Comprehensive Guide to Cerebrovascular Accident CVA Prevention and Management
Introduction
Welcome to our comprehensive guide on cerebrovascular accident (CVA) prevention and management. In this article, we will delve into the various aspects of CVA, its causes, prevention strategies, and effective management techniques. Our goal is to provide you with valuable information that can help you understand CVA better and take necessary measures to prevent it.
Understanding Cerebrovascular Accident
A cerebrovascular accident, also known as a CVA or stroke, is a serious medical condition that occurs when blood flow to the brain is disrupted, leading to the deprivation of oxygen and nutrients. This interruption can be caused by a blockage (ischemic CVA) or a rupture (hemorrhagic CVA) in a blood vessel within the brain. The consequences of a CVA can be severe and potentially life-threatening, making it crucial to focus on prevention and management.
The Importance of Cerebrovascular Accident Prevention
Prevention is always better than cure, and CVA is no exception. By adopting a proactive approach to cerebrovascular accident prevention, you can significantly reduce your risk of experiencing a CVA. Here are some key factors to consider:
Healthy Lifestyle Choices
Maintaining a healthy lifestyle plays a vital role in preventing cerebrovascular accidents. The following lifestyle choices can significantly lower your risk:
- Balanced Diet: Consume a diet rich in fruits, vegetables, whole grains, lean proteins, and healthy fats. Avoid excessive salt, sugar, and saturated fats.
- Regular Exercise: Engage in moderate-intensity aerobic activities, such as brisk walking or cycling, for at least 150 minutes per week. Additionally, incorporate strength training exercises to improve overall fitness.
- Weight Management: Maintain a healthy weight by balancing calorie intake with physical activity. Obesity is a risk factor for cerebrovascular accidents, so it’s important to strive for healthy body weight.
- Smoking Cessation: Quit smoking or avoid exposure to secondhand smoke. Smoking damages blood vessels increases blood pressure, and raises the risk of cerebrovascular accidents.
Hypertension Control
High blood pressure (hypertension) is a significant risk factor for cerebrovascular accidents. It’s crucial to monitor your blood pressure regularly and take the necessary steps to keep it within a healthy range. Lifestyle modifications, such as a healthy diet, regular exercise, stress reduction, and medication prescribed by a healthcare professional, can help manage hypertension effectively.
Diabetes Management
Diabetes is another risk factor for cerebrovascular accidents. Proper management of diabetes through regular monitoring, medication, a healthy diet, and lifestyle changes can help minimize the risk of CVAs.
Regular Health Check-ups
Routine health check-ups are essential for identifying and managing risk factors associated with cerebrovascular accidents. Regular visits to your healthcare provider allow for early detection and appropriate intervention, reducing the likelihood of CVA occurrence.
Recognizing Cerebrovascular Accident Symptoms
To effectively manage cerebrovascular accidents, it is crucial to recognize the warning signs promptly. Familiarize yourself with the acronym FAST:
Face Drooping: One side of the face droops or feels numb.
Arm Weakness: Weakness or numbness in one arm.
Speech Difficulty: Slurred speech or difficulty speaking coherently.
Time to Call Emergency: If any of the above symptoms are observed, call emergency services immediately.
Quick recognition and swift action can make a significant difference in the outcome of a cerebrovascular accident.
Emergency Response and Treatment
When a cerebrovascular accident occurs, time is of the essence. Immediate medical attention can help minimize brain damage and increase the chances of a full recovery. If you suspect someone is having a cerebrovascular accident, follow these steps:
- Call Emergency Services: Dial the emergency number in your country without delay.
- Stay with the Person: Keep the person calm and reassured until help arrives.
- Note the Time: Note the time when the symptoms first appeared. This information will assist medical professionals in determining appropriate treatment options.
- Do Not Offer Food or Medication: Refrain from giving anything to eat or drink until medical professionals provide guidance.
- Be Prepared: If possible, gather important medical information, such as the person’s medical history, current medications, and any known allergies, to share with the medical team.
Post-Cerebrovascular Accident Rehabilitation
Cerebrovascular accident rehabilitation is crucial for individuals who have experienced a CVA. It aims to improve physical, cognitive, and emotional function, helping patients regain independence and improve their quality of life. Rehabilitation programs may include:
- Physical Therapy: Exercises and activities to restore mobility, balance, and coordination.
- Occupational Therapy: Assisting individuals in relearning daily activities, such as dressing, eating, and bathing.
- Speech Therapy: Addressing speech and swallowing difficulties.
- Psychological Support: Counseling and emotional support to manage the psychological impact of cerebrovascular accidents.
Conclusion
In conclusion, cerebrovascular accident prevention and management are of utmost importance for maintaining good health and well-being. By adopting a healthy lifestyle, managing risk factors, recognizing CVA symptoms, and taking swift action during emergencies, you can significantly reduce the risk of cerebrovascular accidents and improve outcomes. Remember, prevention starts with knowledge and proactive steps toward a healthier life.
Now that you have a comprehensive understanding of cerebrovascular accident prevention and management, you are equipped with the knowledge to take proactive steps toward reducing the risk of CVAs. Remember, always consult with your healthcare professional for personalized advice and guidance. Stay informed, make healthy choices, and prioritize your well-being.
Interview with Cerebrovascular Accident CVA Survivor Melvin Milton
Melvin Milton experienced a Cerebrovascular Accident CVA which he is recovering from but some days it’s hard to remember appointments.
Highlights:
00:46 Introduction
02:22 Melvin Milton had a Cerebrovascular accident (CVA)
11:28 Dealing with emotions after a stroke
19:03 Melvin Milton’s levels of recovery
26:48 Juggling two jobs before the stroke
35:00 The dangers of self-diagnosis and self-medication
45:34 Avoiding things that do not support recovery
50:37 Mindset plays a massive role in your recovery
1:00:51 Dealing with emotional situations
Transcript:
Melvin Milton 0:00
So level one was being able to walk again and not use a walker or a cane, and that’s going great. Level two is getting like my arm and you know like riding again and doing all the functions that I normally do, level three would be working on getting back to me repairing those friendships, and relationships that kind of suffer, and moving on from there, you know, and then get back to Me and what makes me happy.
Intro 0:34
This is the Recovery after Stroke podcast. With Bill Gasiamis, helping you navigate recovery after stroke.
Introduction – Melvin Milton

Bill Gasiamis 0:46
Hello, and welcome to episode 258 of the Recovery after Stroke podcast. In today’s interview, I’m joined by Melvin Milton who experienced a Cerebrovascular accident CVA, which is just another name for an ischemic stroke. All right, Melvin Milton, welcome to the podcast.
Melvin Milton 1:06
Thank you. Thank you for having me.
Bill Gasiamis 1:08
We took a long time to get here. Some of the things that delayed us getting together and chatting are very familiar to me. And one of the things that I think was happening, and you’ll tell me in a minute, if it’s true, is I think that you’re having some trouble with calendar appointments, and kind of registering them in your head that you have an appointment coming up in the next however long. Because I used to write them down. I used to have reminders, and I still miss my appointments when I was going through rehabilitation after brain surgery. Is that familiar?
Melvin Milton 1:51
It’s very familiar. People are like, well, you should write it down. I’m like, I can’t write it down because my hand is still you know. Well, you should put it in your calendar like well, typing is a lot. Well, you should like you know, so it’s gotten better over time. But for example, with our meeting, some do fall through the cracks.
Bill Gasiamis 2:18
So what happened to you?
Melvin Milton had a Cerebrovascular accident (CVA)
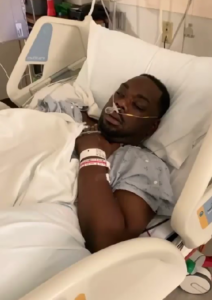
Melvin Milton 2:22
Oh, so July is almost year two right now 2021. Yeah, I suffered a left. I’m going to mess this up. I hope not a left CVA with a right hem.
Bill Gasiamis 2:51
A left CVA?
Melvin Milton 2:53
Uh-huh? With a right hem.
Bill Gasiamis 2:57
Okay, tell me about that. What is that?
Melvin Milton 2:58
That’s what my doctor said. He said cerebrovascular accident. That’s what he said. And I just found this out, because I haven’t really wanted to kind of explore in depth. What happened? You know, my first priority is to get better. And then I’ll, you know, the second step is to find out and the third step is to kind of help others if it happens to which I hope not, and if it does happen to.
Bill Gasiamis 3:39
Okay, I love it. So actually, according to Google, if I type CVA into Google, I get results from a website called healthline.com. It says my CVA is the medical term for a stroke sounds like a special way to say stroke.
Melvin Milton 4:03
I don’t know why you just didn’t say stroke but okay.
Bill Gasiamis 4:09
So, okay, you’ve had a stroke. So on the day of the stroke, what did you notice? How did you realize that was something wrong?
Melvin Milton 4:20
So that day is still really blurry. And I try to think about it and it’s coming back to me, as we go on, but I still don’t remember I remember that day so I had been doing a lot of traveling. I went to Michigan, Boston, and Denver, Colorado like, three weeks in the span of three weeks, then I came back home, which is Hawaii.
Melvin Milton 5:12
Then I flew back out to go to Vegas. So that was just a lot of, you know, like, post-pandemic, I just wanted to travel and get out. So, that whole thing was, is, is still kind of blurry, but I just remember working, and really not feeling well, like, you know, so I went home early, and then I woke up. And I went to the bathroom, and I you know, vomited, and I just did not feel good.
Melvin Milton 5:54
But then I, I woke up and my, my leg couldn’t move. And I was, you know, I just thought I’m gonna, I’m a really wild sleeper. So I just paid it to like, Oh, I just slept on it the wrong way, it should come back, you know. And so I went to the bathroom, and I was just kind of like, nauseated and just, you know, out of, I lost my bearings, and that fell.
Melvin Milton 6:22
And, I crawled back to bed. And I was just like, Well, maybe if I lay down, I will feel better, you know, but then I woke up and still nauseated and still vomiting. And, and then I, I was like, Oh, I’m not. This isn’t normal. So I called a couple of friends. And I finally want to answer. And, you know, like, and by this point, you know, I’m getting worse, as they call it, like, you know, like, I’m not as I’m not making sense.
Melvin Milton 7:03
And she said I think you’re having a stroke. She’s like, where do you live? I didn’t, I had just moved into an apartment about a month ago. So I didn’t really know. And I didn’t know, especially at that point. And that’s all that I remember. And then I woke up and just like, flashes. And so, um, I stayed and see the ICU for about a month. And then I moved out. And I was just in the regular part of the hospital, then I was in inpatient rehab for about a month. And then I went home. So that’s my story and the gist.
Bill Gasiamis 7:57
Yeah, understand. And when you went home, what sort of deficits did you go home with? What did you have to learn how to do again?
Melvin Milton 8:05
that was, Oh, that was. So when I went, Well, let me just back up and say that, when you know, I was in the ICU, the doctors don’t want to, you know, they don’t kind of, you know, let it go give you worst case scenario. And so they’re like, well, well, he’s not going to walk again. And he’s not going to do this and do that. And, so, my family and I will try to make, you know, like, preparations to, you know, get all these because, I mean, I’m in Hawaii, you know, with no family, they live, you know, on the mainland. And so, it was, you know, we had to make some adjustments. And so when I went home, I couldn’t have like, shower by myself, I couldn’t stand I couldn’t, you know, do any normal function really. So I was I had a walker then. So I couldn’t cook clean, or do anything. Basically, you know,
Bill Gasiamis 9:20
have any help at home did they manage?
Melvin Milton 9:24
I did have helped my family for the first part came down, and, you know, took care of me and my sister, my dad, and my Ontario, and then I had tons of friends that I’m so thankful for. I wanted to give them a good shout-out, like they are, you know, took time and made a schedule and, and came and brought me the things that I needed, and some things that the doctor said I I couldn’t have m&ms Hello, I’m so thankful for. So it was it was it was a group effort, to get me where I am today and I’m just totally thankful.
Bill Gasiamis 10:13
Yeah, M&M’s were not recommended by your doctors, for your physical health, but it sounds like they were necessary for your emotional health.
Melvin Milton 10:24
Thank you. Nobody, nobody gets that. Thank you. I knew I needed that to cope. I was, you know, I was going through like, Here I am, you know, so independent and have been, you know, all my life and having to, you know, depend on people it was an emotional toll. And I think one thing that I want to touch on we’re going to talk about this later, but I think that, you know, like, my brain was just like, going through a whirlwind of happiness, sadness, confusion, you know, so it was a lot to kind of, you know, understand,
Bill Gasiamis 11:16
yeah, roller coaster, it’s, yeah, for sure. How to describe it? How old? Were you at the time?
Melvin Milton 11:26
35.
Dealing with emotions after the Cerebrovascular Accident CVA
Bill Gasiamis 11:28
Yeah. So 35, everything’s going well, for 35 years, pretty much. Yeah, you have to deal with all of the drama of having a brain that has been injured by something that’s out of your control. And you have to come to terms with that emotionally, mentally, physically. And you have to do, it’s very rapid, it’s not like you get a warning, and you get time to plan for it.
Melvin Milton 11:54
Right. You have to, like, roll with it. And, and I think that you know, like, some, some people are, I’m sure you can attest to this as well. Like, some people, you know, didn’t quite understand like, Well, why is he mean, or why is he this? And why am I lashing out was it’s not? It’s, it’s I had a brain, I had three.
Melvin Milton 12:21
So I didn’t have one brain surgery, I had three. And so it was just a lot. Like, I was just like, a whirlwind of emotions, and I don’t think people quite understand how all that goes, you know, like, it made me way more emotional. And, and, and that’s just more understanding to people now because you never know what they may be going through.
Bill Gasiamis 12:55
Yeah, it’s so eye-opening. I was 37. So I was angry and emotional, and not myself. And right. Yeah, people were dealing with my illness as well. So they were they thought, oh, my gosh, this guy’s unwell. They thought, Oh, my, he might die. What does this mean for his future for our future? And then why is he screaming at me? And why did he get upset? The wrong ice cream.
Melvin Milton 13:23
You know, like, I’m so like, I I’m so happy that you brought that up. Because, you know, like, I had a falling out with a family member during last year’s Thanksgiving. And I, you know, just like, I just got overwhelmed with being surrounded with some, here I am, you know, mostly by myself with the first part of my recovery.
Melvin Milton 13:54
And then I’m going out of town to meet with my family, I’m exhausted, I’m overwhelmed. I’m emotional. And I just lashed out at one of my family members, and it just turned into this, this big, you know, like, this big thing. And so, you know, like, it’s, it’s, and we’re still not speaking right now. But, you know, it wasn’t me, you know, looking back over it. It’s like, I can’t I don’t even know how to explain it, but it was like, I’m looking back over. And I wouldn’t get upset about, you know, that, you know, but it was just a lot.
Bill Gasiamis 14:44
Yeah. It’s a thing, right? People are dealing with how they have to cope with what happened to them. Okay, so it’s confronting for them, that it makes them maybe think about their own mortality, their own health, and well obeying. It makes them think about their lifespan and all that kind of stuff, maybe. And then they go, Alright, I know what I can do is I can go and help Melvin out, and I can go and do some things for him and be nice and do all that stuff.
Bill Gasiamis 15:16
And then he speaks to me like that. Who would do that? Why would he speak to me like that? And then, you know, they might take it personally, and think that you’re having a personal attack on them. But what they don’t know is that everything is muddled up in your head, and stroke messes things up, and it takes a while for the things to recalibrate, and settle down. The only thing we can do, which I did a lot of was apologize. I just apologized a lot.
Melvin Milton 15:51
Yeah, and then. So like, I was reading, you know, all about you and the things, and one of the things that stuck out, like, when you were saying that you were, you know, not so nice and like that, like it really went home because I’ve had those episodes where I don’t like certain family members, I’m like, that I’m really close to in a real love so much like, they’re not, you know, talking to me right now, because of, you know, an episode that I don’t to be honest, I don’t even remember.
Melvin Milton 16:25
That’s the part about or, like sub certain friends. Like, I don’t even remember, like, you know, and I want to have these conversations, I want to you know, be able to clear the air and move forward. But, you know, how can I say like, I don’t remember when in my minor there probably like you’re just probably saying that, but I really don’t. Yeah, I know that something, you know, bad happened, or some words that weren’t so nice that were shared, but I don’t remember the basis of the argument, you know,
Bill Gasiamis 17:08
Yep. I found myself in lots of arguments that I had no idea what they were about. I was angry A week later, I still didn’t know why I was angry. Right? Right. So silly. But then all we can do is our part. So you’ve recognized that you, you may not remember that behavior, you’ve done it, they told you, you’ve done it, so you might as well believe them. And then you can apply it, you can apologize for it. And then you can go, the rest is up to you now, if you feel in your heart to forgive me, that’s fine. It’s up to you though. I can’t control that. And right, you know,
Melvin Milton 17:48
like, you know, like, the thing that, you know, like, I wish, you know, like people say, like I said before that they understand, but I wish that they could, you know, get a glimpse of how our brains are programmed, and we have to work really hard to get it back to normal, you know, I’ve been, I’ve been working my butt off too, you know, get back and I’m reading and watching podcasts and, and various Facebook groups and, and, you know, therapy, and, you know, so I’m doing my part, but I wish that you know as people would really give, you know, stroke victims a little bit more leniency and benefit of the doubt.
Bill Gasiamis 18:41
That’s excellent. What you just said was leniency and the benefit of the doubt. I mean, we can all practice that when it comes to those people who we come across in the shopping mall. In, in the bus, you know, in the wherever.
Melvin Milton 18:58
Shopping during Christmas.
Melvin Milton’s levels of recovery
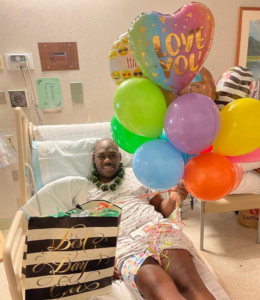
Bill Gasiamis 19:03
During the crazy season, right? We could all give people some leniency and the benefit of the doubt. And if, if we did that for them, and they did that for us, that would make life so much easier, because it means that we can make mistakes. And those mistakes don’t have to be the end of the earth. They just have to be mistakes that we recalibrate from and learn from and move on from and overcome rather than take to the grave. I mean, it’s just not worth it.
Melvin Milton 19:36
It’s not, so what I’ve kind of done for myself, I’m calling it the levels of giving back to me. So level I’m on the level.
Intro 19:54
If you’ve had a stroke, and you’re in recovery, you’ll know what a scary thing can feel Using time it can be, you’re likely to have a lot of questions going through your mind. Like, how long will it take to recover? Will I actually recover? What things should I avoid? In case I make matters worse, doctors will explain things. But obviously, you’ve never had a stroke before, you probably don’t know what questions to ask.
Intro 20:19
If this is you, you may be missing out on doing things that could help speed up your recovery. If you’re finding yourself in that situation, stop worrying, and head to recoveryafterstroke.com where you can download a guide that will help you it’s called seven questions to ask your doctor about your Stroke.
Intro 20:38
These seven questions are the ones Bill wished he’d asked when he was recovering from a stroke, they’ll not only help you better understand your condition, they’ll help you take a more active role in your recovery, head to the website. Now, recoverafterstroke.com and download the guide, it’s free.
Melvin Milton 20:57
Two or three, the level one was, you know, being able to walk again and not use a walker or cane and that’s going great. Level two is you know, like just getting like my arm. And you know, like riding again and doing all the functions that I normally do. And then you know, like level three would be, you know, working on getting back to me repairing those friendships, relationships that you know, have kind of, suffered and move on from there, you know, and then really, like, get back to me and what makes me happy. Like, for example, I love traveling, I love to work and, and I want to you know, get back to that, you know?
Bill Gasiamis 21:58
Yeah, so absolutely great goals. What kind of work were you doing?
Melvin Milton 22:04
So, I’m currently working two jobs. My first job I’ve been working at the Sheraton, Waikiki, and Honolulu. I’ve been there since 2011. Quite a while. And my second job, I’m an event coordinator at our local How would I say, event venue, so we do concerts and things like that.
Melvin Milton 22:39
So I definitely like to high pace jobs where I need to, you know, be on my feet and, and, you know, kinda, you know, be level-headed. And, you know, so I. So I’m working really hard. And actually, I’m going back to my event planning job really soon. So hopefully, I’m shooting for this year to go back to that.
Bill Gasiamis 23:12
I love Hawaii. I’ve been to Waikiki. Oh, great. Yeah. And we stayed somewhere near the Sheraton. I imagine I can’t remember where exactly we stayed.
Melvin Milton 23:24
Did you come into this place called Rimfire ever?
Bill Gasiamis 23:31
I can’t recall that.
Melvin Milton 23:34
That’s where I work. If you’ve come in for something I’ve probably served you.
Bill Gasiamis 23:43
Yeah, right. Okay. Amazing. So we spent time near that pink Hotel. What’s the pink hotel that’s there?
Melvin Milton 23:55
Oh, the Royal Hawaiian, which is next door to the Sheraton that’s our sister Hotel.
Bill Gasiamis 24:04
Okay, so we did spend time there. But we didn’t do a lot of the bar time in bars and places like that, because we had the kids with us. And they were both under the age of 16 at the time, so wouldn’t have been appropriate you see.
Melvin Milton 24:23
No, not yet.
Bill Gasiamis 24:27
And when we were there, I remember when we were there on the main road, they did a block party for the NFL. And they shut down the entire road down there.
Melvin Milton 24:42
They’ve just brought those back this year. And so they do it on the second Saturday of the month. So you just walk down the street and grab some food and grab some drinks and presents for everyone. That was one of the things that I really enjoyed doing.
Melvin Milton 25:05
When I first you know, got out of the hospital was to walk, you know, as far as I could just and then just to be, you know, because I had been away from, you know, no, I call it the real life or normal things or people. So that was able to, you know, walk and you know, purchase things and, you know, say hi to people I haven’t seen in a while. So, you know, that was really good for me.
Bill Gasiamis 25:38
I imagined the community in that part of that industry to be very tight-knit, there’d be everyone would know, you, and you would know, everybody.
Melvin Milton 25:47
Correct. They were everyone was, you know, and still it’s like, checking on me and calling like, the, like my coworkers were, you know, are so amazing. Like, they, you know, gave me you know, gifts and they bought me, you know, blankets for the hospital and the slacks and the m&ms and I weren’t supposed to have and, you know, when my family came to, you know, helped me out that took them around. They were just, you know, God’s sin angels. So, yeah, I want to thank all of my friends and co-workers for helping me out, you know, in so many ways.
Bill Gasiamis 26:33
Yeah. Yeah, it’s good. So now, the aim is to get back to both of your jobs? Or is it just to get back to one of them at this stage? And how far off do you feel you might be?
Juggling two jobs before the stroke
Melvin Milton 26:48
I don’t ever, as of right now, because, you know, I could change my mind. I don’t ever feel like I want to work two jobs again. I mean, I know I loved it. Because, you know, I could take off one hat. And, you know, put on another hat. And, you know, like, one job is not as serious, and one job, I am the boss. So I have to be, you know, a little bit more serious.
Melvin Milton 27:18
But, you know, I’m just, you know, gonna go with the flow and, and, and see how they, which one I liked the best and then just pick one or maybe even another one in the future. But hopefully, I’ll be back to work. Oh, hopefully, this month. Okay. Yeah, best of luck. It’s gonna be very slow. You know, it’s not going to be 40 hours a week, it’s going to be, you know, like, one or two days a week for, you know, three or four hours, you know, just to slowly get back into it.
Bill Gasiamis 28:05
So, you know, when you were working two jobs, how many hours a week we’re doing
Melvin Milton 28:13
Probably, like 50-55 hours a week?
Bill Gasiamis 28:19
Yeah. Did you do that out of necessity? Did you do that out of just the fact that you had time to do it? What was the thinking behind it?
Melvin Milton 28:30
I did it for a couple of reasons. Because my original plan was only to be in Hawaii for two and a half years, and that’s how long it took to get my master’s. But I found this job at the Sheraton and you know the benefits and the money the people I was having a lot of fun postgraduation and I kind of just stuck with it. And then I’ve got this other job as an event you know, manager or it’s, it’s more you know, in my field what I went to school for and I love doing it so I kinda did it for money and because I needed to work in my field.
Bill Gasiamis 29:27
Your master’s was in which field?
Melvin Milton 29:31
In the event planning Social Media Marketing.
Bill Gasiamis 29:37
Okay, so it was all linked there were all legitimate reasons. You are supporting yourself through college and all the things that you need to do. So it sounds like you were going about it the right way.
Melvin Milton 29:50
And definitely, I’m not gonna, you know, not a highlight this but definitely, because the money was good and I wasn’t tired. Hear them. And I was able to travel and, and shop and do everything I wanted to do. So yeah, it was it. You know, when I went to work, it wasn’t like I was, you know, like doing this, um, so tired. I’m like I was, you know, in a great mood happy to be there, you know, I’m gonna see what adventures I can, you know, do next you know? So it was a lot of fun.
Bill Gasiamis 30:32
Yeah. Did you feel like now that maybe you were neglecting your health or anything? Do you think there was anything causing that underlying there might have been no contribution to your stroke.
Melvin Milton 30:43
I definitely think I neglected taking care of myself, for example, my doctor prescribed me, you know, blood pressure medicine. But you know, of course, I took it, but I hated the way it made me feel. I hated that, you know, I felt I didn’t feel like myself, I felt, you know, kind of control. And it kind of brought me back to my childhood where I was on, I was prescribed ADHD medicine and, and that kind of that medicine kind of brought me back to my childhood where I felt controlled.
Melvin Milton 31:35
I felt, you know, tired, like, oh, I wasn’t myself. And so I, you know, me being the, you know, self-proclaimed doctor, well, I don’t need it, I feel fine. I’m gonna stop taking it. And, then that happened. But seeing that that happened now taught me a valuable lesson that, hey, you know, because if it’s not working, it was not quite right, go back and let them change it. And so that taught me a valuable lesson. You know, like, the minute, you know, I’m not feeling so great. I’m going.
Bill Gasiamis 32:11
Yeah, that’s a great lesson to learn. What’s interesting, I’ve never heard somebody say that blood pressure medication made them feel different or not themselves. So is that a common thing, you know? I’ve never heard that.
Melvin Milton 32:27
You know, I’ve talked to people that, you know, are on blood pressure medicines, and I’ve talked to a few and they don’t have any, you know, side effects, if you will, but I’m talking to one or two. And they have said that, you know, they feel a little off or, you know, something isn’t like, I don’t have full energy, you know, and then maintenance, I was talking to someone and somebody was like, well, maybe, you know, the blood pressure medicine was making you feel normal. I had been running off of, you know, not the medicine. And then that was bringing me you know, so that could have been the case too.
Bill Gasiamis 33:18
Okay, so, did a quick search about blood pressure medication making people feel strange. And it says Are they called alpha-blockers reduce nerve impulses to blood vessels, allowing blood to flow more easily. These medications may cause dizziness, lightheadedness, or weakness when standing up suddenly or getting up in the morning. Does that ring a bell? Did you have any of those experiences?
Melvin Milton 33:48
A lot of them like in the morning, you know, like, just like this good. Mornings are already you know, sometimes not the best, you know, like not pleasant, but it was definitely some Sundays have struggled and, and then went right after I would, you know, eat something and take my meds and I will get nauseous and lightheaded. So so but you know, but looking back over, like I said before like it’s one of those things where, you know, that was that was happening.
Melvin Milton 34:29
And it’s happened since then. And I’ve gone back to the doctor, and he said, Oh, well, we’ll just put, we’ll prescribe you this one. This one is better, you know, and it’s, it’s, it’s better. So what I want to tell anybody that’s that will listen to this is that if you’re taking medicine and you don’t feel so great, you know, call back and ask for a different dosage or a different you know, type of medicine, you know, until you get it right.
The dangers of self-diagnosis and self-medication
Bill Gasiamis 35:00
Yeah, absolutely. I hear so many stories of people who have stopped taking the medication for one thing or another, and they’ve had a brain hemorrhage or stroke or something like that. It’s not nice to hear, but it’s common. It’s very common. Yeah, you do hear about it. Especially when you described it. Like, if it’s, people kind of get it in their head, this is not making me better. This is making me feel worse. I’m going to self-diagnose it and not go and see my GP and not get professional advice on that.
Melvin Milton 35:35
That was me. The “I’m okay” I was a nurse, I was a doctor, you know, like, No, I’m okay. I don’t need it now. And then, you know, I was, you know, Google, Google is, you know, so good and so bad, because it, it kind of aides, a self-proclaimed nurses and doctors, oh, I can just, you know, take some apple cider vinegar in the morning, and I’ll be fine. You know, but it’s way more than that, you know?
Bill Gasiamis 36:10
Yeah. Deeper, it’s more complicated, we’re all unique. And my recommendation to you might not be suitable at all. And that might be the same thing for the next person. And it might help the other person a little. But we’re just so unique and so different.
Melvin Milton 36:28
Right. And nobody knows you. What I’ve learned too, is that nobody knows you more than your doctor, especially if you have a rapport with them. And you, you know, you’ve been seeing him or her for a while. You know, they know like, you know what to give you.
Bill Gasiamis 36:48
Yeah, so So Are you fully independent now? Do you live at home alone?
Melvin Milton 36:55
I was living at home alone. But Waikiki is getting so expensive now. So I wanted to, and then I’m not working, you know, those two jobs. So the income was not coming in like it used to. So I moved into a house with two of my friends, I work with one of them. And the other one is her brother. So I have helped if I need it, so my insurance and I just found this out this week, because I was so lost, because, you know, when I call it woke up, I had so many different things put in place.
Melvin Milton 37:46
But my insurance company is covering a housekeeper to help me with chores. So like things that I can’t do with both of my hands, for example, ironing or washing dishes, and, and you know, like, I do try to or making the bed, but I do try to do it but then I’ll you know, I’m sure you know this all too well get lightheaded and so fatigued and then I’m just like, they’re my arm starts to like space and, you know, it’s, it’s a chore.
Melvin Milton 38:29
But I’ve gotten so much better, like looking back at it. I couldn’t even I had to have a health aide come in and, and help me shower. But now I’m showering by myself, you know, I still need, you know, a shower chair because I can’t you know, stand up that long. I don’t want to, you know, slip and make matters worse, but, you know, I have you know, like, come a long way.
Bill Gasiamis 39:06
Yeah, that’s good to reflect on that. It’s so good. I’m glad that you’re noticing that. Stroke is very ADHD, isn’t it? Like, you start a lot of things that you can’t finish and then you need to get distracted and move on.
Melvin Milton 39:24
That is you know, like, I never thought of that. But that is a great way to describe it because like you know, like I’ll start like for example today. I you know, I wanted to you know, I woke up and I had a lot of energy and a great mood and like I’m going to clean the bathroom. So I was you know cleaning the bathroom. You know I get lightheaded and I’m like okay, I’m gonna lay down so like I started the bathroom. I’m about to get my new percentage done. I’ll finish it after this after this zoom, but, you know, if you’re right, like I start a lot of stuff that I just can’t finish.
Bill Gasiamis 40:13
And it’s not because of your attention is deficient that you’re born or lazy. It’s none of those. And it’s, it’s not because you can’t. Because you get distracted by something bigger or bright or better, it’s a little bit different. It’s because fatigue kicks in. Tiredness kicks in, whatever kicks in, and you have to literally sit down and lay down and rest until you feel better and well enough to do that. But I think I remember being in a situation.
Melvin Milton 40:44
I talked to my grandmother a lot, she’s 93. And she’s really excited about you know, as doing this, and she’s gonna be watching when it airs, but she, you know, tells me like you said to, you know, do a little bit at a time, you know, like, rest and get back to it. You know, so that’s what I, you know, kind of do you know, when I get these bursts of, I call it burst of energy. You know, get back, you know, get back to her.
Bill Gasiamis 41:17
Yes, the bursts of energy were great when they came. So you know, we were in Waikiki in 2013, it was less than a year after my tube blades and the brain. Oh, and, and I remember telling my wife, you don’t plan anything for me tomorrow.
Bill Gasiamis 41:37
Because I’ve, if I feel like the way I’m feeling today, I can’t do anything tomorrow, you take the kids, you guys go for a walk, find something that, you know, it’s going to be fun to do. Alone, maybe? Yeah, I can’t do it. And then I would wake up in the morning, feeling amazing having one of those bursts of energy and forgetting everything I said yesterday, we’re on, let’s go and do some stuff.
Melvin Milton 42:02
Right. And I think that, for me, looking back at it and listening to that, like, I think I need to kind of explain that to people because they don’t, you know, quite get it like, Oh, I’m great. I’m great. And then you know, an hour later. You know, it’s, it’s not me, you know, but so my question to you is, will it ever get better?
Bill Gasiamis 42:37
That’s a good question. And I like to be a little bit of the opposite of doctors. And I’d like to create possibilities for people and give them hope. And say things like, yeah, absolutely, it can get better. Because you are so early in your recovery. And your, My recovery has been going on for 10 years, and I’m still having bad days that are stroke related. You know how sometimes before the stroke, you had bad days, and you could just you know, have a rest and you went too hard or for too long? And you just write it off as Okay, I’m going to do nothing tomorrow, I’m just going to flake out somewhere.
Bill Gasiamis 43:18
It’s like that, but the stroke complicates those days and makes them harder than they used to be. And I still find myself in that situation, but less and less. So it’s not as common as it used to be for me to be able to blame, how I’m feeling on the stroke, the brain surgery, the brain damage, all that stuff. It’s less common that I do that. And therefore what I’m offering people is hope and what I try and say to people.
Bill Gasiamis 43:52
Especially the ones who I’m coaching who have really big goals that always let them you know, that seem to let themselves down is a one-year poststroke is like you just walked past the coffee table and smashed your foot on the corner of the leg. It’s like it’s that soon it’s so early in the recovery. And you know, the next day, you realize oh my gosh, my foot still hurts and I’m gonna go and get it checked out and then you get it checked out and then it’s fractured.
Bill Gasiamis 44:25
And the doctor says six weeks and the fracture will have healed and it’ll be better to stay off at an arrest right? Stroke doesn’t have a timeline. That’s the thing with it. And if you damage your foot or toe and I damaged my toe, they do give us the same timeline doesn’t matter how different we are as people. They give us the same six weeks the bone will heal. Everything will be back to normal. Stroke is completely unique.
Melvin Milton 44:57
Yeah, I was on one of the Facebook groups, and some, you know, I always, you know, kind of start my day and now you know, kind of read and see what people are posting. And someone said that I had my stroke, I think tenuous, close, but they said, and then they said, I just got a feeling in my hand, and I was just like, wow, after 10 years, so you’re right, like you, it’s honest on time.
Avoiding things that do not support recovery

Bill Gasiamis 45:32
So, it’s so strange. And it’s so hard to tell people that that don’t give up on having a new experience or something, come back to 10 20, whatever years away, but require some work, we have to look after ourselves and look after our health, and we have to avoid smoking, we have to avoid drinking if we can.
Bill Gasiamis 45:56
And we have to avoid a whole bunch of things so that we can create the right environment for the healing to continue to occur. You know, how some people smoke and drink excessively all the time and forever, they’re always creating the environment for health to decrease and things to get worse, we need to do the opposite, we need to make space for the brain to flourish.
Melvin Milton 46:21
Right. That is really true. And, and I’ve been learning, you know, so. Yes, so I did have questions. So I know that you know, I’ve talked about relationships, and for those relationships and friendships that I, you know, that have kind of suffered?
Melvin Milton 46:50
What do you recommend or what have you done? To kind of, you know, like, you know, we visited Max, I don’t want to lose, you know, the friendships that I’ve built, you know, for 10 plus years, so I don’t even want to, you know, not talk to, you know, my family members, you know, so how do I just kind of go from there,
Bill Gasiamis 47:16
I just got good at making appointments to see people and say, Hey, I know, I know, things have been a bit strange or weird at the moment between us. But I’d love to come and see you, or at least talk to you on the phone. And just explain myself, if not, in those words, you might have different words. But it’s like, let me explain myself and why I was that way.
Bill Gasiamis 47:39
And one of the other things I really did was I made this podcast for all the people that misunderstand stroke survivors. It’s for the purpose of trying to explain the unexplainable in stories. Yeah. And then what I hope is that some of the people who I’ve interviewed can go listen to my interview with Bill because this will explain a little bit about what I’ve been through and what my journey is. And it’ll tell you things that I can’t put in words or don’t know how to put in words.
Bill Gasiamis 48:17
We covered these topics. And we spoke about you, we didn’t mention your name or anything, but we spoke about you and the issue that we had in the podcast. So maybe that will help you understand. And you just reach out to them from your heart. And you just explain to them it’s not personal. And you’ve had 12 months of healing. So now you can reflect on the problem and the challenge that you caused and created. And now you can say, I see where I went wrong, you know, and I just want you to know, it wasn’t personal. It was my brain just being muddled up and rewiring.
Melvin Milton 48:56
Well, do you know why? Because I went through a phase of being, you know, like, I went through like an upset, angry, sad face. Like why do you know why that kind of happens?
Bill Gasiamis 49:15
Yeah, well, a lot of stroke survivors say that they have kind of a similar response where they have a real deep depressive sort of stage. And a lot of the times it’s actually caused by the nervous system being out of alignment and not being able to come back into balance in harmony, you know.
Bill Gasiamis 49:36
And sometimes you’ve heard of people who are bipolar, for example, whose nervous system makes them feel very, very happy at one point, and then very, very low at another point, and they always trying to get back to balance as well.
Bill Gasiamis 49:53
After a stroke. The damage throws out the balance and then you have to find a way to get back there. And the body’s readjusting and trying to get you back there on its own, just through the healing process.
Bill Gasiamis 50:09
And we also might be dealing with the difficulty of learning about, we are mortal now, we might be dealing with the difficulty of learning, if not independent anymore, I can’t do that, because I used to do, somebody will be concerned about not being able to pay the bills, the rent the food, and, and then they come back from the hospital with, you know, hospital bills, and all that.
Melvin Milton 50:35
All these new norms.
Mindset plays a massive role in your recovery
Bill Gasiamis 50:37
All these new things that they didn’t have to deal with before, and they may not have the skills to deal with it. And it’s difficult, because not only is it difficult because you’re dealing with stroke recovery, it’s difficult because they have all these extra problems that they never had before the stroke. So it gets people down, and their mood gets impacted.
Melvin Milton 51:02
I know that I spent probably the last part of last year to the first part of this year, really depressed, like really like in a dark space in. And you know, like, I’ve been climbing my way and, and working on getting out of that. And, you know, I’m currently still and PT, and OT, right, and I’m going to keep going to that for as long as I can. And until my insurances, you’ve had enough, no, because this, like, I still want this to work.
Melvin Milton 51:52
And I still want, you know, I still want to be able to walk, like, for example, like, my leg is fine, I can walk. But then there’s like certain days when I wake up, and it’s hard for me to walk around my leg, the lower part of my leg, it’s really tight. And you know, and then I can’t wear flip flops on my right foot, because my leg doesn’t have the control. So until you know, and, and I can’t write, you know what his right hand so until I can get you to know those things back, I’m gonna, you know, still go to therapy for it.
Bill Gasiamis 52:34
Yeah, I think we should. The other thing is, some people are not as happy-go-lucky as others, some people have just a habit of having a mindset that thinks about the negatives. And if you have that type of habit, and you have a stroke, it’s possible for you to start thinking of all the negative things that come from that, and it takes you a bit lower down, right?
Bill Gasiamis 52:57
So the mindset is really important. And what you seem to me like is, you seem like you’re happy-go-lucky most of the time. And now. And now you’re thinking about things that you’re going to go after to get back to recover from.
Melvin Milton 53:14
That’s exactly true. And, and, you know, one of the things that, you know, I’m getting back to would be, like I said, work, but number one is travel. So, one of my friends, I wanted to say thank you to her like she’s been an angel with taking me to, you know, the grocery store doctor’s appointments. And then for my birthday, which is in August, she is we’re going to see Beyonce Neck. Well, this month. So I’m going I’m traveling again. So, you know, like I am, I’m slowly getting there back to, you know, traveling and going to concerts and working soon. And, you know, like, my mood is great. So I’m I like to think that I’m almost there. Do you know?
Bill Gasiamis 54:13
Yeah, that’s great. One, I think that you’re almost there instead of so far away. Yeah. doesn’t talk, right? It doesn’t help.
Melvin Milton 54:22
Oh, my God. Take everything make everything worse. Yeah.
Bill Gasiamis 54:27
Yeah, think about you’re almost there. And if you’re not there, just keep going toward that place that you want to be. And that does help. Mindset plays a massive role in your recovery. And, you know, what also plays a massive role is gratitude. Now, I’m not saying that you can be I’m not saying that you have to be grateful for everything that stroke has caused or done because some of those things are not amazing.
Bill Gasiamis 54:52
But right be grateful for what you have and what you’ve been able to achieve and what you’ve been able to overcome and what you’ve learned about yourself and the new skills that you’ve acquired that you need. So it just, it’s really important that people practice gratitude, in spite of their suffering, so that they can find a way to look at is there a silver lining in this bloody thing that happened to me, you know.
Bill Gasiamis 55:19
And there might be now you already talked about the silver linings, your friends are amazing, they helped out, you know, you’re, you’re been able to get back on your feet, you appreciate how what other people are going through that you couldn’t appreciate before.
Bill Gasiamis 55:37
You’re more empathetic, you know, you found new ways to solve your problems, instead of living alone, now you live with another two people to bring down your costs. So it’s a bit easier. There are so many things that you can be grateful for, that you’ve worked on, and that you’ve overcome. And if you look for solutions to problems, you get solutions. If you look for problems, you’ll get more problems.
Melvin Milton 56:03
Yeah, that’s, you know, like, I’ve just been, as I said, claw in my, I feel like I’ve been in such a deep, dark place. And I’m just clawing my way out to get to the top. And I, I see the light, and I’m not going to stop to like, you know, the light. So yeah, I’m looking back over it. I’m thankful for, you know, what I’ve been through and how far I’ve become, because, you know, the doctors said that, oh, I’ll never do this. I’ve never done that. And I’m, I’m proving them wrong. And I’m just so thankful for everyone’s, you know, prayers and thoughts. And, you know, like, I’m still here, and I ain’t going nowhere.
Bill Gasiamis 56:59
Because a lot of blessings there. Did you go through that process? Do you separate like, the emotional and mental health side of it? Did you have any of those thoughts? Did you do the Oh, my gosh, I’m mortal? Or were you already aware of that? Like, how did you navigate that part of it?
Melvin Milton 57:27
I think it was, it was hard, because I’m so used to being independent, like, you know, buying everything I need, and, and, you know, just not asking for help. So that part of having to always ask, it’s, it’s like, I’m still not, like, for example, I’m not driving yet. I’m almost there. Hopefully, you know, by the end of the summer, I’ll be back. But it’s tough, having to “Do you mind taking me?”
Melvin Milton 58:05
You know, or, or just, you know, because I don’t want to be a burden to people. So that part is, is still, you know, rough for me to ask. Yeah, you know, but it’s, but I have people that really don’t mind, I just have to ask. But yeah, it’s taught me a lot to you know, appreciate.
Bill Gasiamis 58:31
If there are some people that are listening who are not stroke survivors, I’d like to encourage them also, to feel comfortable saying, No, I can’t help today. And not feel like it’s necessary to always say yes to a stroke survivor who asks for help. that nobody’s making you do it. And they’re just asking, and if it’s not possible, there might be another way to solve that problem.
Bill Gasiamis 58:55
But hopefully, nobody feels the obligation one way or another. Hopefully, it’s just a legitimate conversation. Hey, any chance I can get a lift? No, not today, because I can’t. Well, that’s it. Hopefully, there’s no guilt associated with that or anything else.
Melvin Milton 59:15
So I wanted to ask you something so I did, I had an I would consider this person really close friend of mine. They came to the hospital and sat there and, and, you know, when I was in the hospital, it was, you know, in and out. So I don’t remember a whole lot of things, but I do remember that this person, you know, sat on the bed and then tears and said, I’m gonna help you. I’m going to, we’re going to work out we’re going to eat healthy, we’re gonna, I’m gonna get you back.
Melvin Milton 59:56
And, I reached out to this person and like, hey, I got some extra, you know, exercises when you have time? Can you help me? I’m not saying, you know, twice a week or just whenever you have time. And this person told me, No, they couldn’t do it right now that would have to be, you know, a couple of months, you know, and then this person, so since then this person, we have not communicated.
Melvin Milton 1:00:31
And, you know, he came to say hi to me at my house one day, and then it was just that day when I was, you know, not in the best of moods, and I just wanted nothing to do with the conversation. And, we haven’t talked since then.
Melvin Milton Dealing with emotional situations
Melvin Milton 1:00:51
So, my challenge is how would I, you know, recreate a space that says, hey, I’m, you know, I’m back, or, I don’t know how to do that. Because, for me, I was hurt. Because, you know, I’ve got this goal, like, I’m gonna, you know, get better because I have you helping me. And then when I, you know, try to use that, and you turned me down, it destroyed me. So how would I kind of, you know, recover from that?
Bill Gasiamis 1:01:32
In emotional situations, like seeing a friend that you love in a hospital bed. People often say things they often overpromise, and then they don’t really have the skills to deliver. And it might be emotional skills, psychological skills, or physical skills. And what they do is they, they sort of step back, and when he came to visit you, he might have again misunderstood.
Bill Gasiamis 1:02:01
What is actually going on with you, when you’re having a really low day a really fatigued day and your mood isn’t the best? And he might think that it was personal that you were taking it out on him because of how he didn’t behave. Really. Yeah, right. Okay, so this is the thing, right? So all you need to do is I reckon create a meeting over lunch or something like that at a neutral location.
Bill Gasiamis 1:02:27
When I say neutral, it’s just a lovely place outdoors, right? Guys love to hang out, and just go there and go, Hey, let me buy you lunch. That’s it. And just start with that and just say, Listen, let me buy lunch. And right at the beginning, let me just tell you about how I was and what I thought. And now I’m understanding things differently.
Bill Gasiamis 1:02:48
And I’ve come to have an awareness and I’m sorry if I misunderstood or treated you harshly. And then let them say their part because I bet you they’ll be feeling the same thing that someone is waiting to make the first move to smooth things over, you know. And I think if you just do that a mutual venue at a neutral venue where you guys both love hanging out.
Bill Gasiamis 1:03:16
And it’s over a light lunch or something like that. I think it’ll go really well. And you just create the expectation. I’m going to be here for lunch. One of these days, which day suits you best to make sure that it’s really comfortable for everybody. Just reach out you got nothing to lose. And when you do that, what’s important for that Melvin when stroke survivors do reach out, that really helps to heal the brain.
Bill Gasiamis 1:03:52
If you can get the emotional healing and all of that stuff off your shoulders. It creates a base for healing the brain you know, it allows the energy to go somewhere else. And then you don’t have to worry about all of this additional energy that you need to allocate to healing friendships and relationships. You can do those get them done and then move on to healing yourself.
Melvin Milton 1:04:24
I like that healing the brain because it I feel that you know, I have been doing it and I feel like the there are two or three people that I want to you know, kind of have that conversation and you know, kind of smooth it out and then once I do those three I think I will be you know better because it bothers me, you know, that I don’t have those people I would call every day? You know, or send a meme to you on Instagram, you know? Or go out to eat with you know, so it’s, I will definitely do that soon.
Bill Gasiamis 1:05:19
There you go. So if a bothers you, then it’s getting in the way of your energy and it’s and it’s decreasing your battery for the day, you know, if you’re thinking about it and you’re being bothered by it. That’s, that’s not Yeah, it’s not creating a right the right environment for healing the brain, you know, the thing about stroke recovery, people don’t realize sometimes and it makes sense that you could miss it is that it’s the emotional recovery is really important.
Bill Gasiamis 1:05:50
Mental health recovery is really important. And then the physical recovery is really important, and they all have to happen, you can’t just do, I’m gonna get back to walking again, and then never talk to anybody for the rest of your life. You know, yeah, you can’t do that. And you can’t just neglect your walking, and then just have a really good mental health state, if you never decide to go after your walking and mobile, right?
Bill Gasiamis 1:06:19
They’re all linked, if you do one, it benefits the others, and they are all necessary. So that’s why healing relationships, and at least doing your part so that you’ve done your bit, if they choose not to reciprocate and not turn up to lunch, then you have to give them love and just let that person make their own decision in life.
Bill Gasiamis 1:06:46
And you have to be okay with it. It might be difficult at the time, but eventually, you have to be okay with that and let them go. I think what I learned was, when I did the, when I did the reaching out, and healed my relationships, the ones that I had messed up a little, I felt better about making the effort. And then I just left that other person to, to do their thing, what they needed to do in their own time, you know, so I don’t put, what’s the word, unnecessary pressure, forced them into something, you know?
Melvin Milton 1:07:22
Well, that makes sense. Because they have to, you know, kind of heal on their own. And that’s what I, you know, have been struggling with, because I’m like, well, well, shoot, I don’t even remember what I say, or what happened, you know, but hopefully, I’ll share this with them when it airs, and then they’ll be, you know, a little more okay with that.
Bill Gasiamis 1:07:54
Yeah, it might help. It definitely might help. Hey, I want to really thank you for making such a massive effort to get on the podcast, scheduling and rescheduling and rescheduling again, and being okay. With the fact that you missed a couple of appointments, no big deal, no harm done. And, here we are. So perseverance is really important in recovery. You’ve read, I really want to thank you for persevering and joining me on the show.
Melvin Milton 1:08:27
Thank you so much, Bill. I appreciate it.
Bill Gasiamis 1:08:30
Thanks for joining us on today’s episode to learn more about my guests including links to their social media and other pages. And to download a full transcript of the entire interview please go to recovery after stroke.com/episodes. If you would like to support this podcast, the best way to do it is to leave a five-star review and a few words about what the show means to you on iTunes and Spotify.
Bill Gasiamis 1:08:54
If you’re watching on YouTube, comment below the video I love receiving comments, and I respond to all people who comment, like this episode and to get notifications of future episodes, subscribe to the show on the platform of your choice. Now if you are a stroke survivor with a story to share about your experience, come and join me on the show. The interviews are not scripted, you do not have to plan for them.
Bill Gasiamis 1:09:19
All you need to do to qualify is be a stroke survivor or care for someone who is a stroke survivor or you work with stroke survivors go to recoveryafterstroke.com/contact, Fill out the form, and as soon as I receive your request I will respond with more details on how you can choose a time that works for you and me to meet over Zoom. Thanks again for being here and listening. I really appreciate you see you on the next episode.
Intro 1:09:46
Importantly, we present many podcasts designed to give you an insight and understanding into the experiences of other individuals. The opinions and treatment protocols discussed during any podcast are the individual’s own experience and we do not necessarily share the same opinion nor do we recommend any treatment protocol discussed.
Intro 1:10:03
All content on this website at any linked blog, podcast, or video material controlled by this website or content is created and produced for informational purposes only and is largely based on the personal experience of Bill Gasiamis. The content is intended to complement your medical treatment and support healing. It is not intended to be a substitute for professional medical advice and should not be relied on as health advice.
Intro 1:10:25
The information is general and may not be suitable for your personal injuries, circumstances, or health objectives. Do not use our content as a standalone resource to diagnose treat, cure or prevent any disease for therapeutic purposes or as a substitute for the advice of a health professional. Never delay seeking advice or disregard the advice of a medical professional your doctor or your rehabilitation program based on our content.
Intro 1:10:47
If you have any questions or concerns about your health or medical condition, please seek guidance from a doctor or other medical professional if you are experiencing a health emergency or think you might be, call 000 if in Australia or your local emergency number immediately for emergency assistance or go to the nearest hospital emergency department medical information changes constantly. While we aim to provide current quality information in our content.
Intro 1:11:10
We do not provide any guarantees and assume no legal liability or responsibility for the accuracy, currency, or completeness of the content. If you choose to rely on any information within our content, you do so solely at your own risk. We are careful with the links we provide however third-party links from our website are followed at your own risk and we are not responsible for any information you find there.







