Patrik Hutzel from the intensive care hotline interviews Bill Gasiamis about the survival chances after a stroke.
Previous Interview with Patrik Hutzel on Episode 32
Intensive care at home
Twitter
Intensive care hotline
Highlights:
02:26 Introduction
08:40 Bill’s stroke recovery story
13:31 What’s the next step?
16:46 Knowing when to push back
22:13 The importance of nutrition in stroke recovery
26:26 Age discrimination in stroke treatment
35:46 The seven questions to ask your doctor
41:32 The difference between a stroke victim from a stroke survivor
44:32 Why the stroke is the best thing that ever happened
54:44 You’re not alone
Transcript:
Patrik Hutzel 0:00
I’ll read out the comment from Laurie here who says, I’m four years post hemorrhagic stroke and never recovered. Also, I consider myself a stroke victim, not a survivor.
Bill Gasiamis 0:11
That’s a really important distinction to make. So, if you’re a stroke victim, you’re in a situation where you’re allowing what happened to you, to impact you in a negative way and only in a negative way. If you’re a stroke survivor, you’ve already overcome one thing, you didn’t die from the stroke and as a survivor, you are then guided to help you look for solutions to problems because that’s what we generally need to be.
Bill Gasiamis 0:42
Stroke creates many, many, many problems. If you always focus on problems, you will get more problems. If you focus on solutions to problems, you will get more solutions. As a survivor, a survivor needs to focus on solutions. Victim will not be able to change their mindset to focus on solutions, they will focus on all the reasons why this happened to them. What did I do wrong in a past life? Why has God punished me? None of that is useful for improving your outcomes for a good recovery.
Intro 1:23
This is the Recovery after Stroke podcast. With Bill Gasiamis, it is helping you navigate recovery after a stroke.
Bill 1:37
Hello, and welcome to the Recovery after Stroke podcast. If you are a stroke survivor with a story to share about your stroke experience, now’s the perfect time to join me on the show. The interviews are not scripted, you do not have to plan for them.
Bill 1:49
All you need to do to qualify is be a stroke survivor who wants to share your story in the hope that it will help somebody else who is going through something similar. Also, by sharing your story you feel better about your situation, you get something off your chest, and it does help to improve your case and your recovery.
Bill 2:09
If you are a researcher who wants to share the findings of a recent study, or you are looking to recruit people into studies, you may also wish to reach out and be a guest on my show. If you have a commercial product that you would like to promote, there is a path for you to join me on a sponsored episode of the show.
Introduction – Patrik Hutzel

Bill 2:26
Just go to recoveryafterstroke.com/contact, fill out the contact form and briefly explain which category you belong to. And I will respond with more details about how we can connect via Zoom. Now today’s episode is a little different.
Bill 2:42
Instead of me being the interviewer I am being interviewed by my friend and ICU nurse Patrik Hutzel. Patrik operates the advocacy service for people who have loved ones in the ICU called the intensive care hotline. He supports people from all over the world who need to have difficult conversations with medical professionals when a loved one ends up in the ICU.
Patrik Hutzel 3:08
G’day Bill, thank you so much for coming on to this call. It’s it’s a great honor to have you on. Let me quickly introduce you, Bill, to anyone on this call. And thanks to anyone who’s watching this on replay who can’t join us live. Today’s topic is survival chances after a stroke.
Patrik Hutzel 3:30
And that’s why I brought on Bill today. Bill is a three-time stroke survivor and is an inspiration for many stroke survivors all around the world. And I’m not exaggerating here because I know Bill you’ve got your podcast you have interviewed hundreds.
Bill Gasiamis 3:49
265 people on the Recovery After Stroke Podcast.
Patrik Hutzel 3:55
And you would have interviewed I know I was a guest on your podcast. So thank you very much. But you would have interviewed other stroke survivors, you would have interviewed doctors, nurses, I don’t know. Can you talk a little bit more about your podcast as well?
Bill Gasiamis 4:09
Yeah, so the people interviewed were mainly stroke survivors. So they share the story of the time that they experienced a stroke. They then share their story of how they’re going after the stroke. And sometimes, if they’re long enough, out of stroke, you hear about the story 5, 6, 7, 8 years post stroke.
Bill Gasiamis 4:28
So what we try and do is capture the whole timeline, so that we can tell people that if you’re feeling unwell at the moment it starts to improve and then things get better and then a lot of people most people get back to some kind of a regular life routine and start going back to work or becoming involved in their community again.
Bill Gasiamis 4:49
And then we interviewed doctors who came on and shared some of their wisdom about what people can do to support stroke recovery and what’s some of the available medical options. We also interviewed past physical therapists, I think I’ve interviewed chiropractors, I think I’ve interviewed speech therapists, and caregivers.
Bill Gasiamis 5:10
So some of the caregivers who are caring for somebody that’s had a stroke, we’ve had people that have had a stroke, in utero. So before they were born, we’ve had people that have had a stroke in their teens in their 20s 30s 40s 50s 60s. I mean, it’s just every type of person you can imagine.
Bill Gasiamis 5:32
We’ve interviewed people who have had ischemic strokes, hemorrhagic strokes, strokes caused by atrial fibrillation, strokes, caused by a hole in the heart, strokes caused by sneezing, believe it or not, strokes caused by carotid artery dissections or dissections of other blood vessels. So we’ve had people that have had strokes as a result of car collisions. Every type of person you can imagine, there is a story on there that somebody listening here today will relate to.
Patrik Hutzel 6:06
Yep, that’s fantastic Bill. The reason I labeled today’s episode, is what are survival chances after a stroke. This is a question Bill that we’re getting weekly at intensivecarehotline.com. You know, this is, in one form or another? Maybe not always, in those words, but pretty close to those words, what are survivor chances after a stroke?
Patrik Hutzel 6:28
I mean, you’re well aware that we are serving families in intensive care, you know, we have so many families contacting us, hey, my mom, my dad, my spouse, my child is in ICU after a stroke, what are the odds of survival?
Patrik Hutzel 6:44
My response to that is always, well, the odds of survival are pretty good because 90% of intensive care patients approximately survive. But it is so much better to have a stroke survivor here. And, you know, hear it from you directly. What are the odds? You know, or what are the chances of stroke survival? And if you can share more about your own story?
Patrik Hutzel 7:10
You know, I’ve been very impressed by your answer. I mean, we’ve known each other for years, through various entrepreneur groups. You know, I’ve been very impressed and very encouraged by your story. Can you share more about what you know, about survivor chances after a stroke? And then we also want to talk down the line about your upcoming new book that you’ve just written. What’s the title of your book, again, Bill?
Bill Gasiamis 7:37
Stroke, The Best Thing That Happened.
Patrik Hutzel 7:40
Yeah, yeah, that’s an amazing title.
Bill Gasiamis 7:43
Bit of a weird title. People don’t relate to it immediately. Because it’s not the best thing that happens to you. It wasn’t the best thing that happened to me at the beginning. And the book is about post-traumatic growth. And that’s really what the podcast tries to demonstrate.
Bill Gasiamis 8:00
So every person that is associated with my podcast is either a stroke survivor or deals with shock survivors and supports stroke survivors and gets great results with stroke survivors. So the statistics about stroke say that one in four people will have a stroke in their lifetime.
Bill Gasiamis 8:20
And 20% of those people won’t survive after the first stroke. But most of those people will survive now about 60% Get back to work. And then there’s a large percentage of people that don’t get back to work. But I’m not sure how far out those statistics go.
Bill’s stroke recovery story
Bill Gasiamis 8:40
Whether they track people 4, 5, 6, or 10 years, post-stroke, I know that a lot of people, at least 60% Get back to work after their first stroke. And then a lot of people do get back to work after very many years. I had a hemorrhagic stroke in 2012, the first time that my stroke occurred was because of a bleed that occurred in a blood vessel called an arteriovenous malformation.
Bill Gasiamis 9:10
And that blood vessel burst and it bled. And as a result of that it first bleed. Then I had a second blade on in the same blood vessel, but six weeks later, and then, approximately two and a half years after the first incident, I had a third bleed.
Bill Gasiamis 9:29
That third bleed resulted in brain surgery to remove the faulty blood vessels. So they opened my head on the right side, they went in, they removed the faulty blood vessel and then I had to go through rehabilitation because I had to learn how to walk again and use the left side of my body again.
Bill Gasiamis 9:47
And it was a pretty intense three or so years because at that time, each time I had a blade I noticed different symptoms. They were physical symptoms they were cognitive issues, I had problems with fatigue, I had problems with understanding what people were saying and what I was trying to say to them, and I couldn’t finish and start sentences.
Bill Gasiamis 10:11
At one point, I couldn’t recognize my wife. I had difficulty going to work, I couldn’t work for the majority of three years. I wasn’t allowed to drive. I had a passive life for three years trying to get healthy and heal, and, and recover.
Bill Gasiamis 10:32
And in that time, In February 2012, there weren’t a lot of services available for me to understand what my stroke recovery might be, like, what I could achieve, and what some of the obstacles that are could overcome. So I set out to find other people who were like me, that’s how the podcast came to be.
Bill Gasiamis 10:53
And I discovered that every single person on my podcast is a stroke survivor. And some of them have been locked-in and have experienced locked-in syndrome as a result of a brainstem stroke. And those people were, I would say, in a worse state than any of the other people that I’ve met, because when you experience brainstem stroke, it affects your entire body, not just one side, either the left or right side, like me.
Bill Gasiamis 11:22
And as a result of that, those people tend to wake up after the stroke, not being able to move their entire body. So they’ll be in ICU, and they’ll only be able to blink, to respond to people chatting and speaking to them, their recovery seems to be the longest and the most arduous.
Bill Gasiamis 11:41
But it is the most unbelievable as well because they go from not being able to move anything other than their eyes that go to very, very often and most times becoming rehabilitated and active members of their community. Many of those people go back to work.
Bill Gasiamis 11:59
Many of those people achieve amazing things in their lives. So my journey, when it started, was unexpected. I was 40. I was 37 years old, I was a father of two, and I was married, and I had a business that I ran in Australia. So I was overworked or stressed I was doing all those things.
Bill Gasiamis 12:24
What the stroke led me to achieve was a lifestyle change led me to achieve a different way of going about things asking for help and re-educating myself on what was required for me to move forward, after the stroke, how to outsource all the tasks that I needed to outsource for my business and how to keep it going even though I was quite unwell.
Bill Gasiamis 12:49
At that time, when the podcast started to become popular, people started reaching out for coaching. As a result of that, I still have the property maintenance business, which I started many years ago, that was the way that I made a living.
Bill Gasiamis 13:06
Now I offer coaching counseling and support services, not counseling in a formal situation. I’m not a qualified counselor or anything like that. But just acute counseling for people who want to know what to do next in their stroke recovery path. And often that is with the caregivers, mothers, fathers, brothers, and sisters, of people who have had a stroke.
What’s the next step? – Patrik Hutzel
Patrik Hutzel 13:31
I would be very curious to find out Bill what can they do next because I know that is of high interest to our audience here. After all, we can teach them what to expect in the ICU. But where my area of expertise stops is outside of the ICU, especially for stroke survivors. So can you share more about what people can do after they leave the hospital or after they leave the ICU I think that’s the journey that you’ve been through.
Bill Gasiamis 14:00
It depends on the country that they’re in. But if they have insurance and insurance is covering them for a duration, then I would go after whatever can be offered by the insurance providers and do every single possible thing that they offer.
Bill Gasiamis 14:18
One of the things that I hear often is when the provider or the caregivers or the rehabilitation providers say that the patient has experienced a plateau and as a result of the plateau, that they are going to cut services or they’re going to no longer fund certain services. If it’s possible, I would go out of my way to not accept their diagnosis that the person has hit a plateau and as a result, funding is stopped. Now I’m not exactly sure how you do that.
Bill Gasiamis 14:57
But to not accept that response and that diagnosis, and to push back on the supposedly plateau is a really big thing. Because if you can extend the amount of rehabilitation time that a person has the better results they will get, even though they have reached the supposed rehabilitation plateau.
Bill Gasiamis 15:20
Now it’s just a technique, I believe it’s just a technique for insurance providers to get out of supporting somebody for a longer amount of time. Now, you have to be your advocate. So all you have to be the advocate for the person who can’t be their advocate if you’re a caregiver.
Bill Gasiamis 15:40
So in that case, what I would say is reach out to your local community and see if they are, if there are support services, you can just do a Google search online, stroke support services, in your guide you through the local process, what has to happen locally. So I know it’s different in Australia, I know it’s different in the UK, and in the United States.
Bill Gasiamis 16:01
But some organizations stroke foundations in all those countries, where you can reach out to and get some guidance as to where to, as to how to proceed from a certain spot in the recovery, which perhaps is the plateau spot where people tell you there’s a plateau.
Patrik Hutzel 16:24
Bill thank you for that. And I just want to reiterate what you’ve just said there, because I’m a big believer, and this is what we advise our clients, everything in life is negotiable. It doesn’t matter what your insurance says, or, you know what you’ve said, renegotiate the diagnosis, I could not agree more with you.
Knowing when to push back
Patrik Hutzel 16:46
There’s a lot of that work that we do with a similar mindset saying, well, you can’t just accept what they’re telling you, here are potentially other options. And once we all know, I mean, we both speak to people around the globe, really, in our work, you know, you talk to people in the US, I talk to people in the US.
Patrik Hutzel 17:06
You know, with enough clinical insight, you can always go back to doctors, nurses, even hospital executives, and you can say hang on a second, discharging my mom, my dad, or whatever it is to this facility is premature. We need to continue treatment here. And here’s the reasons why. You will also often find that if you challenge that with health insurance, there is often an appeals process.
Patrik Hutzel 17:34
And if you have, you know, whether it’s you as an advocate, or if you get a clinician in like myself, you know, we have often turned those situations around simply by looking at the clinical diagnosis and saying, hang on a second, this is purely driven by money, it’s not driven on clinical need. Let’s look at the clinical need.
Patrik Hutzel 17:55
And let’s advocate on the clinical need, or sometimes what we see in the US in particular, that trying to send people to other states for rehabilitation, two hours, three hours away from their hometown, and you go like, This is madness. I don’t know, I mean, you and I have spoken offline, I believe you’ve recovered with your family being around. And that was probably also critical to your recovery, I would imagine.
Bill Gasiamis 18:29
Absolutely. And I didn’t have to because I live in a major metropolitan city I didn’t have to travel to and three hours to my appointments, that would have made it difficult. And I had a lot of appointments during the week for rehab, especially after I was released from hospital rehabilitation where I was for a month in outpatient rehab, I had three appointments a week. Now, if I had to travel three hours back and three hours from each one of those appointments, that’s not doable.
Bill Gasiamis 19:02
I mean, it’s not doable for most people, let alone somebody who’s got more resources than, say, most stroke survivors. So my idea about pushing back on the suppose that plateau, and having them try to relocate you to make it harder for you is to ask for proof that the person has reached a plateau.
Bill Gasiamis 19:27
Data, you’ve made a decision you’re telling me about it. But what’s that based on? Show me the data, give me the information that you used to conclude that that person has hit a plateau. Now, when somebody hits a plateau, so to speak that’s the time when therapy needs to be upgraded when therapy needs to be taken to the next level. Not a time for therapy to stop because I have met many stroke survivors who tell me that their recovery they are improving years after the stroke. So there is no time to remove services just because somebody made a decision that you need to be cut off.
Patrik Hutzel 20:12
Bill, obviously you’ve had a hemorrhagic stroke, you know, we have any inquiries all the time, hemorrhagic stroke, ischemic stroke, you know, I mean, I know the difference, and most people that come to us by then know the difference as well, do you think there’s a difference in sort of speed of recovery or options for recovery, whether there’s either an ischemic or hemorrhagic stroke?
Bill Gasiamis 20:39
So this is very interesting because what seems to me is that when I had a stroke, in 2012, it wasn’t referred to as a stroke by the medical profession, it was referred to as a brain hemorrhage. And I didn’t understand what that meant, and why was different from a stroke, I had the same neurological problems that an ischemic stroke survivor had.
Bill Gasiamis 21:01
I also had the same neurological problems that a traumatic brain injury survivor had somebody, for example, has had a massive concussion, we all experienced the same physical, and neurological symptoms, and we all had the same type of impact on our daily lives. And we needed to find a way to move forward. And that was the real issue, we didn’t know how to move forward.
Bill Gasiamis 21:27
So, unfortunately, with stroke, every stroke is different. It happens to every individual differently, it happens in a different part of the brain, and it affects a different part of their function. And as a result of that, you can’t compare my stroke to the other person who had a hemorrhagic stroke in the same spot or place, because their brain is wired differently.
Bill Gasiamis 21:51
They have different ages, they have different comorbidities, and they have all these different things. So all strokes are different. However, just because the strokes are different, doesn’t mean the approach needs to be different, the approach needs to be the same, you need to attend to certain things to make sure that you’re giving the best opportunity for the brain to heal.
The importance of nutrition in stroke recovery
Bill Gasiamis 22:13
My understanding and the way that I went about my stroke is that I attended to certain things that I hadn’t attended to before, but some of them are obvious, right? One of the things I attended to was food, on the nutrition side, once people are released from the acute phase of recovery from hospitals from ICUs, they need to take care of their nutrition.
Bill Gasiamis 22:36
They need to make sure that they’re not eating foods that are inflammatory and going to cause more inflammation in the brain and therefore increase fatigue levels and increase the time that it takes for people to recover from the brain injury. Some of those foods are very basic. I’m not a nutritionist, so don’t take nutritional advice from me.
Bill Gasiamis 22:59
But these are really simple things. Caffeine can cause irritation, and make fatigue worse, sugar can do that. Smoking can do that. Drinking alcohol can do that. So alcohol 100% needs to be avoided same with sugar.
Bill Gasiamis 23:17
And caffeine needs to be limited. But if people are going through stroke recovery, and they are still drinking alcohol, and they are still smoking, and they are still consuming high amounts of sugar, they’re going to decrease their brain’s capacity to recover. So I was trying to make the right environment to help my brain in its recovery. I didn’t want to make that worse.
Patrik Hutzel 23:43
Bill, you mentioned age in particular. And you mentioned at the time of your first drug, you were 37 years of age, which I consider to be very young. How do you think age has an impact? We have many families coming to us and saying Hey, my 77-year-old mom and my 77-year-old dad had a stroke.
Patrik Hutzel 24:05
They’ve been previously fit and healthy. And now this happens. They’re unresponsive. They’ve been in ICU for two weeks, they’re out of an induced coma and they’re still not responding. How do you consider what’s your take on the age? When does the stroke happen? What’s your take on that? How does it impact the chances of survival and recovery?
Bill Gasiamis 24:28
I think age is important. comorbidities are important the older we get the more risk factors work against us. So that is a very standard logical thing to take into consideration. However, there is a bit of an ageism thing occurring where the medical community will consider somebody of an older age. less necessary to rehabilitate though won’t put the resources into Somebody older.
Bill Gasiamis 25:02
And I’m not sure, specifically why they’re ageist, because we all know, we all going to be older, we’re all going to be in the same situation at some stage, and discriminating against older people, just because supposedly they have less possibility of recovery. Or supposedly they have lists of years ahead of them or something along those lines, is something that you need to be aware of.
Bill Gasiamis 25:25
And I think you need to push back on the possibility that if you’re over the age of 60, or 65, and you feel like they are fast-tracking, you’re out of the hospital or fast-tracking you back to home. And the family is not comfortable with that. And you’re not comfortable with that.
Bill Gasiamis 25:42
Pushback, because I’ve seen it where several people who I’m coaching are above the age of 60, and 65. And they are coming to me saying that I wasn’t offered particular services, because they didn’t see that I could have a full recovery, or recover well enough to justify the costs of rehabilitating me.
Patrik Hutzel 26:06
Well, I can give a very real example, I had an inquiry from a client here in Melbourne, maybe three months now would have been around March this year, who had an 80 or 82-year-old mom go into a hospital into a well-known Hospital in Melbourne, with a stroke with an acute stroke.
Patrik Hutzel on age discrimination in stroke treatment

Patrik Hutzel 26:26
And the hospital there was telling the family from day one, we’re not going to treat the stroke, the only thing we can offer is palliative care. Unfortunately, the lady passed away within a few days after the diagnosis without having ever been offered proper first-line treatment for the stroke with an ischemic stroke, for example.
Patrik Hutzel 26:50
And this was an ischemic stroke, could include thrombolysis, you know, I’m sure you would be familiar with that, you know, has been refused right? Now, they only found out about our service when it was too late. So we didn’t even have the chance to advocate for her because her thrombolysis needs to be done within a few hours.
Patrik Hutzel 27:13
So it’s certainly something that we are seeing across the board. And the older someone is when they have a stroke, the less likely it is that hospitals will push towards end-of-life care palliative care, or just symptom management, rather than looking for a cure.
Patrik Hutzel 27:32
And in my mind, that is discrimination. Because you know, with your story, yes, you have a higher chance to recover when you’re younger. But that doesn’t mean you don’t have a chance to recover when you’re 77, or even 87, you haven’t even tried.
Bill Gasiamis 27:47
Exactly right. And the thing about it is nobody can predict the future. Not even doctors might have statistics that suggest certain things, they might use a bell curve, and most people might fall in that part of the statistical data. And then there’ll be some outliers. And that’s okay, but they don’t know who you are yet. They don’t know which part of the data you will stick to and fall into.
Bill Gasiamis 28:10
And that’s the part that frustrates me is that they make decisions on people but they don’t know, the person that they’re dealing with, as you know, how their future may unfold. Especially if well, they could probably predict how the future will unfold. If they refuse to support that person, if they refuse to provide medical care, that will predict the way that person’s future will unfold.
Bill Gasiamis 28:35
But if you do provide the medical care, there’s a good chance that you’ll improve the person’s outcomes, you’ll get them a result, and they will be able to rehabilitate themselves to a certain point. And yes, in some cases, if the damage is too large, and the person is in their 70s, or the 80s, yes, they may not have enough time ahead of them to achieve the type of recovery that you would like.
Bill Gasiamis 29:02
But that’s a different situation, that’s a situation where perhaps scans, etc., do show certain levels of impairment that you don’t have enough time in front of you to rehabilitate. Now, even then, it doesn’t mean that services should be discontinued because every person is a loved one. Every person is cared for every person is required and necessary to be around. And I don’t believe that we should just take the word of doctors for the gospel and not question it.
Patrik Hutzel 29:44
I could not agree more with you Bill because every life is worth living and with the work that we are doing one thing that we are hearing all the time and I’m sure that our viewers and listeners will concur with that. The doctors always say well, even if your mum or dad or whoever it is will survive, they won’t have any quality of life.
Patrik Hutzel 30:05
Well, what is the quality of life? That’s a perception. It’s not more than that, you know, what is acceptable for you is quality of life may not be acceptable for me as quality of life and vice versa. So it’s a very subjective measure. It’s not an objective measure, it can’t be measured objectively.
Patrik Hutzel 30:24
The other thing that I think is important to mention here, you know, the medical community looks at that, quote, unquote, stroke. Whereas the family looks at it, well, this is my mum, this is my dad, they lived a full life until now, and they’ve overcome challenges before, I will not have that stroke, stop my mum or my dad from overcoming another challenge.
Patrik Hutzel 30:48
But it’s a very, very isolated view that often hospitals and the medical community take looking at a diagnosis without looking at the whole person at the whole family. You know, what have those people overcome in the past, and so forth? What’s your take on that Bill?
Bill Gasiamis 31:09
My take is, you know, your family member better than anybody. And, the doctors are there to care, they are there to provide support and services, etc. But they are limited to what they can do by governments, by funding by budgets, etc. And they’re just trying to meet all the criteria. And then they’re trying to also meet the regulations and the bureaucratic criteria that they need to meet.
Bill Gasiamis 31:41
So they are kind of stuck in the middle. And most doctors, when you push back, do kind of what I’m not sure if the word is like, accept you’re pushing back, but they do. Well, they will reconsider, they will negotiate, and there will be a path forward for the person who pushes back on a doctor’s suggestion or decision.
Bill Gasiamis 32:04
The result is that most medical facilities cannot decide on the path forward of a person without the family members or the people who are advocating for that person who’s in the hospital without their consent.
Bill Gasiamis 32:21
So it’s really important that, if you can’t have the conversations yourself you do call somebody else into the conversation on your behalf. Because it’s an emotional time, you’re less likely to make the right decisions, perhaps you won’t make rational decisions.
Bill Gasiamis 32:42
And when you’re confronted with a supposed medical expert like a doctor, it is common for us to take their word for the gospel because we elevate them to positions of power and authority. After all, they deserve it to an extent.
Bill Gasiamis 33:00
But because of that, we feel sometimes that we can’t question their authority. And I believe that you must question their authority in my case. And if we can do it in a way that’s nice and gentle and compassionate for them because they are probably stuck between a rock and a hard place. In my case, I sacked my team of doctors, after my first stroke.
Bill Gasiamis 33:26
And I left the hospital that I was at, and went to another hospital because I did not feel that they had my best interests at heart. And I went and got a second opinion. When I got a second opinion, I felt that the people I was communicating with about my condition did have my best interests at heart, and I was going to receive a better level of care. So that’s exactly what I did. And I think that is something that caregivers and loved ones of stroke survivors can do to get a second opinion.
Patrik Hutzel 34:00
It’s such a critical point, Bill because that’s what we are doing all the time here. You know, we have families coming to us whether it’s, you know, after a stroke or any other condition, they say, well, the hospital is telling us tomorrow, they’re going to stop treatment.
Patrik Hutzel 34:18
And I say to them, okay, so will you just take this for the gospel, Oh but that’s what they said. And I said, Well, if they asked you to jump off a bridge tomorrow, would you jump off a bridge? Oh, no, we wouldn’t do that. So why would you? Why would you just go along to get along? You know, this is a once in a lifetime. situation. You can’t get it wrong.
Patrik Hutzel 34:22
You know, hospitals and doctors are extremely good at pretending they’re operating in a vacuum. Well, end-of-life and discharges to other hospitals and whatnot. It does not happen in a vacuum happens in a framework Right? But like you said, families or patients, put doctors and nurses onto a pedestal, you know what I refer to as perceived authority.
Patrik Hutzel 35:11
And of course, there is a level of authority. Of course, there is. But that authority needs to be used to the benefit of a patient and the family doesn’t need to be used to the benefit of the system. That’s my take. And we wouldn’t be in business with an intensive care hotline if there wasn’t a need for consulting and advocacy for people in need. You know, the minute our families bring an expert in, that can help advocate for them, the dynamics change and change in one phone call.
The seven questions to ask your doctor
Bill Gasiamis 35:46
They immediately change. Yeah, I found the same thing, I found that simply, for somebody to go to my website and download seven questions to ask your doctor after a stroke, it’s a free PDF that they can get from my website at recoveryafterstroke.com.
Bill Gasiamis 36:05
That is enough to begin a conversation with a medical professional that makes the playing field a little more even. It makes the medical professional engage in the conversation, rather than just give information about this is what’s going to happen, It makes them respond to the desires, the needs, the lack of clarity, lack of understanding that the caregivers or the stroke patient has.
Bill Gasiamis 36:05
Now when somebody is a stroke patient, I don’t have the cognitive ability to make medical decisions. Because I’ve had a stroke, my brain is injured. My wife had never dealt with anyone who had had a stroke before she’d never met anyone seen anyone. So she was and she’s not a medical person. So she was navigating this blind.
Bill Gasiamis 36:05
Now, if we had a tool that I could take to a meeting with my doctor, that would have made her life a lot easier. So that’s what that tool is, it’s a tool to start a conversation in a way that perhaps a nonmedical person like me, wouldn’t have been able to previously ask to start a conversation with a medical person about, I don’t have the words, I don’t know the language.
Bill Gasiamis 36:05
I don’t know the abbreviations. I don’t know any of that stuff. It’s overwhelming. So if you can just find a way to generate a normal conversation and share your needs and your requirements for your loved ones’ care, then that conversation takes a completely different path than it being one wire coming from the medical professional, and you’re just passively listening to it.
Intro 37:47
If you’ve had a stroke, and you’re in recovery, you’ll know what a scary and confusing time it can be, you’re likely to have a lot of questions going through your mind. How long will it take to recover? Will I recover? What things should I avoid in case I make matters worse, Doctors will explain things that, you’ve never had a stroke before, you probably don’t know what questions to ask.
Intro 38:12
If this is you, you may be missing out on doing things that could help speed up your recovery. If you’re finding yourself in that situation, stop worrying, and head to recovery after stroke.com where you can download a guide that will help you it’s called Seven Questions to Ask Your Doctor about Your Stroke.
Intro 38:31
These seven questions are the ones Bill wished he’d asked when he was recovering from a stroke, They’ll not only help you better understand your condition, but they’ll also help you take a more active role in your recovery. Head to the website. Now, recoverafterstroke.com and download the guide. It’s free.
Patrik Hutzel 38:51
One thing that I keep saying to my audience over and over again, and I believe it applies to your audience is that the biggest challenge for them is that they don’t know what they don’t know. They don’t know what to look for. They don’t know what questions to ask. They don’t know their rights, and they don’t know how to manage doctors and nurses in those situations.
Patrik Hutzel 39:15
I have no idea. And I do believe the very same applies to your audience. You know, they don’t even know where to start and you putting out this pamphlet or this white paper, whatever you want to call it is a starting point. You know, I have a similar white paper on my website, the Instant Impact Report.
Patrik Hutzel 39:32
It’s a guide for families in intensive care very similar to Okay, Where Do You Even Start when You are Completely Overwhelmed by What’s Happening All Around You You know, I can only recommend it for everyone who is faced with a stroke, you know, to go to Bill’s website at what’s your website again Bill?
Bill Gasiamis 39:53
recoveryafterstroke.com. And one of the things I’d like to add, Patrik is that asking your doctor The question for example, what else do I need to do for my loved one, other than the services that you’re providing? Might be a good way to start the conversation and get you thinking about what else can be done. Who else can I speak to?
Bill Gasiamis 40:15
What other tests do we need to do those types of things? And one of the main things that I think was somebody who’s had a stroke or a neurological injury, traumatic brain injury is to get an evaluation from a neuropsychologist, so it is a psychologist. So it’s not like psychological counseling. It is a psychologist who will assess the deficits that that person who has experienced the stroke is experiencing and must recover from.
Bill Gasiamis 40:46
And with a neuropsychologist’s report, you will be able to direct the resources of the recovery much more efficiently because you will know specifically where in the brain that injury is, and what rehabilitation needs to be. What steps towards rehabilitation need to be taken? So asking simply for a neurological assessment or neuropsychologist assessment will change the way that the recovery, resources are applied to the person’s recovery. Rather than being haphazard, they can be more focused and more targeted.
Bill Gasiamis 41:25
Can you see the comment from Laurie, can you see that?
Patrik Hutzel 41:27
I can’t.
The difference between a stroke victim from a stroke survivor
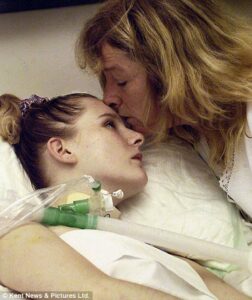
Patrik Hutzel 41:28
I’ll read out the comment from Laurie here who says I’m four years post hemorrhagic stroke and never recovered. Also, I consider myself a stroke victim, not a survivor.
Bill Gasiamis 41:45
Well, that’s a really important distinction to make. So if you’re a stroke victim, you’re in a situation where you’re allowing what’s happened to you, to impact you negatively, and only in a negative way. If you’re a stroke survivor, you’ve already overcome one thing, you didn’t die from the stroke. So we have already overcome a very big challenge.
Bill Gasiamis 42:12
And as a survivor, you are being guided to help you look for solutions to problems, because that’s what we generally need to be. Stroke creates many, many, many problems. If you always focus on problems, you will get more problems. If you focus on solutions to problems, you will get more solutions.
Bill Gasiamis 42:36
As a survivor, a survivor needs to focus on solutions, A victim will not be able to change their mindset to focus on solutions, they will focus on all the reasons why this happened to them. What did I do wrong in a past life? Why has God punished me? None of that is useful for improving your outcomes for a good recovery. So maybe, hopefully, that is a way now that she’s heard the term survivor. Maybe that’s a way to just change the conversation in their head about how to go forward.
Patrik Hutzel 43:13
Already. I think that’s that’s Laurie. Thank you for the comments, Laurie. But I also want to acknowledge you know, what Bill said, but like Bill said, you know, we’re already changing the conversation here. Yes, up until today, you’ve considered yourself a stroke victim. But now you are already seeing that you can look at your situation differently, that you are a survivor. And change the conversation around stroke, change your mindset around stroke. Bill, are you familiar with Dr. Joe Dispenza, as well?
Bill Gasiamis 43:44
I’m familiar, but not intimately.
Patrik Hutzel 43:48
Right, right. Look, I’m not familiar with it intimately either, but I have watched some of his videos on YouTube. Laurie, I would also like to point you to Bill’s work. I would also like to point you to Dr. Joe Dispenza’s work, just type into Google Dr. Joe Dispenza.
Patrik Hutzel 44:05
He I believe is doing some groundbreaking work with helping people from all walks of life with overcoming their limiting mindsets, but also their limiting condition. So I encourage you to look at Dr. Joe Dispenza’s work as well. Bill, coming to your book, tell us about your upcoming book. You know what’s in the book, what do people get? Why have you written it?
Why the stroke is the best thing that ever happened to Bill Gasiamis
Bill Gasiamis 44:32
Okay, it’s a strange title. I said that at the beginning, right? The long title is The Unexpected Way That The Stroke Became The Best Thing That Happened To Me. That wasn’t the case at the beginning of what happened in the podcast while I was speaking to people and interviewing people about their stroke journey.
Bill Gasiamis 44:53
I found myself a couple of times accidentally slipping out of my mouth saying, “I think this is the best thing that happened to me” and then I got curious as to why. Why is it the best thing that happened to me? I’m living with daily deficits, my balance isn’t the best, and my numbness is on my entire left side.
Bill Gasiamis 45:12
I’m not as physically active as I used to be. I have pain, I have muscle stiffness, I have cramps, I have all these things that I never had before. And yet, I still think that stroke was the best thing that happened to me the reason is, is that I’ve had a very huge personal development experience where I’ve grown personally from this situation.
Bill Gasiamis 45:35
And one of the ways that I grew was my mindset was all about finding solutions, you know, recovery, recovery, more, not problems, just solutions, just solutions. So I had an amazing mindset. And then, when I didn’t have answers to some of those questions, I reached out to other stroke survivors. And they filled me in on some of the things that I didn’t know that I needed to know, that helped me with my recovery.
Bill Gasiamis 46:04
One of those things was my take on nutrition, what I thought was healthy, which wasn’t. So in that, I then found that there is a community of people that for the first time in my life, truly, deeply understand me, or the stroke survivors who have had a stroke, really relate to me, and understand what I’m going through. And that was a unique and rare thing, I’d never come across people who related to me so deeply, and I relate it to them.
Bill Gasiamis 46:31
And I thought that was amazing. So I grew this group of people that deeply understood me. In that time, I discovered the benefits of improving my sleep. I then discovered the benefits of changing my nutrition. I then discovered the benefits of exercise, even though I wasn’t able to exercise the same way as before, any type of exercise is beneficial.
Bill Gasiamis 46:56
And then I discovered that I needed to do something to help other people as I was being helped, I found that helping other people was helping me and helping them. So I discovered that this might be one of my goals, I might have discovered my purpose in that the podcast was begun so that I can connect with people who can help me but then it’s helping them.
Bill Gasiamis 47:22
And then they are telling me that strikes the best thing that happened to them because of how they’ve had personal growth. I’m saying the same thing. And then I wanted to know what was what did we had in common. How did we all get there to this point where we can say a stroke is the best thing that happened to us? And it’s not what I expected. But what came from it was 10 things that these people had in common.
Bill Gasiamis 47:44
And, and many people say that strokes are the best thing that happened to them. Many people say that cancer is the best thing that happened to them and the heart attack they had was the best thing that happened to them and all these strange people say that their medical condition was the best thing that happened to them.
Bill Gasiamis 47:58
So anyway, the 10 things they had in common briefly, or that they had a recovery mindset. They had an emotional intelligence upgrade. So they connected to their heart, and they found a way to mend their relationships and improve their relationships. They made access, they access the gut and the gut-brain by taking steps to upgrade their identity and choosing to label themselves in a different way than I’m just somebody who goes to work. I’m a father, I raised children, and they enhanced their identity.
Bill Gasiamis 48:36
And they became more than just the labels that have given themselves. They improve their sleep, they improve their nutrition, and they become more physical. They started a meditation practice to go inside, focus on their breathing, calm themselves, and learn about what’s happening inside their body. They discovered their purpose by doing things for other people and supporting other people. And at the same time, they found a supportive community that deeply understood them.
Bill Gasiamis 49:03
Now those 10 things that they did became the chapters. In my book, I discuss a story at the beginning of each chapter of one of the people who I interviewed for the book. And then we go into emotional intelligence, for example, would describe what it is a little bit of scientific history and background into that, how it applies to life, and how you can improve and upgrade it.
Bill Gasiamis 49:26
So it’s like a how-to do the steps to get to the point that strike is the best thing that happened. And I’m not saying for one minute, that it’s the best medical thing that’s ever happened. I’m not saying that at all. I’m saying it’s a possibility for post-traumatic growth, and post-traumatic learning, and, and just a different way of seeing things in life. And that’s basically what I experienced.
Patrik Hutzel 49:52
That’s amazing Bill. And I think that’s also it’s amazing and it’s very encouraging because you know if you can look thank God, I’ve been pretty healthy all my life, you know, thank God for that. But any challenge that has been thrown at me on a personal or professional level and you can overcome it is the best thing that can happen to you.
Patrik Hutzel 50:13
It is because you can show you can overcome it, nothing really can faze you, you know, and I can see how you would take that perspective now. But it also takes a lot of courage, I believe, to look at it that way, and to share that with the world. And I hope that anyone who’s watching this or listening to this, you know, can overcome their challenge as well. And I know that Bill can help you with that, Bill’s book Bill’s podcast, you know, he’s done it. That means you can do it. You know, there’s no question about that.
Bill Gasiamis 50:54
I believe so. Look, in the podcast episode that is going out on Monday. So tomorrow, I interviewed Clara Woods, she’s an amazing young lady who experienced a stroke in her mother’s womb before she was born. And now Clara is 17. She has become an artist. She has exhibited in the United Kingdom, in Florence, Italy, and Japan, and now is attempting to set up an exhibition in New York.
Bill Gasiamis 51:27
Now, these are a family of people who have had to live through a perinatal stroke and the impact that that has caused to their daughter. As a result of that Clara is not verbal, she cannot speak but she understands three languages. She has become an artist, and she has had an exhibition. And she is not meant to be doing any of those things.
Bill Gasiamis 51:52
Doctors told the family that she was going to be in a vegetative state. So I would encourage anyone listening to just go to the recovery after stroke podcast, and listen to any one of those 265 episodes, especially Clara’s one tomorrow, because it’s my favorite episode so far. And just get a little bit of an understanding of how thinking differently can completely and change your life for the better and improve your life, even after a stroke.
Patrik Hutzel 52:30
If I had $1, for every client that we worked with, over the years where, you know, ICU teams have told them oh they won’t survive, they’ll be in a vegetative state for the rest of their lives. And the minute you challenge this, or you keep going regardless, things will change over time. Now I would you know, there’s always patients that don’t survive, but it’s the minority.
Patrik Hutzel 52:52
You know, it’s the minority. You and I wouldn’t be here today if our ancestors hadn’t overcome many challenges during times when there weren’t even hospitals. You and I wouldn’t be having this conversation today if our ancestors hadn’t been incredibly resilient, without all the bells and whistles that we have today.
Bill Gasiamis 53:17
Indeed, we are living in the best times ever, If you’re going to have a stroke, there have never been more resources to support your recovery, you just have to look for them. And you have to know where to find them. Hopefully, what I’m doing is supplying some of those resources and helping people find the resources that they need.
Bill Gasiamis 53:37
And I’m a bit of a connector. It’s what I do. So I live in Australia, in Melbourne, but I have connected people in New York, who have had a stroke and need to talk to another stroke survivor. I mean, it’s weird that I’m doing that from Australia. But if you know who to ask, you’ll be able to find people to support you.
Patrik Hutzel 53:55
Bill. You know what I’m I believe that the viewer said we’re having a probably mainly in the US that the viewers are alive here now, probably mainly in the US. I mean, I know you are talking to people in the US, I’m talking to people in the US every day. So what we’re doing here, even though we’re both in Melbourne, what we’re doing here is addressing a worldwide issue.
Bill Gasiamis 54:19
You nailed it, Patrik. That’s what I found one of the misconceptions that I had before I started this journey was that we’re all different and that different things happen. And we react differently. We have different needs and different requirements. X, we’re all pretty much the same. Everyone wants to be well healthy, and looked after they need resources to encourage them to recover. And they all need community.
You’re not alone – Bill Gasiamis
Bill Gasiamis 54:44
They all need support. Everyone is the same no matter which community you come from, what your religious background is, or what your ethnicity is, it doesn’t make a difference. everybody’s the same. So I’ve been pleasantly surprised by that. And I love the possibility that my upbringing in Melbourne is going to be good enough to support somebody who’s going through stroke recovery in Canada, in the United States, in New Zealand, in Mexico, in Italy, in Dubai, wherever they are.
Bill Gasiamis 55:19
It makes no difference so, yeah, and what that hopefully does is make people not feel like they’re going through it alone. I’m the only one that this has happened to. And nobody knows what it’s like. You’re not the only one. And absolutely, people know what it’s like, and they relate to you.
Patrik Hutzel 55:39
Absolutely. And look, just by the comment from Laurie, you know, obviously, by what we’ve discussed today, Laurie could already relate to it. And, Laurie, I hope that just by you coming on to this to this show, you know, hopefully, we can change your perspective. In your situation going forward, you will be a survivor, not a victim, you now have the tools, and resources at your disposal.
Patrik Hutzel 56:05
What to do next. You know, change, change your outlook trends change your perspective. Bill, we got to wrap this up in a minute. We do have time for one more quick question. We can quickly get to that if anyone wants to type in another question. But Bill, where can they find your new book, if people are interested?
Bill Gasiamis 56:25
So if they go to recovery after strike.com, that’s going to be the best place to get updates on the stage of my book. It’s not out yet it’s been edited. And now we’re doing the final layout. And we’re just putting it together and making a book for the first time. I’m not sure how long that takes, my editor is in charge of that and my publisher, so that’ll happen in a little while.
Bill Gasiamis 56:45
But if they just go to recoveryafterstroke.com and subscribe to the podcast on iTunes or Spotify or Stitcher or wherever they get their podcasts from, I’ll update people regularly. And soon, but not yet, I will release an opportunity for people to download the first chapter of the book for free. So they’re just going to keep coming back to recoveryafterstroke.com and checking in there, just so that they can be notified as soon as that’s a possibility.
Patrik Hutzel 57:16
That’s amazing. Thank you so much, Bill. Appreciate you coming on to the show and sharing all of your wisdom with my audience.
Bill Gasiamis 57:26
My pleasure.
Patrik Hutzel 57:28
Great, great. So thanks, everyone for coming onto the show and for watching the replay. Now if you have a loved one in intensive care, go to intensivecarehotline.com. Call us at one of the numbers at the top of our website, or simply send us an email to support us at intensivecarehotline.com with your questions.
Patrik Hutzel 57:48
Also, have a look at our membership for families in intensive care at intensivecaresupport.org. There you have access to me and my team 24 hours a day in the membership area and via email. And we answer all questions intensive care related.
Patrik Hutzel 58:03
I also offer one-on-one consulting and advocacy for families in intensive care over the phone, Zoom, Skype, WhatsApp, or whichever medium works best for you. I also talk to doctors and nurses directly if that’s what you want. I also represent you in family meetings with intensive care teams. So that you have someone on your team that speaks the medical language.
Bill 58:24
Thank you so much for joining us on today’s episode. I hope you liked this episode, It was something different and gave you an insight into my thoughts on some of the topics that are seriously necessary for you guys to consider after a stroke. To learn more about my guests, including links to their social media and other pages, and to download a full transcript of the entire interview please go to recoveryafterstroke.com/episodes.
Bill 58:51
If you’d like to support this podcast, the best way to do it is to leave a five-star review and a few words about what the show means to you on iTunes and Spotify. If you are watching on YouTube, comment below the video like this episode and to get notifications of future episodes, subscribe to the show on the platform of your choice. Thank you again for being here and listening. I truly appreciate you see you on the next episode.
Intro 59:15
Importantly, we present many podcasts designed to give you an insight and understanding into the experiences of other individuals’ opinions and treatments. Protocols discussed during any podcast are the individual’s own experience and we do not necessarily share the same opinion nor do we recommend any treatment protocol discussed.
Intro 59:32
All content on this website at any linked blog, podcast, or video material controlled by this website or content is created and produced for informational purposes only and is largely based on the personal experience of Bill Gasiamis. The content is intended to complement your medical treatment and support healing.
Intro 59:49
It is not intended to be a substitute for professional medical advice and should not be relied on as health advice. The information is general and may not be suitable for your injuries, circumstances, or health Both objectives do not use our content as a standalone resource to diagnose, treat, cure, or prevent any disease for therapeutic purposes or as a substitute for the advice of a health professional.
Intro 59:49
Never delay seeking advice or disregard the advice of a medical professional, your doctor, or your rehabilitation program based on our content. If you have any questions or concerns about your health or medical condition, please seek guidance from a doctor or other medical professional. If you are experiencing a health emergency or think you might be, call 000 if in Australia or your local emergency number immediately for emergency assistance or go to the nearest hospital emergency department.
Intro 1:00:34
Medical information changes constantly. While we aim to provide current quality information in our content. We do not provide any guarantees and assume no legal liability or responsibility for the accuracy, currency, or completeness of the content. If you choose to rely on any information within our content, you do so solely at your own risk. We are careful with the links we provide however third-party links from our website are followed at your own risk and we are not responsible for any information you find there.







