older than me, she’s three years older than me. And it’s like, we’ve kind of like free of them and we’re only around the 50 mark.
Bill Gasiamis 1:03:19
It’s really cool to have this relationship and a very small generation gap between us and them, we kind of get most of their stuff and their lingo and their technology, we’ve kind of still there.
Bill Gasiamis 1:03:36
And we have these really great conversations with our kids that I never would have expected at 25 when they’re 25 Now there’s so much good has come from it that I just never in my wildest dreams expected that it would be this good. So you got a lot of amazing things to look forward to and even 34 Bryan, it’s not that old, you know, to have an eight-year-old. That’s not that old.
Bryan Caldwell 1:04:02
So I actually last.
Brittany 1:04:07
December 2020.
Bryan Caldwell 1:04:08
Yeah, December 2020, about two, three months before my stroke. That’s when I had adopted basically her son. So that’s when Logan became my son properly. And I decided then, like, you know, I’m accepting the responsibility to set a better example because, you know, I never thought about that before.
Bryan Caldwell 1:04:29
I was a dad but I wasn’t fully a dad yet. So like, you know, so now my perspective is different. I’m like, you know, I have to while I’m here, it’s my second chance to set a better example. So I even told her all the time, like, we need to not fight we need to, you know, close the door.
Bryan Caldwell 1:04:50
Not let him come into the conversation when he’s not supposed to not let him eat what he wants to eat all the time. But then again, you know, I’m like a kid on the inside. I let him do whatever he wants to do at certain times. And, you know, I’m his buddy sometimes.
Bryan Caldwell 1:05:05
But when it comes to being a dad, I step up. And, you know, I also give him a hard time about, like, doing the right thing and, you know, chiming in and, and helping out when he’s supposed to, and he does, he does a great job.
Bryan Caldwell 1:05:20
And I think that’s what’s raising him to be a better kid is I think my stroke has impacted that times 10. Like, in all honesty, he’s seven and causes a lot of trouble within its own right. But he’s a great kid. He listens.
Bryan Caldwell 1:05:36
He does what he’s supposed to, he does his homework. He helps out he, I mean, even with other kids, he’s motivating. He likes to make friends. You know, stuff that kids should be doing. They don’t sit around and if someone’s hurt, he’s going to help them. He’s that type of kid.
Bill Gasiamis 1:05:53
Just wait until they become teenagers, all those lovely things they do. It just gets buried a little bit for a few years, and then it comes back. Alright, so hold on. It’s about 8 9 10 years worth of pain and suffering that you’re gonna go through. But he’ll come around.
Bryan Caldwell 1:06:07
She said he’s not allowed to have girls over until he’s 35. And I said, Yeah, you watch in a couple of years. He’s gonna have a girl over, he’s going to becoming to me saying, Hey, he calls me babe, because that was his first word, because she calls me babe. He’s gonna say, Hey, babe, I’m gonna have a girl come over and watch movies is that okay?
Bryan Caldwell 1:06:29
And I’m gonna say, Yeah, sure. come on, over. And I think it’s good because when I was a teenager, I was a reckless teenager. I caused all kinds of trouble. And my parents had always told me, you know, when you have a kid, you’re gonna get it back tenfold when you’re older.
Bryan Caldwell 1:06:47
And sure as hell I’m getting it back. So I can remember things I did. So when I see him starting to do things, I’m like, Yay, I can call it out and say, you know, I know you’re lying. I know that this is going to happen. I know that. Don’t even try and play around the bush.
Bill Gasiamis 1:07:04
Yeah. It’s good to remember the things that you did that was stupid when you were a teenager, because then you’re not so hard on the dumb decision that a teenager has made just now you’re kind of like, Alright, I know what you did. I know why you did it.
Bill Gasiamis 1:07:21
Now, let’s talk about how we’re not going to do that again, or how are we going to improve or whatever. And that’s really good that you remember how you got yourself into a stupid situation when you were a teenager. I certainly try and do that. And sometimes my kids are shocked when I say to them, you know, that thing that you did? That was really bad. I’ve done that as well.
Bryan Caldwell 1:07:42
I think it’s easier to talk to a seven year old than a teenager.
Bill Gasiamis 1:07:46
Ah, yeah, yeah, I agree. I agree. It changes. It does. It’s really difficult. But look, you’ll be fine. Brittany, forget about the thing about the girl thing, it’s not going to happen. He’s going to do what he wants in that situation.
Bill Gasiamis 1:08:01
And you’d rather have them, at home than somewhere else. I think that I learned I was better off they were at our house being stupid, or doing whatever having fun. Than somewhere where they weren’t safe or whatever. And it’s like, okay, I’ll live with that. It’s okay. But, so you’re gonna before we said that Bryan was lucky that Brittany was around. But Brittany sounds like she’s a little bit lucky too Bryan?
Bryan Caldwell 1:08:35
I would say that I’m a catch. But I won’t try to be too full of myself.
Bill Gasiamis 1:08:45
I love it. Guys, it’s been so fun talking to you. Thank you so much for reaching out and ask to be on the podcast. I really appreciate it. Thanks for being open and coming on and talking about all sorts of things that are difficult and hard and whatever. Heal well feel like you’re well on the way hope your recovery goes well.
Bill Gasiamis 1:09:07
I hope everything goes well with the kidneys and the blood pressure and all that stuff. Brittany, you’re doing amazing job. Well done. Congratulations. Take time out for yourself. Give yourself heaps of Britney time without Bryan.
Bill Gasiamis 1:09:21
Now that you’ve got all the surveillance gear in action. Catch up with the girls, get your nails done, do all that stuff. Leave him at home every once in a while. And yeah, feel free to reach out anytime and I look forward to hearing from you whenever you feel like it.
Bryan Caldwell 1:09:39
Well, thanks for having us on. I appreciate everything you do. That’s why I reached out. So I just want to thank you for everything.
Bill Gasiamis 1:09:47
Thanks. Thanks, Brittany.
Brittany 1:09:49
Thank you. It was nice talking to you. Nice meeting you.
Bill Gasiamis 1:09:53
Thanks for joining us on today’s episode. I told you it was gonna be fun and we had a lot of fun getting to know each other. These two are such a great team working together to overcome all their challenges taking things in their stride, stepping up where they need to taking responsibility.
Bill Gasiamis 1:10:12
I just really, really love this episode. So thank you for being here. I hope you got a lot out of it too. If you’re watching on YouTube, please comment, like, share, give the show a thumbs up subscribe. Also hit the notification bell so that you can get notified of new episodes.
Bill Gasiamis 1:10:31
Any comments, any interaction with the show, wherever you find it will help rank better. And therefore, when the shows ranking better, it’ll be found easier by other stroke survivors. It’ll make a massive difference to the way the recover their recovery might go. It’ll make a massive difference to their caregivers. You’ll help them feel less alone and hopefully help them reach out and get some support. So thanks so much for listening. I really do appreciate you and I hope to hear from you soon.
Intro 1:11:05
Importantly, we present many podcast designed to give you an insight and understanding into the experiences of other individuals opinions and treatment protocols discussed during any podcast are the individual’s own experience and we do not necessarily share the same opinion nor do we recommend any treatment protocol discussed.
Intro 1:11:22
All content on this website at any linked blog, podcast or video material controlled this website or content is created and produced for informational purposes only and is largely based on the personal experience of Bill gassy armas, the content is intended to complement your medical treatment and support healing. It is not intended to be a substitute for professional medical advice and should not be relied on as health advice.
Intro 1:11:44
The information is general and may not be suitable for your personal injuries, circumstances or health objectives. Do not use our content as a standalone resource to diagnose treat, cure or prevent any disease for therapeutic purposes or as a substitute for the advice of a health professional.
Intro 1:11:59
Never delay seeking advice or disregard the advice of a medical professional your doctor or your rehabilitation program based on our content if you have any questions or concerns about your health or medical condition, please seek guidance from a doctor or other medical professional.
Intro 1:12:13
If you are experiencing a health emergency or think you might be, call 000 if in Australia or your local emergency number immediately for emergency assistance or go to the nearest hospital emergency department. Medical information changes constantly. While we aim to provide current quality information in our content.
Intro 1:12:29
We do not provide any guarantees and assume no legal liability or responsibility for the accuracy, currency or completeness of the content. If you choose to rely on any information within our content, you do so solely at your own risk. We are careful with links we provide however third party links from our website are followed at your own risk and we are not responsible for any information you find there.






