Angela Michelle was unfortunate to have multiple stroke misdiagnoses at 2 different hospitals for blood clots caused by a previously unknown blood clotting disorder which has resulted in lifelong deficits including vision problems.
Highlights:
01:42 Introduction
02:20 Misdiagnosed
04:58 Catastrophic Antiphospholipid Episode
13:54 It Gets Harder Before It Gets Easier
22:14 Angela Michelle Had A CTEPH
29:11 Post-Stroke Deficits
37:43 Slaying The Dragon
43:42 A Gift Of Perspective
51:18 Sexology And Boudoir
1:03:31 Stroke Bein Taboo
1:10:13 Chronically Beautiful
1:18:14 A Deeper Connection
Transcription:
Angela Michelle 0:00
So I’ve always been into yoga. But yoga was definitely more of physical practice before my stroke. And it was after my stroke that I turned to yoga to accept and make peace with what had happened with my anger and frustration at the hospitals.
Angela Michelle 0:17
I do notice like with yoga, some of the poses I struggle with, physically, and sometimes it’s my lungs, or sometimes it’s just like the dizziness or balance issues, those kinds of things. But I will say, because I know you have some amazing people who listen to you is that for me, yoga really helped me emotionally, mentally and physically. And it helped me so much that I ended up becoming a yoga instructor myself. And I actually work with stroke survivors now and I teach them how to do yoga.
Intro 1:03
This is the recovery after stroke podcast, with Bill Gasiamis, helping you navigate recovery after stroke.
Bill Gasiamis 1:16
Hello, and welcome to episode 202 of the recovery after stroke podcast. If you’re a stroke survivor with a story to share about your experience with stroke, and you’ve been thinking about reaching out to be a guest on the show, but we’re waiting for the right time to reach out. This is it. If you go to recovery after stroke.com/contact You will find a form that you can fill out to apply to be a guest on the show.
Introduction
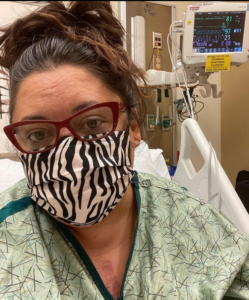
Bill Gasiamis 1:41
As soon as I receive it. I will respond with more details on how you can choose a time that works for you. And for us to meet over zoom. My guest today is stroke survivor Angela Michelle, who is also an internationally published and award-winning photographer, and educator, mentor, certified sexologist, body image workshop facilitator, yoga instructor, public speaker and advocate. Angela Michelle, welcome to the podcast.
Angela Michelle 2:12
Thank you so much for having me.
Bill Gasiamis 2:14
My pleasure thank you for being here. Tell me a little bit about what happened to you.
Misdiagnosis
Angela Michelle 2:20
So it was 2016. And I was going through where I was struggling with my health, I didn’t know why I was really sick. I kept having like chest pain and was coughing a lot. It was in May. And I actually found out I was pregnant the day after Mother’s Day and I was super excited.
Angela Michelle 2:47
We had been trying for two years. But I was really sick. I ended up going to urgent care. They just thought I have like a cold. Two days later, I ended up in a hospital with pneumonia. And I was there for a whole week. And on the last day I was there I woke up with what I could describe as the worst headache of my life.
Angela Michelle 3:13
And it was my head and it went kind of all the way down my neck. I now know that’s my carotid and I kept paging the nurse and I was like something’s really wrong. I just feel it something in my body. Something’s really wrong. And they just kept dismissing me. And then I started having some visual changes just in my right eye like things were zigzagging and not matching up.
Angela Michelle 3:40
And so again, I was paging the nurse and I kept telling them and at one point, the head charge nurse came over and just told me, Oh, honey, you just have anxiety. And they decided, in my opinion, because I kept calling them to discharge me. And they just said you’ve been here a week you need to go home and sleep. We’re going to discharge you.
Angela Michelle 4:05
So they discharged me and my dad picked me up from the hospital. And I have a stroke in the car on the way home. The stroke I never lost consciousness but this I went completely black. Like I have no vision in it to this day. And I was very sick. I was vomiting, and just really nauseous, headache.
Angela Michelle 4:33
My dad took me to a second hospital and they did not recognize it as a stroke either. Because it wasn’t the classic stroke symptoms. It wasn’t the droopy face. It wasn’t the slurred speech. So I sat there for about five hours and I missed my opportunity to get the drug that could have you know potentially reverse some of the damage.
Angela Michelle Had A Catastrophic Antiphospholipid Episode
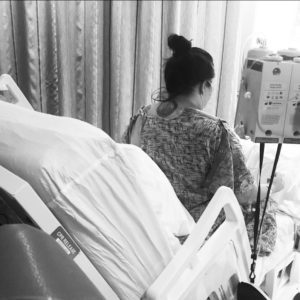
Angela Michelle 4:57
I made it to a third hospital and then by this time it was the following morning when I got there. And they immediately realized I had a stroke. And they realized that not only had I had a stroke, I had clots throughout my body. And I was in what is known as a Catastrophic Antiphospholipid Episode, it was a caps.
Angela Michelle 5:22
And I didn’t know I had a clotting disorder before this happened. So this was kind of the first I’d ever heard of it the first I’d ever. You know, before this, I had never even been like, admitted to a hospital, I had, you know, gone from my regular checkups, but I had never been hospitalized.
Angela Michelle 5:43
And I was in the hospital about three weeks. And at one point, they asked me if I wanted a priest to read me my rights. Like they did not think I would survive. And I did end up miscarrying my child. And I also lost the vision. And I think I’m very lucky in a sense that I didn’t have a lot of physical deficits. But there has definitely been more cognitive, and, like, the emotional impact of everything that I’ve had to work through. And I think, my anger and frustration at the system for failing me.
Bill Gasiamis 6:29
Well justified, I reckon, definitely. So you’re in hospital for such a long time before you had the actual stroke event? Or, you’re going through it and having it and they missed diagnose, did they do tests? Did they do all the things that needed to be done?
Angela Michelle 6:54
No, I didn’t know better. I didn’t, I didn’t recognize that I was having symptoms of a stroke. And they didn’t either. And, you know, knowing what I know, now, they should have realized they should have put it together. And the hospital I was at, calls himself a comprehensive stroke center. Like they sell themselves as we’re one of the best stroke hospitals in the country. And I had a lot of anger about that. And I had to work through that.
Bill Gasiamis 7:26
Yeah, I can imagine. And how long after you were discharged in time? 30 minutes? Hours? Like, how long was it before you were discharged, left the hospital and got into the car? How long did it take for you to actually have the stroke?
Angela Michelle 7:43
Five minutes.
Bill Gasiamis 7:45
And it didn’t occur to you guys to go back to that hospital and tell them?
Angela Michelle 7:50
No, we were closer to another hospital. At that point, we were in an area of town that’s called the medical center. And there’s literally like hospitals everywhere. So we went to the next the first closest one.
Bill Gasiamis 8:02
Okay. And then you got there, even though you’re actually now full-blown having a stroke. You’ve gone in, they’ve gone it’s not a stroke?
Angela Michelle 8:14
They didn’t even see it as a stroke. They were like, you don’t have the droopy face. You don’t have the slurred speech, you can still walk although I couldn’t walk well, I was in a lot of pain and distress. But yeah, because it affected my eye and my vision. They were like you need an ophthalmologist, and we don’t have an ophthalmologist at this hospital. So we need to transfer you to another hospital. And they made me wait for about five hours to get that transfer.
Bill Gasiamis 8:51
In that five hours, did your condition worsen?
Angela Michelle 8:55
It worsened in that I was vomiting profusely, and I was becoming very weak. I was starting to get disoriented. But like I said, I never truly lost consciousness. I was definitely aware of what was happening. Although it was, to me a state of I think your body goes into like a state of shock. And so I was there and aware, but I wasn’t able to even comprehend what was happening.
Bill Gasiamis 9:31
And how far along was the pregnancy?
Angela Michelle 9:34
So when the stroke happened, it was very early. It was about six weeks.
Bill Gasiamis 9:39
Did you know you were pregnant? You did know I think I heard you say.
Angela Michelle 9:43
Yeah, so I had just found out. I found out the week before I got admitted to the hospital, the first hospital that missed the stroke. And I told them you know, I was like I’m pregnant and I was very scared about you know, everything they were giving me is it safe for the baby? Am I okay, you know, what test are we doing? Is this safe? I was very concerned.
Angela Michelle 10:07
Like I said, my husband and I had tried for about two years to get pregnant. So it was very much a wanted and desire pregnancy. So yeah, I did know I was pregnant. I found out that it was not a viable pregnancy. Once I got to the third hospital, and they ended up doing a vaginal ultrasound, and they determined that there was no heartbeat, ultimately, that gave them the ability to actually save me. Had there been a heartbeat, I don’t know if they could have because it was a state hospital.
Bill Gasiamis 10:47
Because of the abortion issue,
Angela Michelle 10:50
Because of abortion issues. And because a state hospital gets state funding and the state is anti-abortion. So they won’t give funding to any hospital that performs them or even does, like a, I think it’s called like a DC or DNC, where it’s like after a miscarriage and they kind of like clear it out that way you don’t have like sepsis. They won’t even do that for me. So I did have to carry you know, unviable pregnancy for another five weeks.
Bill Gasiamis 11:33
And then they allowed you to have the procedure to remove even then? What happened then?
Angela Michelle 11:44
They wanted me to just naturally have my miscarriage. So I had to wait until and hope that my body would do what it needed to do. It did. I had the miscarriage about five weeks later, because I was already started on anticoagulants, because of the clotting disorder, they wanted me back in the hospital when I was having the miscarriage just to make sure that I didn’t have, you know, too much excessive bleeding. And maybe I needed a blood transfusion. So I had to have my miscarriage at the hospital.
Bill Gasiamis 12:22
And you’re going through, you’ve been diagnosed that you’ve had a stroke at this point in time. You’re going through that and dealing with vision loss and all the other challenges. And also at the same time you’re going through a pregnancy that’s not viable. And then you have to go through the miscarriage all at the same time.
Angela Michelle 12:45
Yeah, I did. It was a lot. It was definitely a lot. And, you know, I know, you like to talk about like the recovery part. And that was, it was huge to me to try to get back what I felt like I had lost and I don’t think I brought this up before. But before my stroke, I was a photographer that had been my career for the last 12 years. And so to lose sight for anyone is devastating.
Angela Michelle 13:18
But I think for a photographer, it’s an extra whammy. And so I was a wedding photographer, and I did other types of photography as well. But I had a wedding scheduled two weeks after my stroke, and I had to call that client and just tell them there was no way I could do it. It was out of state and I couldn’t get cleared to travel. I was having to miscarry. And so it definitely, you know, on top of losing everything with my body and my child. I felt like I lost my career that I had worked so hard for too.
It Gets Harder Before It Gets Easier
Bill Gasiamis 13:54
Yeah. Identities getting trampled on every corner, there’s no getting away from it, you know, everything that you knew and did the day before all of that stuff happened is just completely stopped changed and out of your control, and you’ve got to somehow navigate it and you’ve got no skills or tools to navigate it because you’ve never been through that before.
Bill Gasiamis 14:18
And it makes sense when somebody says what the hell is going on? Like what the frick is going on here? You know, how am I supposed to get through this with no skills and no previous experience in this space? And somehow you do and you do come out of it. And that’s what the podcast is really about. It’s giving people some hope that in time there’s going to be a change in the tough stuff and better things are coming but you got to go through the tough stuff unfortunately we all do with stroke.
Bill Gasiamis 14:58
Yeah, so Let’s just go back to the issue with the pregnancy. It was an unviable pregnancy, they knew that. And you still weren’t able to have that pregnancy resolved or I’m not sure what the word is because of legal issue with regards to the state of Texas, and its rules on abortion and therefore the hospital that you’re at. So is it still considered an abortion to end a pregnancy when it’s an unviable pregnancy? And what do you think about that?
Angela Michelle 15:37
I think it’s a gray area. And I think that the hospitals were scared to lose their funding. So they would rather not step into that gray area. I didn’t realize at the time how deadly that could be for me. I think had I realized I would have maybe gone to another hospital or fought harder, I don’t know, I would have probably done something else. I think the the trauma of the stroke and everything that had gone through. I don’t think my brain could even comprehend that.
Angela Michelle 16:16
At that time, I think I was just doing what they told me. And at that point, I was really trusting that hospital because they were the ones that saved me. And the other two had failed me. So I trusted them. And I trusted that my body would do what it needed to do. But I didn’t realize how much danger I was putting myself in until I learned more.
Bill Gasiamis 16:41
Yeah, glad it worked out. And on reflection. What sounds like it was the right move, because the outcome meant that you get to be on the podcast, and you’re still here. And that’s great. But I know what you’re saying about learning things later and going, oh, gosh, that’s a risk that I took that I didn’t know I was taking and wasn’t an informed risk. Right. And that, that’s a little bit alarming to hear.
Bill Gasiamis 17:14
Because I certainly don’t like making decisions unless I’m completely informed about all the risks, whether they’re good or not. And the decision that I make should be mine in the end, not a doctor’s, in my opinion, I don’t believe a doctor should be telling me what I will or won’t do, or what medical intervention I will or will not have. So I argued with my doctors a number of times, and I sacked a couple of them and went to a different hospital and got second and third and fourth opinions.
Bill Gasiamis 17:47
Because they were going to open my head up, they were going to do stuff in there that I needed to make sure that when they did it that I was not being coerced into any of the decisions that were made on my behalf. Because even though I had the cognitive challenges that stroke causes, I still had enough ability to make important decisions about my life.
Angela Michelle 18:20
And I think that’s really important that you bring up informed consent. And that’s something that I realized is so important. And you know, you mentioned firing doctors, I have since fired many doctors and had to get second opinions and really push back on my doctors who sometimes don’t want to run test or don’t agree. And you know, I like you said,Yes, I have cognitive challenges, but also I’m able to make decisions and I’m able to learn new things and gain knowledge.
Angela Michelle 18:56
And so after this happened, I really learned a lot and all I could about strokes and the disease that I have that caused it. And the more I learned the more I wind to one spread awareness and help others because I don’t want others to go through what I did. But I also wanted to kind of take my power back after feeling so you know, helpless, because that’s what it felt like at that time.
Bill Gasiamis 19:27
Yeah, you give your power over to somebody else and you entrust them with that they are experts because they’re in the medical field and they help people all the time. And there is a little bit of power that you give up knowing that they’re experts and that they do that for a living and that they are able to save you or make life or help you out. So there’s a bit of trust but there’s also that I think there’s it’s healthy to have a little bit of not sure if the word is distrust but a little bit have skepticism about what they’re about to do or say.
Bill Gasiamis 20:04
And not necessarily just take everything to face value and to question and to be your own advocate and to make them prove their case. There’s no reason why they can’t. Well, that’s your thought. That’s what your idea is. Well, why? Prove it to me, show me the evidence. Explain to me how that’s wrong. And I think it should be their job to feel comfortable in answering questions of their patients. Because we’re the ones that are attached to our body.
Angela Michelle 20:38
Absolutely. I say, now, I see my care with my doctors. It’s a collaboration it had to be a collaboration between me and my doctor, because like you said, it’s my body, I know what I’m experiencing. And, you know, if I could turn back time, I would go back to when I first started having symptoms in that first hospital, and I would have demanded a neuro check. I didn’t know when to do that. So I think seeing my relationship with medical professionals now as a collaboration in my care, has really changed how I interact with them in good ways.
Bill Gasiamis 21:19
Yeah, I think if you’re driving the communication with your doctors in, in that manner, if you’re driving it with that outcome to collaborate, then I think you will find the right doctors, and you’ll know which ones immediately don’t fit. Because they won’t be able to understand that concept of collaboration.
Bill Gasiamis 21:43
And then it just won’t feel right. And then you’ll be able to go, Well, these guys are not a good fit for me, we need to find another person who is. Yeah, I love that. And that’s such a great way to look at it. That’s what it’s meant to be. It’s meant to be a collaboration rather than you’re just some body or a body that I that I do stuff to.
Angela Michelle 22:09
That they treat.
Bill Gasiamis 22:10
Yeah. And then they send you on your way.
Angela Michelle Had A CTEPH
Angela Michelle 22:13
Yeah, and I think I didn’t understand that until I have this experience. And it was this experience. And I know this is about stroke. So I won’t go too far off on my other thing, but the clotting disorder also caused a lot of pulmonary embolisms, and it led me to develop a rare form of pulmonary hypertension called CTEPH.
Angela Michelle 22:38
And it took me another year after the stroke to get that diagnosis. I ended up on oxygen 24/7. My doctors didn’t know why. And it took me doing a lot of research it’s actually really interesting. Because of my stroke, and because I had been missed, I became very active on being an advocate and raising awareness. And I started posting on social media. So when I ended up on oxygen, I posted about it on social media.
Angela Michelle 23:09
And it was an old high school friend who realized he put it all together and he realized he suspected I had CTEPH. And he was the one who told me I had to take that information to my doctors. And at first my doctors were very resistant. It’s really rare. It’s, you know, really, it’s just so rare. We don’t think it’s possible. And it took me being my own advocate and saying, I need this test because my friend was telling me exactly what test I needed.
Angela Michelle 23:40
And I was able to get the diagnosis. And I’m sure you can kind of see my scar. So I did have to have open heart surgery on my lungs. When I was diagnosed, they gave me less than two years to live with that particular disease. So had my friend not intervene and helped me I don’t know if I would be here right now.
Bill Gasiamis 24:03
Was your friend a medical expert?
Angela Michelle 24:06
Oh, yeah. He’s a heart surgeon.
Bill Gasiamis 24:09
Oh, okay.
Angela Michelle 24:11
So he’s a heart surgeon. And even though it’s not a disease he treats a lot, he knew of it, and he’d seen it. And so he just put it he’s like, you have a clotting disorder. Now you can’t breathe or ending up on oxygen. I think you have pulmonary hypertension from the clots in your lungs. He put it together.
Bill Gasiamis 24:33
Wow. Okay, great. I love it. And that’s the thing. That’s the issue that we have here. And I’m sure that it’s an issue all around the world it’s people going to doctors with information that doctors don’t take seriously. Like without ever having spoken to you they know better or having ever met you they know automatically when you walk in the door that it’s so rare that you couldn’t possibly be the lucky one who’s got it?
Bill Gasiamis 25:07
Give me a break, give me the benefit of the doubt. You know, we have Medicare here in Australia, where medical is free. And when you go into the online portal where you check all your records, and all those types of things, there is an allowance for certain number of blood tests per year. And it’s like $1 value that they allocate. And most people don’t use it, but some people go and they use it up and then the doctor has to approve all these other ones, if they don’t approve them, you have to pay for them.
Bill Gasiamis 25:49
And, you know, that’s fair enough. But my wife requested some blood tests of our GP recently, and he said, No, we can’t do those, because you don’t have all these things that he thinks that she needed to present with to have this particular blood test.
Bill Gasiamis 26:10
And it’s like, even then, it’s within the allowable limit of blood test she hasn’t had blood tests for a number of years, it’s within the allowable financial cost limit to have that blood test. And yet still, you think that it’s better that she doesn’t have the blood test.
Bill Gasiamis 26:29
So that’s kind of what’s going to give you information as to how to begin to treat this lady anyway, it starts with knowing something, not knowing nothing, and then doing nothing, so that you’ve got no information. So even if we rule it out, we’re a step ahead than we were when I came here at the beginning. And this inability for them to grasp that concept is why I really was my own advocate, and why I went, you know, to the extreme to make sure that my doctors were the right ones, etc.
Bill Gasiamis 27:06
And why people need to go back and question their doctors. 99.9% of doctors are great, but also 99.9% of them make mistakes. They’re having a bad day. Yeah, they misunderstand what you’re saying. And they need the conversation to occur.
Bill Gasiamis 27:29
I think they’re better served by us, if we don’t allow them to just say no, and then we move on with it. I think they’re better served by us insisting and then proving perhaps to them, that may be it would have been the right call to agree to this particular test a little while ago. And even if they’re correct, at least they’ve eased the mind of the person who is coming in with a concern.
Angela Michelle 28:01
One you’re getting more info, like you said, you’re ruling things out. And that’s, that’s kind of science, right? Like, we try things and then rule things out. And then but yeah, you have to be your own advocate. And I did have to push a little bit with my doctors have no, I really want this test. I really think this is a possibility.
Angela Michelle 28:25
And you know, I’m so glad I did. And I think I was so lucky to have that friend who was a heart surgeon. And I really felt like the stars aligned for me, like I knew, this is a hard path, but this is my path. And we say I was dealt some bad hands, but I’m gonna play them. I’m gonna play my hand.
Bill Gasiamis 28:53
Yeah, you have to agree. So after the heart surgery, and the stroke, I know you were left with some deficits as a result of the stroke. And then you had the heart surgery. So what do you live with every day that’s related to those medical conditions and challenges that you went through?
Post-Stroke Deficits
Angela Michelle 29:11
Yeah, so as far as like, cognitive things, I forget words, I forget people’s names, like, people I know. Like people like, I know you know, I’ll still forget your name. And then at three in the morning, it’ll come to me or, you know, it’s random. and sometimes I wonder what was the stroke or what was the heart surgery, or you know, the lung surgery.
Angela Michelle 29:38
The lung surgery is a very intense surgery where they actually put you on a heart lung bypass, and they have to stop it for 20 minutes at a time. So your body’s cooled to like 60 degrees Fahrenheit, and that allows them to stop the heart lungs for 20 minutes.
Angela Michelle 29:56
And so I know that there could be some residual effects from that too, because you medically die. But I struggle with like, just staying on task or, you know, staying focused remembering things, things like that. As far as any physical things, the lung disease definitely affected my ability to move.
Angela Michelle 30:25
Like I said, before the surgery I was on Oh to 24/7, I still sleep with it. And I still have to use it on exertion. So like, I can’t run without oxygen. I can’t do aerobics about oxygen. And then the eyesight that was the big one for me, so people think I can still see on my right eye. I’m like, No, it’s completely black. I might as well be wearing an eyepatch.
Angela Michelle 30:52
And, you know, I’ve learned to navigate that as best as I could. After the stroke, I was driving within three months. And you know it for me, driving has always been like a freedom, I guess, ever since I was like a teenager. And so for me, being able to like get in my car and go somewhere was something I really wanted to do.
Angela Michelle 31:16
And it was important for me to feel like, normal again, I guess to do that. So I got behind the wheel within three months. And I just learned like, I have to be aware I have to really turn my head and look and make sure. So yeah, you know, I always tell people driving is almost easier, especially cars nowadays that kind of beep at you like not other cars like our car.
Bill Gasiamis 31:43
Yeah, they have the sensors etc.
Angela Michelle 31:45
Yeah. So I actually struggle more of walking, because I tend to like walk into things or walk into people because I don’t see anything like if you’re on this side of me, I don’t see my hand until, like, right now I see it. So those are the little things that I struggle with. I guess a balance to I forgot. I’ll say that one thing that helped me personally after my stroke was, so I’ve always been into yoga.
Angela Michelle 32:16
But yoga was definitely more of a physical practice before my stroke. And it was after my stroke, I turned to yoga to accept and make peace with what had happened with my anger and frustration at the hospitals. And I do notice like with yoga, like some of the poses I struggle with, physically. And sometimes it’s my lungs, but or sometimes it’s just like the dizziness or balance issues, those kinds of things.
Angela Michelle 32:52
But I will say because I know you have some amazing people who listen to you is that for me, yoga really helped me emotionally, mentally and physically. And it helped me so much that I ended up becoming a yoga instructor myself. And I actually work with stroke survivors now and I teach them how to do yoga.
Intro 33:17
If you’ve had a stroke, and you’re in recovery, you’ll know what a scary and confusing time it can be, you’re likely to have a lot of questions going through your mind. Like how long will it take to recover? Will I actually recover? What things should I avoid? In case I make matters worse, and doctors will explain things that obviously, you’ve never had a stroke before, you probably don’t know what questions to ask.
Intro 33:41
If this is you, you may be missing out on doing things that could help speed up your recovery. If you’re finding yourself in that situation. Stop worrying, and head to recovery after stroke.com where you can download a guide that will help you. It’s called seven questions to ask your doctor about your stroke.
Intro 34:01
These seven questions are the ones Bill wished he’d asked when he was recovering from a stroke. They’ll not only help you better understand your condition. They’ll help you take a more active role in your recovery. Head to the website. Now, recoveryafterstroke.com and download the guide. It’s free.
Angela Michelle 34:20
Because I tell people if you can breathe, you can do yoga.
Bill Gasiamis 34:24
I love it, I love it, love it, love it. And you know why? Because you said the three magic things emotional, physical, and mental. And I think stroke recovery is a three-pronged approach. And I’ve said it a number of times. And the main three headings are in emotional recovery of physical recovery, and a mental recovery.
Bill Gasiamis 34:47
And if you neglect those, or one of those, you’re doing a pretty good job at recovery, but you’re missing one of the key ingredients. And I think one of the most important ingredients is the emotional Recovery, if I can get anybody to do anything, is get them to do the emotional recovery. Because physical recovery is something that everybody else does to you anyway.
Bill Gasiamis 35:11
So when you go to a hospital, they look at you, they think, Oh, well, this part’s not working, or that part’s not working, we can physically see that make that better for them, make that work for them, and send them on their way. And I know that does also help with the emotional recovery and the mental recovery, it kind of is a byproduct.
Bill Gasiamis 35:38
They’re related. They’re interrelated, I have to be, but that, I know that when people become physically active, or more physically active after show their spirits lift, and all those things get better, and I get it. But it’s not a direct approach to the emotional cover. It’s not actually doing emotional intelligence work, it’s not actually checking in with trauma, from previous experiences about your life that are sitting in your heart and impacting your heart, whether it’s a breakup, whether it’s a loss of a child, whether it’s just the stroke or the other condition that you’re diagnosed with.
Bill Gasiamis 36:17
So you have to do the specific work at the heart level to support you, and take that initial emotional recovery that started from the physical recovery to take it to the next level. Just like the mental recovery, you if you support the emotional recovery, and the physical recovery, your mental recovery also improves. But then there’s some specific things that you need to do.
Bill Gasiamis 36:48
At the head level, that is going to support you in your recovery, how you think about things, or how you take information from people or who you will let impact you and affect you. Or whether you’ve got thoughts in your mind that are not serving you well, because they’re just ill formed, maybe they were formed when you were a child. And you’ve kept those with you.
Bill Gasiamis 37:11
And you’re still continuing using the same method, and you’re trying to get a different result. And you’re going insane, because you’re not getting a different result. And you’re still going back there. You know, I’m describing me here, by the way, if anyone was wondering, Where do I know this stuff from I’m describing the guy that I was, and then the guy I became, and I’m still working to become because of the fact that I’ve gone to those three places specifically to do work that I was afraid to do.
Slaying The Dragon

Bill Gasiamis 37:43
And I just finished having a conversation with some a family member of mine. And he’s nearly 50 years old. And he will not go to the emotional center of himself and do that work where the trauma lies. And he clearly told me that it’s really hard and he’s never gone, then he probably never will. And that’s so bizarre to me that you’re aware of where the problem is, you know that you have to go there.
Bill Gasiamis 38:11
And something stopping you from going there. Let me tell you, when you go to where the problem is, you slay the dragon, it’s gone, that dragon can no longer control you, or influence you, it’s going to be hard, don’t expect that you’re going to go and slay a dragon easily and it’s going to be done. And thus it’s a task. And it’s going to be a big fight.
Bill Gasiamis 38:35
And you’re going to have to take a few blows, and you’re going to have to feel disheartened, then you’re going to have to feel all those things. But then you’re going to have to get up and go back there again. And every time you go back there, you take an inch back and an inch back and an inch back.
Bill Gasiamis 38:51
And before you know it, you’re an evolved human being and you’ve let go of the past. And now as trouble comes your way, you’re dealing with them individually, not the whole list of things that you’ve never dealt with, that are compounding and sitting on your shoulders and making life you know, more complicated and more difficult.
Angela Michelle 39:16
I think you bring up something really interesting because I think what you’re talking about is you’re building resilience.
Bill Gasiamis 39:24
I took all that time to say that.
Angela Michelle 39:27
Yeah, no, I mean, you’re building resilience and it is a mindset thing. So you know, I do multiple things. I was a photographer became a yoga instructor. I’m also a body image coach, and I work a lot with clients who struggle with body image and I always say it’s really about mindset. And we really have to do that deep emotional work in order to slay that dragon right to slay that dragon, that little voice that tells you you can’t wear that or you can’t do that.
Angela Michelle 40:00
And you know, a lot of my clients who have body image issues are everyday people who maybe haven’t experienced anything like we have. But I also get clients who have experienced some physical things, whether it be a stroke or another disease that has taken away parts of them, that I then have to kind of help them to see that we adapt. And that’s resilience is learning to adapt.
Angela Michelle 40:31
And I think when people stay, like so fixed, that’s when we don’t grow. So resilience is growth, it is doing the practice of, you know, like you said, like, you know, you chip away at it, right, and it’s not something you’re going to chip away all at once. And it’s going to be a perfectly formed, you know, statue of something, no, it’s something you constantly work at. But it gets easier with time, because you build that resilience.
Bill Gasiamis 40:59
Yeah, if you’ve been avoiding emotional trauma, and dealing with emotional trauma for 48 years, it’s gonna take some time to get to the bottom of that, and overcome that, you know, and I’ve been in counseling since I was 26, or 27, something like that. And that’s my gymnasium. That’s my repetition, I go to the gym, and do my weights, and I come out feeling better for having gone there, and being the lighter, resilient, stronger, whatever it is.
Bill Gasiamis 41:34
The hardest thing that I’ve ever had to deal with, personally, that affected me, my body was the strokes and the and the brain surgery, and it still affects me every day. And I don’t think I would have been able to remain to be in a positive mental state, I’m not always there, I have bad days as well, all those things. I’m a normal guy. I don’t think I would be this emotionally and mentally, as stable as I am, if I hadn’t done that work before the stroke.
Bill Gasiamis 41:34
So I had my strokes at 37 to 40. But I had already been in therapy for 10 to 12 years before then. And I can tell you that I had a “perfect upbringing” you know, my family life was great. My support networks were great. The people I grew up with, and the things that I experienced were all great, but we didn’t have any thing that I could say was a definite massive bump in the road for me.
Bill Gasiamis 42:37
So because I didn’t have any issues arise in my life, I didn’t have the skills to deal with stroke. If I had continued on my merry way and never been to therapy, I would not have a toolbox to dive into and take out some tools to help me get through stroke. And I wouldn’t have known that I can go back to my therapist immediately on the 10th day after I was diagnosed and begin the healing and the therapy once more, you know.
Bill Gasiamis 43:12
So that’s kind of where it’s at for me. And I hope that people have over who have been overthinking that idea of getting help and support or going to the emotional discomfort and tackling it head on. I think I hope that they stop overthinking it, and now just take action and do it. And then experienced the relief, the amazing relief once it’s done.
A Gift Of Perspective – Angela Michelle

Angela Michelle 43:42
Yeah, absolutely. I think that, you know, for me, seeing a therapist was huge in my healing in helping me to address things as they came at me and the way that I had to adapt. And I know this might sound totally out there, but I see my stroke as a gift of perspective. I know. But for me, it was a gift because I tell people, I learned things about myself. And I was forced to face things about myself at the age of 38 when I had my stroke that some people never face in their whole life, because they’re not forced to go there.
Angela Michelle 44:31
And my stroke forced me it took me way out of my comfort zone. And it forced me to address parts of my life and parts of myself that I needed to dig up. And in that way it was a gift. It was a gift of perspective. And I treat life so much differently than I did before. And that’s when I tell people that’s the gift that it’s given me and I can see I can be mad about the hard parts.
Angela Michelle 45:01
And I think I can personally hold the two truths, because that’s nuanced. I can hold the truth that it’s hard. But it’s also a gift of perspective. Because it’s forced me to think it’s forced me to address these shadow parts of myself that maybe I didn’t want to address before.
Angela Michelle 45:22
And I think if people can see, and hold those two truths, that then that can help them to move forward. Because, yeah, it’s awful. And it’s really like, shooting experience. But this time, there’s beauty, there’s beauty and the community that came out and supported me, the friends who have been there for me, my husband has stood by my side, there’s beauty and all that. And I can see the beauty in the darkness. And I hope that other people can do,
Bill Gasiamis 45:57
You have to have the darkness, you do, to allow the beauty to be illuminated, because that’s how it stands out you. You take it for granted that it’s there when you’ve had a gifted life or the perfect life. And I did, I’ve got to say that I had a perfect life until I was 37. And all my problems were created in my head, they were all bullshit, they weren’t true at all.
Bill Gasiamis 46:22
And, that was my undoing. It could have been my undoing even further, even worse and worse. And it was because I had never had the resistance of the difficulty of life to show me what I think is difficult is actually not true. That’s not difficult. That’s just fear that I’m allowing to control me. What’s actually difficult is waking up one day in the morning, not being able to feel your entire left side, and not having any control about how that happened.
Bill Gasiamis 46:58
And then putting your trust into somebody else to make a better for you. And you don’t know if they can, if they will. And if you’re going to see 38 And then what? And I’m not saying that I would like if I could go back, I wouldn’t change the stroke. I bloody would I would rather not have had it and not had brain surgery and not done all that stuff. But then I never would have gone into the deeper dive of personal development of challenging my beliefs of seeking out new and amazing teachers and people who are going to guide me and support me and teach me new things that were going to help me.
Bill Gasiamis 47:49
And I never would have been able to pass that on to my children. And I never would have been able to be an example of how to tackle something, as shit as stroke, and how to come out on the other side, banged up by it and wounded and a little bit molded by it but still come out victor, in my opinion. And then I would have not been on a podcast with Angela Michelle.
Angela Michelle 48:19
And I wouldn’t be here.
Bill Gasiamis 48:20
Yeah, you know, and we’re doing this thing that I never ever would have done. The before stroke Bill never, ever would have reached out to meet people on the other side of a planet, let alone for something like stroke, who I’ve never met before, there would have been a million reasons in my head that I would have made up to say, that’s not possible. Why would they want to talk to me, etc, etc. It just never would have happened. And here we are. I think this is going to be episode 201 or 202.
Angela Michelle 48:54
That’s amazing.
Bill Gasiamis 48:55
Yeah, it’s been a journey and a half. And it’s been such a good one. And now, you know you’re working in the accessible yoga space. I mean, what a gift, like what another gift for you to be able to A. participate in yoga, actively get a lot out of it, and then have the other emotional part that helping other people gives you because it’s a cycle, right. If you help others, it helps you and so on.
Angela Michelle 49:26
Yeah, I think one of the best things we can do as stroke survivors is try to find ways to be a service to others. And I think you do that with your podcast. And I think I do that through my advocacy work. And through all the other work that I do is of being of service to others. That’s a gift to us too, because it makes us feel valued and proud and like we’re contributing to something that’s larger than us.
Angela Michelle 49:55
And that comes back to the emotional right like we need that emotion Additional sense of recovery. And for me part of that recovery was being of service. And so when I decided to become a yoga instructor, it was because I knew I wanted to work with people like this, like me. I wanted to be there for people who didn’t think that yoga was accessible to them.
Angela Michelle 50:19
And, you know, I used to go teach yoga class, and I would teach like a general open class for everyone. And I was there with my oxygen. And I was teaching. And, you know, I’m like, I’m not here to show you how to do handstands. I’m not here to show you how to do inversiones. I’m here to teach you about yoga and like the emotional aspect and how it can help you transform your life.
Angela Michelle 50:43
And so like you said, you wouldn’t be doing this podcast, I would have probably never become a yoga instructor. And I would have never gone down the route that I have, because of a stroke, I’d probably still be burning myself out doing photography. And I was burning out, I really was, I still love it. I miss it. And I hope to get back to it soon. But it forced me to look for other ways to fulfill my life.
Sexology And Boudior – Angela Michelle

Angela Michelle 51:18
And the other thing I did, and I know I didn’t bring this up, but I do a lot of things is I became a certified sexologist. And because I did a lot of work with boudoir, it kind of fit in really well. And my specialty there is also in helping people with chronic illnesses and disabilities find intimacy in their life. And I think that that is another important element. And when I talk about intimacy, I’m not necessarily always talking to just about sex, it’s about intimacy, as far as like, just even like a hug, or a touch or a deep conversation of someone, it’s opening ourselves up to other people.
Bill Gasiamis 52:02
Let’s talk about that further. Because I never experienced the lack of intimacy, because of stroke, as in, I was able to participate in intercourse with my wife, all that stuff was all fine and normal. So I don’t have an experience in and I haven’t been able to raise the issue of it and the question of it and have the deep conversation about it, because I just don’t know.
Bill Gasiamis 52:36
And I haven’t come across anybody who has been willing to so far, but the only reason I had to refrain from intercourse with my wife intimacy in at that level was because the doctors told me not to. And I remember being at hospital and the first seven days, and then going home, and they said to me, now when you go home, no going, no doing any strenuous work, which meant that I had to stay home from work.
Bill Gasiamis 53:08
No doing this, no doing that. I said, can I go to the gym? And they said, No. And then of course, I asked the next question was, what about sex? Can I have sex? And they said, No. And my wife went all? Yeah, typical, of course, he would ask that question. And so we made sure that we took doctor’s orders and didn’t do that, because the blood vessel in my brain had burst, it was still leaking, and a high blood pressure episode, or elevated heart rate too much, or straining too much could make the bleed dramatically worse.
Bill Gasiamis 53:43
So we took their advice. But then at some point, things settled down. Because I’d say quite a few months later, when things settle down, and I kind of just said to my wife, we’re going to do this, let’s go there, you know. And it’s like, and whatever happens, happens, you know, what a way to go? All that stuff.
Angela Michelle 54:08
And there’s a way to go.
Bill Gasiamis 54:11
So we got through that. And, that was the extent of it. Right. But I know some people then have had serious strokes where they might have hemiplegia and they may not be able to physically get into certain positions or participate in the same way that they used to have you come across people in that space from other conditions doesn’t have to be from stroke, and how do you help? What are they the key things that they need to come to terms with or overcome to help them start to explore that space again?
Angela Michelle 54:52
Yeah, so I think everyone’s different. You know, everyone’s stroke is different, as you know. And so I do think it’s important that we talk to our doctors. I don’t know how it is where you are. But here, doctors aren’t trained much about sex. Which baffles me a little bit. So when you bring it up, sometimes they’re very, like, flustered and they don’t know how to respond.
Angela Michelle 55:19
Like I said, nothing’s taboo for me. And that’s part of why I do this work, because I can talk about these things. So I remember asking a doctor, like, is it okay, if I have sex? And they’re like, why are you asking me? And I’m like, Well, I don’t know. Like, I just had heart surgery, as you know, I feel like I should ask. So I do think it’s important to have a conversation with your doctor first.
Angela Michelle 55:45
And if you’re not comfortable having that conversation with the doctor, I think that you need to address that, whether it’s finding another doctor, or you know, finding another like medical professional, maybe it’s a nurse, or maybe it’s someone else who can have that conversation with you. I also think it’s important that we have conversation with our partner. In my experience, a lot of people who are with someone who’s had, you know, a devastating illness or disability, they’re scared to have sex with you, like, because they don’t want to hurt you.
Angela Michelle 56:23
And so you have to be able to have that conversation. One of the things that I really recommend, is, I don’t know how aware you are with kink, but in kink in the kink community, we do things like green light, red, light, or yellow. And so it’s like, a red is like, stop. A green is like, I’m good to go. And yellows like this is okay, but don’t take it further. And so that allows you and these conversations need to happen before sex before the intimacy because you need to be able to communicate.
Angela Michelle 57:04
And for someone like me, who may be getting shorter breath, right? Like, I need to be able to let my partner know like, I’m still okay, right? Or, hey, I need to back off, I need to catch my breath. And the same thing, if you have any kind of deficit, or pain, you know, you may be screaming out in ecstasy, but your partner may not know that they may think you’re actually in pain.
Angela Michelle 57:29
And so being able to have that communication will really help put your partner’s mind at ease. Because you could be like, No, I’m good to go. But your partner’s like, I’m scared. I’m not really sure. Then the other thing, I think it’s we have to adapt, because, you know, I talk a lot about adapting in the work that I do. But it’s so true. And it’s really true for stroke survivors as we’re learning to adapt to our new body, right?
Angela Michelle 57:56
A new old body. And so yeah, you may not be able to have sex the way you used to, but that doesn’t mean you can’t, right. So there’s other ways. And so sometimes it’s finding different positions, it’s using props, it’s using intimacy devices. It really at the basis boils down to that communication. But there are plenty of things that we can use, like the props like the intimacy devices that can help us to find that level of intimacy we want of a partner, even if our body can’t do what it wants did.
Bill Gasiamis 58:37
Yeah, that does make sense and that and see, I never would have been able to hold a conversation in that space. Because I’ve never delved into different forms of sexual intercourse with anybody about any, I’ve never studied it, I don’t understand that I’ve never helped anyone. So it’s like, how do you begin that conversation? I think that’s where a lot of people suffer, because sex was and always was, like, a certain way.
Bill Gasiamis 59:06
And whatever that way is, even if it’s a unique to you and your partner, it’s usually always a certain way. And then it’s like, how do you mix that up? Like anything? How do you adjust and change and find a different way? And, because sex is so taboo, there aren’t a lot of conversations about in your general, everyday life unless you’re hanging out in those circles. I couldn’t have that conversation with 90% of the people that I know I just can’t have a conversation about how, because what do you do different in the bedroom, you know, tell us so that we can try this?
Angela Michelle 59:49
Because I have these conversations with people all the time. But no, really it is about exploring. It’s about exploring your body, your partner’s body and also keeping a sense of humor. Because bodies, right, they’re weird. And they change. And the thing I tell people is our body’s always in a state of change, it’s always changing, right? Like, our bodies changed much faster, because we had a stroke. And it was like an instant, where our bodies change. Everyone’s body is always changing.
Angela Michelle 1:00:24
So learning to adapt to those changes, and, you know, it’s just gonna look different, and that’s okay. It’s okay, that sex is going to look and feel and be different, you can still find intimacy. And I think it’s important, because sex is a part of the human experience. And if it’s something that’s important to you, then it’s important to you. And it’s something that you need to, you know, for you to have the quality of life that you want, you need to address it if it’s important to you.
Angela Michelle 1:00:58
Now, sex isn’t important to everyone, you know, some clients are asexual or demisexual. And it’s like, you can take it or leave it. And so maybe those people are fine without it. But it’s a very individual experience. And so if it’s important to you, I think it’s important to find ways to adapt and explore, to make it a part of your life in a way that you’re going to enjoy in that is safe.
Bill Gasiamis 1:01:24
Yeah, I had an interesting conversation with Misha Montana, an adult film industry actress. And she was talking about how she had her stroke at 31. And she’s really involved in her films in the, I imagine in the production and the whole range of skills that are required to put a film together, not just in the acting. And she was really concerned that she wouldn’t be able to go back to work.
Bill Gasiamis 1:01:59
And she lived for a little while in denial about the stroke, because she had to go back to work. And she went back to work. And she kind of faked being well. And then she went back to review the films that she had made to see that she actually pulled it off quite well, then people, most of the people around her did a notice. But then X amount of months later, the acceptance or the fact that she had a stroke may have dawned on her or, you know, she has gone through the phases of denial and all those different phases.
Bill Gasiamis 1:02:40
And then people were surprised by her saying, I’m not feeling well, I kind of had a stroke and all that kind of stuff, because they were connecting her behavior at the beginning of the whole process. And her behavior now. And it’s like, you didn’t look like you had a stroke, you didn’t behave like you had a stroke, it didn’t tell us that you had a stroke. And now, you’re telling us that you are and it wasn’t computing, they were getting confused about what she was trying to say about how she was feeling nine months or 10 months later. And it was really interesting that in a taboo industry, like the adult film industry, that stroke is taboo. That was like, weird.
Stroke Being Taboo
Angela Michelle 1:03:29
I think it is taboo in a lot of settings. I mean, I think sometimes, you know, like people don’t know how to respond to it. Right? And I think especially those of us who’ve had stroke in our younger years, right? Like you said, you were 37 You said she was 30? Right. 31. I was 38. And so I think sometimes it is hard because, and, you know, I’m assuming it and she didn’t have a lot of like she didn’t physically look like she had a stroke. You don’t physically look like you had a stroke. I don’t think I physically look like I had a stroke.
Angela Michelle 1:04:16
And because of that sometimes we’re met with, you know, confusion or like are you sure? Like you know, or people like doubting our experience. And that can be really invalidating to us. And so I think it’s important that we, you know, face and embrace, like where we are in our journey. And I think that it’s important that we let those around us know like what our wants and needs are because we have to honor our bodies. We are at the mercy of our bodies. And so we have to be honoring them. And so I’m sorry that she had that experience but I hope that they are now in a place where they are empowered by their life’s experiences.
Bill Gasiamis 1:05:08
Yeah, I think a lot of people most people get there. I say that, well, look, most people that are my podcast get there because I imagine that some people who don’t get there, or are not there yet, and they haven’t been on my podcast yet. And they haven’t expressed that to me yet. So this is the people that this podcast is for those ones who are not there yet in acceptance and are not there yet, in going through different phases and are evolving and emerging from this somehow.
Bill Gasiamis 1:05:40
Misha has made it her thing now to overcome the taboo of stroke in her industry. And I’m pretty sure at some point, she was doing a documentary, or they’re doing a documentary or something like that, which is going to discuss the issues that she faced around stroke, and then having to go back to work in the industry to raise more awareness. So she’s got to the point where she is more determined than ever to tackle this other taboo in an industry that she’s tackling taboo in.
Bill Gasiamis 1:06:22
And she’s got the opportunity to do some amazing work, coz she got at least 50,000 followers on Instagram. And if the statistics are accurate, one in four people will experience a stroke in their lifetime, at least 10,000 of those people either know somebody who has experienced a stroke or has had a stroke, or will experience a stroke. So it’s great place.
Angela Michelle 1:06:50
She can be of service now. And that’s got to be very fulfilling for her to like, be a service, right? Like she’s helping other people. And she’s changing the culture around the tabooness of talking about our bodies, whether it be about sex, or about, like health. And so I think that’s amazing. I’m really excited to check them out, because I hadn’t heard of them before.
Bill Gasiamis 1:07:17
Yeah, yeah. I posted a question on my Insta. And it was as a result of somebody else asking me, has anyone ever been on your podcast that had vision problems? And the question I asked is, How do you manage? Or how have you adapted to vision loss after stroke, and you responded, and that’s what caused me to reach out to you and ask you to be on the podcast.
Bill Gasiamis 1:07:47
And you told me about the fact that you lost vision completely in one eye. And as a result of that, that impacted your ability to be a photographer. And then I asked you, so how have you adapted without your full vision into photography, and you mentioned that you had to step back from it.
Bill Gasiamis 1:08:08
So this is the part where I love to indulge with this little piece of me, which sort of says, I reckon you should get back into photography as a person with your knowledge about photography, and take it or leave it this advice. It’s not really, it wasn’t advice that you asked for.
Bill Gasiamis 1:08:33
So I don’t mind how it gets received. But from your understanding about photography, and with this different perspective that you have now because of the vision, I think you could do some amazing work. And it would be a compelling story. To hear how your photographic life has evolved and changed as a result of this challenge that has been thrown to you that you didn’t ask for.
Angela Michelle 1:09:10
I didn’t stop doing photography. I still photograph I do. I will tell you that the thing that made it the hardest, the vision loss wasn’t the hardest thing about coming back to photography it’s the lung disease. That was the hard part. However, I still photograph I said that God has a sense of humor because he took my right eye. And even though I’m right-handed, I’ve always been left-eye dominant.
Angela Michelle 1:09:43
So when I pick up the camera, I do that. I don’t have to do that anymore. Because I can’t see out of the sight at all, but it’s like muscle memory so my eyes still like does that. I can’t shut just this I for some reason. So I’ve always been left-eye dominant. So I never stopped photographing. Well, I stopped photographing at the start of the pandemic, because I was scheduled for lung procedures out in California.
Chronically Beautiful By Angela Michelle

Angela Michelle 1:10:13
And I stopped in order to go have these lung procedures. COVID delayed them about two years. But I actually just have my last procedure done last May. So I’m actually in the process of looking at getting photography back up and running. But in the meantime, I’ve still done personal projects, I still photograph. And my personal project that I’m really passionate about right now, is I photograph people with chronic illnesses and disabilities.
Angela Michelle 1:10:46
And it’s called chronically beautiful. And so I photograph people to show and share the beauty that exists in all of us. And it doesn’t matter if we have, you know, a body that doesn’t work the way that it used to. Like, there’s still beauty in us. And I want to show people that. And I want to show people to invisible disabilities and invisible illnesses. For me, mine is of visible, I think for years to you, it’s probably mostly invisible for you.
Angela Michelle 1:11:20
And so I want to show that too, is, you know, you have worse stroke survivors, we don’t always look like stroke survivors. I’m sure you get that all the time. As do I have like, well, you don’t look like you’ve had a stroke. And I always say, Well, what should I look like to you? Would you prefer? Yeah, how would you? How do you expect me, but I’d like to challenge them and challenge that. So I do still do photography, I stepped back mostly because of the lung disease.
Angela Michelle 1:11:51
The one thing I’ll say is, I can’t do it at the same level I did. And that’s part of the change that I know I have to adapt. I can’t keep up with the number of sessions I used to do because of the amount of doctor’s appointments and blood draws I have to go do my mom have weekly blood draws at the lab. And it would just be impossible for me. And then, you know, the eye thing. I always say when I’m behind the cameras kind of when I feel the most normal, because I would have shut my blind eye anyways.
Angela Michelle 1:12:26
So I feel normal. When I photograph, the hard part for me is staring at a computer editing photos for hours. That’s the hard part for me. And that’s why I say I won’t be able to do it at the same. What’s the word I’m looking for? Not the level. Yeah, I guess like the same, like the amount that I used to, like instead of doing like, you know, 20 shoots a month, I’m gonna probably only be able to do like seven or something like that. So I’m working, how that’s going to work. But the photos you see actually behind me, those are actually my photos that I’ve taken. So yeah, I still do photography.
Bill Gasiamis 1:13:09
And I’m looking at your Instagram. That’s why I mentioned a lot of your photos on your Insta. And I’m looking at him going like.
Angela Michelle 1:13:17
What Insta are you on?
Bill Gasiamis 1:13:18
Hi, Angela. Michelle.
Angela Michelle 1:13:20
Go to ravenredphoto.
Bill Gasiamis 1:13:23
Okay. Yeah.
Angela Michelle 1:13:24
That’s my photography work.
Bill Gasiamis 1:13:26
I think I was there a bit earlier. Yes, that’s it. I mean, I’m looking at those photos, and you’re a talented photographer. And whether you’re doing it for a living or for whatever reason you decide to doing it and go back to doing it. It’s just necessary, though, I think that you’re still doing it, because the photos that you’re capturing are really amazing photos. And that’s kind of where I was coming from. It was about me trying to encourage you thinking that you were discouraged and you weren’t doing it anymore, it was just me reading further into that message than what was actually happening.
Angela Michelle 1:14:08
So when I had my stroke in was 2016. I didn’t stop photographing until like I said, the beginning of 2020. And that was to go have additional lung procedures. COVID just kind of set everything back a couple of years. But no, I continued to run my business for several years after the stroke. And so yeah, it’s still my passion. It’s still what I love. It’s still a part of me for sure.
Angela Michelle 1:14:40
And I think that’s really important, too, that you bring that up though, because I think that you know, as stroke survivors, we have to find our passions and, you know, you can’t, don’t give up everything you love. You just may have to figure out a different way, whether that’s doing less, or doing it differently. Or you know, one of the things I did this year because I knew I wanted to start photographing more is I switched cameras, and I needed a lighter camera, I needed something that wasn’t as heavy.
Angela Michelle 1:15:11
My old camera was a workhorse, and it was heavy. And it was hard to carry around. And the other thing is, you know, because my right eye is gone, my left eye is good on a good day, bad on a bad day. And that’s from the clotting disorder. So I was struggling with focus. So one of the things I did is I went to a camera that’s got a better like, autofocus on it. So that way, I’m not missing shots that are, you know, important to me, because I’m not focusing, right. So finding ways to adapt to still do to what you love is so important, because that’s part of our healing, too. It’s part of our emotional healing, I think.
Bill Gasiamis 1:15:51
And I’ve met stroke survivors, who were musicians play guitar, you know, and the rest of it. And then, of course, they’ve lost the ability in one of the arms or hands or whatever. And at some point, you know, they got down on themselves, because they weren’t able to go back to play the way they used to. But they haven’t, they haven’t unlearned all the hours and hours of learning that they put into that.
Bill Gasiamis 1:16:24
And I just feel like they can still express themselves and just be creative about the way that they re express themselves. And that’s really what I’m driving at, just find a way I had no form of expression before that I just used to do my work and go home and be the kind of regular ordinary, everyday guy, and then I needed to start expressing myself.
Bill Gasiamis 1:16:46
And that was what was also part of how the podcast came to be it was I needed to find a way I needed to learn how to do it, I need to solve all the problems about podcasting, recording, equipment, editing, uploading all the junk syndicating and it’s like if I do that I’ll be able to connect with people have amazing communication with people that I have nothing in common with other than stroke.
Bill Gasiamis 1:17:14
But then we’re going to find similarities and things that we agree on. And things we don’t agree on, which is perfectly fine. And I’m going to be able to express myself. And I’m not doing it, believe it or not, it was a selfish pursuit at the beginning, it had nothing to do with you or anybody else, it was all about me. And then is when I realized that all about me, that’s about other people became this loop of amazing stuff.
Bill Gasiamis 1:17:43
And, I can see your photos. Some of them are just amazing, where you’re taking a photo of somebody, and then that’s a pursuit that you love, right photography, and capturing people images or whatever. And then you hand it over to that person, they look at that photo of themselves. And they go, Wow, that’s just amazing, you know. And I’ve responded like that when somebody’s taking my photo, and they’ve shown a side of me that I never knew was there.
A Deeper Connection
Bill Gasiamis 1:18:14
And it’s like, wow, and I think that you have now you have a greater ability to take even better photos, because of all the stuff that you’ve been through. And you can see things in people that you couldn’t see before. Whether it’s their light, or their mood, or whatever.
Angela Michelle 1:18:41
It’s about intimacy, because what it’s allowed me to do is connect to people. And I think that’s what you do on your podcasts too, is we connect to people, and we connect on this very deep soul level. And I think that that has made me a better photographer. And I think that that has taught me to really look at someone and see, like their soul for a better word, like who they are that light in them.
Angela Michelle 1:19:20
And then I try to bring that out. And so yeah, I think in many ways, it did it changed the way I thought about Absolutely. But I don’t think that’s bad. I just think it’s different. And that’s the thing I think about strokes is that your life is gonna change, but that doesn’t mean it’s gonna be bad. It’s just gonna be different. And we adapt. I mean, we’re so resilient humans, we’re very resilient.
Angela Michelle 1:19:48
And we have this ability to adapt. To me, what gets in our way is just ourselves. We get in our own way. Right. And so I think, you know, like you said that through three prong approach, the mental, the physical and the emotional, and having something you’re passionate about and something that can connect you to other people, you know, you do it through your podcast, I do it through yoga, through photography, all these other things, but finding ways to connect, will really help you in your own journey.
Bill Gasiamis 1:20:23
Yep. And do it about yourself, make it for you then make it for anybody else. And if other people happen to like it, maybe that’s a bonus. Maybe it isn’t, it doesn’t really matter. And I get really not inspired. But I really love the works of Frida Kahlo, the Mexican painter, who painted mostly self portraits of herself. And she was doing, you know, her version of a podcast putting out there things that were taboo to talk about in the 1930s and 1940s, about your illness and your condition.
Bill Gasiamis 1:21:04
And she would have broken down so many barriers by painting and depicting herself in this person struggling with her condition and all the challenges that she faced. And I look at it, I can’t say that she was and I don’t know anything about art. So in my mind, I don’t know if she was a talented or gifted artist or not. But she has amazing art, that tells an amazing story that was really important. And ahead of her time because she was a female in Mexico, drawing about taboo subjects, like living with chronic illness. She was a trailblazer. Nobody was doing that back then.
Angela Michelle 1:21:54
Yeah. And I think that’s what makes her art so compelling, is it connects on this like soul level to people. And, you know, I do think she’s an amazing artist. But I think it was her ability to transmute her pain, her suffering into something else. And I think that that’s part of the gift of for me, is like I’ve been given this, how am I going to transmute it. And, you know, I think you’ve seen like, on my social media, I call myself an alchemist. Because it really is about transformation. For me. It’s about transforming. How we think how we see how we interact with the world, how we connect, it’s about just that transformation that can facilitate so much healing and so much beauty.
Bill Gasiamis 1:22:50
I love it. On that note. That’s a lovely way to end the podcast, I’m going to share all of your social media on the show notes, so people can go and find them, click through to your pages. But just for the people that are listening, if they did want to find out a little bit more about the stuff that you do and connect with you, where would they go?
Angela Michelle 1:23:17
Sure. So I have a website. It’s a ravenredmaven.com. And then on Instagram, my photography is ravenredphoto. And my handle for my personal where I do a lot of advocacy work is HeyAngelaMichelle. And that’s h e y.
Bill Gasiamis 1:23:39
Fantastic. Thank you so much for being on the podcast. I so much enjoyed our chat.
Angela Michelle 1:23:44
Thank you so much, Bill. I really appreciate you and I love what you’re doing. So thank you for doing it.
Bill Gasiamis 1:23:51
Well, thanks so much for joining us on another episode of the podcast and listening to today’s episode. To learn more about my guests, including the links and to download a full transcript of the entire interview, please go to recoveryafterstroke.com/episodes You’ll find the episode in the list there. If you would like to support this podcast, the best way to do it is to leave us a five-star review, and a few words about what the show means to you, either on iTunes, or Spotify.
Bill Gasiamis 1:24:23
And if you’re watching on YouTube, comment below the video, like this episode and get notifications of future episodes by hitting the subscribe button and the notification bell and subscribe on the other platforms of your choice. Now sharing the show with family and friends on social media will make it possible for people who may need this type of content to find it easier. And that may make a massive difference to somebody that is on the road to recovery after their own experience with stroke. Thanks again for being here and listening. I really appreciate you see you on the next episode.
Intro 1:25:00
importantly, we present many podcast designed to give you an insight and understanding into the experiences of other individuals. The opinions and treatment protocols discussed during any podcast are the individual’s own experience and we do not necessarily share the same opinion nor do we recommend any treatment protocol discussed.
Intro 1:25:17
All content on this website at any length blog, podcast or video material controlled this website or content is created and produced for informational purposes only and is largely based on the personal experience of Bill Gasiamis, the content is intended to complement your medical treatment and support healing. It is not intended to be a substitute for professional medical advice and should not be relied on as health advice.
Intro 1:25:39
The information is general and may not be suitable for your personal injuries, circumstances or health objectives. Do not use our content as a standalone resource to diagnose treat, cure or prevent any disease for therapeutic purposes or as a substitute for the advice of a health professional. Never delay seeking advice or disregard the advice of a medical professional, your doctor, or your rehabilitation program based on our content.
Intro 1:25:39
If you have any questions or concerns about your health or medical condition, please seek guidance from a doctor or other medical professional. If you are experiencing a health emergency or think you might be, call 000 if in Australia or your local emergency number immediately for emergency assistance or go to the nearest hospital emergency department.
Intro 1:26:19
Medical information changes constantly, while we aim to provide current quality information in our content. We did not provide any guarantees and assume no legal liability or responsibility for the accuracy, currency or completeness of the content. If you choose to rely on any information within our content, you do so solely at your own risk. We are careful with links we provide however third party links from our website are followed at your own risk and we are not responsible for any information you find there.






