Gloria Morgan had just given birth to her third child when a brain stem pons stroke threatened to turn what was supposed to be a happy time into a tragedy.
Socials: www.instagram.com/howglodoesit/
Highlights:
01:14 Introduction
03:18 Pons Stroke and Brain Stem Stroke symptoms
14:16 What is the Pons?
20:36 Stroke caused by pregnancy?
27:35 Nystagmus
36:50 Refusing to become right-handed
45:12 Tinnitus
50:17 The lessons
Gloria 0:00
And so now I’m recovering my left hand. And I know of a few other survivors who just switch to writing with their other hand, either because they were faced with paralysis, or they just couldn’t make it work, or they just decided that was the best decision for them.
Gloria 0:21
And so I thought about it, and I toyed with it a lot, but I am proud of being a lefty. I feel like it’s part of my identity. And I also realize that because I mean, like I have full use of my fingers like, it’s just a very fine control. And I felt like if I make the conscious effort to start writing with my other hand, then I feel like that will become a learned non-use that will be hard to overcome.
Intro 1:01
This is the recovery after stroke podcast. with Bill Gasiamis, helping you navigate recovery after stroke.
Introduction
Bill 1:14
Bill from recoveryafterstroke.com This is Episode 117. And my guest today is Gloria Morgan, Gloria experienced a rare Pons Brain Stem Stroke caused by a blood clot that may have formed around the time of giving birth to her third child.
Bill 1:29
Although she had some serious symptoms that were not usual stroke symptoms, it took doctors more than two weeks to make the diagnosis. Now just before we get started, if you have ever wondered what else I can do to help you with your stroke recovery, you should know that I have set up a few recovery after stroke support packages, where stroke survivors can come into a community while trying to get better on their own, and get help from people who are already further along in the recovery timeline.
Bill 1:57
I too am a three times stroke survivor, and a brain surgery survivor and I have built for you what I was missing when I was sent home from hospital in the hopes that you don’t have to do stroke recovery as tough as I did.
Bill 2:10
Support packages give you access to a variety of tools 24 hours a day, seven days a week, so that you can also work on other areas of stroke recovery that you don’t get the chance to at physical therapy or rehabilitation. With tailored support available for less than $8.50 per week all recovery after stroke support packages, bring stroke recovery to you in the comfort of your own home.
Bill 2:32
To try our recovery after stroke support and see if it is right for you to get the first seven days free, as well as a 30-day money-back guarantee no questions asked. As a bonus, you will also get to face to face zoom support calls with myself to take your recovery to the next level.
Bill 2:49
Go to recoveryafterstroke.com/slash support to sign up. It won’t cost you anything for the first seven days. And you’ll get a full refund. If you’re not happy after 30 days. You have nothing to lose and everything to gain. And now it’s on with the show. GLORIA Morgan, welcome to the podcast.
Gloria 3:08
Thank you.
Bill 3:09
Thank you for being here. I really appreciate it. I know it’s late where you live. Tell me a little bit about what happened to you.
Pons Stroke and Brain Stem Stroke symptoms
Gloria 3:16
Well, I had an ischemic stroke a left cerebellar stroke. So ischemic obviously I’m sure anyone who listens to this podcast is familiar it’s a blood clot rather than a hemorrhage stroke which is rupture of a blood vessel.
Gloria 3:38
But my stroke was extra special in that the location is very unique. So it happened in a part of the brain called the Pons. I think it stands for something I don’t really know. But basically, it’s part of the cerebellum, which is part of the brainstem. So cerebellar strokes are, I know you’re in Australia. So I don’t know if the statistic is the same worldwide, but I assumed it would be similar but in the US the statistic is less than 2% of all strokes, of any kind are cerebellar.
Gloria 4:24
And because the cerebellum deals with more delicate systems like vision, balance, swallowing and things like that, being part of the brainstem, it doesn’t present with the typical symptoms of stroke.
Gloria 4:42
So you know the acronym fast face, arm, all that stuff. Those are not the typical symptoms. So what I learned is that cerebellar strokes typically present with the three V’s violent headache, vomiting, and vertigo, which I did have all of those three. But we didn’t know. And those are not typical symptoms.
Gloria 5:10
And I’ve never heard of the three V’s. So we didn’t know. So, what happened is, I had a baby. And, about a week after having the baby, I started getting headaches, and they were pretty bad, which was unusual, because I don’t usually get headaches, but you know, I just had a baby, which is a big experience, and all of a sudden, you don’t sleep at all.
Gloria 5:40
So, I just didn’t think anything of it, I just thought, Oh, I need more rest. And I need to drink more water and eat more high protein foods, you know, now im feeding a baby that really depletes your body a lot. So, and then after about a week, after the headache started, I started in addition to a really bad headache, like, I mean, like, it was so bad, it would wake me up at night, it wasn’t a headache I could sleep through.
Gloria 6:13
After about a week of that off and on, I started getting some like, I would have moments where it would look like the room was kind of like swimming around. And after about that, about four days of that happening off and on, all of a sudden, one day, I got double vision, just like the room split in half and just started going like this.
Gloria 6:40
And, you know, that went on for like a minute. And then it went back to normal and just a headache. And at that point, I was like, okay, that’s not normal, I should call my doctor. But the symptoms had already been going on for like a week and a half, almost two weeks at that point.
Gloria 7:00
And so, I talked to my Obgyn, she referred me to my primary care doctor, and my primary care doctor wanted to see me right away. And I’ll just kind of push this all together, because of course, there’s a lot more detail in there. But basically, I went to see my primary care doctor, and she wanted me to see an EMT and otolaryngologist nose, throat guy, just basically to rule out vertigo.
Gloria 7:35
And she insisted on having me see that guy that day. And so I went straight from her office to his office, like she called him up, he was a friend, she called him up and had me go over there and straight away. And this is the only part of the story that I feel like is important, because I think for many of us, especially young stroke survivors, it’s like those little things that we missed that we regret that now we feel like, I need to tell people so that if this happens to them, like they won’t skip over this and think it’s nothing.
Gloria 8:13
They’ll just go like, go get the MRI, go get the test, go get the scan, just call the doctor, you know, so that they’ll find out hopefully, it’s a false alarm. And if it’s not a false alarm, you’ll catch it in time.
Gloria 8:28
So we went to the EMT, and he asked me about all my symptoms, and I did a few tests and stuff. And then he explained at the end of the appointment that probably I had benign positional vertigo, which is you know, very mild thing like crystals and calcium crystals in the ear getting displaced and it can cause dizziness and even cause novel visions.
Gloria 8:57
So I was like, okay, that’s obviously what I had, because it wouldn’t be anything more serious than that. And no just had a baby, you know, that’ll really really mess you up. And little did I know. And so he gave me something called the Epley maneuver, just it’s like a set of exercises you do where you like turn your head to different sides at different angles, which can apparently help roll the calcium, the displaced calcium crystals in your ear and just reposition them so that it basically resolves the vertigo.
Gloria 9:36
And I explained that I needed to do these exercises, you know, at so many times per day, and if I didn’t see the symptoms improve, then I should go to the ER because that means it’s not a physiological problem. It’s a neurological problem. And he didn’t say it was a lot of alarm, because I guess he’s a doctor.
Gloria 10:04
But he didn’t say it seriously. And so when he said, that means, you know, if your symptoms don’t improve, that means you should go to the ER right away because that means it’s not a physiological problem. It’s a neurological problem. And so I said, you mean like a stroke? Like, just joking. And he looked at me and said, Yes, not joking.
Gloria 10:30
I know, right? And so we went home. And by that time, my eyes were just like, not really seeing clearly. And so I was having to walk, I remember I was having to, like, touch things to kind of, like, keep my balance. But I’ve got, displaced crystals in my ear, I just, you know, and just need to rest and do these weird exercises.
Gloria 10:42
So I wake up the next morning, and do the weird exercises, and which it should be noted, these exercises, were literally laying on my back, turning my head in a series of directions, very specifically, which, obviously, I never realized I was basically moving blood clots around in my head, is what happened.
Gloria 11:24
So within about 15 minutes of doing those maneuvers, I got up from doing the exercises, and then you know, I have a baby, I haven’t really slept that much before, I need to eat something. So I scarf, like a piece of toast and some water and then, like, all of a sudden, it just all comes up all of it violently into the sink over and over and over again.
Gloria 11:55
And basically that was the rest of the day. That was it. Like I couldn’t, all of a sudden, I couldn’t walk, I had to like shakily crawl back to my bed. And I couldn’t see I was seeing double, everything was moving around and there’s two of everything. And I couldn’t stop throwing up. And that’s when we knew it was really bad because I couldn’t hold that water and, like not even water, like it would just all come up violently over and over and over again until I was just dry heaving over the toilet.
Gloria 12:30
Nothing would stay in my body. And you know, I had a 24-day old baby who needs to eat like every two or three hours. I couldn’t hold him. I couldn’t see him. I couldn’t see what I was doing. So my husband had to go out like two hours later, he had to go out and go to the store and get baby formula.
Gloria 12:48
And our baby went from breastfed to formula fed, like literally overnight, like in one feeding. He went from breast friend to bottle fed and that was it. Because I couldn’t feed him. And so we thought, I don’t know what we thought at that point. It just the word stroke never entered my mind.
Gloria 13:10
And I’ll be honest, I don’t actually remember making that joking comment to the EMT. I didn’t remember that until months and months later. Like when I was telling the story to someone I was like, Oh, yeah, I actually joke with the guy like he was trying to tell us like this could be a stroke. I joked with him like do you mean I might be having a stroke? And he was like, Yeah, and I didn’t even remember.
Bill 13:40
Well, you’re probably having a stroke. And that’s maybe why you didn’t remember it. How long did it take? How long did it actually finally take for you to get diagnosed?
Gloria 13:54
From the original, like the very first onset of symptoms to actual like, I’m in the hospital getting MRI, it was about two weeks. But from the point of me, calling a doctor to getting diagnosed was probably like 48 hours.
What is the Pons?
Bill 14:16
Yeah, well, even then. So it took you two weeks, you’re dealing with this for two weeks. So just for people listening, who might not know the pons, according to teach me anatomy.info is the largest part of the brainstem. It’s located between the medulla, which is the bottom part of the brainstem that comes up from the spine just before it gets to the actual brain.
Bill 14:44
And then, and then there’s the pons, quite a large area of the brainstem. It’s the last part of the brainstem. And then it attaches to the middle brain, the part that actually is nearest to the cerebellum.
Bill 14:56
I had my bleed near the cerebellum and the second time it bled, and the blade was really large, I had vertigo I had throwing up and I had all those symptoms, except for the headache or didn’t have the headache that you described, I had those other things.
Bill 15:14
And I didn’t have those at the beginning and the, and the symptoms that you described, less than 20% of people who experienced a stroke have the standard fast symptoms of stroke. So the other people, the 20%, that don’t fit that category have all these different versions of potential neurological issues showing up that you ignore.
Bill 15:44
Like you, it took me a week before the hospital to tell them that I couldn’t feel my left side. You know, it took me a long time to come to terms with the fact that the changes in my body were potentially something serious and I was 37. Like, as if I was having a stroke. How old were you?
Gloria 16:05
I was 35. So this was two years ago, almost two and a half years ago.
Bill 16:11
Yeah. What was the hardest thing? not physically or emotionally for you at that time? What was the hardest thing that looking back now you had to deal with?
Gloria 16:24
Emotionally? Really, it was the fact that I just had a baby, like, I had a 24 day old baby who just all of a sudden didn’t have a mom. And we have three kids. And the oldest is six just now. So when the stroke happened, he was not even four and a half. And then we had a two year old who, and he was still having a bottle with me every morning.
Gloria 16:52
So he would get up, have his bottle of milk in my lap in the rocking chair. And then he would go play and I would feed the new baby. And then, you know, all of that, like they didn’t understand. So the hardest part emotionally was basically feeling like my kids were being ripped away from me.
Gloria 17:14
And then also being separated from my husband for six weeks, because we’re very close. And but yeah, the hardest part. For me, it was emotionally, it was definitely feeling like I was losing my kids. And like, knowing that my kids were missing their mom, like I will never forget, my husband’s a tech guy.
Gloria 17:36
So he had everything set up, like connected to our phones. And so even in hospital from my phone, I can click into the monitor in our son’s room, and look, and so I made the mistake.
Intro 17:51
If you’ve had a stroke, and you’re in recovery, you’ll know what a scary and confusing time it can be, you’re likely to have a lot of questions going through your mind. Like now how long will it take to recover? Will I actually recover? What things should I avoid? In case I make matters worse, doctors will explain things. But obviously, you’ve never had a stroke before, you probably don’t know what questions to ask.
Intro 18:15
If this is you, you may be missing out on doing things that could help speed up your recovery. If you’re finding yourself in that situation. Stop worrying, and head to recoveryafterstroke.com where you can download a guide that will help you it’s called the seven questions to ask your doctor about your stroke.
Intro 18:34
These seven questions are the ones Bill wished he’d asked when he was recovering from a stroke, they’ll not only help you better understand your condition, they’ll help you take a more active role in your recovery. head to the website now, recoveryafterstroke.com and download the guide. It’s free.
Gloria 18:53
The second night I was in the hospital. I was in the ICU at this point. I clicked into the the monitor in our kids room and like eight o’clock at night around them time basically. And there was my husband on the floor holding my four year old who was screaming with his entire being like just as loud as he could scream like his whole body is just shaking and he was just like screaming and thrashing.
Gloria 19:31
Just in that moment, I physically felt like my heart is going to just rip in half and die like I’m going to die this hurts so bad. so that that was the hardest thing emotionally.
Bill 19:45
Yeah, I’m sorry to bring it up. I just wanted to give people an understanding that when people have a stroke, everything stops automatically and it doesn’t matter what you’re in the middle of nothing continues. And I know that’s the same for anyone else who has any other type of, you know, health challenge, I get it, I get that too, right?
Bill 20:06
That you have to go from being a mom of three kids to a stroke survivor and happens so quickly and leave a 24 day old baby at home with your husband. Yeah, and then somehow you have to navigate all these things, just all at the same time, and you don’t have any of the skills, you don’t have any of the support any of that. No idea. And all of a sudden.
Gloria 20:35
It’s just thrust on you.
Stroke caused by pregnancy?

Bill 20:36
Yeah. And it’s emotionally really challenging, I didn’t have that kind of separation, anxiety from my kids, they’re a bit old, and we’re able to see them and there was none of that stuff going on. But I can’t imagine what it would have been like to be such a young mom, and there is a theme in some of my podcasts as a few ladies who have had a stroke, or near or around childbirth, Is this some kind of underlying reason that may have caused that to happen then for you.
Gloria 21:07
I’ve never actually talked about this before. But this is the terrifying and sad truth, I probably did this to myself. So what happened is that, you know, I like to be healthy. And you know, I’m young. And I like to consider myself an attractive person. So you know, I want to take care of my body.
Gloria 21:32
And we always talked about having three kids. So this was the third kid and I was like, you know, after this, we’re going to be done. And now I’m going to focus on me and taking care of my body and getting myself back to where I want to be where I feel good in my own skin.
Gloria 21:47
Any mom listening to this is gonna relate. So the third time was, for whatever reason, it was the easiest delivery super fast, I felt great, almost zero pain, like just barely any discomfort, like nothing. So I was feeling really good really fast. And within a week, I decided, you know what, I’m not going to do anything crazy, I’m not going to go run a marathon, I’m not going to get on the treadmill, and I’ll just do some yoga, I’ll just do a little bit of yoga, something very gentle.
Gloria 22:25
And what I realized later, is that, you know, after childbirth, you have an open wound in your uterus that is bleeding. And a major problem, the opposite problem is when women bleed out after birth, so that’s why most women, and after immediately after delivering a baby, they’ll get a vitamin K shot, because vitamin K helps your blood clot.
Gloria 22:57
And what you want is for your blood to clot. So that the wound in the uterus, seals up and you don’t hemorrhage and bleed out. Because that’s a very serious life threatening problem for women who’ve had a baby.
Gloria 23:13
But the thing is, you have an open wound healing up in your body and what I did, because in yoga, you know, the downward dog position, you’ve got your hips up above your head.
Gloria 23:24
And so basically, I was pointing an open clotting wound at my head. And so I mean, this is my theory, and I talked about it with my obgyn she concurred that that was a very likely cause, that it was the yoga of all things. I’m not saying Yoga is bad. But for women who have just had a baby.
Bill 23:52
You don’t need to do that.
Gloria 23:54
Don’t do handstands, like it’s okay to do some stretching, if you feel up for that. But you should never put your hips above the level of your head when your uterus is bleeding. Because those blood clots those teeny, tiny, microscopic blood clots. I mean, just gravity is gonna do its thing, it’s going to pull them down.
Gloria 24:16
And if your head is down there, it’s going to go into your head. That’s why women who just had a baby are also very closely monitored for something called DVT. deep vein thrombosis, which is basically the same thing. It’s just the clots going into your legs rather than your head. So I don’t know, maybe if I hadn’t been doing yoga, maybe I would have had DVT instead. I don’t know. We don’t know.
Bill 24:46
It’s a hypothesis worth thinking about. But the fact that there’s no underlying cause is a good thing in that now you know that it’s not something else going wrong that’s causing these things to occur and how how long Are you in the hospital? And what deficits Did you have when you came out of hospital.
Gloria 25:05
So I was in the ICU for a week, and then I was in a rehab hospital for five weeks, so a total of six weeks. And when I was discharged home, I was not able to walk, I was barely able to stand on my own. Excuse me. And so part of the cerebellum, as you must know, is that it affects your balance.
Gloria 25:35
And my major deficit is I lost fine motor control on my left side. So I can still move all my limbs, thankfully. But the muscle tears basically, in the whole left side of my body didn’t work together. So like, you know, if any stroke survivor, you probably had to do this test where you do this thing, I can move all the fingers in my hand. But like, if I tried to hold a pen, say, like, guide, I can’t.
Gloria 26:14
But it was a lot worse when I was in the hospital, like I would hold up my two arms and my left arm would just float away on it. So and I couldn’t do anything about it, I would have to wait for it to stop floating, and then like, consciously pull it back.
Bill 26:32
So when you went home, you also weren’t able to fully be involved in your motherly duties, your responsibility, your baby again, you still had to sit on the sidelines.
Gloria 26:48
Yeah, basically, I would just move between the bed and the chair so that I would get put in a chair. And anytime the baby needed to feed, they would hand me the baby. And that would just like subtract one of the kids to be taken care of. And so every time he needed to be fed, I would feed him like I would hold him and give him a bottle, which I really appreciated.
Gloria 27:12
But that was about all I could do. Until I was able to start walking again. Which actually happened pretty soon it came together pretty soon after I was discharged from the hospital, I was almost kind of there, which is why I think they were like, Okay, get her out. She’s gonna be fine.
Nystagmus
Gloria 27:35
But that was the biggest physical deficit. But I really the biggest deficit overall was my eyes. So basically, when we went to the hospital, I was seeing crazy double, and everything was just like shaking around. And it just stayed like that. And it’s slowly improved to where I don’t see double all the time. And the movement is less. But that is the greatest misery of every waking moment of my life now.
Bill 28:19
So the slight vibration of the eye, what’s it’s called?
Gloria 28:25
Nystagmus.
Bill 28:27
Say it again?
Gloria 28:28
Nystagmus. So it’s not very obvious here all this. But if you can see, like you’ll see my eye just kind of ticking.
Bill 28:43
Yes, yes, it’s moving. Left and Right, left and right all the time.
Gloria 28:48
Right. And if I look up, then it goes up and down. And if I look straight, like, if I look directly at the camera, it looks like I’m just kind of looking around. But that’s because I can’t directly focus my eyes. So what you see is my eyes just kind of looking around, like I just don’t want to look in the eye.
Gloria 29:10
But what I see right now looking at the camera is I see two edges of the laptop, and four little dots kind of jumping around. And so my eyes are like constantly trying to pull things together and like make things stand still. And that’s every waking moment. And it’s maddening. So that’s the worst thing.
Bill 29:35
Is there. Anything that can be done about that? Does it resolve does it get better?
Gloria 29:44
No. I’m no farther. There’s no treatments and the only treatment I’ve been offered by traditional medicine is opioids. And all that does is basically just it’s not a treatment. It’s it’s symptom management. So it’s supposed to basically just sedate the brain so that hopefully the eyes would less.
Gloria 30:16
And I mean, we were desperate, you know, so we tried one that my neuro ophthalmologist recommended. And it made me It did nothing. It changed absolutely nothing in my eyes, but it made me so like kind of woozy that I would fall over from a sitting position, just like sitting Indian style, or what do you call it? You know? Just on the floor. Cross legs I just fall right over. I fell over on my baby and hurt him. So nope, can’t do that.
Bill 30:55
Wow. Yeah. That’s tough. So you’ve been going through it now for around two years, your husband stepped up and did all the things he had to do. We had a chance to speak to him about what he went through and what it was like for him to suddenly not know what’s happening to you, and what might that mean for his children and him?
Gloria 31:20
I’ve gotten sort of a picture based on things he says, but he’s the kind of guy who’s like, just do what you got to do. Like, I mean, he will push through everything, whether it’s like, his wife having a stroke, or like just doing the dishes or putting the kids to bed or if it needs to be done.
Gloria 31:37
He’s He’s a German engineer. If it needs to be done, he’ll just do it. But I did, just like from his comments here and there, or to other people or things, like his mom told me a lot of things because when I was in the ER, and like, unconscious, his parents and his brother came up.
Gloria 32:00
And so we were in Northern California, they’re in Southern California, it’s about a six hour drive. And so we went to the ER Friday afternoon, and I don’t want to freak anybody out. But it was July 13th. So it was Friday the 13th. I’m not superstitious, but I do like to point that out to people. Because, I mean.
Bill 32:27
It’s fun. It’s quirky.
Gloria 32:32
I like that. It’s fun. It’s quirky. That’s what I’m gonna say about it next time. But yeah, so we went to the ER, four o’clock on a Friday afternoon. And probably within two hours, we knew that it was serious. And I think they diagnosed it, like within three hours or less. It took several stands, because FYI, a cerebellar stroke will not show up on a CAT scan. It might look like a tumor, but it will not present on a CAT scan, you have to have an MRI. So just good to know.
Bill 33:17
So then, are you driving now? Are you back at being physically active like that?
Gloria 33:24
No, I’m able to walk. But I have to fight for my balance every single step. So I’m not yet able to balance on either leg actually, which means that walking is very much a challenge.
Gloria 33:39
So that’s my physical recovery goal for the next year of my recovery is I want to be able to balance on one leg, because having that balance will mean that I have a better command of my body in order to control motion like jogging, like, ultimately, I want to be able to go back to jogging.
Gloria 34:02
I wasn’t a big jogger before the stroke. But that’s mainly because I had small kids. So I was actually starting to ramp up and invest in good workout gear. And like training abs, like I was starting to get into it. And then I had a stroke. Well, when I had a baby and then I had a stroke. And so everything just like you said just everything. It just stops without warning no matter what it is.
Bill 34:32
Yeah, your recent posts on Instagram. You show photos of your face before and after. And how it’s improving. Was one side drooped for quite a while and was the eye affected for quite a while.
Gloria 34:53
Yeah, so I would say I mean it was the whole left side of my face was basically immobile probably for at least the first two months, or no, I should say at least the first month. And then by the end of my time in rehab, I was starting to see a little bit of improvement, they had exercises taped up in my room that I was supposed to do where you like, you know, open your mouth and stretch your lips, and use your tongue and all that kind of stuff.
Gloria 35:26
And, you know, make a fish face and make a big O and all those kinds of things. And because I didn’t know what else to do, there was very little else I could do on my own, I would just do that over and over again. So I was starting to see a little bit of improvement by the time I was discharged.
Gloria 35:48
And then I haven’t been like, consistent with exercises, specifically for my face most of the time. But recently, I have been trying to be more consistent with it. Because to be honest, when the pandemic started, and everything shut down, I basically lost the ability to do any kind of meaningful recovery therapy of any kind.
Gloria 36:17
And doing face exercises, or something for which you don’t need equipment, you don’t need a therapist, you can just, you know, oh, I’m sitting here while my kid plays with this toy in my lap, and he doesn’t need to get some students in here.
Gloria 36:35
I’m just gonna sit here and pull funny faces.
Bill 36:39
Yeah, I’ve also seen a post there with regards to your writing. So were you right-handed? And now you can’t write with your right hand, what happened with the right hand?
Refusing to become right-handed
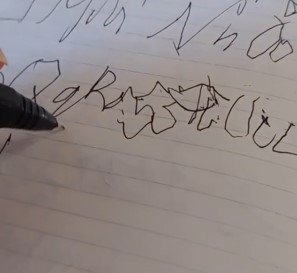 Gloria 36:51
Gloria 36:51
So it was the left side and I was left-handed before. And so now I’m recovering my left hand. And I know of a few other survivors who just switch to writing with their other hand, either because they were faced with paralysis, or they just couldn’t make it work, or they just decided that was the best decision for them.
Gloria 37:17
And so I thought about it. And I toyed with it a lot. But honestly, I am proud of being a lefty. I feel like it’s part of my identity. And I also realize that because I mean, like I have full use of my fingers. Like, it’s just a very fine control. And I felt like if I make the conscious effort to start writing with my other hand, then I feel like that will become a learned non-use that will be hard to overcome.
Gloria 38:01
Yeah, yeah. So I decided, basically, my motto as stroke recovery, in general, is do the hard thing. And like, so even in the rehab hospital, if my therapist like at the end of the session, they would say, Oh, we have time for one more exercise. Do you want to do this? Or do you want to do that? I would always ask, which one’s harder? Ok let’s do that one. Like, whatever is hard, do that.
Bill 38:28
Yeah, that’s not a bad approach. I know that some people avoid doing something hard, that’s painful, that’s difficult. Because they’re going through a lot of other things right. And doing another thing hard and difficult might be, you know, not on the to do this, just let it go push aside, find the easy solution.
Bill 38:48
Sometimes that’s a really good approach to because if that makes you feel better, that you found an easy solution and a quick solution. That’s a positive thing as well. But I’m like you, I tend to take the stairs instead of the elevator or the escalator. And I won’t or if I’m extremely tired, but I will do it when I’m feeling good about it because I can walk and most people wouldn’t notice that I’ve had a stroke.
Bill 39:12
And they would have noticed that our left side struggles a little bit, especially going upstairs, you know, if if I’m tired, I might clip at the bottom of one of the steps. And that might cause me a trip or lose my balance. But if I’m feeling well, I’ll make sure that I take the escalators because I don’t want to get to that point where I’m avoiding doing something that is really important, like walking upstairs because we have stairs at home. And, you know, just want to make sure that I practice that. And it’s such an easy way to practice. Without putting in too much effort.
Gloria 39:46
Absolutely. We just moved into a house that has stairs. And thankfully when we were looking for a house. We didn’t put any limits. assumed it would have stairs. And we both the day we got the keys to the house, I went up the stairs and came down again. And of course, I had to hold the handrail and be careful.
Gloria 40:11
But by the end of the day, I got up and down the stairs probably, I don’t know, half a dozen times, or maybe more, maybe 10 times or a dozen times. And I had to you know, concentrated Be careful each time but I was when did I feel exhausted or fatigued? Or, you know, all I had to do is just be careful and carry things.
Gloria 40:37
And so my husband and I were both like, oh, the stairs are no problem. Yeah. And we Yeah, even just today you’re like, well, so when the stairs problem, and he’s, you know, you asked earlier what his feeling is what his reaction wasn’t, I don’t think I quite answered it.
Gloria 40:56
But basically, he was just like, oh, you can do it. You can do it. But then whenever it’s like, oh, I can handle stairs and it’s fine. He was like, oh, but can you just see the relief Like he wasn’t willing to show that he wasn’t worried. But then the relief comes out like, these are no problems. You’re just like running up and down the stairs. No problem.
Bill 41:15
Yeah. So he’s trying to protect you from showing concern or worry. But then when something amazing happens, he is unable to withhold.
Gloria 41:26
There’s a little crack like, Oh, I really was worried.
Bill 41:30
Yeah, yeah, I understand. That’s a man thing. And that’s probably a German man thing more than it is an Australian man thing. But yeah, it’s definitely a man thing.
Gloria 41:40
Thank you for translating.
Bill 41:41
Yeah. With regards to the children now, how have they been getting their mom back? Have they kind of transition back to, “what was normal” beforehand now with a new sibling, and all that stuff?
Gloria 41:59
Yeah, I mean, you know how adaptable kids are, especially young kids. So they adapted to the changes. But on the other hand, they’re just kids. So like, they understand that mom, had a brain owee that’s how I explained, because, you know, our kids are so young, her oldest was four and a half when it happened.
Gloria 42:21
So he understands owee he is. And so I explained it like, well, I had an owee in my brain made me forget how to walk and I can’t drive anymore. And so he understood that. So that’s what my kids understand. I have a brain owee. And now my oldest son understands that brain owees are called strokes.
Gloria 42:42
Doctors call a brain owee a stroke. And strokes are very serious. And, you know, we try not to get too serious with them. But like, on the one hand, they’ll ask me to come play with them. And they’ll, like, run up to me and like, just like, run into, you know, barrel into me and grab me around the legs. And I’ll have to scream. Don’t hit mama, mama can fall down, you know?
Bill 43:12
They can bring you on stuck.
Gloria 43:14
Yeah. So they’ll like play with me. Like they forgotten that I can fall over and get hurt. But on the other hand, like our oldest is, like, Sometimes he’ll show an extrordinary concern, like, unusual concern, like, you know, Mama, I want to protect you. So you don’t get hurt. Like he’s conscious that’s something happened to me that was serious. And he worries and like our four year old, who was only two and a half.
Gloria 43:46
And it’s hard to tell him because he’s still so young, but he hates being alone. So if you can’t find Mama or Dada, he’ll get really upset. And now that we’re in, like, we used to be in an apartment now we’re in a bigger house, so even if I’m just downstairs, so just want to come in, like, even if he’s just, you know, watching something on his tablet, he has to be where he can see us.
Gloria 44:15
And he’ll like, he still wakes up in the middle of the night and comes into our room and wants to sleep next to me or on me or like, just be closer, all the time. And all of our kids are like that they constantly want to be close to each other or to us and so, it’s sweet.
Bill 44:31
Sensitive Kids, that’s all that’s all.
Gloria 44:35
Yeah, on the one hand, they’ve adapted to what my limitations are and they tend to forget, sometimes they need to be a little extra careful. But they’re just kids, they just play which is great. But on the other hand, they do have this slight kind of awareness in the background on to that thing happened to Mama so they’re extra sensitive about like, being careful sometimes. and wanting to they’re just very affectionate, which I think is wonderful.
Tinnitus

Bill 45:13
It’s beautiful. It’s awesome. Tell me about the noise that they make. So being young and being kids, they’re going to be very loud and boisterous and fully energetic does the noise and the energy that they have sometimes tire you out and take you kind of to that place of fatigue?
Gloria 45:33
Every single day. So I don’t talk about this as much on my Instagram or in person, because I honestly just don’t have time to think about it. But I also lost all the hearing in my left ear and I have really bad tinnitus. So right now, for example, I’m really only hearing you in my right ear.
Gloria 45:59
And in my left ear, I hear like a really high pitched electronic buzzing, almost like a sound machine or like an old CRT TV like that high pitched electronical. And it’s really, really loud. Like, I can hear it over the noise of a vacuum cleaner, or a blender, it’s really loud.
Gloria 46:21
So any background noise at all just like air conditioning, or a fan or like the dishwasher or just like, while I’m washing my hands, any background noise at all, I won’t be able to understand someone talking to me, even if they’re standing right next to me. So any noise the kids make let’s just say I’m really glad we have a big backyard,
Bill 46:53
You can send them out when you need to.
Gloria 46:55
Yeah, and so I just after a while I just decided like this needs to be a rule. Now we have a house, we have a backyard. And so I just tell my kids loud noises are for outside you can make if you’re going to make loud noises, you can go outside. So when they start yelling in the house, I’ll give them morning counts. Like that’s one loud noises outside.
Gloria 47:17
And if I get to three, I just tell them like, it’s not really a punishment, per se. It’s like, okay, that’s three, you need to go outside, go outside, that’s where you make loud noises. Or if they want to like seeing or if they’re just playing a loud game, I tell them like your noises are just for you, you can go do that in your room.
Gloria 47:37
And, you know, if you’re playing that game, or you want to sing that song or whatever, like you can do that in your room. But if you’re going to be in the living room, this is a space for everyone. You have to share, and your noises are just for you. So I’m trying to use it as a way to teach them basically respect and consideration for others.
Gloria 47:51
So I try not to make it too much about me and the fact that I’m deaf. I’m trying to partially deaf, I’m trying to make it more about just educating them to be sensitive to the existence and comfort of others.
Bill 48:13
I think you’re doing a great job.
Gloria 48:15
Cool. Thank you.
Bill 48:16
Yeah, it sounds like it because it’s a really unique approach and a lot of mums and dads will be listening, wondering how to navigate this. And I stuffed that up because I would just lose my marbles and yell and scream and be really insensitive to them and really treat them unfairly.
Bill 48:32
But not because I was trying to be nasty or aggressive. It’s just because I was at my wit’s end. And I didn’t know how else to do it. And they copped it. And, and then I would spend a lot of time apologizing, and try to make up for the mistakes that I made.
Bill 48:48
But I didn’t understand. And perhaps they were a bit older. They were teenagers. So we didn’t have those rules previously. So trying to create new rules around, something like, this was almost impossible anyway.
Gloria 49:03
Oh, yeah, for sure. I mean, my kids are really young. So they’re learning the world for the first time anyway. So in that sense, I’m glad that this happened earlier on, so we can just kind of like all learn and grow. And so I’m just teaching them. Like, they’re learning everything for the first time as it is.
Gloria 49:24
And this is just kind of part of that. Yeah. And I also realized that, you know, everyone’s deficits are different, like, the tinnitus is horrible and terrible and unbearable, and all the negative things, but there are some people who deal with like, you know, noise sensitivity or photo sensitivity or other things that were the reaction to noise or light or things like that is extreme. And, you know, so everyone’s deficits and struggles are different.
Bill 49:59
Yeah, that’s it. I asked now I know, I’m aware of the time because I know it’s after midnight already where you are. So as we come to wrap up, I just wanted to ask you about what some of the biggest lessons have been like, is there something that has stood out?
The lessons

Bill 50:17
That you’ve kind of gone? Oh okay. And, and It happen for me, there was a lot of them. And I know a lot of stroke survivors talk about getting something good out of this thing, like, has there been something like that for you?
Gloria 50:32
Definitely a number one lesson. And this is just a phrase that I made up for myself, everyone’s pain is their own. Which basically, to me means don’t compare you suffering. And I seen those two things as basically a gateway to empathy, like, that should bring you to empathy.
Gloria 50:55
So that was the big aha moment for me was, like, in order to really empathize with people or someone has gone through something hard, so that when you are going through something hard, you know, they get it.
Gloria 51:27
So, I realized early on, you know, if I started talking about what I was going through, people would say, Oh, I totally know what you mean, I get headaches too. Or sometimes my eyes bother me too or, oh, sometimes I get tinnitus too. Or Oh, I know what you mean. Like some days, I just am so tired. Like, oh that’s insane.
Bill 51:58
So they try and have a conversation with you by bringing themselves to a place where they can relate and then continue the conversation in a cordial way. But they don’t know how to relate. And they use skills available to relate. And they failed dismally. But then it’s also important for us, to allow them to fail dismally, and to just not make it.
Gloria 52:27
Not make it a big deal. Yeah.
Bill 52:29
And try to teach them a lesson all the time.
Gloria 52:31
Yeah. But as a survivor, I mean, I’m sure you know, it’s hurtful to just be like, Oh, yeah. And to minimize your own suffering. And after doing that many, many times, and I’m sure, you know, I’ll probably continue to have to do that permanently now. It really just helped me realize like, you know, I probably do that to other people.
Gloria 53:00
And just because I’m going through something harder than them, or that I feel is harder than what they’re going through. That doesn’t mean they’re suffering in any less of a struggle, like my suffering doesn’t invalidate yours. So I remember talking to a friend one day, and she’s just, you know, your typical stay at home mom.
Gloria 53:25
And she was having a hard time. And, you know, you’re talking to him, like, oh, but I know it’s nothing compared to what you’re going through. And that was the little moment where it clicked. I was like, You know what? You know, she has had a stroke. But that does not mean her day is not fresh, straining, or that she should feel frustrated and like vent a little bit.
Gloria 53:48
And so I told her, you know, just because your biggest struggle this week, was that your toddler mashed banana into the carpet. Like if that’s the biggest thing you struggled with this week, if that’s your most frustrating problem this week, the fact that you didn’t have a stroke doesn’t make the mashed banana in the carpet any less frustrating.
Gloria 54:15
So that, to me, it just became this mantra to meet everyone’s pain is their own, like, it still hurts to them, it’s still a struggle to them don’t invalidate what other people are going through. Because it’s not the same.
Bill 54:33
We can win the I struggle more than you battle every time. I mean, if we wanted to, apparently, you know, our like you said it’s worse for us than it is for them. But when the banana gets mashed into the carpet, it’s not the banana in the carpet that’s the issue. It’s all those little things that have led up to the banana in the carpet. That we cop and cop and cop and cop and cop and cop and then one day, a banana in the carpet just drives you bonkers.
Gloria 55:03
Yeah, exactly. See, now I can tell you’re a parent, you know, you get. It’s not about the banana in the carpet, it’s all the other little things. And so I just realized whether it’s a mom at home with her kids getting frustrated over, you know, the mess at home and just never having enough me time, whatever, or it’s, you know, I’ve had friends who have lost a loved one suddenly and tragically in ways that were just devastating.
Gloria 55:32
You know, there are, you know, like, I don’t know what it’s like to have, I just told a friend this the other day, like, I would never compare the tension headaches I get with my eye problems to a migraine because I have never had a migraine. You know, she gets migraines all the time, which is terrible. And I know how much how painful and what of what a struggling is for her.
Gloria 55:58
So you know, I’m not gonna be like, Oh, well, you know, that’s nothing compared to what I went through. Like, I’ve never had a migraine in my life. Yes, I had a stroke, but I never had a migraine. So, like, Why make her feel like, what she’s going through? Isn’t worthy of weight? Yeah, it’s like, there’s no reason to invalidate it. Her suffering is still valid.
Bill 56:22
Yeah. Gloria, thank you so much. I really appreciate you reaching out and being on the podcast, I realized that it’s 12:30am, where you are right now.
Gloria 56:34
You’re very kind to keep the time I wasn’t paying attention. And I didn’t notice.
Bill 56:39
I know. If I was a stroke survivor, I probably wouldn’t get on somebody’s podcast at 12:30. I am. Because I don’t do well, if I haven’t slept enough. So I really just appreciate you being on here. I appreciate your sharing on Instagram. It made me curious about getting to meet you and understanding a little bit about what you do and how you’re going about your recovery.
Bill 57:03
I think it does help for me to see what you’re going through and the sharing that you’re doing. And I think a lot of other stroke survivors respond in the same way. So well done, keep doing what you’re doing. And I hope everything goes well from here on.
Gloria 57:16
If you don’t mind. Can I just mention one thing for anyone interested in checking out my story on Instagram, I do want to caveat that, like I do like sharing progress and recovery and hope. But a lot of what I share on Instagram is related to grief and the struggle just because I find that for me at least, I just really believe that sharing the grieving process is very healthy and productive.
Gloria 57:46
But I also don’t want to alarm or depress anyone, I’m not there, constantly, like grieving over my life. Just sometimes whenever those really hard moments happen. That’s what I share. So I do tend to share a lot of that stuff. Just as when I first came on Instagram looking for other young stroke survivors, I mostly saw people who were like your stroke four years, we can do this. And I didn’t see a lot of people who were expressing what I was feeling. So I just started thinking like, Guys, this really sucks and I hated it.
Bill 58:18
And that’s so fair, because it does suck and it is shit. And I go through this a lot. And I didn’t get that from your page. I didn’t get that you just talk about the negative or the grief and all that kind of stuff. I’ve got that it’s an inspiring thing. And your stories are true. And they’re real. And for me, I do post about things like the screws in my head hurt, and why do they hurt and you put that out there and people respond and they go yeah, the screws in my head hurt as well.
Bill 58:46
And then it’s because of the barometric pressure, and oh my god, like it’s scientific. Wow, like, you know, there’s a whole different kind of level of learning and understanding. You know? So thanks for saying that. But I didn’t get that from your Instagram for people who want to follow you.
Bill 59:04
I’ll have a link to your Instagram there. And they can reach out and have a look for themselves. That kind of stuff. your photos are pretty cool. There’s some photos there. There’s food photos. There’s handwriting photos. There’s a lots of stuff. There’s even a book that is about the foods that you should eat to help with health and well being and it’s next to a cake.
Gloria 59:33
Yes, hashtag doing it wrong.
Bill 59:38
I love it thank you Gloria so much.
Gloria 59:40
Welcome. Thank you for having me.
Bill 59:44
Well, thanks for listening to this episode of the recovery after stroke podcast. If you like this episode or any other episode, please hit the like button. If you’re watching on social media. Give us a thumbs up if you are watching on YouTube and give the recovery after stroke podcast a five star review on your favorite podcast app. Doing that, we’ll make the podcast more visible to other strike survivors that are doing it tough right now, and it could help them feel inspired and feel better about the road ahead.
Intro 1:00:19
Discover how to heal your brain after stroke go to recoveryafterstroke.com.
Intro 1:00:29
Importantly, we present many podcasts designed to give you an insight and understanding into the experiences of other individuals opinions and treatment protocols discussed during any podcast are the individual’s own experience and we do not necessarily share the same opinion nor do we recommend any treatment protocol discussed.
Intro 1:00:46
All content on this website at any linked blog, podcast or video material controlled this website or content is created and produced for informational purposes only and is largely based on the personal experience of Bill Gasiamis.
Intro 1:00:58
The content is intended to complement your medical treatment and support healing. It is not intended to be a substitute for professional medical advice and should not be relied on as health advice. The information is general and may not be suitable for your personal injuries, circumstances or health objectives.
Intro 1:01:14
Do not use our content as a standalone resource to diagnose treat, cure or prevent any disease for therapeutic purposes or as a substitute for the advice of a health professional. Never delay seeking advice or disregard the advice of a medical professional, your doctor or your rehabilitation program based on our content if you have any questions or concerns about your health or medical condition, please seek guidance from a doctor or other medical professional.
Intro 1:01:37
If you are experiencing a health emergency or think you might be called triple zero in Australia or your local emergency number immediately for emergency assistance or go to the nearest hospital emergency department medical information changes constantly. While we aim to provide current quality information in our content.
Intro 1:01:53
We do not provide any guarantees and assume no legal liability or responsibility for the accuracy, currency or completeness of the content. If you choose to rely on any information within our content you do so solely at your own risk. We are careful with links we provide however third party links from our website I followed at your own risk and we are not responsible for any information you find there.







