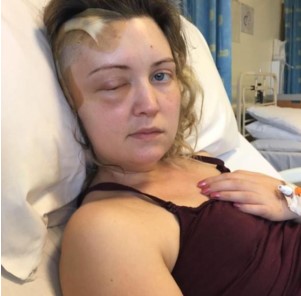
Ruth Carroll gave birth to her son on March 31 2017 and the very next day experienced an ischemic stroke which was a result of complications from a brain tumor.
Social:
www.instagram.com/ruthie_carroll84/
Highlights:
01:08 Introduction
01:46 Ischemic stroke caused by a meningioma
07:18 Doctor’s predictions
13:45 Losing Your Independence After Stroke
19:07 Grade 1 meningioma
28:58 During the early stage of recovery
34:43 Neuro fatigue
45:18 Motherhood during stroke recovery
56:06 The hardest part of the journey
1:00:19 Supporting stroke survivors
Transcription:
Ruth 0:00
You know, for example, my husband, we were newlyweds really, when this happened, we weren’t married quite a year at that stage coming up to a year. But for him, for example, you know, he married a very independent woman, and you know, within the space of a few hours, I was completely dependent on him, for everything to stand up to use the bathroom to move an inch, I mean, he had to do everything.
Ruth 0:31
The stuff that a newlywed husband shouldn’t have to do. So, all the little mechanics of standing up from the wheelchair, Dave had to physically lift me up and, you know, taking down my trousers, for example, I couldn’t do it. I didn’t have the stability in my body to even bend down.
Intro 0:54
This is The Recovery After Stroke Podcast, with Bill Gasiamis, helping you navigate recovery after stroke.
Introduction
Bill 1:08
It’s bill from recoveryafterstroke.com. This is Episode 131. And my guest today is Ruth Carroll. Ruth had to give up her independence as a result of an ischemic stroke caused by a brain tumor just one day after the birth of her son in 2017. Ruth Carroll, welcome to the podcast.
Ruth 1:29
Thank you Bill.
Bill 1:30
So is it Ruth or Ruthie?
Ruth 1:34
It’s Ruth.
Bill 1:35
Okay. Instagram has Ruthie. And sometimes I don’t know whether the Instagram name is the real name or not the real name.
Ruth 1:43
Yeah, course. No it’s Ruth.
Ruth Carroll had an Ischemic stroke
Bill 1:46
Tell me a little bit about what happened to you?
Ruth 1:50
So yeah, in 2017 April 1st actually April Fool’s Day. In 2017, I suffered a stroke. I was nine months pregnant initially with my first baby. And in my ninth month, I just started to get some swelling in my right eye, and my pupil became quite dilated. So I went to Specsavers to get that checked out.
Ruth 2:16
And I was advised to go into a&e to get an MRI scan. So of course, I did that. And I was diagnosed with a brain tumor called a meningioma. So we very quickly had to have a C section to get my baby out. So my little baby boy, Bobby was born on the 31st of March 2017.
Ruth 2:36
So he was perfectly healthy thank God the very next day, then it was less than 24 hours, it wasn’t quite a full 24 hours, I was back in his ward visiting him. And that’s where I suffered an ischemic stroke, essentially, because of the pregnancy hormones. It grew my tumor very quickly. And tumor growth blocks the flow of the blood flow to the brain. And that’s what caused the stroke. So I was left side paralyzed.
Bill 3:09
That’s too much for a new mom, a new baby, that’s just too much. That’s not supposed to happen, is it?
Ruth 3:17
No, not at all. It was a crazy time.
Bill 3:22
How do you manage the emotions that are related to that? Because there’s this amazing, beautiful reason to be happy and joyful. And then there’s this other stuff that’s happening. What do you do that? How do you manage?
Ruth 3:39
Yeah, you know what I don’t think my mind allowed me to take in the seriousness of it. You know, I just went obviously, I was very emotional, very upset, my family were distraught.
Ruth 3:54
But I just went day by day. My world was in the hospital beds that I was in, the nurses who were taking care of me, the doctors coming and going. And that’s all that I was able to focus on.
Ruth 4:08
You know, I couldn’t really stand back and think, Oh, my God, I’ve just had a newborn baby, I’m paralyzed, I can’t move. I wasn’t able to take in all of the trauma that was happening. And I just kind of let it go over my head really, and just survived day by day.
Ruth 4:26
That seems a common thing. When I’ve interviewed people who have had multiple life events happen at the same time as their stroke. It really is just let it pass through to the keeper and don’t worry about everything at once because it’s impossible.
Bill 4:46
Also, stroke survivors are not sometimes capable of creating those types of worries and connections because the brain has been switched off or is partially not working or there’s other stuff going on. Who took care of the baby?
Ruth 5:02
My, my husband poor Dave, my husband. I mean, he never held a newborn baby, you know, never change in nappies. So it was very traumatic for him as well as me and everyone else.
Ruth 5:17
Well, we live next door to my in laws. So Dave’s parents live next door. And they were a great support they took in Bobby, for a couple of months, I think, maybe two or three months. So Dave was able to go back and forth and be with Bobby. So that was a huge help and a huge relief for me as well, obviously, knowing that he has been taken care of so well.
Ruth 5:40
Did you have any challenges connecting with your baby? Because, you know, they talk about those first. few moments are really important. And then the next few months are extremely important for mom and baby to connect. Did you find later on any of those issues reflecting back on your connection with your baby?
Ruth 6:03
Yeah, you know, I was lucky, it didn’t impact our relationship. When I kind of stand back and look at everything that happened, it was the hardest part to deal with. Because Bobby was seven months old when I came home from hospital.
Ruth 6:19
So I essentially had missed the first seven months of his life, which, you know, is obviously very upsetting. But a lot of consultants in hospital, I saw a few neuro psychologists, I think, you know, had said to me, look, it’s probably likely that you will suffer from postnatal depression, after such a trauma the day after birth.
Ruth 6:43
So I think everyone’s expecting that to hit. But luckily, thank God that never happened. I think it was the support that I had, from family and friends, everyone, I was just surrounded with love, and support.
Ruth 6:59
My Bobby was brought into me every single day in hospital. So I did get to hold him in my head and on my chest. And that helped. Even though to be honest, I was out about half the time, and I was very fatigued. So it was you know, it wasn’t a lot of engagement with him.
Doctor’s predictions
Ruth 7:18
I get I get cranky when people tell me what’s going to happen to me. When doctors are trying to predict the future and all that kind of thing. They never normally try to predict the future in a positive light, they always try to predict the future in a negative light. What’s it like for you to hear that at that point in time? And did you pay attention to it? And then reflecting on it now, what are your thoughts on these predictions that doctors make?
Ruth 7:46
I can see why they made that prediction. You know, now that I’m so much stronger, I often find myself looking back going, Oh my god, I can’t believe that happened to me. And I can see how someone would slip into that postnatal depression.
Ruth 8:01
But I can see why. But I completely agree with you, in terms of doctors, focusing more on the negatives and the positives. One experience I had Bill when I was in our rehab hospital here, my left arm is still non functioning. The hand is completely paralyzed, but I am getting some movement back and the arm.
Ruth 8:23
But I did have a physiotherapist actually sit me down and say, Ruth, you’ll never ever get movement back in this upper limb, you need to just go away and learn to live life one-handed for the rest of your life, you need to understand that.
Ruth 8:39
It was heartbreaking at the time when I was told that and looking back now I’m like, you know, a positive slant would have been so much better. You know, for example, Ruth, there’s hope work hard and you’ll get this arm back. I can’t understand why they focus on the negative so much.
Ruth 9:02
In hospital, I put a lot of doctors in their place, especially when they spoke to me in this kind of way. If a physiotherapist told me to do that, I would have reported that person to their superior. And I would have told their superior that this person is not worth the salt, not worth their salt.
Bill 9:22
They’re not worth having, in an organization that’s supposed to encourage people to be rehabilitated and set an expectation of a long road forward fine set an expectation of very small gains, and maybe no gains for a few months and maybe no gains for few set all those expectations but never create the expectation that something is not going to get better.
Bill 9:45
I just think that’s the most terrible thing that somebody who’s helping is supposed to do and if any one of those types of people are listening whether there’s a doctor or nurse or a physiotherapist listening now, it is not your job to try and predict the future for your patient. It’s your job to help them right now.
Ruth 10:05
Absolutely, we should know, but nobody can predict the brain is so complex. And so plastic as well the whole neuroplasticity side of the brain. I mean, nobody no matter how amazing or educated they are, they can’t predict what each person’s individual brain is going how they’re going to react to the paralysis, whatever the trauma was.
Ruth 10:29
Another thing about It is what do they base their response on or that answer on? I know that they’re in their job, and they say lots of things. But they don’t have the data for every single person’s version of their stroke and outcomes.
Bill 10:47
So instead of knowing instead of just going based on I don’t know their version of the world, I think they just need to take a breath and just stop before they speak and just smile and encourage rather than the opposite, but I don’t blame them. But it really frustrates me and I don’t take it to heart anymore. But I could see how people would and then also set themselves up for failure.
Ruth 11:18
Absolutely. Because it demotivated me for quite a long time I found myself before she said those words to me, I was like, right, let’s go. Let’s work hard and physio every single day.
Ruth 11:30
And then she, you know, those words were said to me, and I found myself going off, why bother getting up early in the morning? You know, and work trying to work hard if there’s no hope. So really, it’s a really awful thing to do to someone.
Bill 11:44
Yeah. I going through the stroke journey that I’ve been through, at some point, I stop and reflect on what my experience is doing to the people around me. And it’s fair to say that the people around me, were losing their shit. While I was going through my stroke experience, how’s your stroke affected the people around you?
Ruth 12:11
You know, I think it’s actually worse for friends and family a lot of the time than it was for me, because as I said, just there earlier, you know, a lot of time, especially in the acute stage of stroke recovery, I had no awareness of what was going on or when I was in ICU and I was just out of it.
Ruth 12:34
You know it’s fine for me to just lie there while medics take care of me, but I mean my family where there watching all of that, they were completely distraught. So it impacts so many people. You know, for example, my husband, we were newlyweds really, when this happened, we weren’t married quite a year at that stage coming up to a year.
Ruth 13:00
But for him, for example, you know, he married a very independent woman, and you know, within the space of a few hours, I was completely dependent on him, for everything to stand up to use the bathroom to move an inch, I mean, he had to do everything.
Ruth 12:16
The stuff that a newlywed husband shouldn’t have to do. So I mean that’s had a hugh impact on his life, my parents had to give me alot more support now than they would’ve had to. So it impacts alot of people.
Bill 13:38
With regards to using the bathroom, forgive me for asking, but for the lung, or just to get you there.
Losing Your Independence After Stroke

Ruth 13:45
For everything, I mean, I was so bad I couldn’t hold my upper body up, I was just bent over to the left, absolutely zero movement. You know, so we have to get a commode into the sitting room in the house because there was no physical way that I could get out of the wheelchair and sidestep into our downstairs toilet, which is quite small.
Ruth 14:09
So all the little mechanics of standing up from the wheelchair, Dave had to physically lift me up and, you know, taking down my trousers, for example, I couldn’t do it. I didn’t have the stability in my body to even bend them.
Intro 14:26
If you’ve had a stroke, and you’re in recovery, you’ll know what a scary and confusing time it can be. You’re likely to have a lot of questions going through your mind. Like how long will it take to recover? Will I actually recover? What things should I avoid in case I make matters worse?
Intro 14:43
Doctors will explain things but obviously you’ve never had a stroke before. You probably don’t know what questions to ask. If this is you, you may be missing out on doing things that could help speed up your recovery. If you’re finding yourself in that situation? Stop worrying and hit recoveryafterstroke.com, where you can download a guide that will help you.
Intro 15:05
It’s called seven questions to ask your doctor about your stroke. These seven questions are the ones Bill wished he’d asked when he was recovering from a stroke, they’ll not only help you better understand your condition, they’ll help you take a more active role in your recovery, head to the website. Now, recoveryafterstroke.com and download the guide. It’s free.
Ruth 15:29
So nothing, absolutely nothing was possible to do on my own. So he did have to step up and do everything.
Ruth 15:36
That’s dramatic. And I remember being out of I think it was out of surgery and being in hospital and needing to go to the toilet, but the nurses weren’t answering my buzzer. And I couldn’t walk, I couldn’t use my left side at that point in time. I hadn’t been to rehabilitation yet I was waiting to get to rehab.
Bill 16:02
And I was using a wheelchair and they weren’t coming. And I needed to go because they’d given me laxatives after surgery to get the bowels moving and working and everything running again. And the laxatives kicked in, and there was nobody there. So I dragged myself with my right side of my body into the wheelchair to start pushing myself towards the toilet, which was maybe five meters away.
Bill 16:32
And by the time I got to the toilet, the nurse came and said, What are you doing? And I said, well, I just want to get to the toilet because these laxatives have kicked in and I need to get there. Let’s not talk about it. Let’s just get me there.
Ruth 16:47
Exactly.
Ruth 16:48
They finally got me there. And when they got me there, they wanted to stand inside the room while I did my business. And I said to him, No, you can’t please, you can’t do that you need to get out. And they wouldn’t get up for safety reasons. And I was having argument with these people, amazing nurses at the toilet.
Bill 17:08
And eventually I convinced them to go I told them I promise I won’t move. I won’t get up. I won’t try and do anything. I just need you to get out. Because I couldn’t imagine what it would be like for me to have them in there while I was doing my business not to mention, what do you talk to somebody when they’re watching you in the toilet?
Ruth 17:26
I know. It’s awful. I’ve been through all of that. It really, I just found I had to switch off. You know, and really not focus on the fact that, you know, there was it could be a male nurse standing next to me while I was on the loo chatting about the weather. I mean, embarrassing stuff.
Ruth 17:44
But it was just it was reality. You know, there was no other way I wouldn’t have been able to be left alone. You know, I would just flip over to the left hand side and be on the floor.
Bill 17:57
Well, you understand, have you spoken to your husband about those times? Have you guys reflected on that time?
Ruth 18:05
Yeah, he mocks me. You know, he’d always say you owe me big time. We can look back and laugh about it now. But at the time it was upsetting. Which has it’s funny now.
Bill 18:19
How old were you both at the time when this all happened?
Ruth 18:23
I was 33. Dave was maybe 38, 39?
Bill 18:34
Did you both take vows that said something like in sickness and in health and all that?
Ruth 18:39
Yeah, we did. So yeah, we really stuck to that.
Bill 18:43
Poor guy. He never knew what he was getting himself into when he said those vows.
Ruth 18:48
Exactly. Yeah. I’m very lucky to have him. No, he’s great. very supportive.
Bill 18:55
Sounds like you guys are gonna get through this difficult time. Where are you at with the diagnosis and with what was discovered in your brain?
Grade 1 meningioma
Ruth 19:07
Yeah, so they basically discovered it was called a grade 1 meningioma tumor, which is actually my neurosurgeon said to me, if he had to pick a tumor to get that would be the one he would pick. It’s not a very dangerous tumor itself. Not that anyone would be picking that but the problem for me it was the location of tumor.
Ruth 19:32
It was wrapped around my optic nerve behind the right eye. And it was going right through the carotid, the internal carotid artery, which is a very dangerous and very important artery to supply blood to the brain. So the location of it was a big problem.
Ruth 19:49
So there was a lot of conversation between my family myself and our neurosurgeon, and he kind of bounced ideas and procedures with us. They’re neurosurgeons not just in Ireland, but in Europe and America. I think he said he went as far as. So it was a lot of a lot of discussion about that before the surgery took place.
Ruth 20:11
So I had a craniotomy, then, in April 2017, and that removed the tumor pretty much removed about 98 point something percent of the tumor. I still do have little crumbs left, but there are luckily fine. They just have to be monitored every six months. Yeah, to make sure they don’t grow.
Ruth 20:36
How’s your emotional state leading up to that next appointment? Do you find yourself being cool, calm and collected about it? Or do you have a different experience?
Ruth 20:49
When those MRI scans are coming up every six months? I’m nervous. You know, my neurosurgeon is great guy, Dr. McNally. As in, he’s really relaxed and casual. Like the last time I went in, you know, you’re waiting there. And he comes in Hi. And I’m, like, no, no chitchat just say yes, how is everything?
Ruth 21:10
You know, and he’s like, it’s fine. Everything’s fine. There’s no problems. He’s really relaxed about it. And, you know, he said to me, the last time Ruth if those crumbs were going to grow, you’re looking at 10, 15 years for those crumbs to grow.
Ruth 21:25
So, you know, he was like, I wouldn’t worry about it. We just keep an eye on it. So he’s a very relaxed kind of person, which helps to relax me. But yeah, quite nervous, though. Coming up to it, just in case. You know.
Bill 21:40
How do you enjoy being in the tube of the MRI scanner?
Ruth 21:45
You know what, initially, I hated it, the noise and I was quite panicked. But now I have had so many, it doesn’t faze me at all. The last two scans that I had, I actually fell asleep. I was coming out. And you know, I was woken up to Ruth tap, tap tap.
Ruth 22:04
I was like, Oh, that was quick. I mean, they were laughing at me going. It’s not often people fall asleep. I actually found the noise quite relaxing. I’m a pro now. I’ve done so many of them.
Bill 22:16
Interesting how many do you reckon you’ve done?
Ruth 22:20
Like, I don’t know, I was in about four different hospitals here in Dublin, and Ireland. I mean, I don’t know 50, maybe. I mean, I honestly spent my time being transferred from my wards or my room, to the MRI, or a CT scanner, back and forth, back and forth. I felt I was doing that every every few days.
Ruth 22:45
Now, that’s quite the record, I reckon that’ll be up there. I think I’ve done maybe over the five or six years that I was getting scanned, I think I’d probably done at least, I’d say maybe 15, something like that. And by the end of it, I was doing the same thing. And because you can choose your own music, I was choosing meditation, kind of music.
Bill 23:08
So I’d go in there and meditate. And that would get me through very quickly and make it feel like it went fast. And also, that was really it was almost putting me to sleep. But I’ve got to say that’s awesome. What you’ve been able to achieve. I’ve never felt asleep.
Ruth 23:26
I did have one scan, and I came out and there was two guys and a girl and they were giggling when I came out. And they were like that was some good singing Ruth. I was like what? They were like obviously they can hear everything through the speakers. I didn’t realize I was singing away that was embarrassing.
Ruth 23:46
Yeah, I found you on Instagram. Where is the most amazing place where I’ll find all my guests and other people who would discuss things that are stroke related. It’s become kind of a community of a lot of familiar faces and new faces coming in and out. How long? How long have you been on Instagram? And why did you choose to get on there and do what you’re doing?
Ruth 24:16
I joined Instagram, I think it was last summer sometime. And before that I was absolutely clueless when it came to social media. I did have a Facebook page. And when I was traveling, I threw up pictures, more for my family and friends to see. But I just wasn’t glued into the world of social media and I had no interest in it really.
Ruth 24:38
Until all my friends and everyone I knew started going on it. So someone said it to me a friend of mine said you know you should talk about your stroke experience. And you know, there could be someone out there who you might help. So then I was like that I like that idea instead of just posting you know, when I go out for dinner, what I eat and all that kind of stuff.
Ruth 24:59
I though, there was a reason why I should do it. So I just set it off last summer. And it is amazing. There’s a whole community of people out there who have had strokes, like young people. I’m, really enjoying Instagram, I must say, the amount of messages I get from people if I post a video positive, and then no, no, no negative comments, really.
Ruth 25:24
But people looking for further information. And it’s great. It’s a good feeling to be able to help someone, a lot of people, you know, would come on to me going, Oh, I never knew that you could do that exercise for your arm, for example. You know, so it’s nice to share what knowledge I have. So I’m really enjoying it.
Ruth 25:46
Yeah, it was selfish. When I started this whole journey. It was selfish, it was about me. And I quickly realized it wasn’t really about me, it was about other people. And what I say it was about me was, I found that as a way of expressing myself made me, you know, ease the burden and get things off my chest.
Bill 26:08
And then it started helping other people. And then that completely changed the the type of satisfaction that I was getting from posting. It was a twofold It was a two way path. It wasn’t just me getting things off my chest and making it about me. And the other part of it is the more addictive part of it.
Bill 26:33
It’s when somebody says thank you, or I needed to hear that or asks another question. That is something I can’t stop doing. Because I never knew that what I had to share was important enough for other people to, to hear.
Ruth 26:51
To connect with. Yeah, and the exact same. I remember a moment I was in a hospital called St. James’s hospital here in Dublin. And I was in the stroke Ward, it was quite early days. And I just remember I was turned on my right hand side, you know, probably in my queue, I needed three nurses, or healthcare assistants to actually turn me on the right hand side while protecting my left shoulder.
Ruth 27:16
But I just remember lying there, and I have my phone up to my face. And I was thinking, I thought I was the only person in the world at 33 years of age who has had a stroke. And I typed into YouTube, I just said, you know, young stroke survivor girl, and a video came up of this girl, she was 33 as well, when she had her stroke, really a beautiful girl with long brown hair.
Ruth 27:45
And she came onto the camera, you know, and she started talking, she was kind of she was normal, she was happy. And she was like, Look, you know, this is awful what happened, but it’s not the end of the world. And then the next video from her was her walking in the park with her mom.
Ruth 28:04
And I can’t explain to you the hope that that gave me. I was just so happy to see that. And so hopeful. So I often think you know, if there’s some girl or guy out there in the hospital bed, if they could see me on Instagram, you know, doing well. And just, you know, to be able to help them the thought of that is amazing.
Ruth 28:27
That’s the point of this podcast. It’s the point of it is, you’re gonna be 131 episode. And that’s the point of it. The point is it to have, I’m not sure if it gets to 1000 but 1000 ways that people can find other stroke survivors who are post stroke at some point. And they can just say, this is how far I’ve come even though I’ve got all these dramas and problems and things that haven’t been resolved yet.
Ruth 28:55
There’s still life after stroke.
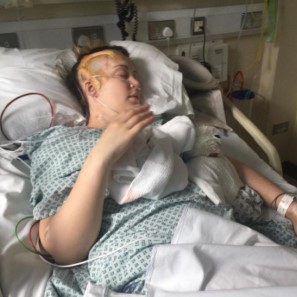
Ruth Carroll during the early stage of recovery
Ruth 28:58
Yeah, I’m still doing stuff. I’m still on an interview. I’m still meeting people. I’m still getting back to work. I’m still recovering all those things. I mean, it’s so important your mindset in hospital, was it doom and gloom? And if it was, that’s fair enough, is how would you have described your mindset when you’re in that really early stage of recovery?
Ruth 29:24
It was it was doom and gloom and it was fear was my main feeling. I was just so afraid. Like I couldn’t foresee I couldn’t get my head around the fact that I was paralyzed. It was just such a crazy thing to me, looking at my body and trying to move it and not being able to so it was a lot of tears, a lot of crying. I was completely in shock as well as my family.
Ruth 29:52
But my mindset is stronger than I thought. You know, I still luckily have a lot of motivation and drive. You know, I was the type of patient who, you know, was saying, I want more physio, come on, can I have another ot session and bring it on, you know, I don’t want to just lay here in the bed. So I was driven. I was like that before the stroke as you know, in terms of work and in my personal life.
Bill 30:24
What kind of work did you do?
Ruth 30:27
I worked in marketing as a brand manager. For McDonald’s. I was there for 10 years. So it was a busy, stressful, fast paced job. In a way, this brain injury was one of the best things that happened because I’m no longer working, I’ve been advised not to work for for a good few years.
Ruth 30:49
So I’m enjoying this new way of living, you know, stress free. And, you know, I’m getting great quality family time in that I know I wouldn’t have got if I was still stuck in that crazy world of stress and work. So there is a positive in every negative situation. I’ve learned that it’s just about making yourself focus more on the positive and the negative.
Ruth 31:16
Yeah, and give yourself enough time to see the positive as well, because sometimes it’s hard to see when you’re in that acute stage. It’s interesting that lockdown has been similar for me in that again, when we were in COVID lockdown here in Australia in Victoria, we were locked down for six months solid, we had nightly curfews we weren’t allowed to work almost under any circumstances.
Bill 31:46
We had nowhere to go, nothing to do. We weren’t allowed to meet with people anywhere. And Australia being an island has been able to really maintain, maintain its ability to decrease the number of cases of COVID through these really severe lockdowns, which people hated and I hated.
Bill 32:08
But as a result of that, we’ve come to that point where there are very few daily cases and almost no cases from community transmission. And I was going through that lockdown at one stage thinking this reminds me of my stroke. Recovery when I came home from hospital and my wife went back to work and my kids went back to school. I was alone at home doing not much most of the day.
Bill 32:37
And that was a really good time for me. Because when I came home, the noise was too much for me to handle. The business was too much for me to handle. My brain really needed recharge time, I needed to not be overwhelmed so that I could manage for the three or four hours before bed, and before dinner and all that type of thing.
Ruth 33:03
Yeah, absolutely.
Bill 33:04
What kind of things do you have to deal with now that are related to the stroke that you have to pay attention to and be careful of?
Ruth 33:14
Yeah, so for me, it’s mainly physical, you know, the, I can walk independently now. But for a long time, I needed a cane and I was in a wheelchair for a long time. It’s my left arm and hand that is my main physical disability really, cognitively, I was quite lucky that I wasn’t too impaired.
Ruth 33:36
I suppose in the early days, like you mentioned there Bill, my brain was very sensitive to noise or to distraction. You know, I remember I was being wheeled down to the patient’s canteen in one hospital. And there was definitely over 100 people in the canteen eating, you know, the noise of the cutlery people walking past.
Ruth 33:59
And I mean, I had to scream to say get me out. It was so overwhelming. My brain just couldn’t, couldn’t deal with it. Even you know, if I was sitting in my wheelchair and someone walked past I was like, Wow, it made me dizzy and made me feel sick. Everything was just so overwhelming in those early days.
Ruth 34:20
But naturally, that just seemed to improve over time, thankfully, but I had problems initially, with concentrating. I found it hard to concentrate for a long period of time. You know, I could be having a conversation and I might just kind of switch off because that’s improved as well.
Neuro fatigue
Ruth 34:42
But my main issue from this whole brain injury is fatigue. This neuro fatigue I find really, really difficult. From day one. It’s been my biggest struggle, and now four years on, it’s my biggest struggle. It’s, crippling is the word I would use. I mean, it impacts every minute of every day.
Ruth 35:09
But, I’m learning to, to tackle it better. You know, I’ve come up with a few strategies to make life a bit easier. Like, you know, I have to plan out my day now, even before you and I spoke today, as the most recent example, you know, I went out for a walk with my husband and son in the park.
Ruth 35:30
And we went to the playground and a lot of people there, you know, talking and catching up with a lot of people. But I knew that I had to do that early on. So I could come home and relax, and go up and get my 40 minute nap. And then I’d have the energy to sit here and talk with you.
Ruth 35:47
But, you know, if, for example, I had done that a couple of hours ago, I would find it very hard to to sit here and engage with you. So I just have to be smart. And I have to plan out the day, I have to plan in my naps. So I do get at least 140 minute nap in. And once I can lay down and switch off the brain, I’m energized then. You know, which is great.
Ruth 36:11
Yeah, that would be very familiar to a lot of people listening. And the fatigue to me, although was debilitating was one of the hardest things I had to put up with as well, was a really good way. It was something that taught me to pay attention to my body for the first time and to listen and to respond not only just know that I’m about to get tired, but also respond and do something about it.
Bill 36:41
I did all the same things that you say that you do, which is plan my day. And I would often we have some plans for the weekend with my wife. And I’d say, Listen, don’t make any plans for tomorrow. Because I don’t know if I’m going to be up to all the things that you want to do. And that was about me, don’t make plans for me. And then I would wake up that Saturday morning. And I said to remember that thing that I said yesterday about Mike my plans. I’m feeling great. Let’s go for it.
Ruth 37:13
Yeah, you just never know. I mean, the days that I should be exhausted, and say I went out for dinner with friends for four or five hours talking. And when you think the next day, next morning, I’d be exhausted, I could be bursting with energy. And vice versa when I should be alert. I mean, I could read on the floor with exhaustion, it’s really hard to figure out fatigue, I find you just never know when it’s going to hit.
Ruth 37:42
And I can just hit like that, you know, I could be absolutely fine one minute, and the next minute, I would struggle to hold my head up myself, it would just take so much energy to do that. And people don’t see how difficult fatigue is.
Bill 38:04
One of the things that I found that was making my fatigue worse was my thyroid function. The neurological fatigue that occurs from the thyroid gland that is not working optimally, is exactly the same as neurological fatigue after they had been my head.
Bill 38:21
And I developed a thyroid condition a few years before my brain issue. And it was an ongoing issue after the brain surgery. And we hadn’t done anything about the thyroid, because I was still fresh from a brain injury. And I got to the point where I didn’t know that my thyroid was causing the neurological fatigue, I thought it was related to my head until I went to a chronologist.
Bill 38:50
Who said by now the fatigue that you’re experiencing is more likely related to your thyroid challenges rather than your head challenges. So one little tip that may or may not have anything to do with what you’re going through is for people listening is to get their thyroid checked out just as a general thing that gets them some blood tests get a urine test.
Bill 39:15
That’s the best way to get the thyroid checked out. Because sometimes if the thyroid is underactive, and it’s under duress, or you’re not consuming enough iodine, sometimes what happens is the brain needs more resources than it used to, to get us through the day. And going everywhere, it’s going everywhere to try and get resources and if the thyroids not working optimally, it might struggle a little bit.
Ruth 39:49
Yeah, I never heard of that. That could really be another problem. That definitely contributes to my fatigue is anti-seizure medication that I’ve had to started taking, I developed focal epilepsy after my craniotomy just due to a tiny scar that was left on my brain while with the surgery.
Ruth 40:10
So as a result of that I have to be on and I will have to be on for the rest of my life anti-seizure medication. The first medication that I was on was called Keppra. And that the main side effect of that, and supposedly every anti-seizure medication is fatigue, I had to come off Keppra.
Ruth 40:30
I mean, it was I couldn’t function. I couldn’t get through the day fatigue wise on that. So I did switch over to another one that I’m currently on called Lamictal. And I did see a slight improvement initially, but then it got bad again and back and forth. But my neurosurgeon said to me, you know, what, one time I was talking about the different strategy strategies I was putting in place for fatigue.
Ruth 40:56
And he said to me, Ruth, at the end of the day, your brain is damaged as a result of the stroke and the tumor. You know, no matter how many good strategies you have in place, you are going to have neuro fatigue, until the brain fully recovers.
Ruth 41:13
Yeah great advice. And I feel like my fatigue is mostly gone. But then it still comes I’m nine years post my first stroke and brain surgery was in 2014. So I’m nearly on beyond six years after brain surgery. And I have those days where I’m having a great day, and then the wall just turns up out of nowhere, I hit that wall.
Bill 41:40
And then it’s just tools down and has nowhere to go or do anything and it’s just relax and rest and go to bed early. And then I fully wake up the next day feeling better. But some days, if I don’t get a good night’s sleep, then then the struggle lasts two or three days.
Bill 41:58
And I’m supposed to be online every two or three days doing things. And if I go quiet, I go quiet. There’s nothing I can do about it. I’m not worried about it. I’m not concerned about it. I just go quiet and gather myself and then I get back to doing what I have to do.
Ruth 42:16
Yeah. And so people handle fatigue better. What I mean by that is, you know, my family, for example. They are well educated on neuro fatigue. And you know, they’ll know, you know, if I go home down to South of Ireland, where I’m from County Cork, you know, my parents and my sisters will say to me, okay, we’ll do this, we go shopping, we go see the nieces and nephews do everything that I love to do.
Ruth 42:44
But you go you sleep, and then we’ll do this. So they get it and they encourage it but I find other people don’t understand this and kind of like why aren’t you coming here? Why aren’t you doing that? Why do you need to go home and rest? What’s it’s other people’s understanding of it is different I find my experiences are.
Ruth 43:06
It’s just ignorance and not in a negative, bad way. Like they’re ignorant about fatigue and stroke. And why would they know about fatigue and stroke? You know, fair enough, better they don’t ever know what that’s like. But if they want to be less ignorant, they can just read a little bit about it. Someone just do a Google search and you’ll find enough information to explain what neurological fatigue is.
Bill 43:31
Lights used to make my fatigue terrible if I’m sitting on the couch, you know, watching some TV, I cannot have the lights over my head. Because it just makes me suffer. I can’t do it. It hurts my brain. And people don’t understand when you explain to them that my brain is hurting. How? How is it hurting me? How is that even possible? But it does hurt I don’t know how.
Ruth 43:58
Yeah, it’s like a physical pain almost. With me I find people with different energy affects my fatigue, you know, you might come across a bit like you and I barely seen, you know, we don’t know each other very well. But a relaxed kind of person. But there’s some people out there who are hyper and want a lot of energy from you.
Ruth 44:22
How are you tell me what you did yesterday. Give me all the details and the information. You know that happy, loud, bubbly people. But I find that exceptionally draining, so I’m more comfortable hanging out with chilled out kind of not quieter people but people who don’t demand as much energy. Does that make sense?
Bill 44:43
Yeah, completely. I know exactly what you mean. And those people are the I call them the woo woo people, you know, the ones that just go nuts and they go off all the time. And they’re lovely but.
Ruth 44:57
Yeah, exactly. You have to learn to walk away and switch the brain off. You know, and come back refreshed then.
Bill 45:08
Yeah. How is your, how you manage now coping with running around after a toddler?
Motherhood during stroke recovery

Ruth 45:18
Yeah, I’m it comes back to support. Again, I’m lucky we have a childminder, who helps to drop Bobby and my little boy to school. And she collects them afterward and brings them home to me a bit later in the afternoon. So that allows me time to get to my physiotherapy and my hydrotherapy.
Ruth 45:37
And I do my home exercises here, and I get my nap in. So I’m ready for him when he comes in. And that makes such a difference. If I didn’t have those few hours to prepare, and to get my work done, and to get out and get a walk in fresh air helps with fatigue as well. And so it can be difficult at times.
Ruth 45:59
And it makes me feel guilty a lot of the time, because if I didn’t have this, nauro fatigue to be battling every day, I would be engaging with my son a lot more doing more things with him. A lot of the time, I have to almost not ignore him but not engage with him as much as I’d like to do you know, so that I can survive until the evening until my my husband is home. You know, so there’s that battle to deal with as well.
Ruth 46:28
Most normal people try not to engage with their kids as well, for various reasons. So you’re just using your health reasons as the reason to not engage at the moment. And it’s pretty legitimate. It’s not, it’s not terrible. I mean, you’re not doing it because you’re a terrible person. It’s legitimate.
Ruth 46:51
Exactly. And he’s at the stage now he’s three and a half. He’ll be four in March, that he understands it. Now, you know, he might say to me, are you going to go up for a nap mommy? And you know, he gets it and he knows when I’m, you know, getting a bit tired, Or, you know, he knows Mommy’s going up for a nap now, he knows that. It’s not strange to him.
Bill 47:18
Children are very smart. Does he ever asked you about your hand? Have you had a conversation with him about what’s going on there?
Ruth 47:25
He does it actually, initially, it definitely has affected him. You know, I’d say about a year, maybe a year and a half ago, he started to get almost obsessed with my arm, you know, and he’d get a bit angry with it. You know, he’d come over and be like, slapping us pinching advising us.
Ruth 47:48
You know, I’d be like, stop and he’d be like, your sore hands Mommy, and it would just became a thing to him. So that was something my husband and I were a bit concerned about. You know, he’s clued in he knows little things like, I’m not able to zip off his clothes before we go outside and he gets pissed off.
Ruth 48:07
He’s like, come on, zip up my clothes. I know you have a sore handy but come on, you know, there’s things that I can’t do that, you know, all other moms can do. You know, I’ve never been able to pick him up with two hands, for example.
Ruth 48:22
And he did go through a phase where I he’d pick me up mommy. So he’s very clued in. He knows that there’s something not right there. So he just gets annoyed and peed off with my hands. And my arm but he’s coming around that now.
Bill 48:38
Yeah. When he’s pinching and biting your hand, can you feel it?
Ruth 48:43
I can yeah, sensation is wrong. When I say that, you know, like, someone could be hurting my shoulder. But to me, I feel like the pain is on my wrist. So like the pain receptors to the brain are all wrong. I’ll give you an example. Early on in my recovery when I was in my wheelchair.
Ruth 49:05
I remember going outside the front door of the hospital and it was raining. And the raindrops hitting my left arm. It was as if every droplet was stabbing me, the pain I was like get me inside quick cover me up. So this sensation, is I can feel but it’s all wrong. If you know what I mean. I’m screaming when he’s pinching and biting me.
Ruth 49:31
Shower, me sometimes causes irritation on my left side. And when my wife is gentle, say if I’m driving the car and I have my left hand on the gearstick and she leans over, reaches over to put her hand on my hand, just gently.
Bill 49:51
I can’t do that that’s really painful and it does it instinctively and I rip my hand away and appears to be the meanest thing you could possibly do, but she started to understand that it’s not me being mean, it’s seriously painful. But if you grab my hand with force, it doesn’t hurt. It hurts when you do it gently.
Ruth 50:17
With me sometimes. And I mean, it sounds crazy. But I have sometimes found myself going, where’s my left arm? I, like I’ve said to Dave, I’m like, Can you see my left arm? I can’t find it. I mean, how crazy is that? But perception of where the limb is has always been a problem.
Ruth 50:37
You know, like, I might wake up in the morning, and my arm is under my bum or under my legs. And I wake up going, Oh, God, something is wrong. There’s pain somewhere. But I don’t know. My arm could be up there. It could be down here. Trying to figure out where the arm is in space. It’s quite difficult for me. So people laugh at me when I say Did you see my arm? I can’t find it that’s weird.
Ruth 51:06
We went to the beach yesterday in Melbourne, it’s summer at the moment, we had a quite a hot day it was you know, 35 or something. And I sit under a beach umbrella and make sure that I don’t get too much sun because I don’t really enjoy getting sunburned or any of that junk had a swim.
Bill 51:24
So I had my shoes off we’re sitting on the sand under the shade it was fine. And then a friend of mine came to the beach, to let me know that he was there. So I went to find him. And I waited without shoes. And because it’s the sand, I can normally walk on the sand fine without shoes.
Bill 51:41
Little pebbles of rocks on concrete. Feels like I just stepped on the most jagged rock. And it was the size of the moon. And it just destroys my foot is what it feels like. So I very much avoid it however, I was walking on the sand and it was all fine. And I realized that my feet were getting hot, too hot for me to continue walking on. So I was trying to find a cooler place to step on.
Bill 52:09
And when I came home about two hours later, I realized that on my left side, I actually had burnt my foot and had blisters underneath it. Which I didn’t notice at the time, I didn’t feel the pain. Didn’t know that that was burning to the extent that it was causing blisters. So I have that thing as well. Where hot doesn’t register quickly enough. But cold is more painful than hot for me.
Ruth 52:41
Yeah, I’m similar enough I’d often have the sink on upstairs and you know I’d get a nice and hot for my good hand. But without realizing it. I might have my left baby finger in the water. And the pain is incredible. And it might just be maybe lukewarm. To me it registers like I’ve just dipped my hand and lava you know, it’s it’s just all the sensations are wrong.
Bill 53:11
How do you manage the shower?
Ruth 53:14
Yeah, we had to get a walk in shower when I came out of hospital because the previous one we had had the most humongous step. You know, which is very difficult, which was very difficult to would be stepping in and out of that without my footstool.
Ruth 53:29
So we basically got a walk-in shower, and we did get a rail put onto the wall. So that’s been a lifesaver. So I depended on that alot in the early days, but it’s there now just for a bit of security. But I don’t need to hold on to it for dear life anymore.
Bill 53:47
Yeah, that’s a relief when you don’t have to do that anymore in the shower. I remember that as well. That phase of thinking I’m gonna slip and hit my head, especially with a craniotomy was that was a real concern of mine.
Ruth 54:01
Yeah, oh, yeah. We had to get that gripped tile everywhere as well for safety. But then I remember when I was in the rehab hospital, praying for the day to come when I could stand in a shower. You know, I have to sit down like I’m sure you did at some stage as well.
Ruth 54:21
You know, to have a shower in one of those horrible shower chairs that are in every hospital. But I just I never thought the day would come that I would be able to stand up and shower at the same time. So I often think that in the shower, that I’m just grateful that I can do this. I genuinely never thought that day would come.
Bill 54:42
Adjusting the water and getting in and I know that one of your sides is thinking this feels amazing. This is the perfect temperature. The other side.
Ruth 54:50
Yeah, exactly. Yeah, it’s it’s weird because I would say right down the middle of the body. This sensation on the left is just complete dulled compared to the right. So yeah, I do find myself having to adjust, it’s perfect on the right and oww turn it down and turn it off on the left. So it’s a bit of a longer process, having a shower, really trying to balance out the temperature and all of that. But you get used to it.
Bill 55:20
Have you ever found yourself sweating on one side of the body and not the other? So I’ve done that where one side of my body is perspiring, usually, I think it was my left side was perspiring and my right side wasn’t. interesting.
Ruth 55:35
No, I never, I wasn’t aware of that. But I look out for that now. Like with my, feet, for example, my left foot, which is the affected side, like, I mean, it can be like a block of ice, compared to my right foot. And that could be roasting hot. So there’s temperature can be very different. And same with my arms, like at the minute, it’s quite cool to do in the room. And my left arm is freezing, whereas my right arm is normal, you know, but it’s different.
The hardest part of the journey for Ruth Carroll
Bill 56:06
That’s so strange. I’m just aware of coming up the time. And I want to ask you what the hardest part of your journey has been so far.
Ruth 56:18
I would say, Bobby, and missing those seven months and coming home to a seven-month-old baby. And just knowing when I was in hospital, that my newborn baby is at home and that I wasn’t at home with him. Even though like, you know, he was bought into me in my hospital bed for a few minutes. It wasn’t things so that was definitely the hardest. out of everything. I had to take paralysis and brain surgery over that.
Ruth 56:45
Wow, and did you seek out counseling and support for coming to terms with the types of issues that you had? Because that’s not what you expected? until, you know, you’re nine months into your pregnancy? Everything, you know, this is what’s going to happen when I give birth. And that’s what’s gonna happen when we come home. And this is how it’s all gonna go. And then that was all gone. Did you find you needed to get help to come to terms with that?
Ruth 57:17
In the I didn’t find I needed help. But I was advised to get help. When I was in the rehab hospital. They referred me to a company called headway. And it’s basically they I don’t know, what do you have them in Australia? I don’t know. Yeah, so they’re great. They basically offer all the different services for anyone with a brain injury in Ireland. So I was referred to them.
Ruth 57:42
And I did see and I still am seeing fabulous lady there. She’s a psychologist. So she’s great initially, three Irish thing. I was like, No, I’m grand, I don’t need to go talk to anyone. But I totally see the benefits of therapy now of sitting down and just talking about how I’m feeling.
Ruth 58:05
And as you said, there, you know, what I expected life would be like after having a baby versus the reality of what it is. So it’s beneficial. So I know, initially, I was kind of in there going, Oh, talk about how I’m feeling I hate this. But now I actually look forward to going in and just talking, you know, you come out feeling much lighter.
Ruth 58:27
And there’s also kind of a group session that we go to, in their cognitive behavioral therapy, I think it’s called. And that’s great. You’re sitting in a room with people, everyone in there has been through the exact same, you know, experiences as myself. So we literally just bounce ideas off each other. And that’s, I find that a lot more helpful and impactful, really than one on one. But it’s great to have that service here in Ireland.
Ruth 58:59
I was in counseling, I think, at day 10 or something like that. But I had a good, track record of being in counseling, I’m the kind of guy who I don’t do well with not resolving things in my mind. So not that everything needs to be resolved. But I need to at least turn the cogs of the discussion on and get another perspective and express my perspective in a way that it doesn’t get judged, etc.
Bill 59:32
And I would recommend to everybody who has thought about it to just do it and it’s not about going and solving a particular issue or problem. It’s just about going there. And then whatever it comes from it because you don’t ever really know what you’re going to get from it. Something just comes up and you realize, Oh, I didn’t think I was gonna talk about that or I didn’t understand that or to learn that.
Ruth 1:00:00
It helps with your awareness. I often find myself going Oh, yeah, I wasn’t aware of that. No, I didn’t see that. I didn’t understand that, but I do now. It’s great. It’s very therapeutic to me. But yeah, it’s something I would really recommend anyone to do as well.
Supporting stroke survivors

Ruth 1:00:19
Yeah, I also support stroke survivors through coaching. And some people, all they want to do is have their questions answered. So they, they’ll send me, you know, three, four or five questions. And all I’ll do is answer those questions, whether it’s me in a video chat scenario, whether it’s one on one or via zoom like we are now, or whether it’s just via a message through an app or whatever.
Bill 1:00:48
That ability for a stroke survivor to answer their questions rather than going and asking that question of a doctor really changes the game because they’re not asking me medical questions. I’m not responding to medical questions. I’m responding to personal experience questions related to exactly what their experience is.
Ruth 1:01:14
That’s what I was just thinking, I have two good friends who have had strokes as well, who I met during the stroke journey. And, you know, they’re the best I often was just sent a message God has this happened to you? And we kind of bitch with each other.
Ruth 1:01:29
That happened to me, how did you handle it? And that’s actually the best way to get advice I find. And you can be knowing that someone has experienced what you have experienced. And I find that very comforting. So I talk and I engage with those, those two friends of mine. Alas,
Bill 1:01:52
that sounds short talk. But it sounds like why you jumped at the chance to be on the podcast when I sent you a request?
Ruth 1:02:02
Absolutely, yeah. As I said earlier, it’s if you can help one person I often think of someone being in hospital upset, feeling afraid and alone. Like how amazing would it be for someone out to listen to you and I talking here? You know, it would have to give hope to the person. So I think it can’t be that.
Ruth 1:02:25
And it does. Ruth, I get messages every day. And it gets downloaded at least 3000 times a month, this podcast now. So it reaches a lot of people, a lot of people listen. And you would think that after 130 episodes that they will starting to sound the same. They’re not every episode is different, even though we’re talking about stroke all the time, because every human is different.
Bill 1:02:50
Every lesson that I’ve learned, has been learned in a different way, for different reasons. So I think, this is really an ideal way. And we’re blessed to have a technology that wasn’t available even 10 years ago, and five years ago, nobody really paid attention to it. And that’s when I started my podcast.
Bill 1:03:13
It’s been about five years. At the beginning of the episodes were few and far between because I was unwell. But in the last five years, there’s at least another three or four podcasts related to stroke that I’m aware of. And, some people have told me that they were like you are very early stages of stroke lying down on a hospital bed or even at home and googling stroke podcast, and then bang, they come up. And their prayers have been answered because all of a sudden, they start to feel like you and I feel which is okay, I’m not alone. And people understand me.
Ruth 1:03:54
Yeah, I wish I had found you in this podcast in the early days, I could totally see the benefit that would have been so it’s brilliant. fairplay to you for doing these podcasts. It’s great.
Ruth 1:04:05
Thank you for being a guest on the recovery after stroke podcast. I really appreciate it. I know you want to connect with people on Instagram so what is your Instagram handle? I’m gonna of course put it in the show notes for people to find easily but where would people find you?
Ruth 1:04:23
Yeah, so my Instagram account is Ruthie_Carroll84
Bill 1:04:31
Ruthie_Carroll84.
Ruth 1:04:35
Yeah, that’s exactly it.
Bill 1:04:38
All the best on an amazing ongoing recovery. Enjoy your family and give yourself heaps of time to get better. Thanks so much for being on the podcast.
Ruth 1:04:50
Thank you Bill.
Intro 1:04:54
Discover how to heal your brain after stroke go to recoveryafterstroke.com.
Intro 1:05:04
Importantly, we present many podcasts designed to give you an insight and understanding into the experiences of other individuals. opinions and treatment protocols discussed during any podcast are the individual’s own experience and we do not necessarily share the same opinion nor do we recommend any treatment protocol discussed.
Intro 1:05:21
All content on this website at any linked blog, podcast or video material controlled this website or content is created and produced for informational purposes only and is largely based on the personal experience of Bill Gasiamis, the content is intended to complement your medical treatment and support healing. It is not intended to be a substitute for professional medical advice and should not be relied on as health advice.
Intro 1:05:44
The information is general and may not be suitable for your personal injuries, circumstances or health objectives. Do not use our content as a standalone resource to diagnose, treat, cure or prevent any disease for therapeutic purposes or is a substitute for the advice of a health professional.
Intro 1:05:59
Never delay seeking advice or disregard the advice of a medical professional your doctor or your rehabilitation program based on our content if you have any questions or concerns about your health or medical condition, please seek guidance from a doctor or other medical professional if you are experiencing a health emergency or think you might be called triple zero if in Australia or your local emergency number immediately for emergency assistance.
Intro 1:06:20
Or go to the nearest hospital emergency department. Medical information changes constantly. While we aim to provide current quality information and our content we did not provide any guarantees and assume no legal liability or responsibility for the accuracy, currency or completeness of the content.
Intro 1:06:36
If you choose to rely on any information within our content, you do so solely at your own risk. We are careful with links we provide however third party links from our website or follow that your own risk and we are not responsible for any information you find there.







