Overcoming foot drop thanks to some amazing technology has inspired Emily Knosher to join the board of the Freedom To Walk Foundation.
Socials:
www.instagram.com/knosher_average_recovery/
www.instagram.com/freedomtowalkfoundation/
freedomtowalkfoundation.org/
Highlights:
02:09 Introduction
02:35 Brain Tumor
10:58 Having A Positive Recovery Mindset
18:27 Conversation Before The Surgery
24:35 Seek The Right Kind Of People
27:15 The Six Months Deadline
36:42 Coming Home After Rehab
42:29 The Small Steps
47:32 AFO For Foot Drop
50:07 Running A Marathon With A Foot Drop
53:57 Freedom To Walk Foundation And Bioness
1:03:14 Meeting People With Foot Drop
1:12:37 Repurposing Walking Aids
Emily 0:00
But I didn’t know anybody when it happened to me right? Until I started looking online.
Emily 0:07
I lose my train of thought sometimes. Which we probably all go through the advocating for ourselves.
Bill 0:25
Let me take you it’ll come back to you.
Intro 0:44
This is the recovery after stroke podcast with Bill Gasiamis, helping you navigate recovery after stroke.
Bill 0:57
Hello and welcome to recovery after stroke a podcast full of answers, advice and practical tools for stroke survivors to help you take back your life after a stroke and build a stronger future.
Bill 1:09
I’m your host three times a stroke survivor Bill Gasiamis after my own life was turned upside down, and I went from being an active father to being stuck in hospital. I knew if I ever wanted to get back to the life I loved before, my recovery it was up to me.
Bill 1:24
After years of researching and discovering I learned how to heal my brain and rebuild a healthier and happier life than I ever dreamed possible. And now I’ve made it my mission to empower other stroke survivors like you to recover faster, achieve your goals and take back the freedom you deserve.
Bill 1:40
If you enjoy this episode and want more resources, accessible training and hands on support, check out my recovery after stroke membership Community Credit especially for stroke survivors. This is a clear pathway to transform your symptoms, reduce your anxiety and navigate your journey to recovery with confidence.
Bill 2:00
Head to recoveryafterstroke.com to find out more after this podcast. But for now let’s dive in to today’s episode.
Introduction

Bill 2:09
This is Episode 146. And my guest today is Emily Knosher who experienced a bleed in the brain age 25 due to complications from brain surgery, Emily has learned to overcome hemiparesis, foot drop, and many other challenges stroke survivors face.
Bill 2:26
Emily Knosher, welcome to the podcast.
Emily 2:29
Thank you very much.
Bill 2:31
Thanks for being here. Tell me a little bit about your story. What happened to you?
Brain Tumor
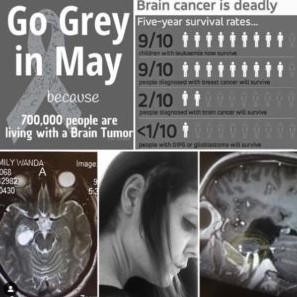
Emily 2:35
My brain injury happened when I was 25. It was 2015. I was in my fifth year of teaching public school. I was a chorus, teacher, and piano and theater and all the active stuff. I was even coaching on the cross teams.
Emily 2:52
Because the girls were just desperate. I guess they found that I played the cross. So they knock on the door, the chorus teacher to do that. So I did but I wasn’t heavily involved in a lot of stuff.
Emily 3:02
And one night, I was going to sleep. And the next thing I know I woke up. And my fiance at the time, told me I had a seizure. A grand mal seizure a big one.
Bill 3:15
He noticed you were having a seizure. And the first time you found out about it was when he told you?
Emily 3:22
Yes, so it happened in my sleep or right as I was going to sleep or something, but I was definitely unconscious. And that was scary, so you know, I wake up, and there’s just EMT in my room.
Emily 3:37
And they’re taking me to the hospital. So they did a CT scan. And for me, my story is a little unique. I actually doctors told me I had a brain tumor in my temporal lobe on my right side.
Emily 3:51
And it was that night where it looked really big on the scans. And the neurosurgeon was like, I’m just gonna take that out the next morning, right? So I went under for a brain tumor resection and during the surgery at some point or they mentioned shortly after they closed me up or something they’re not sure.
Emily 4:12
I had a hemorrhage. And I woke up paralyzed on my left side a lot of brain fog, a lot of confusion. Nothing was right. So I relate to the stroke community. I know. It’s not exactly a lot of strokes are different.
Emily 4:35
It’s not the typical experience. But the experience it seems that we all share is the being one person and then waking up the next day and being someone totally different.
Bill 4:49
Yeah, It’s really interesting is that you relate to stroke survivors. The thing is, I went for about nearly three years. before somebody said to me, you’ve had a hemorrhagic stroke, because it wasn’t typical.
Bill 5:06
And because a bleed is not considered an ischemic stroke, it’s not really dealt with in the stroke ward, in the same way it’s dealt by a different specialists group of people. They kind of don’t tell you that what’s happened to you. It’s different from a blockage or ischemic stroke or a blood clot in your head or whatever.
Bill 5:29
But it makes you feel the same, and you have the same impact and your brain goes out of action in a similar way, and then you have to recover in a similar way. No one did tell me any of that.
Bill 5:39
So I felt like you and I was kind of wondering like, did I really have a stroke? Or didn’t I like, was it the same? Can I say that? And it turns out that it was a hemorrhagic stroke. And that’s the best way that they can describe it.
Bill 5:55
But it’s not dealt with in the hospital by the same group of people that deal with the ischemic strokes and makes kind of sense, because we’re dealing with blood vessels that have burst rather than rather than a blood vessel that’s blocked.
Bill 6:11
Now, the tumor was that the first time that you sensed that there might be something going on in your head? Did you ever get massive headaches or, you know, all those challenges?
Emily 6:25
So something I do like to speak about, on the rare occasion I get to, is that I was experiencing short focal seizures for years, but we didn’t know what it was and pediatrician didn’t know what they were.
Emily 6:45
So what my pediatrician told me was that they thought they kind of miss diagnose it as a headache. Right, you’ll hear headaches or seizure you have any kind of seizure activity can be very diverse way of presenting itself with brain tumors, or any kind of seizure activity.
Emily 7:06
And my mother had a history of migraines. So my pediatrician at I think 17 or so said, oh, they’re probably just mini migraines. And so for me, it felt like I knew they would come on because I had an aura.
Emily 7:21
And they lasted nearly 30 to 60 seconds, I would feel like a warmth wash over me from the top of my head down. And I would have a little involuntary muscle movement, like swallowing was the thing I get kind of hot.
Emily 7:35
And then it would go away. I was driving through these. I was teaching through these at 25. I just lived with them for years just thinking oh, I’ll get migraines one day, that was the only sign that I have this tumor growing larger and larger in my brain.
Emily 7:51
Until finally, it presented with a grand mal seizure just out of the blue and I’m really lucky and really blessed that it happened in my bed on a soft surface with someone with me, because that’s not the case for everybody.
Bill 8:05
No. How big was achievement by the time it was discovered?
Emily 8:10
It was about the size of a golf ball. I have a few scans I post every year on my Instagram that assigns a golf ball. It’s a pretty rare tumor. It’s called the ganglioglioma. Mostly benign, but mine happened to be a grade two, just a little more aggressive.
Emily 8:28
So but because of the nature of it, and how big it was, and how close to the surface of my skull, it was I suppose the neurosurgeon was like, let me just get it. Let me just go in there and take it all out.
Emily 8:41
And what do I know? I’m scared. You know, nothing. When you get to hospital and someone gives you bad news like that. Nobody wants a brain tumor. So you’re like, do whatever you got to do to get it out of me. And so it goes, oftentimes, I do want to say, through my own healing and research, brain surgeries aren’t a death sentence.
Emily 9:03
They don’t typically happen the way it happened to me, there are plenty of safe and fine brain surgeries that happen and the patient just walked out the next day. I’ve actually had two so my second one went fine. But yeah, but to me, I was a little I’m lucky.
Bill 9:22
Not that you’ve got a door there that they can just open whenever they feel like and go in.
Bill 9:26
Wouldn’t that be nice.
Bill 9:30
Did they go in from the same spot? Or was it a different spot?
Emily 9:32
It was the same spot because it was a little regrowth of the same tumor five years later. Another shock but teeny tiny they had to go in there and get it. But believe me, I held my same neurosurgeon to the wall and he said, I can’t do it again, man.
Emily 9:49
Like I’m so inspired by you because you’ve had three experiences. And I have to tell my neurosurgeon like you’re not going in there. Unless you can promisee that’s not going to happen again, because I could do it once. I don’t know how I did it. But I know I can’t do it twice. So just know that.
Bill 10:09
That’s fair enough. He, or she?
Emily 10:13
He.
Bill 10:13
Yeah, my neurosurgeon was an amazing lady. She was the second neurosurgeon that I consulted with and when I met her in, so it happened in 2012. Then it happened in March 2012. And then it happened in 2014, in November 2014.
Bill 10:31
And when I met her, in November, 2014, she came up to me, she says, Are we going in? That’s it, we’re getting it out. And then I said, Okay, you know, whatever, Kate, you do whatever you like, you know.
Bill 10:41
And by now I was over it, I just wanted it out. And then I said to her, and then she came back and said, are we going to take it out? Is that what you want? And I said yes, please, please, I trust you do whatever you got to do, and I’ll deal with the stuff that happens later, whatever happens happens, you know.
Having A Positive Recovery Mindset

Bill 10:58
And I was good, I didn’t do the fear. I didn’t do any of that stuff. I was really, really well prepared emotionally and mentally. And physically, I had just decided that it was going to be an experience that I was going to have, and I was going to just deal with anything.
Bill 11:18
I’ve never been so focused and so comfortable with somebody opening up my head, you know, ever like it was just so amazing. And the issue for me was that when I woke up, I had left side numbness, so it wasn’t paralysis, per se, but it was more sensory neuron issues.
Bill 11:44
Therefore, the neurons are kind of a little bit sleepy, they don’t know when my foots on the ground, I don’t know where my hand is in space, and all that kind of stuff. So I had to learn how to walk again, and all that kind of stuff.
Bill 11:55
And I’ve got a little bit of left side atrophy and all the stuff that most people had a stroke talk about with one of their sides. And for me, I didn’t even think about it for a minute as if I shit now I’ve got this atrophy stuff. It’s like, Okay, this is just the next part of the process.
Bill 12:16
This is just the next thing that I have to get through and overcome. I’ve never thought about, I can’t walk again, I never thought about I might not walk again. It just did not enter my mind. It was just like, what’s the next job? This is the next job I get on to it. Let’s get that done.
Bill 12:30
So perhaps I would have had a different outcome or outlook if I did end up being permanently in a wheelchair or for a longer period of time. But I don’t know, it just didn’t occur to me. When you were preparing for that second surgery. I know you put him up against the wall on that. But what were your feelings, saying and doing to you like? What was the feeling like?
Emily 12:58
So something I think we have in common, which I like about you is the acceptance, but also a little bit of the kind of fed-upness with what resources we have out there, which are very limited.
Emily 13:12
And just being in this position. And we really have to advocate for ourselves to get anything done. So the first time was surprise and grief happened years went by five years went by I didn’t expect to have a recurrence of the brain tumor, right.
Emily 13:30
So that was a big shock when I got the yearly scan and they saw a little something. I was very cool in the same kind of way you’re describing because it’s like, well, I guess I’m just a brain tumor person. I didn’t avoid it, I almost avoided that. But if that’s just not my path, now I need to monitor it for the rest of my life.
Emily 13:51
Like that kind of gravity hits you. But what do you do? You know, like, that’s just how it is. And again, through all of this, I’ve found myself and with all the stories shared online, I’m so grateful for Instagram, which is a funny thing to say. But I had no I didn’t know anybody when it happened to me right until I started looking online.
Emily 14:15
I lose my train of thought sometimes. Which we probably all go through the advocating for ourselves.
Bill 14:34
Let me takeover, it’ll come back to you.
Emily 14:36
I knew this would happen. We’re just dealing with it. At this point. We find a place of peace with it. So I was fueled that way. I went to I’m now a cancer patient. Oh, that’s what I was gonna say, I feel so lucky, after hearing everybody else’s stories, that I still feel like I got it a little better than others.
Emily 15:18
Maybe because my brain tumor is practically benign. It’s not an aggressive cancer, it could always be worse, right? So, always remembering that and realizing that I was given this because I can manage it, kind of as a perfect person to give this stuff to.
Emily 15:41
That’s what kind of hit me the second time that I realized that I have to have my brain cut into again. And however, when I did leave the consultation, because I was at the consultation, I saw that man for the first time in years. And yeah, we never really talked about it. I don’t know if that happens to other people.
Emily 15:59
But your neurosurgeons, if something goes wrong. Sometimes we don’t hear a lot about what happened. And you’re kind of left to wonder, and I didn’t get closure for a long time until that day. Like we’re not there anymore. Like if you’re gonna go back in there, I need to trust you.
Emily 16:15
So in consultation with my mom and dad. I was like, okay, what’s going to happen? Blah, blah, blah, like, how are we going to do it? And then when I drive home from the initial MRI, when they’re getting ready to map out my brain surgery, I have a complete freakout.
Emily 16:29
All the walls crap crumble down. And I was like, how could I possibly let someone into my head? Like are there possibly other options? I can’t like what if it happens again, I was scared. I had a big freakout moment, I think I was just crying on the drive home.
Emily 16:46
So that’s what I called him and not sleeping backwards advocacy thing. Because it’s really unfair that neuro patients don’t really get an in-depth explanation to what is about to happen to us. What did happen to us, right?
Emily 17:04
So before I told him, I was gonna rip that surgery off the schedule. Unless he treated me with the same respect as what a colleague and explained to me with technical terms where he’s getting into, I mean, you know, like all of us stroke survivors are basically neurologists, at this point, we are brain experts, we can be doctors.
Emily 17:25
Like, it’s not like we’ve studied ourselves, because nobody tells you anything. So I was like, you’re gonna use technical terms, I want to know where you’re cutting in, I want to go beginning to end process, I want you to tell me this part of the brain, nothing happens there.
Emily 17:37
Like what, you know, if it were to bleed again, what am I looking at? And he respected that. He walked me through it, just like a med student. And he confirmed that that little interior part of my temporal lobe basically has no purpose. So if something were to go wrong, there’s like no chance it can bleed somewhere else.
Emily 17:59
So I’m like, okay, we’ll do it. But that’s the confidence and like the power I’ve come to build over time, with not getting any answers in the medical community much. you’ve explained in other podcasts like you feel like nobody, like people don’t know what to do with you. Half the time, there’s not the resource that we need. Especially if you’re a young stroke survivor, we just thrown for a loop.
Conversation Before The Surgery
Bill 18:27
Because it’s all the people dealing with you. And when you’re a younger stroke survivor, they can’t relate. Most of them are neurosurgeons and doctors, they can’t relate to normal people anyway.
Bill 18:39
Almost impossible to relate to a young patient, you have to be a really unique person, you know, my surgeon, what you just described that you needed is what I needed. She had me an hour before I was in surgery, in the room in the consulting room with all her team, all the guys and gals who are going to cut me open at some way shape or form.
Bill 19:03
And asking them in front of me with my scan on the screen. Show me where the entry points gonna be. And the guy, one of the guys goes here, and then she goes no, and hits him, like gives him the elbow and he goes, no, that’s not the entry point. We’re not going in through there.
Bill 19:23
We can’t go there if we go through there, what are we going to get to or what’s gonna happen? And he’s freaking out in front of the patient and, you know, his colleagues and everybody, and he got it right. He fumbled through it and he got it right.
Bill 19:36
And I just looked at her and she looked at me, and I thought, Oh-oh hopefully she’s gonna be there telling him No, no, no, that you got to go around the corner go the other way. Don’t go that way.
Bill 19:46
So I got that was great. I had a insight into what they were doing, how they were doing it. What I didn’t know was, what the impact might be because of course, they can’t breathe. addicted, so they don’t really tell you. And then when I woke up, I realized that I had these issues.
Bill 20:06
And from the, the, and what happened to me was like, Hmm, I wonder that part of the brain and they’re part of the brain? What does it do ask the same questions that you asked.
Bill 20:16
And then I put that in a PDF. So somebody can go to my website and download and download a document, it’s free called Seven Questions To Ask Your Doctor About Your Stroke.
Bill 20:28
And it’s those questions that I wanted to ask, which was, okay, so, you know, where that stroke happened? What does that do to a person if they get affected there? And a couple of other questions.
Bill 20:39
So I feel like maybe there’s only that we’re unique, there’s not a lot of people that are as curious as we are, and need to know all the answers, I certainly have seen that lots of people just put all the faith in the doctors. And that’s kind of okay. When you’re not sure about how to approach things, perhaps, and you’re scared or whatever.
Bill 21:05
But I don’t trust people a lot, you’ve got to earn my trust. And if your approach is wrong, then I don’t care how gifted you are, and how amazing a surgeon you are, and how much they say you’re the best in the planet, like, I’m not going to rate you if I can’t trust you, I’m not going to rate you. So that’s my approach. It sounds similar to you.
Emily 21:29
I, I truly think those resources will make a big difference. Because I think it’s fear. It’s not always just, oh, maybe, you know, we just grew up more curious, or we read more books or something, you know, on our minds just go there.
Emily 21:49
But there is that? Well, I trusted my doctor too the first time because truly I know nothing at that point. You know, brain tumors are not on my list of things to research. So, but the fact that we’ve learned from that, and if we even have a one chance of changing somebody’s recovery, because we empower them to ask the right questions to not be afraid. Doctors are very intimidating.
Intro 22:16
If you’ve had a stroke, and you’re in recovery, you’ll know what a scary and confusing time it can be, you’re likely to have a lot of questions going through your mind. Like how long will it take to recover? Will I actually recover? What things should I avoid in case I make matters worse, or doctors will explain things.
Intro 22:35
But obviously, you’ve never had a stroke before, you probably don’t know what questions to ask. If this is you, you may be missing out on doing things that could help speed up your recovery. If you’re finding yourself in that situation, stop worrying, and head to recoveryafterstroke.com where you can download a guide that will help you, it’s called the seven questions to ask your doctor about your stroke.
Intro 23:00
These seven questions are the ones Bill wished he’d asked when he was recovering from a stroke, they’ll not only help you better understand your condition. And they’ll help you take a more active role in your recovery. head to the website. Now, recoveryafterstroke.com and download the guide. It’s free.
Emily 23:19
There’s some real sad stories out there of people that do not get the care they need. Because they don’t know how to ask they’re too afraid to ask. So I think it’s really important work you’re doing.
Emily 23:30
And that’s one thing that really breaks my heart connecting with other, you know, survivors online. Some people are right at right at Ground Zero. And I just talked them all night. Until you gotta do this, you got to do that.
Emily 23:44
Like don’t let them tell you that. Like, we just have to take what we’ve learned and give back because that’s really heartbreaking when someone falls through, you know, and you know, they could have had a good recovery.
Bill 23:56
Yeah, that mentoring kind of role is really useful. And that’s basically what I try and do now after stroke, because you very rarely get to speak to somebody, as they’re about to go into surgery or before surgery, you very rarely get to speak to somebody about that.
Bill 24:11
But I definitely feel like we need to mentor more people that are seeking support and answers because we know we’ve been there, right? So that’s what it’s for. So you know, I went into I was afraid and all that kind of stuff. But I went into my first few meetings with my doctors and said, these are not the right people for me.
Seek The Right Kind Of People

Bill 24:35
So I left that hospital six weeks after my first and second bleeds and I went into another hospital and I found somebody who did suit me who did speak to me the way that I needed to speak to. He taught me what I needed to know about my procedure rather than turn up at the end of my bed, talk about me and not involve me in the conversation.
Bill 24:57
It was just wrong and it was old school. And things are changing, and they’re moving on. So I feel like people that are listening to this who feel like they need to be more empowered, just seek it out, seek it out from wherever you can and don’t listen to people tell you things you don’t want to hear.
Bill 25:18
If you’re being ridiculous, and they’re telling you something that you have to hear, but you don’t want to hear it, that’s different. But if you’re not feeling them, you know, if they’re not your kind of person, don’t go down that path.
Emily 25:34
That’s very good advice. There have been a few times on my grief journey, you know, after 2015, where I’ve looked at other hospitals that have this new like, kind of brain surgery, this new device, or this whatever, they’re on the West Coast I’m in, I’m on the East Coast, you know, I’m like, oh, man, if I just said, can I think about it?
Emily 26:02
That night? Of course, that just wasn’t the environment I was in it was an emergency. He said, I’m going to take care of it in two hours. See you in the morning, you know, and we’re just at the mercy sometimes so. But if I knew, because I heard other people talk about this, then I might have said, like, I’m gonna think about is it gonna kill me tonight?
Emily 26:25
Like, well, but we don’t know. But if I could have had another minute, I wonder if it might have gone differently. However, I also regret nothing. Because I really have found the journey, irreplaceable, and I love where I am today.
Bill 26:45
Yeah, a bit weird journey to find the replaceable, you’re supposed to go on a trip to a beautiful island with crystal blue waters. That’s unbelievable and amazing journey.
Emily 26:59
We could still do that, though. With the right attitude.
Bill 27:04
Yeah, I love it. It’s really cool. So when you woke up from surgery, you had to overcome some physical deficits, what were they?
The Six Months Deadline

Emily 27:15
So I had just classically presented, hemiparesis face arm leg, everything on the left side of my body, my tumor was removed over on my right side here. So they noticed as I was waking up that I wasn’t moving. And I was transported to the nearest Rehabilitation Hospital.
Emily 27:43
And I spent a month there, just getting back on my feet. Walking came first, you know, they try to get you up on your seat. Which I also think my age made a difference, thank goodness. But I spent about a month in the hospital. And that’s where I learned other things that made me frustrated about hospitals and stroke recovery.
Emily 28:07
Like wanting the answers, then when you’re in rehab, and you’re learning about your new body, and you’ll have people telling you exactly what to do or what not to do. And you just trust them. And years go by for you and I right and I’m reading more things about the complete opposite that you could have tried. Or, you know, you’ve heard the dreaded six months deadline, right? Don’t you hate it?
Bill 28:37
I hate it with a passion. It’s so bad. What is gonna happen, you’ll probably be like that for the rest of your life. You’ll never walk again. All that stupid shit that your doctors say it’s just, it is pathetic. I can’t believe it. It still happens. It happens every day. If I make a post on Instagram and ask did your doctor last week say this? I’ll probably get a million responses saying yeah, they did. Don’t believe them.
Emily 29:04
Nothing is more depressing when you’re already dealing with. I don’t even know the word for what that is. When you wake up and you realize your body left you in a way and you suddenly can’t walk and it’s an it’s a? I don’t know. Maybe you have a word for it.
Emily 29:23
But I don’t um, but the depression sets in motion the shock? shock? Yeah. So nothing more depressing after the shock factor of someone telling you. Oh, by the way, if you don’t get better in six months, that’s all you’re gonna be. To which I’ve learned by example, and by seeing so many beautiful people just kick stroke strokes ass. Like that’s not the case.
Emily 29:49
Why is that still the narrative? And I’ve spoke on this a few times, like a few times when I ever get to share my story. I let people know that just the average crowd. That that’s what People with stroke or history, brain injury, anybody with paralysis get this death sentence, which is why I’m so passionate about helping people get up out of bed.
Bill 30:12
I tell people, don’t tell me what I can and can’t do. Please don’t give me your limitations. I’m not interested in hearing that. I’ve had other people who I’ve coached to have said that to their, rehab therapists, you know, and when they’ve referred to, for example, the arm has the bad hand or the bad leg, or as I don’t call it bad.
Emily 30:35
It’s fine it’s beautiful.
Bill 30:40
It’s what we’re working on things, but don’t call it bad it hasn’t done anything bad.
Emily 30:46
Gosh, I mean, there’s got to be a, they have to do better. You know, we all have to do better with how we talk to stroke patients.
Bill 30:59
Part of it is their own. Well, firstly, they’re not a stroke survivor. So I get that part they don’t understand what we’re going through. Secondly, they, just kind of, in order to understand what they’re doing is they’re saying a word, to get feedback for the word, they say, to understand like, how to try and approach the situation.
Bill 31:24
For example, you know, it’s like, it’s like, when you tell a child, it’s like, you tell the child, instead of hold the glass tightly. So it doesn’t fall, when you’re walking with it, you tell the child don’t drop the glass. And in order for the child to actually understand what the hell that means, because they probably never heard that conversation before, they have to drop the glass.
Bill 31:53
And now they know what don’t drop the glass means because they have to have the experience to be able to respond to it appropriately. So the people who are caring for us, they’re on the other side, I’ve never had this experience. They’re saying, Look, you’re not walking now.
Bill 32:11
And I hate to tell you, I don’t want to be the one to tell you. But I don’t want you to get disappointed in the future. But you might not walk again. That’s like, no, no, that might be the case. But still, you don’t need to tell that story, you don’t need to be the one who takes the responsibility to give me that information.
Bill 32:35
You need to say to me, that here are your challenges. And here is how previous patients have overcome them, and choose the ones that had a good outcome to set me up for a good outcome. Don’t choose the ones that didn’t have a good outcome, because they are completely different than me that are completely different strokes, they have completely different resources, all sorts of things. So don’t do that.
Emily 33:01
These words, that the doctors and nurses and physical therapists and some of them use, and of course, I have much respect for our nurses and doctors. And you know, they kept us alive, they changed my bed sheets and stuff. I love them. But the words the education, the continuing education on how far people go after stroke these days, like needs to be integral in the hospitals.
Emily 33:35
Because the more people I see or meet or talk to, especially when I see them not walking, yet, they’re still in a wheelchair because I want to get them maybe on board with the freedom to wealth foundation and get them a device or something. When I see that I talked to them.
Emily 33:52
And they just some people just take the sentence they’re given, you know, and maybe they don’t have the full family support, you know, carers have a hard time or maybe there are no carers. And I’ve talked to people young people like in a nursing home, because that’s the only option they had. And they think like that’s it for them because someone told them that.
Emily 34:18
And we have to undo that. Because you could have a device, you could not have a device, you could have medication, no medication, whatever, you could have access to anything. But if someone tells you like no, that’s the end for you. It doesn’t matter what access you have, because you’re not even going to have the spirit to use it. And it’s so heartbreaking.
Bill 34:38
Yeah, to not have to undo that that work. Then it is to set a very cool, lovely intention and a great possibility and provide hope. You don’t have to undo providing hope. But you do have to undo the shit that somebody implants that’s not real. And when the person as well is that their most vulnerable? They just came out of surgery. You know, they’ve got a hole in their head, you know?
Bill 35:09
Give them a bit of time to overcome some shit. You know, they just got out of surgery.
Emily 35:16
Absolutely. I’m so glad we can curse by the way, I’ve been holding myself back.
Bill 35:19
Yeah we can say a little bit of shit. This one is a real passion of mine like I do I get really frustrated about it that annoys the heck out of me. And I don’t to mince my words about it. There’s no point because people don’t appreciate, you know, when we’re being polite people think, Oh, he’s alright about it.
Bill 35:38
No, I’m not alright about it at all. I’m really annoyed about it, it happens too much. And it happens to too many people. And I’m here to tell you that you need to not do that. And it’s you that needs to change not that person that’s in the room, that’s there for you to help them.
Bill 35:54
You need to advance your intelligence, so that you’re a better therapist, so that you do not implant negative thought patterns of your own into your vulnerable patients.
Emily 36:10
100%.
Bill 36:11
And if I have to say shit, while I’m talking to you, I’m gonna say it. And if you get offended, that’s your problem. So that’s my little rant over. So yeah, okay, so you had to, you had to do a fair bit of rehab. So, you’re in rehab for a month, and then you went home was ir outpatient rehab? What was life like when you went back home? Because that was completely different?
Coming Home After Rehab
Emily 36:42
Well, I’m 25 years old, living in my own apartment or condo at the time, I went home to mom and dad. So that I mean, if I didn’t have my family for support and being the positive cheerleader, then I don’t know where I would be.
Emily 37:02
So I was very blessed to have that family. That was, you know, happy to go on with mom and dad and try not to think about that. I’m a 25 year old with a cane. And I just got the call every once a while my where’s my cane? It’s just funny. You gotta laugh.
Emily 37:16
Yeah, I mean, when you go home when I finally deem you, not a fall risk, right, I left with a cane. And I fo brace just the type of getting in the hospital, I got a better one and outpatient to start kind of walking a little more. It was a little stressful. My cares, my wonderful, sweet parents had to watch me 24 hours.
Emily 37:43
And I’m not in a good mood, of course, because there’s all sorts of things happening. I’m teaching. My goodness, I was like, What am I students doing right now? As if I needed to care? I didn’t need to care. But it’s in, you know, it’s ingrained in you of like, How can I be away from work this long.
Emily 37:58
So it was a lot of just being helped to the bathroom, being helping fed, going to outpatient rehab. And really just kind of understanding this new part of existence. I didn’t know how long it was going to take. I didn’t know. Everyday was kind of a, you just go through the paces right?
Emily 38:22
But something and I love to hear these stories about folks with their carers, is that for me, I was sick of it very quickly. I knew I could walk with a cane. So I’m like, what’s with this 24-hour watch thing. And pretty shortly, to my mother’s dismay, I was taking calculated risks for myself that I think you mentioned earlier, which is about kind of just empowering yourself trying things, to find out if you can do it.
Emily 39:01
That’s how we’re going to recover. It’s not by someone telling us what we can and can’t do. You have to find out for yourself in the safest way possible. I do. Even though, even though I like to say that I had a big dose of F this, I’m going to do what I want. I still made sure I was doing it either observed or safely, I wasn’t being too reckless.
Emily 39:22
So it wasn’t very long before I told my mom, I’m like, I’m gonna make my own breakfast today. And I walked over with a cane and I hung out on the counter and I just had like a bowl of cereal.
Emily 39:35
But I tell you, when you make that first bowl of cereal for yourself, and you take a piece of your independence back, that is the start of it. If you can do that, you start thinking about well, maybe I will wheel myself to the bathroom. Maybe I will walk with my cane to the bathroom and then suddenly you’re on this snowball of like did it did it, did it.
Emily 39:59
It’s not that’s scary, it is scary. But once you achieve these little things, they start to add up. And before you know it, I walked down the stairs by myself. And my mom yelled at me had a heart attack. But I ended up on the bottom floor without anybody knowing about it.
Emily 40:22
But that’s such an integral part for me, because that’s when I knew I had to not limit myself because of everyone else’s fears around me. They fear out of love, of course, they don’t need me falling down the stairs after a brain injury.
Emily 40:42
But sometimes, listening to those voices and reading that material, and just will prevent you from trying, and then it’ll prevent you from having this having an amazing recovery that you might not have gotten to have. If you listen everybody else.
Bill 41:00
It’s like the old days, isn’t it? when you were growing up when you were little, you know, you go to climb a tree, and mom and dad would sit at the bottom of the tree the first few times and make sure you didn’t fall in the third fourth 10th time. They’d say look just be careful, you don’t fall.
Emily 41:16
Yeah, also gave me a heart attack, I’m sure.
Bill 41:19
But that is, it’s not that they’re scared for you, because they love you or like, they’re scared because they’re scared, because they can’t relate to the whole situation. And they don’t know what it’s like, again, and they see you as vulnerable and they see you as you know, injured or whatever they see you as and then they try and go.
Bill 41:48
We don’t want her more to have more of that, you know, we want to have less of that. So if she doesn’t go down the stairs, then should we Okay, well, how long am I not going to go down the stairs for? How many years I’m gonna sit at the top of the stairs and look at them, you know, it’s not how it works.
Bill 42:04
And and you’re right, that’s what you do, you kind of have to go against authority or against, you know, the emotional blackmail, or whatever it is, and you got to put your toe in the water and you got to see is it gonna burn? Is it gonna? What’s the situation? And then if you overcome it, then you can go well, how can I do that again, next time, or what is the next biggest risk.
The Small Steps
Emily 42:29
And that’s the best so that mastering of my own house and testing the waters and saying sorry for upsetting my because she’s my mother. I’m not sorry for taking the risk, but I’m sorry, she got upset so much. And just you know, balancing your household with your carers and keeping open communication of what you need and what you need to do is very important.
Emily 42:59
So what that led to was being trusted with more movement. I had my AFO at that point. And my cane. And I started with a walk around the block, a hobble around the block, you know, whatever. But at that point, I had enough fed upness and kind of anger in me.
Emily 43:20
I was like, I don’t care what I look like, I’m gonna get walking. So I took my little cane, and they walked around the blocks, you know, I was going by myself. And soon I was going without the cane. You know, and that’s that level up that stroke survivors can do, just by testing the waters, like you said, and not being afraid of upsetting anybody. not being afraid of your own body. You know your body better than anyone else, no matter who they are.
Bill 43:49
And did you ever fall?
Emily 43:50
You know, the only falls I’ve ever had was one in the hospital where the nurse drop me. And I have had one or two falls. Only when I started practicing jogging. Because I got there. After taking these baby steps. I was like well I can do that. I had my dad with me the first time I did it safely.
Emily 44:23
It was more of like a old man shuffle you know in the beginning, but it’s something and the more you practice, I mean practice makes permanent in the brain injury world. So yeah, I’ve gone a little cocky and years later and tried to run on maybe a little tired left ankle, and I’ve definitely eaten pavement but and then I stopped so I reel it in and make sure I’m being as safe as possible. That’s it. I didn’t fall.
Bill 44:53
That’s not too bad. I got dropped by nurse in hospital as well. Probably four hours after surgery,
Emily 45:03
Oh my God the paperwork, imagine.
Bill 45:06
I don’t know that there was any. It was really bizarre, right? So my left side’s out of action, and then they, come to get you up to take you to the toilet for the first time, all that kind of thing then when you’re moving straightaway, and they haven’t assessed me yet nobody knows what the impact of the brain surgery has had what impact that’s had, and she was, I’m not quite six foot, but maybe 10 or something 5 11″.
Bill 45:36
And she’s maybe five foot. And she said to me, have you been to the toilet yet? And I said, no, she goes, Oh, let me help you out. I get out on the left side of the bed because she happened to come to the left side of the bed, I put my left foot down. And she says, I’ll hold you and she does the whole you can put her arm around me.
Bill 45:56
I’m 84 kilos or something, and she’s 50 kilos. And I just, we took one step and I just went bang straight on my arm. And I screamed my head off. And it was shock horror. Everyone was just shocked. And I’m not sure what happened. But they must have all swooped me up and got me back in the bed. And then they brought me a pan or a bottle or something like that. It wasn’t gonna happen any other way. So was your fall in hospital? Was it the first surgery or the second one?
Emily 46:32
The first it was the first surgery the first surgery led to the stroke. My second surgery was great. I walked out. hours later. Thank God. Yeah, it did go as well as it was supposed to. It was just a normal brain surgery. But no, that was the first one it was in the rehabilitation hospital.
Emily 46:50
And it might have been like, it was like a new nurse maybe or something maybe not my first trip to the toilet in my room. But it was somebody Oh, you know what it was like, we’re bending down to get graphic. We’re, you know, bending down because that’s tough. And she’s taking your weight. And she said 123 but like I went on three and she went on two or something.
Bill 47:16
You didn’t discuss the number count beforehand. So we’re gonna go 123 and then go or we’re doing.
Emily 47:23
It was a soft fall. Thank goodness, it was definitely like I had, you know, my right arm was on it and stuff. And I was like, Okay, here we go.
AFO For Foot Drop
Bill 47:32
So you told me that you got back into jogging. So you’re going to really appreciate Episode 28 you’re going to be Episode 148 or something. 147. Episode 28 was Donna Campisi. And she’s a local and she was a friend of mine from Melbourne, came and saw me when I was in hospital.
Bill 47:57
And she had a stroke when she was a young kid. And she ran a marathon about 30 years later. And she wanted to jog and run she has an AFO okay, so for those who are listening, an AFO is an Ankle Foot Orthosis. So it supports the ankle from dropping down. Because she has foot drop.
Bill 48:20
And she runs a 40 kilometre marathon full marathon. She She trained and trained and trained, she got injured she got she went through the wringer to get there and she finally got there. And when she got there, it took her forever, you know, compared to everybody else who was running, but she made it she ran the whole marathon.
Bill 48:39
She’s just one determined gal. And you’d love that episode. You’d relate to that a lot. I’ll share the link on the show notes. And I’ll send you the link as well. So you can have a listen. But how far have you gone from you know, if you’re jogging? How much has it evolved?
Emily 49:00
Well, I started maybe a year after I really kind of got a pace going. And there was actually in 2016. There. I’m near Washington DC, currently. So there was a race for a cure for brain cancer research. But what a perfect reason to get my butt up and be able to complete free miles.
Emily 49:33
So that was my goal. I also saw a few others on Instagram that took two running after their stroke or they have a history of stroke and their runners and ultra-marathon runners and marathon runners. Oh my god, oh my god. So I did talk to a few of them. I was like, does your ankle hurt?
Emily 49:52
Do you ever fall like and of course they say Oh, it hurts all the time. Just go. Just do it. And that’s where I adopted the whole If you feel something, then it’s good. Like this is just muscle growing, you know, it’s got to grow back, it’s got to get strong, you got to test it.
Running A Marathon With A Foot Drop
Emily 50:07
So that was my attitude. And, I did successfully complete a 5k no walking, no walking, you know, just that shuffle sometimes after my stroke in 2016. And that was incredible, because, that was one of the things I was dreading was never being able to run again.
Emily 50:33
And taking that for granted, just like being able to move your body in that way. And I still, you know, it’s very careful, I don’t run regularly, because I found bodybuilding, which is much more static and so, so I really enjoyed that. But, um, I was worried about that.
Emily 50:54
And I still, you know, years later, part of a little grief moment comes when you can’t just sprint, you can’t just go run for the sake of running, you have to think about every step you take, you have to be careful, you have to, you know, and that’s a bit sad. But that’s me being picky.
Emily 51:17
Because I know that me running at all in any sense of the word, and whatever it looks like because you know, my arms flopping around all over the place, and I’m limping mostly, it’s such a beautiful achievement to have done after going through a stroke. And I’m so grateful for that.
Bill 51:35
Absolutely. I know what you’re saying I I was asked recently, you know, don’t you ever think about the fact that you’re always feeling your left side feels weird and colder and, and burning? and all that kind of sense. Like, most days, I don’t think about it, but sometimes I wake up and I think Yeah, I wish it didn’t bloody happen. You know, I wish it just felt normal today, because it’s bothering me or annoying me.
Bill 51:59
But that kind of wishes, like doesn’t achieve anything. It’s fruitless. Like you don’t get anything out of it. You just wish something that’s never gonna happen. So you get frustrated. So you have to accept that as well. And some days it’s okay to not accept it and to be crappy about it and to, reminisce on your old self. Absolutely. I mean, there’s nothing wrong with that. I’ve been there.
Emily 52:21
You know I heard a really great saying from one of my colleagues, she has a pastor for father, right. And he said to her, and I love this regarding these pity moments, we’re allowed to have for sure, but we don’t want to get trapped in it for too long, right? She said, her dad would always say you’re allowed to have a pity party. But it has a beginning and an end time.
Bill 52:50
That’s perfect, isn’t it? I mean, that’s it. Thank you for the permission for me to go down that path. And thank you for giving me time to get to my in time and I’ll eventually get there and then I’ll move on and be fine.
Bill 53:03
You found bodybuilding. But were you a you were you a bodybuilder beforehand? Did you do any of that?
Emily 53:11
No.
Bill 53:13
So you’d really also then appreciate and get along with Kelly Studebaker who was on episode 106. And she’s a powerlifter. And this girl she is jacked on one side other side is not so jacked.
Emily 53:30
That’s the life.
Bill 53:32
And then she got sucked in as well because somebody said to her oh you know, you could probably still do it with one hand, just give it a go, whatever. That’s it. She just got into it. And she was off and running. So now on episode 106 I interviewed Kelly and that is a really cool episode as well so I can’t remember exactly how she ended up having a stroke but it’s a really cool episode check it out now.
Freedom To Walk Foundation And Bioness

Bill 53:57
You’re still a real busy person. He doesn’t sound like you’ve slowed down at all You picked up a cheeky directors role or Board of Directors role at the Freedom To Walk Foundation, which is on Instagram as well @freedomtowalkfoundation. And I’m so glad I connected with you because I didn’t realize this until today. But this is really cool because of the Freedom To Walk Foundation supports people with foot drop. Tell me about it.
Emily 54:31
So I met the Freedom To Walk Foundation because when I was getting my newer AFO device at a Hanger clinic in Baltimore, Maryland, they handed me a pamphlet and they said you know you’ve seen some pretty good ankle movement. At this point we can tell you’ve been walking. So you might be a good candidate for the walk aid, which is one of the two leading competitors of a functional electronic stimulation device, FES device.
Bill 55:04
Who are the competitors, because I reckon people have heard of them.
Emily 55:07
The ones that we help people we subsidize the cost for is the walk aid, which is actually owned by Hanger at this point. And Bioness, Bioness has all sorts of fun things, they have a cuff for walking and foot drop, they have arms attachments and all sorts of things, which is really cool.
Emily 55:28
So, yeah, so I got in touch with the freedom to walk foundation. And at that time in 2015, and still, insurance, major insurance does not cover these devices, it is a travesty. That device was $5,000 out of pocket, when I was able to grasp it at that time. And I couldn’t tell you how devastated I was to hear that price tag.
Emily 55:53
Because what else could go wrong? Like at this point, you know, it’s like that’s, like I could get some physical therapy, or I could take a chance on this walk aid or, or I don’t need to pay my bill, I can move in with my parents. And it’s just the kind of decisions that people don’t need to be making when they’re vulnerable.
Emily 56:12
So I can’t hide the freedom to walk foundation. They have an amazing founder, her name is Daisy Vega, and she is an MS. Warrior. So when she developed MS, she developed foot drop, which we might have said earlier is where your ankle muscles are weak, and you end up dragging your toe and you might trip over yourself.
Emily 56:35
And you’ll see people walk with kind of a funny gait where they kind of lift their leg real high to avoid your foot dragging on the ground and happens with a lot of neurological chronic conditions. So her, I think it was her husband, who was able to just afford it straight out, he got her walk aid, and she’s such a giver.
Emily 56:55
She’s such a great woman, she decided to create the foundation to try to reach others that need assistance at this walking and subsidizing the cost. So because she doesn’t want anybody to go without it. So I got to call her and we fundraised, we did a just a typical GoFundMe type of fundraiser I shared with just my family and friends and I was really embarrassed about it.
Emily 57:20
And I didn’t want to do it. But she, you know, asking for help. Suddenly, you’re put in this vulnerable position, not me, not Emily, like never before. And asking for money is the worst, you know, but what we do is, we really encourage folks to try it. And what almost happens 99% of the time is that their device is funded within two days, by their community, their family, and the love around them they never knew existed.
Emily 57:55
And that’s what happened to me. My friends and family and schoolmates all helped me subsidize that cost. And I had a walk it and I tell you, that’s what I attribute to getting me to the jogging point. It was, if you’re not sure what a walk aid is, it has I mentioned in my little stimulation kit over here, so I could show the camera, but I did it. It just has two electrodes that will sit in a cuff is very discreet, it’s not huge, like a AFO, you don’t have to wear it over your clothes, you can wear it under your clothes.
Emily 58:26
Which is a cuff that sits right below your knee, and it stimulates the right muscles. But what’s great about the technology is that the clinician will program it to your gait. So with the swing of your affected leg, it will buzz on with this kind of weight teetering system.
Emily 58:44
And suddenly, with every step, you take the electrodes just lift your ankle for you. And you can set it on Max, you can set it on min, because the point is, you want to think it through you know, we’re always thinking about every step we take. So you want to help sink it into existence.
Emily 59:03
But over time, it’s like you’re taking physical therapy with you everywhere you go. And you don’t have to think about physical therapy. So the fact that these people don’t know about these, first of all, there’s I don’t have access to them. They’re way too expensive, is just heartbreaking.
Emily 59:18
And that’s what Freedom To Walk Foundation helps remedy. So yeah, so I was a recipient, it got me to running a 5k I believe in them. And I did some testimonials at the Freedom To Walk Foundation gala in Florida. They’re Florida based, but we help everybody around the US.
Emily 59:38
We’d love to go international too. It’s just who we meet, you know. And by last year, they were looking for more volunteers on the board. And I was elected a board member. So now I help direct the operations of the foundation as community outreach. I’m a big advocate. I find them on On Instagram, I have a great eye for foot drop, in the grocery store and out in the world I’m like hi have you ever heard of a walk aid? Sorry to bother you.
Bill 1:00:09
You know what they look like? They look like a strap that people put their iPhones in. When they go running and they’re listening to the music. That’s exactly what they look like.
Emily 1:00:28
It’s just a little cuff and a battery pack. It’s really incredible technology.
Bill 1:00:33
And these days, I think it’s cool to have stuff attached to you when you’re doing things. Makes you look like you’re with the times or something. The website is freedomtowalkfoundation.org. And they’ve got a really cool looking website, easy to navigate a lot of pictures of the product.
Bill 1:00:54
And then can either talk about their purpose, and they asked him for donations there. And they also have a really cool little statement that says changing lives one foot at a time. Isn’t that lovely? Yeah, it’s rewarding, isn’t it?
Emily 1:01:19
You know, we were talking about this, before we started how I’m so inspired by people who take the shit that happens to them. And they turn it around to help others. They learn from it, they accept it, and they don’t want other people to go through the same thing they did.
Emily 1:01:41
And I think that’s a really beautiful part of the healing process. It can be and it’s just it, it gives them purpose, maybe you know, to what happened to you. Some people like to think of it that way like it gives, instead of wondering why why why me, you may be able to formulate an answer to that, as you realize that you’re a key. You might be key in somebody else’s recovery is really beautiful thing.
Bill 1:02:10
That’s a pretty cool, why me I mean, that’s better, nothing better than that. If you’re supporting somebody to go through what you went through, because you’re further along the line, and you know what it’s like on the other side, then that’s a real good reason to get involved and help people and it is really rewarding.
Bill 1:02:29
I find the same thing when I do these podcasts and chat to people from all around the world like you and everybody else. One, of my biggest challenges is the lack of men who come on the podcast, that’s one of my biggest challenges is I asked a female to come on and she Yeah, no worries, they’re falling over themselves, you know, I can’t keep them away, which is not common in for me in my life.
Bill 1:02:53
Normally females repelled you know, except for my wife, she’s stuck with me, but the others just repelled. And men getting them online is so hard A there’s not a lot of them on Instagram doing the kind of stuff that you know, a lot of other stroke survivors are doing.
Meeting People With Foot Drop
Bill 1:03:14
Or if they are they do it in the background. So I’m curious about your experience with meeting people with foot drop, is there a difference to the way the men handle the situation? Or talk about it? Are they a little bit more reserved? Do they? Do they do the stiff upper lip routine a little more?
Emily 1:03:37
Well, I like to think that I’m very charming in person. So I don’t think I give them a chance to stiffen up about it. Especially if I if I meet them in person. I first of all, catch them off guard by saying, hey, do you have foot drop? Me too. Cuz they’re like, Who knows? Who knows about that? You know so I do find that after I get that kind of sensitive question out of the way.
Emily 1:04:04
And like, I’m Emily, and I want to tell you about this. Then, it’s like, Okay, and then I might give them Freedom To Walk Foundation information. Just sometimes I asked if they’ve ever heard of a walk aid kind of thing. And we might exchange information to get them to the website. But no I’ve never had an issue with talking to someone about it.
Bill 1:04:28
I’m not charming enough is what you’re saying. That’s why the men won’t come on board, because I’m not charming enough.
Emily 1:04:36
I mean, I feel like that might just see the inherent nature. You know, society has just made poor guys you have to ignore feelings and not fess up to emotions when it comes to mental health and emotional health. They’re already starting behind. And I think that’s probably adds to it. The few folks that runner I initially talked to was a man.
Bill 1:05:04
We’re always running away from shit. That’s why men run because they’re running away from everything.
Emily 1:05:10
You just got to put them on a treadmill, so they don’t go anywhere. But you know, once you break the ice So yeah, that’s interesting get some kind of recruitment kind of said you got to maybe talk to them privately. First give your spiel.
Bill 1:05:30
No I have a podcast I’ve spoken to them enough they listened to the podcast, they just don’t do much about it. If there’s any men listening to the podcast and they’ve got to the end of this one. Hit me up for an interview. Just come on board. Let’s have a chat about what’s going on in your life. I promise I won’t ask any probing questions that are too uncomfortable.
Bill 1:05:51
Emily, you vouch for me? I did all right?
Emily 1:05:54
Absolutely. It’s been a pleasure.
Bill 1:05:58
On the freedom to walk Foundation website as well. There’s some testimonials little Zoey regaining her independence. She’s a little girl. And then is there is George in the walk aid. George Kosinski, his new walk aid. So there’s some real cool ways to get to understand what it is that walk the walk aids do and how they help, especially when you get to see videos of people and you get to see how they are attached to the leg below the knee.
Bill 1:06:31
They look like they’re going to be very comfortable for most people I don’t see it being an issue at all. And they’re available. You can follow the freedom to walk foundation on Instagram and Twitter and Facebook as well have all those links there.
Bill 1:06:45
So it’s a really cool foundation. I didn’t know it existed. So I’m just so glad. And you need to get somebody from the foundation onto the podcast so I can interview them. Other than you because I know, we’ve brought you on for a different reason. But I can bring on somebody and really give them a lot of time.
Emily 1:07:07
Yeah, I could absolutely speak to our founder. It’s a very small nonprofit. It’s run by her and me. And there are four other board members. And that’s it. And so, growth plan, you know if, like, if we’re able, it’s a humble nonprofit, helping, being able to reach a lot of the community in Florida because Daisy is such a networker, and she’s lovable.
Emily 1:07:35
Everybody in Clearwater knows about her, I think I’ve, you know, poached people off of Instagram, and we’ve gotten blockades to California and Pennsylvania and things like in Texas just recently. So it’s like, it’s just a little it’s like, just piece by piece. We’re trying to make a difference. So that’ll be one, but she’s really lovely. So that would be fun to get her on.
Bill 1:07:57
Yeah, How so? How many people have you guys helped? Do you think with this? How many people a year received support in some way?
Emily 1:08:04
Well, last year, we did. I got those folks I mentioned California, Pennsylvania, Texas. We’re also thinking of expanding into any walking aid. Because there’s still folks especially in Florida, which have a higher population of senior citizens might just need a walker, I think Daisy have gotten has gotten a few of those out walkers and canes and things that make mobility more comfortable.
Emily 1:08:32
So we’re thinking of maybe expanding to that, say about five, just ad hoc over the over the year last year. And then at our gala, every year, we do identify, usually a child, we try to get a family who’s in crisis with their child that sometimes have a diagnosis of stroke, or cerebral palsy, which the blockade absolutely helps as well. kind of keeps things straight allows them that Zoe on the website, she’s a CP patient.
Emily 1:09:04
And so before she couldn’t walk very well around, but with that walk it it really streamlines things and she’s just running. So our main goal every year on the side is to fundraise to have a walkout to give away at the gala per year to a child in need. And then we do what we can on the sides with our small workforce, just as we can.
Emily 1:09:30
And I do want to say, I did tell you in 2015 walk aids were going for $5,000. Some good news for all of us is that the walk aid and probably Bioness meeting their cost as well. The walk aid has definitely come down to $2,950 which is still prohibitive for families. So we still want to help and do that work.
Emily 1:09:56
But just in case someone’s listening and like you said never heard of it. I think everybody should have one. It’s, it’s game changing for recovery, it is ridiculous that people don’t know what it is that you’re not hearing about it in the rehab hospitals that you know, it’s still privatized.
Emily 1:10:13
So I do want to let everyone know that that the cost has come down if you were hearing it, and then you heard $5,000, and you feel sad about that, so down to 2950, on average, and they do include unlimited adjustments, once you get your clinician at hanger, you know, your patient for life, as long as you need it.
Emily 1:10:33
I do want to say that I don’t use it anymore. I am a client’s free. Nothing’s perfect, but but you know, through my acceptance and just loving my body, as far as I could take it, and this is me, I wanted to drop all the AIDS at one point, I felt confident that I can get about safely. And so I stopped using it maybe after two years or so. And I said, Well, let’s see what my body can do now that I’ve thought it and the electrodes helped it for two years, I do pretty well.
Bill 1:11:09
Can they be repurposed?
Emily 1:11:12
You know, that’s something I’ve asked before too, which is frustrating, because I asked, Can I recycle this to somebody? And, of course, it’s not that easy. Because it’s pharma, you know? Or else we’d all be sharing $5,000 stuff like our netflix accounts, right?
Bill 1:11:28
It’s like a phone I mean, is if you can’t just give it to somebody else and give it a new strap.
Emily 1:11:33
I still have it. Yeah, it just needs to be programmed, I still have it, I keep it because one day, as these things develop and costs and all the insurance crap, and all that stuff happens one day, I hope to recycle it and just give it back to hanger.
Bill 1:11:47
I feel like there’s a opportunity there massive opportunity there for all the ones that are out and about that aren’t being used. They can be repurposed for people who can’t afford three grand or five grand. And who could get it for 1000 bucks or whatever. But there’s surely there’s got to be an opportunity anyway.
Bill 1:12:06
Look, that’s me just doing my problem solving stuff again, and solving problems and all that kind of thing. And you could harass the manufacturer about that I think you should harass. And if you don’t want to I will, because I think that’s what should happen.
Emily 1:12:24
I know one of the top salesmen in the US because he’s come to speak at our gala before, so I know him personally on Instagram. And I should check in. He’s not the CEO, but you know.
Repurposing Walking Aids
Bill 1:12:37
Yeah it’s a good question you know, with all these corporations that want to do better things for the world these days, here’s a better thing that they can do, here’s a something that they can do, that’s going to make a difference in people’s lives.
Bill 1:12:49
And they could get a real, you know, little ticks for achieving not just an amazing product and selling it for a shitload of money, but also for having an amazing product, and repurposing the ones that aren’t being used for people who can’t afford it.
Emily 1:13:06
I’m gonna take that idea. I’m gonna do at least one action with that and see, see how far I can go.
Bill 1:13:11
I love it. We’ve achieved a lot today, we’ve solved problems. I’ve put you in touch with people who are power lifters and marathoners and your we spoke about the freedom to wall Foundation, I really appreciate you being so keen to jump on and share your story and tell us about some of the things that you’ve been through. Thank you so much for being on the podcast. I just truly appreciate it.
Emily 1:13:39
Absolutely. Thank you for the platform. This is so important the work we’re doing it really is it’s gone through my head. I know it goes through other people’s heads that, gosh, we should do so much. We should write a book we should get resources on but some of it Yeah, I didn’t do it. But you did and I really thank you for that.
Bill 1:14:01
I love what you said thank you for that. I really appreciate it for you acknowledging me, but you did what you did, and you’re on the board of something and you’re doing that and somebody else is doing something ever so simple, which is even responding to an Instagram post that you might not think means a lot and it’s not that important.
Bill 1:14:24
But the fact that somebody did do that for me one day years ago, makes a massive difference. And we don’t all have to do podcasts because they’re bloody time consuming and no one’s got that much downtime. Believe me, I don’t either they they take about eight hours an episode to get live.
Bill 1:14:24
Like it’s just a huge amount of work, right? So don’t feel bad. If you can’t do that. Do something little something that you can do. Just be nice to somebody just send them a message on insta just touch base with them, just do those things. You’re volunteering in this Foundation, I’m not going to do that, that means I’ve got to leave my house, I’m going to go somewhere else to do that and meet people in person.
Bill 1:15:07
And that takes way too much. I’d rather be recording a podcast from the comfort of my own home with heating or air conditioning. You know, I’m that kind of guy. So everyone can participate the way that they feel. And some of us don’t have more limitations than us.
Bill 1:15:22
So they don’t have the ability to be so proactive and make it a bed in one hour. And you know what, it’s also really important sometimes to just make it about you and stuff everybody else.
Emily 1:15:34
Yes especially at the beginning.
Bill 1:15:39
And that’s you and me, giving permission to people to just make it about yourself every once in a while, but have that party, at some point, it starts and at some point it ends. So when it ends, kick in and bringing other people into your world, because what that does is that is also rewarding, isn’t it? And that really makes recovery. And the experience that you had, it does make it a little bit kind of worth it. Would you say?
Emily 1:16:05
I said I have no regrets. I love my life. And I know that’s hard for some people to understand. But I know that other survivors like us can understand what I mean when I say that.
Bill 1:16:17
Thanks, Emily. I appreciate it. Thank you so much for having me. Thanks so much for joining me on today’s podcast. Do you ever wish there was just one place to go for resources, advice and support in your stroke recovery? Whether you’ve been navigating your journey for weeks, months or years, I know firsthand how difficult it can be to get the answers you need.
Bill 1:16:39
The road is both physically and mentally challenging from reclaiming your independence to getting back to work to rebuilding your confidence and more. Your symptoms don’t follow a rulebook and as soon as you leave hospital, you no longer have medical professionals on tap.
Bill 1:16:54
I know for me, it felt as if I was teaching myself a new language from scratch with no native speaker inside. If this sounds like you, I’m here to tell you that you’re not alone and there is a better way to navigate your recovery and rebuild a fulfilling life that you love. I’ve created an inclusive supportive and accessible membership called recovery after stroke.
Bill 1:17:18
It’s all in one support and resource program is designed to help you take your health into your own hands. This is your guidebook through every step of the journey read from reducing fatigue to strengthening your brain health, to overcoming anxiety and more. To find out more and to join the community. Just head to recoveryafterstroke.com See you on the next episode.
Intro 1:17:44
Importantly, we present many podcast designed to give you an insight and understanding into the experiences of other individuals opinions and treatments, protocols disgusting any podcast or the individual’s own experience and we do not necessarily share the same opinion nor do we recommend any treatment protocol discussed.
Intro 1:18:01
All content on this website and any linked blog, podcast or video material controlled this website or content is created and produced for informational purposes only and is largely based on the personal experience of Bill Gasiamis the content is intended to complement your medical treatment and support healing.
Intro 1:18:18
It is not intended to be a substitute for professional medical advice and should not be relied on as health advice the information is general and may not be suitable for your personal injuries, circumstances or health objectives did not use our content as a standalone resource to diagnose treat, cure or prevent any disease for therapeutic purposes or as a substitute for the advice of a health professional.
Intro 1:18:38
Never delay seeking advice or disregard the advice of a medical professional your doctor or your rehabilitation program based on our content if you have any questions or concerns about your health or medical condition, please seek guidance from a doctor or other medical professional if you are experiencing a health emergency or think you might be call 000 if in Australia or your local emergency number immediately for emergency assistance or go to the nearest hospital emergency department.
Intro 1:19:03
Medical information changes constantly. While we aim to provide current quality information in our content. We did not provide any guarantees and assume no legal liability or responsibility for the accuracy, currency or completeness of the content. If you choose to rely on any information within our content, you do so solely at your own risk. We are careful with links we provide however third-party links from our website are followed at your own risk and we are not responsible for any information you find there.






