Shannon Nelson is a young stroke survivor who has achieved great results in overcoming aphasia and other deficits caused by stroke.
Highlights:
01:50 Introduction
05:19 Patent Foramen Ovale (PFO)
08:24 Initial Stroke Deficits
14:04 Dealing With Apraxia
25:49 Living With Aphasia
31:07 Asking The Right Questions
39:52 Therapy After A Stroke
46:21 Aphasia And Alcohol
54:51 Recovery During Pandemic
1:00:22 A Night For Aphasia
Transcription:
Bill Gasiamis 0:00
Is your aphasia is it worse at some times of the day? Is it better at some times of the day? When is the best time for it?
Shannon Nelson 0:08
At the end of the day, particularly if I’ve worked and when I’m tired when I’m stressed, when I’m excited. So yeah, so anytime, but particularly at the end of the day, so I worked three days a week now. And I work three days in a row by Thursday, my Aphasia really plays up.
Intro 0:54
this is the recovery after stroke podcast. With Bill Gasiamis, helping you navigate recovery after stroke.
Bill Gasiamis 1:06
Hello, and welcome to episode 205 of the recovery after stroke podcast. Thanks to everybody who’s reached out so far, and asked to be a guest on the show I really appreciate it just makes my life a little bit easier when people reach out and offer to be on the show. And actually, it’s a really good experience that people do come on the show share their story makes a massive difference to them and their recovery.
Bill Gasiamis 1:31
And maybe to be able to share your story, it will be a good thing for you too. So if you are a stroke survivor with a story to share about your experience with stroke, and you’ve been thinking about reaching out to be a guest on the show, but we’re waiting for the right time to reach out. Or for the right sign this is it.
Introduction – Shannon Nelson

Bill Gasiamis 1:50
If you go to recovery after stroke.com/contact, you will find a form that you can fill out to apply to be a guest on the show. As soon as I receive the form. I will respond with more details on how you can choose a time that works for you and me to meet over zoom. Now my guest today is Shannon Nelson, an ischemic stroke survivor who at 45 is living with aphasia. Shannon Nelson, welcome to the podcast.
Shannon Nelson 2:21
Thank you for having me today.
Bill Gasiamis 2:24
Thank you so much for joining me. Tell me a little bit about what happened to you.
Shannon Nelson 2:28
So I went to bed as normal on a Sunday night. It was Mother’s Day 2018. And I was fine. And then I woke up at three o’clock in the morning to go to the toilet. And I was fine then. And then I woke up again at 5:30 and I was thrashing around in bed and then I fell out of bed.
Shannon Nelson 3:02
And my husband Stuart tried to rush around the bed and try to pick me up and he couldn’t. And he recognized my stroke straightaway. So I had the facial droop, couldn’t lift my arms, and I couldn’t speak. And I remember him saying to 000 operator.
Shannon Nelson 3:29
I think my wife is having a stroke. So the ambulance officers arrived about 10 minutes later. And they agreed with him. And then they because I was between the bed and the window. They struck me into a proper mat and drag me down the hallway of a house.
Shannon Nelson 3:58
And then I saw Gemma, my daughter holding the dog in the doorway of her room. And I began to cry and I said to myself, I might not get through this. So I arrived at Box Hill, approximately 6am And I was diagnosed I was met by the stroke team.
Shannon Nelson 4:30
And I was diagnosed with the left middle cerebral artery stroke. It was a clot. So I had the clot busting therapy at 6:20 and then I was transferred to Royal Melbourne Hospital for clot retrieval. And the clot was retrieved at 7:35am so lucky Stewart heard me get up to the toilet because I was weak in the four and a half hours of the clot busting therapy.
Bill Gasiamis 5:10
Yeah, pretty dramatic. Do they know what the cause of the stroke was of the clot?
Patent Foramen Ovale (PFO)
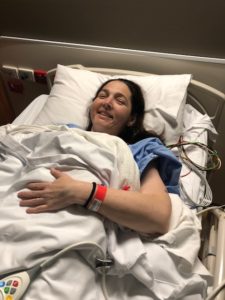
Shannon Nelson 5:19
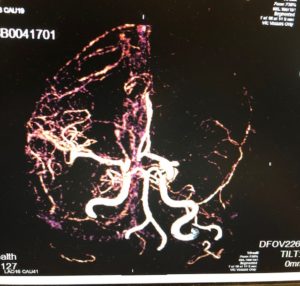
I think later, I had an echocardiogram at Royal, Melbourne at Box Hill. And they found a hole in my heart.
Bill Gasiamis 5:37
Did you have any indication? Did you know at all about the hole in your heart? Did you have any symptoms around that? And stroke was the first symptom that you had that you became aware of the PFO?
Shannon Nelson 5:52
Yeah.
Bill Gasiamis 5:52
Yeah. So you’ve gone to Box Hill Hospital initially. And then did you end up at the Royal Melbourne Hospital? Did they transfer you for some reason?
Shannon Nelson 6:08
So Box Hill doesn’t do clot retrievals. So they transferred me to Royal Melbourne to do the clot retrieval.
Bill Gasiamis 6:21
And a 45 would you have considered yourself pretty healthy otherwise?
Shannon Nelson 6:28
Well, yeah, I had weight loss surgery two and a half years beforehand. So I was under 70 kilos so I was walking most days.
Bill Gasiamis 6:55
So it sounds like you were on a journey a little bit earlier to become healthier. And do you think that that journey that you went on helped you in your recovery?
Shannon Nelson 7:06
Absolutely. I’ve said all along if I didn’t have the weight loss surgery, I would have been dead, or I would have been in a nursing home. Because I was fit.
Bill Gasiamis 7:23
Yeah. So it helped you. So what’s it like, leaving your house going to hospital? Were you aware of your surroundings? And what was happening? Or did you go there in a different state?
Shannon Nelson 7:38
No, I was aware. Yeah. I was fluctuating in and out of consciences. But I was aware.
Bill Gasiamis 7:52
So when you woke up from hospital the first time, did you have an idea that you had a stroke? Were you aware of all of it?
Shannon Nelson 8:08
When my husband said to this 000 operator, I think my wife is then having a stroke. It dawned on me that I was having a strike.
Shannon Nelson Initial Stroke Deficits
Bill Gasiamis 8:24
When you woke up, what were you left with? What kind of deficits did you have to deal with?
Shannon Nelson 8:28
I couldn’t speak and paralyzed in my right side, I was walking in the next day. And I was raising my hand by day three, but I have no usable function in my right hand.
Bill Gasiamis 8:57
Yeah. How long has it been? How many years?
Shannon Nelson 9:02
Four years?
Bill Gasiamis 9:03
And where’s your right hand now? Are you able to use the right hand?
Shannon Nelson 9:07
Oh, yeah, I’m using the right hand I taught at work. I use writing. Six or seven months after my stroke, I write 35 Christmas cards with my right hand. I was determined to get my right hand function back.
Bill Gasiamis 9:30
Do the writing looked terrible or was it decent?
Shannon Nelson 9:32
It was really decent, actually.
Bill Gasiamis 9:38
That’s good. So people on the other end knew that it was a letter from Shannon, and they knew what you were saying.
Shannon Nelson 9:46
And I wrote on each Christmas card I’m writing this with my right hand.
Bill Gasiamis 9:57
Wow. So that was a big deal it sounds like it was a really big deal for you to write those Christmas cards out?
Shannon Nelson 10:04
Yeah. And I address them all with my right hand as well.
Bill Gasiamis 10:11
So, is that something that you were looking forward to? Did that just come up out of nowhere you decided that that’s what you’re going to do and give it a try? Or were you really impacted by the thought and the knowledge that your right hand side wasn’t working, as it did prior to the stroke?
Shannon Nelson 10:31
So I used to practice with my left hand writing before my stroke, so I was able to write with my left hand, so the handy thing they gave me was a whiteboard in the hospital on the first day, and I was able to use my left hand, so I was finally able to communicate with my family and the doctors.
Shannon Nelson 11:05
But I did weekend, Friday and Saturday call it, my aphasia is coming right now. It was sort of like a two tiered course therapy course. So the object it was run by an OT and a physio. And it got me back into handwriting.
Bill Gasiamis 11:58
Okay. So why would somebody practice writing with their left hand? Even though they don’t need to before the stroke? What was going on in your mind there? Just something for fun?
Shannon Nelson 12:15
I don’t know.
Bill Gasiamis 12:21
You’re strange like that. Yeah okay, fair enough. I mean, it’s kind of cool to be able to write with both hands. I get it. I’ve never met anyone that said, I’m just gonna start writing with my left hand one day, just because they felt like it well, their opposite hand.
Shannon Nelson 12:34
Yeah, well, I don’t know. I needed it some time down the track, which I did.
Bill Gasiamis 12:46
It sounds like you were pre empting something and you’re planning ahead?
Shannon Nelson 12:52
Yeah.
Bill Gasiamis 12:54
That worked out good on you. Well done. So clearly, you lost your ability to speak and then.
Intro 13:01
If you’ve had a stroke, and you’re in recovery, you’ll know what a scary and confusing time it can be, you’re likely to have a lot of questions going through your mind. Like, how long will it take to recover? Will I actually recover? What things should I avoid in case I make matters worse? Doctors will explain things that obviously, you’ve never had a stroke before, you probably don’t know what questions to ask.
Intro 13:26
If this is you, you may be missing out on doing things that could help speed up your recovery. If you’re finding yourself in that situation. Stop worrying, and head to recoveryafterstroke.com where you can download a guide that will help you it’s called seven questions to ask your doctor about your stroke.
Intro 13:45
These seven questions are the ones Bill wished he’d asked when he was recovering from a stroke. They’ll not only help you better understand your condition. They’ll help you take a more active role in your recovery. Add to the website now, recoveryafterstroke.com and download the guide. It’s free.
Dealing With Apraxia
Bill Gasiamis 14:04
Was that ability to speak lost because of issues with your vocal cords. I know some people who suffer loss of speech as an issue with the vocal cords the strength and the deficits there, or was yours cognitive totally aphasia.
Shannon Nelson 14:21
Apraxia. So Apraxia is defined as having difficulty planning and using the muscles during speech. So I knew what I wanted to say. But I couldn’t get the words out. So I slipped out the F word in frustration at my husband the day before I actually spoke deliberately. So the first words I said was 12345. And the speech therapists I mirrored the speech therapists. So I knew what to say, but I just couldn’t get the words out.
Bill Gasiamis 15:21
Which was the F word again. Can you repeat the F word for me?
Shannon Nelson 15:26
No. F U C K.
Bill Gasiamis 15:33
You got that out? Was that the first word you said? How rude.
Shannon Nelson 15:38
The day before I actually spoke. So yeah, I couldn’t repeat it.
Bill Gasiamis 15:48
You couldn’t repeat it because you didn’t want to?
Shannon Nelson 15:50
Because it was an automatic F***. So I was so frustrated with my husband, because he was trying to finish my sentences.
Bill Gasiamis 15:50
One of my pet hates is when people try and finish a sentence. I know that sometimes with people with aphasia, when they can’t come up with the word, there’s this real urge to finish the person sentence or to give them information that might help them get there. So is it helpful sometimes when people do that? Or is it always better to just let the person go through that process?
Shannon Nelson 16:38
I don’t mind because my family and friends have been patient with me and let me speak. But in the workplace, I just let it go.
Bill Gasiamis 16:58
I get really frustrated when you see adults answering for children. And so I love hanging out with young kids when we get together with families that have got young kids and all that and I’ll go up to them or start a conversation. And then the parents will chime in and they’ll come in and they’ll speak on behalf of the child as if I asked the parent that question.
Bill Gasiamis 17:25
It drives me absolutely insane. I don’t know if it’s my place to say no, I don’t want you to answer the question for your child, I want your child to answer the question, in case they get offended or something like that. I don’t know how to handle it. But I just can’t understand why it’s necessary for the adult to get involved in that conversation. Especially when the conversation is not with them.
Shannon Nelson 17:53
Yeah, I don’t know the answer to that. But yeah, I just in the workplace. I don’t pull them up. But in the community, I say to people, bear with me I’ve got aphasia, I’ve had a stroke, just bear with me I’ll get the words out eventually.
Bill Gasiamis 18:22
At home. After four years, are you still reminding everyone to hang on a sec? Just wait, wait, wait.
Shannon Nelson 18:30
Yeah, well, I say (inaudible) a lot. Because my aphasia is between verbs and nouns, and I say (inaudible) a lot. And my son Shawn, who slept through the whole ordeal, he often reminds me, Mom, I don’t speak strokes. And, yeah, I say to my husband now and then just let me get the words out. So they learned.
Bill Gasiamis 19:19
Yeah. It’s a difficult adjustment for them. I imagined, because they don’t understand stroke. They definitely don’t understand apraxia. They definitely don’t understand aphasia. And they are just going back into the normal mode of the same pace that they always spoke to you at. And the same way you always spoke back.
Bill Gasiamis 19:42
So it’s a real challenge for them to adjust even though it’s been four years, compared to how long they’ve both known you for. It’s only a short amount of time. And often they’re not speaking to people with aphasia, most of the rest of society doesn’t have aphasia. So having to adjust backwards and forwards.
Shannon Nelson 20:08
Yeah. And I think we’re adjusted to a new kind of normal. But I think my children see me in the same way as before my stroke, so they don’t treat me any differently now. We joke, and we’ve laugh so yeah.
Bill Gasiamis 20:40
Does aphasia interfere with writing? So I’m completely oblivious. I don’t know about aphasia. So when you’re trying to speak words don’t come out, you know what you want to say. But when you’re writing them, do they get stuck in the same way?
Shannon Nelson 20:55
No, so aphasia is a language disorder that affects reading writing numbers, and it can be in speech, it can be a combination of the two, but my aphasia is speaking, but my numbers are fine. And that sort of thing. In saying that, I can’t add it up in my head anymore. I used to be really good at math, but I have to write. Whit simple math, I have to write the numbers down now. But my reading wasn’t affected. And my comprehension wasn’t affected as well.
Bill Gasiamis 22:02
So your numbers, when you’re writing them down, they add up correctly, and then your brain doesn’t know that the numbers are correct?
Shannon Nelson 22:10
Yeah.
Bill Gasiamis 22:12
But doing it in your head, you don’t know how to get to the correct number?
Shannon Nelson 22:16
I can do simple. So eight plus five equals 13. But when I get larger numbers, or subtracting, I have to write them down.
Bill Gasiamis 22:35
Okay, so you write them down, you look at that, you know, it’s the correct answer. Because, you know, numbers and basic numbers and math. But when you’re doing, say 27 plus 37.
Shannon Nelson 22:51
I have to write them down.
Bill Gasiamis 22:53
Right to do that in your head, you can’t get to the answer.
Shannon Nelson 22:59
Well, I could. So 27 plus 37 is 64. But I used to do it a lot quicker.
Bill Gasiamis 23:14
Faster than I would have done it.
Shannon Nelson 23:18
Well, yeah.
Bill Gasiamis 23:20
Okay. So there are some numbers just because they’re harder to get to or takes longer to get to. You just prefer to write them down. And then that way, does writing that down also give you any memory issues there? Does it also then give you the memory on the paper?
Shannon Nelson 23:41
No, not really. So yeah, I don’t have any memory issues so I write everything down or I put a reminder in my phone all that sort of thing, but my long term memory wasn’t affected at all.
Bill Gasiamis 24:09
How about people that don’t understand about stroke or don’t know you’ve had a stroke don’t know about your aphasia, and then they come to you to talk to you. Do you often come across people who slow their speech down or think that you’re intellectually impacted by the stroke?
Shannon Nelson 24:31
No. So I’ve worked really hard to get my speech back. So in the beginning, I felt that people thought I was stupid. But now they can’t now. Yeah. And so I did on strike stake ambassador for the strike Foundation, and I was doing a talk last month for a retirement village. And a doctor came up afterwards and he walked in light, because I knew you had a stroke. I could tell. But other lay people can’t. Yeah.
Living With Aphasia
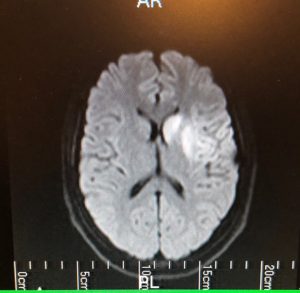
Bill Gasiamis 25:49
Is your aphasia is it worse at some times of the day is better at some times of the day? When is the best time for it?
Shannon Nelson 26:00
At the at the end of the day, particularly if I’ve worked. And when I’m tired, when I’m stressed, when I’m excited, so anytime, but particularly at the end of the day, so I work three days a week now. And, but I work three days in a row by Thursday my aphasia really plays up.
Bill Gasiamis 26:51
Okay, so it even gets worse as the week gets on. Okay, so Monday is your best day, and then by Thursday, we’ll call it at its worst, but it’s when it’s more prevalent?
Shannon Nelson 27:08
Yeah, exactly. But word finding is particularly difficult on Thursday nights. And so it’s fine on Friday, because I’ve had a rest but, particularly on Thursday nights. It’s really bad.
Bill Gasiamis 27:29
Yeah, I’m smiling. But I’m the reason why I’m smiling. Because I relate to that. I don’t have aphasia, or any of those challenges with my speech, although my wife sometimes think I do. And sometimes I do kind of like… and then I kept going again, you know, like, I pause, and then I get going again.
Bill Gasiamis 27:54
And for me, it’s not difficulty finding the words, but it’s just, there has to be like, I have to rest for a little bit in between the previous word. And this word, I don’t know if that’s the best way to describe it. But I know with my other deficits, I’m really good in the morning. And then by middle of the afternoon, or by the end of the day, the deficits are starting to play up.
Bill Gasiamis 28:20
If I’ve missed out on sleep the night before, I’ve had a couple of days of you know, light sleep or not enough sleep, then my deficits on that next third day are really playing up the most. And I noticed that the most, nobody sees them. Still people still don’t see my deficits, but I really feel them.
Bill Gasiamis 28:43
And that’s when they’re on my mind the most. So sometimes, I don’t think about my deficits at all. But sometimes, it’s like, wow, the legs really feeling weird today, or my arms are feeling really weird. Do you have days where the aphasia is on your mind? And you’re overthinking it, or it’s bothering you, and then some days when you don’t?
Shannon Nelson 29:10
Yeah particularly if I haven’t slept the night before, like you and then just I’ll go to work or get up. But I don’t talk much that day.
Bill Gasiamis 29:29
And is that a conscious effort to rest you’re talking part of your brain?
Shannon Nelson 29:36
Yeah, exactly.
Bill Gasiamis 29:40
That’s a pretty good strategy, though, isn’t it because you’re becoming aware of what you need to do to give your brain a rest to give say, the connections or the pathways to your mouth and your brain a rest from being overexerted?
Shannon Nelson 29:58
Yeah, exactly.
Bill Gasiamis 30:02
I like that. And then how do people around you comprehend that? Do they go why isn’t she talking today? Is she sad? Is there something wrong? What do they do?
Shannon Nelson 30:16
Yeah, I had a day like that this week. And they were concerned. And I said, I’m fine. And they said, Oh, will you tell me if something’s wrong? And I said, No, actually, but yeah, I was just tired. And I just couldn’t speak.
Bill Gasiamis 30:44
And would you say it like that? I’m tired. And I can’t speak at the moment.
Shannon Nelson 30:49
Not really. So I didn’t. But yeah, I just said, I’m fine. They said, what’s wrong? And I said, nothing. I’m fine, but yeah, I just got tired.
Asking The Right Questions – Shannon Nelson

Bill Gasiamis 31:07
I know that experience. I think the problem is the question that people ask, because then we default to that standard answer. What’s wrong? Nothing. Because nothing is wrong. Are you okay? Yeah, I’m fine.
Shannon Nelson 31:23
I’ve had a stroke. That’s all that’s wrong with me today.
Bill Gasiamis 31:29
Yeah. Whereas if they asked a better question, like, are you having a tired day today? Or are you having a rest day today? Or whatever the question is, that would allow you to have a better conversation with them about what’s going on?
Shannon Nelson 31:44
Yeah. Exactly.
Bill Gasiamis 31:48
I like that. I like the difference in that part of the question and the answer in the response. It’s, they’re going to, you know, she’s somebody who’s had a stroke, they are remembering that you’ve had a stroke, or they are seeing you behave differently. And they are going, Oh, my God, is it another stroke, what’s happening with her?
Shannon Nelson 32:12
Well, so I went back to work four months, and three weeks after my stroke, I had a graded re-entry to work. And I’d started out five hours a day, three days a week. So I was in nursing allocations at the time. So I was back at work full time, after 10 months. And then I was in an allocation shifts, two days in a row.
Shannon Nelson 32:46
So I work there, Tuesday morning, and then the Wednesday morning. So it’s a lot of speaking on the phone, doing allocations. So you’re ringing up people, to agencies, and bank staff and call staff to tell them their wards or put out bookings. And then buy the next morning, I’ve worked Monday take in my normal job allocations on the Tuesday starting at 5:30.
Shannon Nelson 33:27
And allocations on the Wednesday, starting at 5:30. And by 10am, on the Wednesday morning, I was slurring my words. So I took a phone call from a nurse unit manager. And she said, are you okay? Because I was slurring my words, obviously. And I said, yeah just really fatigued. And she goes, what’s wrong? And I said, you know, I had a stroke 10 months ago, or a year ago, it was 10 months. And she said, No, I thought you were having another one. She was going to ring triple zero.
Bill Gasiamis 34:29
Yeah, and that’s a lovely thought.
Shannon Nelson 34:30
Because I was slurring my words that much.
Bill Gasiamis 34:33
Yeah, that’s a lovely thought, because at least she knows the signs. And she’s checking in with you. And she’s getting a response. And then thankfully, you were able to say, oh, that you were tired. And that would have made her feel better about your situation. It sounds like Shannon maybe what’s a great idea would be is to have like a sign that you put on your computer monitor at work saying today I’m resting my brain or my voice or I’m tired or I haven’t slept for three days just so then you can give people a bit of feedback or updates.
Shannon Nelson 35:13
Yeah, I’ll take that on board.
Bill Gasiamis 35:17
Yeah. And it’s an anxiety that people also have I often talk about with stroke survivors, that their anxiety about having another stroke. But then your colleagues and your loved ones are also potentially having anxiety over the fact that you might be experiencing another one.
Shannon Nelson 35:36
Yeah, but I have the PFO closed before I went back to work. So before I had the PFO closed, I was anxious about having another stroke because I think a clot broke off, traveled across the hole in my heart and quicked up to my brain.
Bill Gasiamis 36:11
After the PFO was closed, how did you notice a difference in your body, in yourself, in your heart, in any way? Did you know like before and after version of you?
Shannon Nelson 36:25
No, I had no idea I had the hole in my heart. And I had surgeries before I had , three surgeries prior I gave birth to two children. And they didn’t pick it up.
Bill Gasiamis 36:50
Yeah, maybe they’re not looking for it. And therefore it doesn’t really come up if you’re not looking for it or something like that.
Shannon Nelson 36:56
The surgeon, the cardiologist who closed my hole in the heart said it’s not the biggest hole I’ve plugged.
Bill Gasiamis 37:12
One of those things. How old was your son at the time?
Shannon Nelson 37:18
17 and my daughter was 16. Shawn was doing BCA at the time.
Bill Gasiamis 37:30
Was he doing the last year of school or?
Shannon Nelson 37:32
Yeah, last year.
Bill Gasiamis 37:35
And your daughter would have been in year 10? Again, yeah, yeah. Okay. How did they cope with it? Or how did they deal with knowing the man was unwell and heading to hospital, etc.
Shannon Nelson 37:49
So Gemma woke up Shawn at seven o’clock. And she’d heard from Stuart, that I’d had a stroke. So Gemma, she woke up Shawn at seven o’clock. And she told Shawn that mums had a stroke. And they went off to school, like normal.
Bill Gasiamis 38:31
Is that because they had no idea what a stroke was?
Shannon Nelson 38:34
Stuart told them to go off to school and act as though it was a normal day.
Bill Gasiamis 38:43
Is that a good move? Did he do the right thing? Or was he in trouble for that?
Shannon Nelson 38:47
I think so.
Bill Gasiamis 38:48
Okay, good. I think that’s the best move.
Shannon Nelson 38:51
Yeah, and they went to school all through my recovery. And so Shawn went to work. Gemma went to work. So they just behaved as though was normal.
Bill Gasiamis 39:16
Okay. Yeah. I like the idea of that because therefore that means that they are going about life as normal. They are probably still concerned, but they’re not being anxious that haven’t got a lot of time to overthink things. And they just dealing with what’s coming as necessary, rather than trying to solve all the problems that might come up going forward that may never come up right?
Therapy After A Stroke
Shannon Nelson 39:52
So I got a mental health plan from my GP About two months afterwards.
Bill Gasiamis 40:03
That’s like seeing a psychologist, right?
Shannon Nelson 40:05
Yeah. So I felt I wasn’t coping cuz I couldn’t say the word monotony I never used it anyway.
Bill Gasiamis 40:19
Say it again?
Shannon Nelson 40:22
Monotony and can’t say it anymore, so I had a meltdown. And so I threw books and that sort of thing cried. And then I went off to get a mental health plan from my GP. So I had three visits by myself, one with Stuart and one family therapy session. And that was, I think that was good.
Bill Gasiamis 41:10
I did something similar after my first episode with a brain hemorrhage I went, I think it was maybe in less than 10 days after I was in hospital. Because the first time I was in for a week, and then released, I was in therapy with my wife. And then after that, I think I went a few times with my kids, etc.
Bill Gasiamis 41:32
But I’ve been going to therapy for since I was 25. Anyway, so it’s not, it wasn’t anything new to me, but it was something that I just did. What about you, though? Was that enough? Therapy? mental health therapy sessions? Do you feel like more would have been better? What were you with that?
Shannon Nelson 41:55
So I joined a sleep and fatigue study in 2019. And I got near a psych therapy through the sleep and fatigue sub. And I continue to see my neuro psych after that. And then I also see the neuro psych once a month or once every six week through NDIS, I have been seeing neuropsych.
Bill Gasiamis 42:40
Yeah, so it sounds like he did put a fair bit of work into making sure that certain things were okay that you were managing and you’re coping with everything. Why did the word monotony? Why was that the word that was the one that sent you over the edge?
Shannon Nelson 43:05
It was. So I was doing word lists. And that’s the word that I struggled with. And that’s the straw that breaks the camel’s back as they say.
Bill Gasiamis 43:25
Everyone has their limits. And yours was monotony.
Shannon Nelson 43:31
Or is it a monotonous task I was doing at the time.
Bill Gasiamis 43:44
Understand. What’s something that has been placed on hold because of your stroke? Or was placed on hold that you’re doing now? Was it interfering with stuff that you were in the middle of doing that it stopped you from doing?
Shannon Nelson 44:06
No, not really. I’ve been overseas since my stroke. So I was an avid walker before my stroke, so five months after my stroke, I walked the five K’s in the Melbourne Marathon with my family and raise money for the Stroke Foundation. And then we decided to do the Melbourne Marathon in 2019 as well. So 10 weeks before I signed up for the 10K, and 10 weeks beforehand.
Shannon Nelson 45:10
I wasn’t a runner before my strok. And I ran the 10K in the Melbourne Marathon with my family. Shawn and Gemma, my children walked and Stuart my husband ran. And then I decided because of COVID I decided that I was going to do the toughest half marathon in 2020 by COVID heat. So, hopefully I’ll do like, this year, I’ll walk and run in Tasmania the Point of Pinnacle. So yeah, that’s the only thing but that’s because of COVID.
Bill Gasiamis 46:12
Is the stroke anniversary? Is it something that you celebrate? Or is it something that you prefer not to mark?
Aphasia And Alcohol – Shannon Nelson
Shannon Nelson 46:21
The first year I celebrated I didn’t drink for a year to allow my brain to heal. So I celebrated with my friends and my family. And I bought a bottle of Cristal champagne and drank that all day.
Shannon Nelson 46:23
That make the aphasia better or worse?
Shannon Nelson 46:51
Ah I think better actually. Drinking helps with aphasia.
Bill Gasiamis 47:06
It helps you with your aphasia is that because you’re not overthinking it or something?
Shannon Nelson 47:13
Yes exactly.
Bill Gasiamis 47:16
So drinking helps me play pool. You know, the billiards or pool. Because when I’m sober, and I haven’t played for many, many years, but when I’m sober and not playing and playing pool. I’m overthinking where I should put the stick. And where I should hit the ball and how much power I should use. So I’m thinking about that process.
Bill Gasiamis 47:41
And then when I’ve had a couple of drinks, I don’t think about it. I just do it on instinct, or more on knowing what I know about pool because I’ve played it for so many years. Never as a professional just with my friends in that. So I’m far better after a few drinks than I am when I have to be completely totally unaffected by alcohol.
Shannon Nelson 48:09
I’m better after two champagnes, but when it gets to 4, no good. I’m slurring my words. I drink it all day.
Bill Gasiamis 48:27
I wonder if anyone else out there who’s had aphasia or has aphasia gets better after they have a couple of drinks. If anyone’s listening and you have experienced something similar, just leave a comment in the comment section wherever you hear this podcast or watch this podcast let me know on Instagram. Anyway your life let me know. What’s something that stroke has taught you has taught you about life about yourself. What has it taught you?
Shannon Nelson 48:57
I don’t sweat the small stuff anymore. So yeah, I’m more relaxed. It’s taught me to be patient with me, and also my family and friends. And I don’t sweat the small stuff anymore. So I go into Shawn’s room, which is at absolute peak sigh. Just my mother visits Shawn when she comes down so they live in rural New South Wales. And my mother said to Shawn, clean up your room. He’s healthy, he’s not doing any harm by I just shut the door.
Shannon Nelson 49:46
You shut the door knowing what’s behind there. Yeah. And now you can just walk past it. And you don’t have to open the door.
Shannon Nelson 50:15
Yeah, exactly.
Bill Gasiamis 50:18
Yeah. Okay, I can relate to that.
Shannon Nelson 50:21
Yeah, I value my family and friends more.
Bill Gasiamis 50:31
Yeah, I can relate to that whole, shut the door and not look into the room. But sometimes when I have to go into the room to speak to my son, then my eyes they go to where all the rubbish in the junk and the clothes are. And I’m trying not to say anything about it. I’m really, really trying not to say anything about it, and have a conversation with them about why I walked in the room. But sometimes I can’t resist. After the conversation, I have to say something like, clean your room, clean your room. And then I’ll walk out.
Shannon Nelson 51:08
I say, every month or so, please clean your room, please just vacuum. And then he puts the washing out. So he’s 22 now.
Bill Gasiamis 51:26
Yeah, I think as long as you and he have the mum and son relationship inside your home, it’s really hard to shift the the dynamics of that I noticed that with my oldest son who moved out about a year ago, about a year ago. Now conversation when he’s at home. And living in the house was the usual conversation that we had for all the 25 years that he was at home.
Bill Gasiamis 52:00
And now that he’s moved out, the conversation has changed, it is different. And the dynamic has changed. So there’s no more me being the dad, asking him to do things in the house that he should be doing in his own place. He handles all of that stuff he does anyway. And I don’t need to go into his house and say Your house is a pigsty, for example, any of that stuff.
Bill Gasiamis 52:31
He’s an adult, and he acts like an adult because he isn’t in that environment where there is somebody who is kind of in the hierarchy of the home is above him in the hierarchy. Whereas now we’re equals because he’s a homemaker, and I’m a homemaker and now we’re equal.
Bill Gasiamis 52:57
And I think that’s what I learned. I appreciate that you would look forward to that. That’s what I discovered when he moved out, which was a really, because even though he was 25 I didn’t want him to move out. Right? Yeah, I wanted him to stay at home forever. But the the part of me that wanted to kick him out was glad that he left. And now that’s what I’ve learned from it.
Bill Gasiamis 53:24
I’ve learned that the dynamic has shifted. And our relationship has taken a different level and we don’t interact like although he’s my son and we don’t interact like father son in the hierarchy. We act like Father Son equals it’s a good experience. And your daughter what about your daughter? What is she like? Is she very different to Shawn?
Shannon Nelson 53:53
Yes. So Sean’s more laid back. Gemma. Gemma’s, Gemma. So she is finding her way I’d say. So she’s 20 now. So yeah, she got into uni last year, but she dropped out. After seven weeks. It wasn’t for her because she did online learning in for the last year of her schooling, and it was all online learning at the start of last year. So she’s working.
Recovery During Pandemic

Bill Gasiamis 54:51
Was COVID a difficult time to do stroke recovery in? Because for the first two years you were doing stroke recovery. Normally, and then COVID, shut everything down, did you miss out on accessing services and the things you needed?
Shannon Nelson 55:07
So I didn’t have traditional therapy for 18 months. So when I went back to work I, so I was in community rehab. So I did so. So I was in hospital for three and a half weeks and then discharge to ESD, early supported discharge program for stroke patient, which ran for four weeks. So I was doing OT and speech one hour a day, Monday to Friday for four weeks.
Shannon Nelson 55:54
And then I think the doctor and the nurse, both center and home based, then I was transferred to community rehab. And I did two sessions of speech a week, one telehealth and one sentence base. And then I do an OT session a week and group a week so once a week. So I was discharged from speech just after I returned to work. And then I was discharged from OT at the end of the year. So I worked on my own speech therapy and OT by myself, and then my OT at the community rehab encouraged me to apply for the NDIS.
Bill Gasiamis 57:22
And so did you do any zoom therapy?
Shannon Nelson 57:26
So yeah. So at the beginning, I was denied, so I didn’t have any traditional therapy in 2019. And then I was accepted in to the NDIS.
Bill Gasiamis 57:26
That’s the National Disability Insurance Scheme, right?
Shannon Nelson 57:51
Yeah. And then I had one session in person and then lockdown hit.
Bill Gasiamis 58:06
Locked down. Did that move to online?
Shannon Nelson 58:09
So I did one zoom session. Oh, one zoom session, a fortnight speech. And mind your site went on to ZOOM. But my OT because I use machines for my OT I had clinic sessions once a week.
Bill Gasiamis 58:37
Did you enjoy the online version of therapy compared to the regular version?
Shannon Nelson 58:44
Well, no difference. Yeah. Yeah.
Bill Gasiamis 58:50
Yeah. I know. My son was also finishing had also finished school just before locked down in 2019. So then his spent, but he finished in 2018. He took a year off and then his spent 2019 Just chilling out and doing the work. And then he really didn’t enjoy trying to do anything for the two years that we were in lockdown in Melbourne, and get some stuff going.
Bill Gasiamis 59:27
So he’s kind of he seems like he’s a little bit been impacted or delayed by the lock downs in the things that he wanted to do. And I know for other children that were still at school, they really didn’t enjoy the online version of schooling and I know a lot of stroke survivors didn’t enjoy the online version of their therapy and felt like they missed out on a lot.
Shannon Nelson 59:54
I think because I had done my stroke in 2018. And then I went without therapy for 12 months. I was just so thankful to get therapy again.
A Night For Aphasia
Bill Gasiamis 1:00:22
It’s been an interesting journey. I met you at the Night For Aphasia. That was being held in Melbourne quite some few weeks ago now. And facia is an annual event run by another guest that has been on this podcast. Olivia O’Hare. Yeah, yeah. And that was a really cool event. She’s a speech therapist, and she has an organization that helps people from all backgrounds with this speech.
Bill Gasiamis 1:00:57
You spoken presented at that event. That was pretty cool you did really well, in front of a group of people speaking about the challenges, and it was late at night. And you were drinking a couple of champagnes. But you got through it really? Well. And you’re going, you’ve sort of taken the this thing, and you’re turning it into a bit of a passion project where you want to raise awareness about aphasia, and all those things,
Shannon Nelson 1:01:36
About strokes. So it can happen to anyone, every anytime, anywhere, any age. I’m a nurse, so and I only treated elderly people who had a stroke. So I’ve worked in the rehab settings. So I didn’t know that strokes can, well I did, but I wasn’t aware of how many strokes happened to young people 25% of working age, people have strokes. So yeah. I wasn’t aware.
Bill Gasiamis 1:02:27
So you were a nurse. And you had been in situations where you were helping people that had experienced stroke, etc. Wow. Okay. So when you went back to work, did you go back to work as a nurse?
Shannon Nelson 1:02:41
No, I was working in nursing administration. So then I left my job last year, and then I work in an OT practice three days a week now and I do one clinical nursing shift a fortnight now for an agency.
Bill Gasiamis 1:03:14
So you work in occupational therapy practice now in what capacity?
Shannon Nelson 1:03:20
Admin.
Bill Gasiamis 1:03:21
Yeah, fantastic. If anyone’s going to understand what you’re going through, or the challenges that you face, it’s going to be an occupational therapy organization.
Shannon Nelson 1:03:35
I went there as a patient. And then I continue to do therapy once a week there.
Bill Gasiamis 1:03:54
And then you decided to work there as well.
Shannon Nelson 1:03:57
Yeah. Well, they offered me a job.
Bill Gasiamis 1:04:02
Fantastic. I love that. Well, I really appreciate all the things that you’re doing to raise awareness. Thank you so much for being on the podcast, and well done on all the stuff that you’re doing to raise awareness about stroke and aphasia, and thank you so much.
Shannon Nelson 1:04:24
Thanks for having me.
Bill Gasiamis 1:04:26
Well, thanks so much for joining us on today’s episode. I hope you enjoyed it. To learn more about my guests, including links and to download a full transcript of the entire episode. Please go to recoveryafterstroke.com/episodes. If you’d like to support this podcast, the best way to do it is to leave a five-star review and a few words about what the show means to you on iTunes and Spotify.
Bill Gasiamis 1:04:52
And if you’re watching on YouTube, comment below the video, like the episode and to get notifications on future episodes, subscribe to the show on the platform of your choice. Sharing the show with family and friends on social media will make it possible for people who may need this type of content to find it easier, and that may make a massive difference to someone that is on the road to recovery after their own experience with stroke. Thanks again for being here and listening. I really appreciate you see you on the next episode.
Intro 1:05:27
Importantly, we present many podcast designed to give you an insight and understanding into the experiences of other individuals opinions and treatment protocols discussed during any podcast are the individual’s own experience and we do not necessarily share the same opinion nor do we recommend any treatment protocol discussed.
Intro 1:05:44
All content on this website and any linked blog, podcast or video material controlled this website or content is created and produced for informational purposes only and is largely based on the personal experience of Bill gassy armas, the content is intended to complement your medical treatment and support healing.
Intro 1:06:01
It is not intended to be a substitute for professional medical advice and should not be relied on as health advice the information is general and may not be suitable for your personal injuries, circumstances or health objectives. Do not use our content as a standalone resource to diagnose, treat, cure or prevent any disease for therapeutic purposes or is a substitute for the advice of a health professional.
Intro 1:06:22
Never delay seeking advice or disregard the advice of a medical professional your doctor or your rehabilitation program based on our content. If you have any questions or concerns about your health or medical condition, please seek guidance from a doctor or other medical professional.
Intro 1:06:36
If you are experiencing a health emergency or think you might be, call 000 if in Australia or your local emergency number immediately for emergency assistance or go to the nearest hospital emergency department medical information changes constantly.
Intro 1:06:49
While we aim to provide current quality information in our content. We do not provide any guarantees and assume no legal liability or responsibility for the accuracy, currency or completeness of the content. If you choose to rely on any information within our content, you do so solely at your own risk. We are careful with links we provide however third-party links from our website are followed at your own risk and we are not responsible for any information you find there.






