Unraveling the Complexity of Arteriovenous Malformations: Cutting-Edge Treatments
Navigating AVM Recovery: Comprehensive Insights into Effective Rehabilitation
Introduction
Embarking on the road to AVM recovery requires a nuanced understanding of effective rehabilitation. In this guide, we unravel the complexities of Arteriovenous Malformations (AVMs) and delve into cutting-edge treatments that pave the way for successful recovery.
Grasping Arteriovenous Malformations
AVMs, disrupting natural blood flow with abnormal connections between arteries and veins, demand expert intervention. Our mission is to demystify AVM complexities, shedding light on innovative treatments tailored for recovery.
A Closer Look at Neurological AVMs
Focusing on neurological AVMs, these unique challenges within the brain necessitate specialized care for optimal recovery.
Precision Diagnosis for Targeted Recovery
Accurate diagnosis forms the foundation for effective recovery plans. Modern medical imaging techniques, including angiography and MRI scans, empower clinicians to visualize AVM intricacies, tailoring treatments to individual needs.
Innovative Recovery Approaches
1. Endovascular Embolization
A cutting-edge technique involving catheter-guided embolization reduces bleeding risks, promoting targeted recovery.
2. Stereotactic Radiosurgery
Non-invasive and precise, radiosurgery targets small, deep-seated AVMs, advancing recovery outcomes.
3. Microsurgical Resection
Advancements in microsurgical techniques enhance recovery by meticulously removing accessible AVMs.
Beyond Treatment: A Holistic Approach to Recovery
The recovery journey extends into comprehensive rehabilitation, integrating physical therapy, cognitive exercises, and continuous monitoring for a full recovery post-AVM intervention.
Conclusion
Navigating AVM recovery is not a solitary endeavor. Embrace the support of communities and resources like “Recovery After Stroke” podcasts. Connect with others on the same journey, sharing insights and triumphs on the path to recovery from AVM challenges.
Navigate your AVM recovery journey armed with knowledge, cutting-edge treatments, and a supportive community. Triumph over challenges and emerge stronger on the path to recovery.
The Interview
Chet Ciccone had one side of his skull removed so that his brain could have space to swell after the faulty blood vessel in his head burst when he was 27.
Highlights:
00:42 Introduction
01:32 First signs of AVM rupture
09:39 Recovery after a cerebral edema
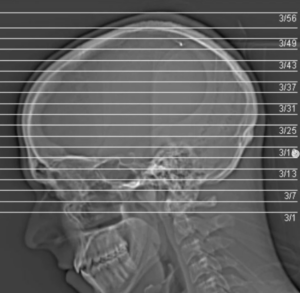
21:45 X Rays can cause cavernous angioma
26:21 Dealing with Anosognosia
29:37 Navigating the deficits after a stroke
42:21 Driving a vehicle after a stroke
48:05 Post-stroke effects and driving limitations
55:07 Living with half a skull
1:13:31 AVM recovery and career path evolution
1:24:04 Lessons from the stroke
1:26:21 The message
Transcript:
Intro 0:00
Hello everyone, my book about stroke recovery is now available for purchase on Amazon. It’s called the unexpected way that a stroke became the best thing that happened. In the book you will find chapters on mindset, the brain that resides in your heart, as well as the brain that resides in your gut, you will learn about all the benefits and downsides to Neuroplasticity.
Bill 0:23
You will learn the benefits of getting better sleep, you’ll find out about the food that you should avoid after a stroke. The amazing benefits you get from the smallest amount of exercise. You will learn what happens when you follow your heart’s desires and how it can transform your recovery.
Introduction – Chet Ciconne

Bill 0:42
And you will learn about the amazing benefits you get from surrounding yourself with the right people and how to discover your life’s purpose. Go to recoveryafterstroke.com/book to learn more. Now, this is episode 289. My guest today is Chet Ciccone who was 27 in 2016 when he experienced a hemorrhagic stroke due to a previously undiagnosed arteriovenous malformation, also referred to as an AVM Chet Ciccone welcome to the podcast.
Chet Ciconne 1:17
Thank you for having me. It’s an honor.
Bill 1:21
Pleasure, absolute pleasure. You’re another AVM brother.
Chet Ciconne 1:25
That’s right.
Bill 1:27
Tell me about what happened to you, man.
First signs of AVM rupture
Chet Ciconne 1:32
In 2016, I was 27 years old and had like a pretty normal day at work. I was working as a geotechnical engineer, it’s a subset of civil engineering, and made it all the way home and decided to unwind and play some competitive video games online, which is not unwinding but is kind of intense.
Chet Ciconne 2:01
Yeah, and got my blood pressure going a little bit. And halfway through one of the games that we’re competing in, I just started to feel warm and kinda confused a little bit. And so we finished the game, but I went to the bathroom and just washed my face because I was feeling so warm and uncomfortable.
Chet Ciconne 2:28
And just walking to the bathroom, I kind of knocked over some stuff that was in my apartment. And noticed that my balance wasn’t great and my coordination made it to the bathroom and washed my face. But I just knew something was wrong. I had no idea what it was.
Chet Ciconne 2:52
And ironically, like at that exact moment, one of my best friends and roommates came home from work. And so he opens the door and he’s all excited like, Oh, hey, like what’s going on? Because we always greet each other. And we’re always excited to see each other.
Chet Ciconne 3:08
But he could just tell that something was wrong with me. And I was like because I was not excited at all about it and was just like, Yeah, I don’t feel all that great. And he’s like okay well just sit down. And so I sit down. And he’s asking me questions and whatnot. And as time goes by, you know, I go to move my left arm and I think I’m moving it, you know, just to lean on a door.
Chet Ciconne 3:35
But I end up punching the doorframe because I have no awareness of where that arm is in space. I had no control of that arm. And I still had a little bit of feeling because it hurt. But so I was like, that’s weird. Like, I can’t feel this arm. And so yeah, I just couldn’t feel my arm at all.
Chet Ciconne 4:01
And my friend who had just come home, he was he had worked in an old folks home retirement home as one of his jobs. So he was kind of aware of stroke symptoms and what to look for. And so as time went on, and I started getting worse, he suspected that I was maybe having a stroke.
Chet Ciconne 4:23
It sure didn’t make sense to him because I was 27 and seemed you know, really healthy. But so luckily he and one of my other roommates decided to call the ambulance and they got there and asked if I could walk downstairs I said no, like, I definitely can’t walk.
Chet Ciconne 4:45
And I started to lose my memory at this point. I remember the ambulance ride there. Kind of realized that the paramedics were asking me questions to keep me alive and felt like, like they were trying to like, keep my attention. And I noticed that I was like, Okay, this is like really serious. So I was just kind of in a daze or whatever.
Chet Ciconne 5:12
And once I realized that, like, my life was on the line I really, I tried to stay focused and answer all those questions and pay attention. And I wasn’t really scared, I was just really determined and focused. And at some point, during the ambulance ride, I started just vomiting over and over, which I guess is common when you have blood on your brain.
Chet Ciconne 5:39
And we get to the emergency room. And I checked later, like, because I was playing this online video game, so I have like chat messages with a timestamp on them. And then I was able to look on Google Maps to like when I arrived at the emergency room and is only 45 minutes from, like, the initial onset of symptoms to get into the emergency room.
Chet Ciconne 6:05
And I think because of the vomiting and because of my symptoms, they diagnosed me pretty accurately. They even assumed AVM very early on. And so that’s 100% The reason that I’ve been able to recover so well. And for the reason I’m even alive, because you know, I had a roommate come home at perfect timing.
Chet Ciconne 6:29
Kind of knew what a stroke could look like. And got me to the hospital, like as quick as possible. So that just shows how important stroke awareness is. And teaching people about the symptoms of stroke, because you never know, who we might save, like, just knowing about a stroke.
Chet Ciconne 6:54
So that was that was on April 11. And they were able to stop the bleeding that day, you know, my memory is pretty foggy of some of those times, but they went in with a catheter and shot like some kind of glue it’s called embolization and stop the bleeding.
Chet Ciconne 7:23
But they wanted to wait to do surgery for whatever reason, maybe they knew that my brain would swell, I guess the younger you are, in these instances, your brain begins to swell as a reaction to your brain bleeding. And so they’re like, on the seventh, I think their plan was the 18th. They’re going to wait seven days to do a small incision in my skull, go in there, clean everything out, and try to remove the AVM.
Chet Ciconne 7:57
But I never made it to that surgery date. I ended up flatlining on the 17 which was a crazy experience. My parents had been staying at a hotel nearby, just to check up on me and support me in all the ways. And it was just another night where I was saying goodnight to them, and they were gonna go back to the hotel.
Chet Ciconne 8:26
Said goodnight, love you, all that stuff. They leave. And I don’t know how long after but that’s when I flatlined and so they called back like, Oh, he’s not doing well, you guys have to come back. And what I remember was kind of replaying all the family members that had visited me throughout my whole time that whole week, I had been in a hospital.
Chet Ciconne 8:55
And then all of a sudden, I’m with my grandma, like, in this like yellow sky on pink clouds. So, you know, obviously, depending on how spiritual you are, or how scientific you are, because I have been on you know, I’d been on opioids for a week, right? Like being on Dilaudid and painkillers, morphine, whatever.
Chet Ciconne 9:23
I’m either hallucinating or I’m in heaven with my grandma. So I feel like, you know, I was actually with my grandma. That’s what I like to believe. But I accept if somebody wants to say that I was just hallucinating on drugs. I’m fine with that, too.
AVM recovery after a cerebral edema
Bill 9:39
I like it. It’s something for everybody.
Chet Ciconne 9:42
And yeah, that was it. I woke up and basically, my brain had swelled too large for my skull. And that’s what had made me flatline. So they had to do an emergency craniotomy, where they were just going to do a small circle, just to focus on the AVM. Now it’s a new issue, it’s not just my brain bleeding, it’s, my brain needs space.
Chet Ciconne 10:13
So they cut almost a third of my skull off and put it in the freezer. And that just gives my brain room as well. And so I wake up to my mom, and she just is trying to explain, you know, hey, don’t touch the right side of your head, because you had a major surgery, you know, we almost lost you.
Chet Ciconne 10:40
And it’s just like a very powerful moment between mother and son, because, you know, I almost just passed away. But then kind of fitting because I am sick right now. The next thing that happened was a doctor came in and was like, just trying to break down like, you know, hey, you probably can’t feel the left side of your body. And I’m like, Oh, I can’t.
Chet Ciconne 11:07
And explaining my symptoms to me and why they exist. And he was like, you know, as time goes on, hopefully, you’ll feel better. But maybe when you get sick, some of these symptoms will come back. But it’s definitely like, years later, the first time, maybe a year later was the first time I got sick after my surgery, and I got all this numbness like coming back times 10 On the left side, and it’s really scary to not once you’ve had it once, and you associated with a stroke.
Chet Ciconne 11:40
When you get that numbness on that side of your body, it freaks you out, like I’ve gone to the dentist and gotten numbed. And it’s like, really anxiety-inducing. But uh, yeah, notice, like, whenever I do get sick, that numbness come back stronger, and dizziness would come back a little stronger.
Bill 12:01
And then does it settle after you get better?
Chet Ciconne 12:04
It does, for sure. And now eight years later, like I don’t, I didn’t feel that at all, with this sickness that I have today. So eight years, you know, things have changed so much. And I think that’s why people get so annoyed with stroke survivors when they hear the one-year thing because, yeah, in one year, like a lot of things changed. But so many things have changed in my recovery since just one year, like, smooth find improvements every year.
Bill 12:35
That’s my biggest issue is that the people who are just starting their journey, getting ill-informed about the long-term possibilities. And then they do tough, you know, for the first 12 and 24 months, wondering, you know, that’s it is that it, you know, and then probably losing hope. And that’s the point of the podcast is, I love it the most want to get people who are 10 years out, 15 years out, 20 years out, because then we can demonstrate the changes that have occurred in the recovery journey.
Bill 13:15
And that, you know, stroke recovery is not like breaking a leg, you don’t have a six-week recovery period, and then you’re back on your feet, a little bit of rehabilitation to get the muscles working again, and then you’re done. It’s unlikely that you know, six weeks in a stroke recovery is you know, 12 months in a stroke recovery. It’s just like you’ve broken your leg like it’s so early on in the journey. And a lot of things have to change and settle. And we can adapt and soak in the brain. And people just need to know that this is a long game, not a 12-month thing.
Chet Ciconne 13:57
There are so many factors too. Because like, I like you know, my recovery is not just a straight line, like, oh, now I’m better. Like, it was like, within a year I went back to work, but that was too early. And then I realized that had a regression, tried to switch careers, and got good physically, but I had never emotionally thought about anything that happened to me and PTSD came.
Chet Ciconne 14:29
And so then I you know, I’m going from like, Oh, I’m up here and my I’m like 70% better, you know, like, I think I’m better and then got worse than I ever was within my first year of recovery. I would have rather have like, you know, been back in the hospital because I was emotionally just depressed and had panic attacks every day. So like, what is recovery? You know, is it your physical recovery from stroke or is it how you feel just as a human like how happy you are like, you know, because sometimes you would trade depression for any of your physical ailments.
Bill 15:07
I’ve got a model that I’m working on to explain what recovery is. And it goes some way. But it’s a very high-level model, it doesn’t break down the details to the next level. But what it does is talk about emotional recovery, physical recovery, and mental recovery. And if you don’t do one of those three, you’re not going to get anywhere near being able to say that you’re recovered.
Bill 15:38
Now I’ve got left side deficits, I wake up in the morning, my left side needs to wake up a little, it takes a bit longer, when I’m tired, I get you know, I lose my balance. And when, when it’s hot, my left side plays up. And you know, it’s not as strong and has a little bit of spasticity in the muscles. So it hurts from time to time. And I still think I’m fully recovered. Because I’ve done the emotional work, I know that physically, my AVM has been removed, so it’s not going to bleed again.
Bill 16:18
And I’ve done the mental health work. So I’ve been in counseling, where I’ve attended to my emotions and my thoughts. And I’m doing the physical work as much as I can by going to the gym twice a week for an hour in total. And I’m just doing, you know, meeting better, I’m trying to sleep better. I don’t I don’t I don’t drink alcohol. You know, so I’ve done all these things.
Bill 16:44
And I’m at that point where I can when people say to me, how are you going with your health, I’m working, I fully recovered, but I don’t have great days, every day, there’s a lot of bad days still because of what I went through. And I just put them down to you know, like, now you’re going through a little bit of a cold, I just put down my stuff too. What’s the It’s like a cold, I’m having a bad day, the symptoms are worse.
Bill 17:09
And if I rest, and I eat, okay, and I don’t overdo it. I’ll be back to normal, I don’t know, whatever normal is now for me, you know, normal, my normal self again, in a couple of days. It’s a similar kind of experience. For people who don’t know what an AVM is. It’s an arteriovenous malformation. It’s a malformed blood vessel, it usually is described by doctors as being kind of like a Steel Wall. And because of the way that it, it’s formed in a really clear, tight curly pattern. Small, high bright, high blood pressure episodes, like, just from simple exertion, right chat, like from either playing sport.
Chet Ciconne 17:58
Or a video game, in my instance.
Bill 18:02
Getting overexcited can just cause it to pop blood vessels to pop because they’re tiny, they’re really little, they’re not massive so they’re a little weaker than normal as well, and they can pop and bleed. And the junk, the challenge is, is whether you can stop the bleeding or not. And in some cases they do. In some cases, they don’t. Some people have catastrophic bleeds, and they don’t make it, and other people do.
Bill 18:28
So you didn’t have high blood pressure, you didn’t have any of the regular fast symptoms. You know, you didn’t need to look after your supposed cholesterol levels and your blood sugar levels and all that kind of stuff. You were just the regular guy going about business and didn’t know about this thing that you were born with? And what’s weird is I hear about ATMs all the time, and they’re possible to have all over the body.
Chet Ciconne 18:56
Yeah, I have a friend with one in her hand.
Bill 19:02
Uhuh. Tell me about that. How would it affect her hand?
Chet Ciconne 19:06
I mean, she just has like, a finger that you can see this large vasculature running through it. And so that finger is, you know, less useful, but, uh, you know, I don’t know that she’s gone. Maybe you can interview her too about her whole journey of like, you know, they tried to embolize it, and then it’s failed, you know, I don’t know, I don’t imagine because, you know, AVMs are like one in 200,000 or something.
Chet Ciconne 19:39
And, most of them are in the brain as far as I know. So she’s even, you know, more rare, but we don’t you know, I talked to her almost every day, but we don’t talk about, you know, her hand so, I don’t know, you know, how much I’d be comfortable saying.
Bill 19:57
I hear you it’s not something they talk about.
Chet Ciconne 20:01
It’s more of like a physical ailment, you know, like a visual, probably thing you know, especially as a woman, you know, to have something visible on your hand. That’s, I would assume that’s most of her issues, but I don’t want to speak too much for so her.
Bill 20:18
Yeah, yeah. But it’s something different from other people’s strokes in that most strokes. 80% of strokes are ischemic strokes, blood clots, or something stopping blood flow in the brain. And then 20% are hemorrhagic strokes. And hemorrhagic strokes are caused by AVMs or they’re caused by.
Intro 20:43
If you’ve had a stroke, and you’re in recovery, you’ll know what a scary and confusing time it can be, you’re likely to have a lot of questions going through your mind. Like now, how long will it take to recover? Will I recover? What things should I avoid? In case I make matters worse, and doctors will explain things that, you’ve never had a stroke before, you probably don’t know what questions to ask.
Intro 21:07
If this is you, you may be missing out on doing things that could help speed up your recovery. If you’re finding yourself in that situation, stop worrying, and head to recoveryafterstroke.com where you can download a guide that will help you it’s called Seven Questions to Ask Your Doctor about your Stroke. These seven questions are the ones Bill wished he’d asked when he was recovering from a stroke, they’ll not only help you better understand your condition, they’ll help you take a more active role in your recovery. Head to the website now, recoveryafterstroke.com, and download the guide. It’s free.
X Rays can cause cavernous angioma
Bill 21:47
Because of the bulging the bulging of the blood vessel, the aneurysm, and then sometimes they’re caused by a cavernous angioma, which is a similar weird-shaped blood vessel. , You can have a cavernous angioma form later on in life. People aren’t necessarily born with it. And then what’s weird about the cabinet Sanjay is it can be brought on by X-rays. So there’s some evidence that some cavernous angiomas can be brought on and can form after people go through an x-ray, for some reason.
Bill 22:33
So there are too many ways. There are way too many ways. That’s what I found nearly after 290 episodes, check this out any ways that people can have a stroke? It’s ridiculous, right? It’s just Yeah. Intense. So you’re, you’ve spent the first seven days in the hospital, then you’ve woken up half your skull’s missing it’s in the freezer. You can’t feel your left side, and then how does the journey go after that? How did they finally kind of rehabilitate you enough to get you home? What does that look like?
Chet Ciconne 23:11
So I had a great doctor, because, you know, they gave me physical therapy. Maybe a physical therapist came in one time and, you know, tried to get me to move my left arm and whatnot, and see if I could move my fingers and move my left leg. And it was limited. And they’re trying to get me to walk and I couldn’t yet. And then I’d say within a week. I think I walked while I was still at the hospital.
Chet Ciconne 23:43
Maybe it’s it’s hard for me to remember but I got to a certain point where there was like, okay, he’s done, all they care about is can he survive? If he leaves here? It’s like, Sure, we’d love it if you could walk, but not necessary. It’s like, Can you breathe? Can you eat? Can you drink? And then can you walk would be great. And that’s all they care about. And that’s all the insurance companies care about.
Chet Ciconne 24:07
And so I was going to be discharged from the hospital very disabled, I would say. And my doctors like no, you know, we know we have scientific studies that show the more rehab you get early on, the better. So we want him to go to this acute rehab center. And so thankful to my doctor for that because I got sent to an inpatient rehab center, which was a huge upgrade in food to as a hospital food was terrible.
Chet Ciconne 24:44
I didn’t eat, you know, mostly I was on IV for a lot of the time. But once they were trying to get me to eat the food was terrible. But then I go to this inpatient rehab center, which is you know, everyday physical therapy, occupational therapy, use speech therapy, and good food. And I was there. So if my surgery was on the 17th, I just know I got, what I wanted, I had a girlfriend at the time, and I wanted to get discharged by her birthday, which was May 9.
Chet Ciconne 25:20
So when I went to the rehab, I’m not very sure I just know, the surgery was 17th and on May 9, I got out. But uh, so in between there, they transferred me and ambulance to this rehab center. And that’s where, you know, my rehabilitation started. And I don’t know about you. So do you know where in your brain your AVM was?
Bill 25:49
I don’t know that the lobe, it’s four centimeters, which is about one and a half, two inches, I think something like that from the ear, from my right ear near the cerebellum.
Bill 26:02
Like the back of your temporal lobe.
Chet Ciconne 26:10
Where I was going with this?
Bill 26:12
You were just about to tell me about where in your head the injury happened?
Chet Ciconne 26:21
Yeah, I don’t know. But so mine was in the parietal lobe, which is your main sensory, which contains your primary sensory cortex. And so the right side of my brain, sensory cortex. That’s the reason I can’t feel the entire left side of my body, right? And, oh, this is what I was gonna say.
Chet Ciconne 26:47
So people who have right hemisphere brain damage, oftentimes suffer from Anosognosia, which is where they’re not aware of their deficits. And so I was wondering if you experienced this at all, but I had it bad. Like, it’s kind of a superpower, depending on how bad your brain is damaged, because if you’re, if there’s a level, because, you know, if you have very severe damage, you can only recover so much, right?
Chet Ciconne 27:19
I was blessed to be at the hospital as quickly as I was. So I have a lot of room to recover. And so not being aware of a deficit, when you have a lot of room to recover, gives you this false sense of confidence, which I think allows for a little more recovery.
Chet Ciconne 27:38
But basically, what it was was like, I would think I was fine, and nothing was wrong, which is very dangerous. You can hurt yourself, because, you know, I couldn’t walk. But I was very drugged in the hospital and had to pee. So I just got up to go pee and just stepped right out of the bed and fell. And you know, could have killed myself.
Bill 27:58
I did the same thing. Day one.
Chet Ciconne 28:01
Yeah. And as probably probably a little bit of not being aware of do you have any other recollection of not being aware of your deficits?
Bill 28:10
Well, yeah, a few times. So when I woke up from surgery, they told me I needed to go to the toilet. To just do the regular movement thing, bowel movement thing, and all that stuff. So I said okay, no problem. So I stepped out of the bed on the left side, a big mistake, because my left leg was the one that wasn’t working.
Bill 28:28
And there was a nurse, I’m about six foot. Sorry, I’m about five foot 10, somewhere there and this nurse would have been four foot nothing. And she was really small and tiny framed. And she goes, I’m going to help you get there. And just lean on me is what she said. And I’m like, oh, okay, cool.
Bill 28:49
So I leaned on her fresh scar just stitched up literally hours earlier, and I’m on my ass in the ward outside of my bed, just screaming. Ahh, yeah. And I had no idea. But then I knew I knew what my deficits were. But then when I was at home, I did get up. So when I was at home just a little while after surgery, I’d say about maybe. So I was in surgery. November, late November. I got home just before Christmas. And then I was at home from about the 24th of December.
Navigating the deficits during AVM recovery

Bill 29:37
And I reckon it was in January, sitting on the couch, no one was at home. They’ve gone to work. Kids have gone to school when schools restarted and I’m having. I’m having lunch. I’m holding a little plate. And I just stand up and I gotta lean or go to stand up and lean on my left leg. And then the leg has just totally collapsed. And I’d fallen onto the couch smashed, didn’t break anything smashed my ribs onto the arm of the couch, fell over and broke the plate onto the concrete, we’ve got concrete floors.
Bill 30:12
So that was happening and there was a time when I needed to. Okay, I’m gonna get up off the couch, stand with my right leg, okay, and then now, okay, put your left leg out. Okay, make sure it’s touching the ground tap the ground a few times, and then stand up. And then make sure the knee’s operational and moving, and then move forward.
Chet Ciconne 30:39
That’s what’s the difference between you and going home. Right away after your surgery, I got to go to a rehab center where they taught me how to get out of bed. You were a little, probably a little more capable than I was.
Bill 30:55
I had a month in rehab, had a month in rehab, they got me back at my feet in a month. And they didn’t sort of say to me, your leg is that didn’t give me that feedback that didn’t say to me, you kind of need to tell you like, what’s happening and talk yourself through this process and don’t step up on your left leg that didn’t give me any of that info. I learned the hard way. But that’s ok.
Chet Ciconne 31:18
Yeah, see, I got the whole, like, it was probably really annoying to me at the time. But you know, they focus that I made sure I knew how to get up out of a bed and all this stuff. Where I had to practice that over and over and over. It was probably annoying but very necessary. But another interesting deficit that I had, which is common in the right hemisphere is left-side neglect. Did you experience that at all?
Bill 31:49
Neglect how?
Chet Ciconne 31:51
So I’ll just explain to you what it was for me. So basically, my brain completely disregarded things existing on the left side, okay. And so I’m in the rehab center, and they have me draw a clock. And I draw a clock. And it starts at 12. When it goes to six, and there’s nothing on the left side. I just don’t even draw the left side of the clock. But I don’t think there’s I don’t think there’s anything wrong. So I’m like there’s my clock. And it’s good, right?
Bill 32:24
I never had that. So even though you knew what a clock was before. And when you were a kid, you did all the numbers. And you know that.
Chet Ciconne 32:31
I still knew what a clock was. My brain just ignored the left side of the clock.
Bill 32:37
So you represent it. Half a clock.
Chet Ciconne 32:41
Yeah, and I’m solving word searches. And I find every word on the right side, I find no words on the left side. And, just every single aspect that you could imagine like I go to write a word. And I don’t write the first two letters, because it’s the left side of the word. So it’s just really like, it’s fascinating to me.
Bill 33:06
Are they saying Apple is missing A and P? And then are you going I can see that it’s missing it now, or you’re going I know it’s all good.
Chet Ciconne 33:17
I don’t remember well enough to answer that question. But I think mostly, a lot of what they were doing early on was confirming things. Because I’m actually in school right now to learn how to be a speech therapist, which was some of the therapy that I received in rehab, because that’s, that’s what I want to do.
Chet Ciconne 33:41
I want to work with brain injury folks and help them in their recovery process because I fell in love with the recovery process when I had to go through so um, but from what I gauge they were just kind of based on the location of my brain injury, they suspected certain things. So they would test for them to make sure that they are there.
Chet Ciconne 34:06
And then they say, Okay, we have to work on this later. So it wasn’t a lot of like, you know, things like that, that I was terrible at, it’s more like just draw the clock. I’m like, okay, is that good for you? And I’m like, yeah, they don’t say like, okay, no, what’s wrong, and like, you’re missing this and all that they just note it down, because they know, especially there is a lot of spontaneous recoveries, you know, in that first year, and that’s what you know, that’s where the one-year thing comes from.
Chet Ciconne 34:30
But they knew that by the end of therapy, I would maybe realize that I was missing these things. And they don’t want to, I think because I didn’t notice it. They didn’t get real with me, probably till a couple of days into this rehab. And I remember when the moment was when I realized that like, Oh, this is going to be longer than a few days. Because I you know, I just thought it was like, Oh, I’m gonna learn how to walk again. And then I’m gonna go back to work and it’s all gonna be good.
Chet Ciconne 34:59
But, I go into this room and my physical therapist, she has a deck of cards out on the table deck of playing cards, and they’re all face up. And she gives me a deck of cards. And she says, Alright, all you got to do is flip over the deck, flip over a card, and match it with its twin on the table. And I Oh, that’s so easy. Like, I’ll do, I’ll do with my left hand, even, you know, and I flipped over the card.
Chet Ciconne 35:28
And it took me a solid, like, four minutes to, I don’t know what card it was, was had picked a jack of hearts or something, I pull it out, and I’m just looking. And I cannot do it. Like my mental processing whatever it was, it was just impossible for me at that time. And I was like, wow, like, I felt stupid. You know, I felt terrified that this was going to be a permanent thing for me. And that was when I realized that, you know, I had a lot of work to do.
Bill 36:02
You know, with a feeling stupid thing? Is that just your insecurities coming up something that you’ve had from the past that have come up, because I’ll give you a little bit of an insight. I have these similar conversations with people and I don’t understand them on other episodes. And I don’t understand because I don’t experience them. So I’m just trying to understand them, right?
Bill 36:26
So it took me almost three years to get to brain surgery. So I had one bleed. I never once thought what if this happens again? And then it happened to Ken. And even after it happened again. And they told me it might happen again. I never once thought, what if this happens again? I just kind of went through it. And so okay, whatever. And then I assumed that it wasn’t going to happen.
Bill 36:48
And then when it happened, it’s like, Okay, I better do something about it. And then when I couldn’t do the exercises that they told me to do, I was just still thinking like, Wow, I can’t do that. And that was it. There was no you’re dumb, or you’re not intelligent anymore. I’ve never had any of those concerns at all, none. And then the other thing I didn’t do is kind of when I realized I couldn’t walk, but didn’t get worried about it.
Bill 37:20
By ashamed that was going to walk. And I just went about what I needed to do to get on my feet. And they gave me two months. They had booked me into their rehab facility for two months. I got out of there in a month. So it’s like, I didn’t I didn’t get the anxiety and the thoughts of all of the stuff that people worry about. I don’t know, maybe I hadn’t couldn’t worry like that. It’s weird. So I don’t know, what was behind your I’m feel stupid comment or thoughts about yourself.
Chet Ciconne 37:59
I think a lot of it was this Anosognosia thing where, you know, I was not aware of these deficits. Like, I just thought I was completely fine. And like I was going to be out of rehab in a couple of days, which is crazy. Like, I could not walk. I couldn’t, whatever that is reading, I don’t know, comprehending, playing cards. I don’t know what a real process that is.
Chet Ciconne 38:24
But I think it was just the first time that something broke through that lack of awareness. I was so unaware of my deficits, that something finally broke through it. And it just scared me. And, you know, I don’t know if it’s directly like an intelligence thing, but maybe also to just like, you know, because I was an engineer, I considered myself intelligent, or like, I valued that piece of me.
Chet Ciconne 38:54
So to like, see me fail at a task that I, you know, thought going in, oh, this is gonna be so easy and completely fail, especially, you know, as time goes on, you’re holding this card in your hand, it’s more and more time, like, you get embarrassed and then you start to think about oh, it’s taking so long, you’re not even focusing on your task. And also, it was like a, it was just an eye-opening thing.
Chet Ciconne 39:17
And I think that’s why she did it. Because I had so much confidence and I, you know, just as I was so confident she had to like to bring me down to earth a little bit and like really show me you know where I was. So probably just the length of it, you know? Because I think if anyone asked you, you know to match a card with another card, and you stood there for five minutes failing, you know, it would just kind of hit me.
Bill 39:45
I hear you might start feeling a little nervous or what have you, and I get that I get why people would like it, and I get why they would I don’t understand why I didn’t and I don’t know, maybe it was what you said. It’s just that you had the realization, I didn’t have the expectation. But I think I’m intelligent. But I didn’t expect my intelligence.
Bill 40:14
So my identity, this is what might be my identity didn’t cop abating when I couldn’t remember a word or fix this or fix that or answer this way to that. I didn’t identify as less intelligent because I couldn’t do this after brain surgery, but kind of associated brain surgery with messing up your head. And it’s like, oh, yeah, that’s what happens after brain surgery.
Chet Ciconne 40:39
Yeah, and see, maybe my, Anosognosia thing was just like, you know, I didn’t even have brain surgery. So like, you know, I’m fine. You know what I mean? Maybe I didn’t have that to relate to like a lack of intelligence or something. I just, I just think, Oh, I’m fine. But no, I’m stupid now. You know. So that’s why it’s so the, you know, the things like the left side, neglect, and the agnostic nosy are so fascinating.
Chet Ciconne 41:08
No matter how much you tell the person who’s going through at that time, they just can’t, the brain just doesn’t even compute it. So it’s like, and it’s just, I don’t know, it’s an amazing thing. Some people, you know, I was blessed. To slowly feel my left side and neglect disappear, I’d save six months was probably when I stopped noticing it.
Chet Ciconne 41:35
But because I had to actively like, turn my head. And like, actively make sure I look at left side paper, if I’m, if I’m trying to, you know, look at some information or whatever, you know, I had to just force myself to recognize the left side of the world for months. But luckily, it went away some people never went away.
Bill 41:55
Yeah, was that then more energy-consuming? So when I had to focus when my leg went, when I had to look at my leg and make sure that it was that the foot was landing correctly and my knee was in the right position, it would be exhausting. So did that become more exhausting having to make sure that you’re paying attention to your left side
Driving a vehicle after a stroke
Chet Ciconne 42:22
100% Still, even to this day. So another thing that your parietal lobe does in your brain is, that it’s in charge of proprioception, which is knowing where your limbs are in space, without looking, you can just feel it. And so for my left side, like I used to drive a manual stick shift vehicle.
Chet Ciconne 42:50
Once happened, and I got my license taken away. And then I tried to drive again, and I was like, Oh, let me see if I can drive a stick shift full, the clutch is pushed down with your left foot. Well, if you have no proprioception for your left foot, and you don’t know where it is, without looking, I couldn’t push in the clutch without looking, which is not, you know, safe for driving.
Bill 43:12
I had that experience. I’m doing, I’m doing what you guys would call 60 miles an hour, I’m doing 100 kilometers an hour on a freeway in a stick shift because we went to hire a car. And I told them, I wanted an automatic and they couldn’t get me one. So I had to drive a stick shift. And for me to drive a stick shift, I have to take my shoes off. So my left foot can have more feeling and know where the clutch is.
Bill 43:49
But even then I’m doing 100. So I’m probably in fourth. And I’m looking for a fifth. And I got to change gear, and I got to press the clutch and I press the brake instead. And try and crunch the gear at the same time. And then it’s it’s a disaster. It’s like oh my god, what am I doing? And then I’ve got to look down and put my foot on the clutch and then change gear. And then go again. It’s just Yeah.
Chet Ciconne 44:24
So like even on that note, like even today, or you know, current current day, not necessarily today, but uh my friends do like indoor rock climbing in the gym. And so I’ll go with them because I think it’s great, you know, therapy for me and it’s fun. But physically, I’m less tired from the climbing than I am like focusing on your left hand your left foot like that mental exercise I’m so exhausted mentally.
Chet Ciconne 44:57
Before I am physically not that I’m you know I’m still physically tired, I’m climbing, it’s hard. But the mental part is so much more exhausting for me, just because I have to focus on the left, I have to watch it. As I do each grab as I do each step with the left foot, otherwise, I’m gonna miss.
Bill 45:17
So what about walking next to somebody so I walk next to my wife from time to time, when we go to our or whatever. And I’m always bumping into her, it feels like there’s a magnetic force pulling me into her. And I’m always bumping into her. And she’s always going to stop bumping into me. And I’m not bumping into him just walking in or whatever. And a walk. When I’m walking next to somebody, it looks like I’m drunk I know what it is about when people are next to me, when they’re not next to me, I can walk perfectly straight.
Chet Ciconne 45:51
So definitely the girlfriend that I had at the time, I would always make her walk on my right side, just because we’d always want to like hold hands or whatever. And holding my left hand that I couldn’t feel was like, very creepy to me like, is a very strange sensation. So I always prefer just for people to walk on my right side in general. But as far as walking goes, I think I’m very, you know, acceptable. Like, I can feel a slight difference than you know, before my stroke, but I think most people would not notice.
Chet Ciconne 46:34
And it’s kind of like a warm-up thing, like you said, when you wake up your left leg needs to warm up. It’s not just right away. So my first few steps every day are probably a little weird. I’d say the bigger thing is one of the biggest struggles of the left side, neglect was always running into things on the left side of me because my brain was not even acknowledging them existed. And it was like the left side of my vision was off. So I was always bumping into things.
Chet Ciconne 47:05
And even though that left side, neglect is gone, just the lack of proprioception on my left side, I still, I just went on a snowboarding trip this last few days, and I stubbed my toe there we had a cabin. And the fireplace had this stone base to it that kind of extended out. And I think it’s so nobody puts anything in front of the fireplace, and I stubbed my toe on that thing my left toe like three times.
Chet Ciconne 47:33
So that’s painful. So I think balance-wise, obviously I was you know, it was my first time snowboarding, I was able to figure that out. So obviously, you know, I have some level of balance. But I think walking passes as normal to the naked eye can feel slight differences, but nothing I would bother complaining about. Mine’s more like, the proprioception is still an issue and I bump into things and I stub my toe and I kick things with my left foot or trip over things with my left foot.
AVM Recovery effects and driving limitations
Bill 48:05
Yeah, same me doorways, when I’m really tired. I seem to not notice doorways and just my left shoulder. Also just bumps into them. And then, and then my wife’s not allowed to touch my hand when I’m driving. So we drive on the opposite side here.
Bill 48:26
Yeah, and I put my hand on it’s an automatic car now so but sometimes the rest of my hand on the shift on the shifter, and then should just be climbed or sweet. And she just laid her hand on my hand. And it’s like, why touch my hand for it? Don’t touch. Something uncomfortable about it, right? It hurts, it bloody hurts.
Chet Ciconne 48:48
It hurts.
Bill 48:49
If you’re going to touch it, touch it hard, but be rough with it. Don’t just be gentle with it. God’s sake woman. And it’s been eight years since my surgery. No 10 years since my surgery this year hasn’t changed. But she hasn’t learned yet. She’s still gentle and nice. And I’m still an idiot. She still does. Being gentle and nice with me. And I still overreact. But I can’t not. I don’t know. It just messes with my entire being it’s the most age-inappropriate response to something so nice and gentle. And I don’t know how to I don’t know how to not do it.
Chet Ciconne 49:28
Something creepy about it. I don’t know. I always call it my ghost arm. Yeah. And it was just like, I don’t know, it’s just I feel it. Maybe it’s just a reminder of your stroke. And that’s all it is. It’s like you have this weird sensation. And it’s just oh, I had a stroke and it just reminds you of it and it’s just annoying. I don’t know.
Bill 49:48
One of the things I used to do was chat rooms to tell me if this happened so I used to wear glasses until the age of 40. This happened to me started happening to me at 37 the reason I don’t wear glasses days because I had cataract surgery, and I removed the cataract, and I don’t need glasses, but I wore glasses from the age of five. So after brain surgery, I still had, it because it was so close to my eye surgery.
Bill 50:20
Only six months, maybe nine months difference, right, I had eye surgery. And then later on, I needed brain surgery. Because I studied for six or nine months, I still had the sensation that the glasses on my nose had slid forward. And I used to slide them back up with my left hand. But no, there were no glasses there anymore. But I still had the habit of just lifting something that wasn’t their backup. And because the glasses weren’t there, I poked myself in the left eye.
Chet Ciconne 50:52
Oh my gosh. So I didn’t start wearing glasses. So when I had my brain surgery, they immediately suspended my driver’s license in America, at least for a year. And then this kind of segues into another part. But like a year, after my surgery, I’m like, alright, let me try to get my license back. But around the same time, I ended up having my first seizure.
Chet Ciconne 51:25
So because of my brain surgery or scar tissue on my brain, I’m more susceptible to seizures. They put me on medication. I didn’t like how the medication made me feel. So I stopped taking the medication and I had a seizure. But uh, but back to the glasses thing. I didn’t have to get glasses until I wanted to get my license back. I’m gonna like okay, well, let’s check your vision.
Chet Ciconne 51:52
And then like, now, this isn’t good enough, you need glasses. So I was like, Okay, I have to get glasses. So I didn’t wear glasses ever until after my stroke. The stroke was in 2016. I didn’t get my license back in 2021. So that was when I started wearing glasses. Right? But I do even, always use my right hand to pick my glasses up. And when I’m not wearing my glasses, I’ll find myself going to do that when there’s no glasses there. So I relate to you on that. But different situation, because I don’t use the left hand. I’ve never poked myself in the iron. Man.
Bill 52:31
It’s so annoying. I did it so many times. What’s interesting is that nobody took my license away. I had brain surgery. I had three brain hemorrhages. Nobody took my license away. I went straight.
Chet Ciconne 52:46
Yeah, that’s why I said in America because I don’t know. And I don’t know. Also, like I said, I had a great doctor. I’m very happy he did it. Definitely should not have been driving. And I probably would have tried to just because of my confidence and lack of awareness. But uh, yeah, I don’t know what it is. But in America, if you have brain surgery, or if you have a seizure, they are the doctor is required by law to send that to our DMV, which is in charge of our licenses and stuff. And they are supposed to put your license on hold for a year. And then you get reevaluated and try to get your privilege back.
Bill 53:34
I was told not to drive but they didn’t give me a time limit that didn’t say Don’t try for the next 12 months or whatever. Yeah, something like that. Okay, no worries. So, I drove. I came out of surgery, end of out of the hospital, I got home like I said that December, 24th. And then a month later, literally a month later, four weeks later, I was driving I did a five-hour trip to see a friend of mine who lives quite far away from where I live.
Bill 54:09
And I still couldn’t feel my left side properly and turning the steering wheel with my left side was not fun because I had to again make sure that my hand was holding the steering wheel and wasn’t going to slip out and all that kind of stuff. And I was so fatigued when I got there. I shouldn’t have done it. But I was so fatigued when I got there. I couldn’t believe how wasted I was.
Bill 54:33
And then I had to drive back two days later. And I didn’t tell anybody that it was a problem. But I shouldn’t have done it. Like I would I would not have wanted to be in a situation where I did something, caused a collision, and then injured myself or somebody else. You know, it’s so wrong. But again, I didn’t think because nobody said don’t drive you’re not allowed to drive without taking a license. I didn’t think I shouldn’t be driving. I thought, yeah, I’ll be fine.
Chet Ciconne living with half a skull

Chet Ciconne 55:07
I mean, there’s also another, I’m sure there are people who have had strokes and in America and they, you know, I had, I was missing half of my skull I had to wear a helmet just to walk. So, probably not a good idea to be driving a car, you know, an accident would be fatal for sure.
Bill 55:28
Yep. I’m gonna ask a few questions. I don’t have to answer them straightaway all at once. Okay, so the question is how long we live without half your skull. But then were you alright with living with half a skull? Because on your Instagram, you’ve got some awesome images there of how you’ve compared yourself to a mountain.
Chet Ciconne 55:57
Sort of like the North. I don’t know if it is, I just went to Yosemite for the first time. But there’s a clothing brand and an outerwear brand called The North Face. And their symbol. Is that a little mountain? Yeah, that’s definitely when I went there. I was like, that kind of looks like me.
Bill 56:26
And it does Man. You guys could have been twins. How did you live with that? Emotionally? Mentally? Like, what was that like? That’s an interesting thing to be missing half your brain for some time.
Chet Ciconne 56:45
You know, I just woke up, there’s no decision to be made. I just woke up. And that was my life. So when you wake up, and somebody says, you know, oh, you almost died. But they could have your school off. And so now and now you’re not dead? You don’t say, Oh, what did they do that for? You know, like, why did they take half my school? I think I was just, you know, happy to still be around.
Chet Ciconne 57:10
And, and it looked funny. I’ve always enjoyed humor and been able to, I always appreciate it when people make fun of me, I don’t get upset at it. I laugh It’s not a good joke, I might get upset. But if it’s a good joke of power, laugh at my own expense. Anytime, right? And so, you know, as far as appearance wise, they said, they put it back later. And I believed in their ability to make me look normal.
Chet Ciconne 57:43
Again I feel like I look amazing for what I’ve been through. Yeah, most people would never know. I won’t have this hair for many more decades. But I think for 10 more years, I’ll be able to hide the scar that’s under there. Because it’s a pretty gnarly scar. And there’s no hair growing on the scar.
Chet Ciconne 58:01
So I have a little like, racing stripe in my hairline. But so as far as like, appearance goes, I was confident that they would put it back and I’d be passable. The bigger issues were just like sleep. So, you know, I had no skull, all of this was just skin the hair that they left, and then if you touched you’d feel my brain under there. And it was most of my head.
Bill 58:35
Did you ever go for the touch?
Chet Ciconne 58:36
I did. Yeah, of course. I was curious I had to ask other people like, please be gentle. But add you want to touch my brain. And you know, some people did and most people were not interested. But it’s a you know, it’s a unique situation I had my doctor take cellphone pictures inside my head when they were putting it back in. So I had cell phone pictures.
Chet Ciconne 59:03
The first one kind of looks like a chicken cutlet. So there’s a, you have a membrane around your brain called the dura mater. And obviously, they have to cut through that if they’re going to get to your brain. And if they cut through that, that means they have to replace it with something.
Chet Ciconne 59:19
So they replace it with a synthetic one. And so he has a picture, they put that in place, we took a picture. Then they put my they call it a bone flap, which is the piece of school that was in the freezer, they put that back in, they screw it back together with these brackets and screws. And he took a picture of that. So I have a literal picture inside of my head of my school, which is super rare. You know, nobody has that.
Bill 59:48
I wanted something like that. And nobody did it for me.
Chet Ciconne 59:53
The best you get is an MRI or something right now I have literal cell phone photographs of the inside. In my head, but yeah, so it’s just scalp, hair, and then brain. So I can’t lay on my right side at all, I can’t even like couldn’t even lay on my back. Because it just felt weird. I had to sleep on my left side, from April 17 the day of the surgery until I think it was October 19.
Chet Ciconne 1:00:24
They put it back in. So that whole period, I have to sleep on my left side, my left side is already spastic, yeah, because I’ve had a stroke, there’s already tightness, and you know, just all kinds of things you’re dealing with, and I have to sleep on the same shoulder. So I had to figure out, you know, eventually, excuse me, I got a, like a wedge pillow in my bed.
Chet Ciconne 1:00:49
And that way I could kind of like sleep, not on my head, you know, kind of rest more on my shoulders, and I use like a neck pillow, and the wedge and that allowed me to sleep on my back. But I just had to sleep on my left side for so long that I had so much shoulder pain and tightness. From who knows if it’s from the sleeping or just the stroke, you know, many people just have so much best spasticity anyways, yeah. So I’d say that was the biggest issue I had with it.
Chet Ciconne 1:01:18
Otherwise, it was like just a wild experience that I was able to make light of, and I enjoyed taking the funny pictures. And you know, they saw, when they’re going to give you life-saving surgery, and you’re flatline. They’re not like, oh, let’s give him like a nice haircut, they just shave off, you know, and then they saw your head, like, so I had a funny, you know, half my head haircut.
Chet Ciconne 1:01:45
So, I had a cousin who does hair, and she kind of gave me a mohawk to balance it out or whatever. So, you know, I just You just make the best of it kind of thing that didn’t break my spirits you know, I think for a woman, you know, too, that would be such a more traumatic experience because I think just hair means so much more to them and to have half your hair cut off. And then just, you know, the way physical appearance is, you know, forced on them to matter more than that as ugly guys. We can live with it a little longer.
Bill 1:02:21
We can live with being uglier, even more than we already are. Yeah, I hear you. It’s fascinating to see that image of you and the way your head looks, I have a coaching client who is currently in that state. And then, you know, it’s really, he’s trying to get to the point where it’s not in that state.
Bill 1:02:53
And what we’re working on is we’re working on, because he’s not compliant, you know, maybe it’s part of his personality, maybe it’s part of the stroke, don’t compliant with what the doctor’s requests are. So the aim is to try and get him to feel like what he needs to do if you want to get your skull back, is what you need to do all the right things so that you can create the right environment for your brain to stop swelling and for the skull to go back. So you know, we we’ve, yeah, we’ve been working on that all let’s get your skull back on your head.
Chet Ciconne 1:03:32
I don’t feel like, you know, my doctors put the onus on me. It was just like, oh, you know, I was eager I was I was like, Hey, can we do it yet? And like, I know this enough. But it wasn’t like, oh, the swelling is not down enough. Because you haven’t done XYZ is just like, Oh, you just have to wait more time.
Bill 1:03:52
He was drinking.
Chet Ciconne 1:03:54
That’s probably why See, I didn’t even think I had my first drink when I was like, 24. So I was never, I was never a big drinker anyways, and then so this happened. So it was really easy for me to be like, Oh, I’m not gonna do that anymore. So same, but I can see so if he’s if he’s making bad decisions that are still causing his brain to swell and yeah, that makes sense.
Bill 1:04:17
Yeah, bad decisions in hindsight, but still more just living the way he always lived. That’s all it’s just that I’ve always had a drink or I’ll have I’ll have a drink. That’s all you know.
Chet Ciconne 1:04:31
I don’t know if he experiences this but another interesting thing about that situation is you don’t realize how much and it makes a ton of sense but just having a complete seal on everything. Keeps the pressure inside of your head normal. So like when I was missing if I bent over to tie my shoe or to pick something up Everything would shift in there very quickly.
Chet Ciconne 1:05:02
And I would get a sharp, terrible headache almost immediately. And I was like, Is this just my life forever? But no, as soon as they put that thing back on, you know, I’m able to bend over and tilt my head. And there’s not this dramatic shift. And maybe it was like a quick movement of the brain. I don’t know what it was. But just the worst headache, or not the worst headache I had experienced, but very painful headaches. And so just getting that kind of equilibrium back together, got rid of those headaches. And that was huge for me.
Bill 1:05:38
I find it very interesting to learn that your brain is missing its skull, and then the dura has been impacted. Where does their cerebrospinal fluid go? Like? Does it leak out? Literally? Are they then able to contain it?
Chet Ciconne 1:05:56
So there’s so I’m going to piss off my neuroanatomy teacher. So I’ve taken I mean, I’m in school to be a speech-language pathologist, speech therapist, depending on what you call it. And so I’ve taken a couple of neuroanatomy classes, but there’s the dura is not where the spinal fluid goes. It’s the layer below that, which it’s the dura mater. And then the arachnoid monitor. The arachnoid mater has legs like spider Wade connections, and that’s like a spongy space that has, you know, gaps for the spinal fluid to go through.
Bill 1:06:45
Uh-huh.
Chet Ciconne 1:06:46
But, uh, I mean, I’d imagine they had to cut through that in mind, too. So I still to answer your question. I’m not, I’m not exactly sure. What would happen to it? But, uh,
Bill 1:06:59
I perhaps incorrectly assume that anytime I’ve seen a brain specimen, it’s been in a jar or something like that. So it’s, you know, surrounded with a fluid to keep it intact. And I imagined that the cerebrospinal fluid was fluid, like, in that kind of way. You know, that it seemed liquidy and you could see it gushing or losing or whatever, but perhaps it’s not specifically in that way. And I do recall hearing, you know, people having subarachnoid hemorrhages, and then subdural hemorrhages so that the different spaces,
Chet Ciconne 1:07:40
yeah, there are three different membranes, depending on where your bleed is, given those categories.
Bill 1:07:48
So the arachnoid layer might be the layer that kind of contains all of the cerebrospinal fluid. Yeah, that goes through a system rather than physically. Allowing the brain to float in it. Correct?
Chet Ciconne 1:08:06
Yeah. It’s like, yeah. Oh, no, I don’t want to. Let’s see. We’ll get somebody man.
Bill 1:08:13
Yeah, that’s all right. I mean, that’s just us just trying to work it out. I get Yeah, that’s cool. So no, severe loss of brain fluid that they have to refill or anything like that. We just call it the whole thing is just fascinating. The fact that you’re here, and I’m talking to you the fact that the process that you went through was so perfect. 45 minutes in the hospital, immediate, being able to diagnose it immediately, and then action to get that sorted. And then amazing. Doctors, technology, science,
Chet Ciconne 1:08:55
how many how many years ago? Does this happen? And they don’t know how to remove your school and put it back in like, how many years ago? Do they just say? Oh, well, sorry, check goodbye.
Bill 1:09:06
Yeah. I don’t think it was that many years ago, man in our lifetimes, for sure. I think. I think in our lifetime, you know, for sure. It’s just crazy. I love your sense of humor, though. Not only do you see similarities between between you and the north face of potentially El Capitan, but also there’s a CIT GPT. That’s pretty cool. There’s Netflix.
Chet Ciconne 1:09:37
That’s what that was in the deepness of, you know, no job. No school recovery. What do you do you just make let’s make a Netflix logo. Be creative.
Bill 1:09:49
So I’d encourage people to go to your Instagram and check it out. I’m gonna have links to your instinct for people to reach out if they need to. As we wrap up ask three questions, what was the hardest thing about a stroke for you?
Chet Ciconne 1:10:08
I would say, the mental health aspect of it. You know, when I look at my recovery, I see a great physical recovery. And then a huge mental health dip. As I had to process everything that happened to me that, you know, early on, it felt like a video game, it was like, Oh, I just have to learn how to reuse my left side, like, this is kind of fun. You know, I gotta figure out how to do things differently. This is cool. And then once you kind of plateau, your physical recovery for a while, obviously, I still improved after that. But once I hit that plateau, then everything emotional hit me. And it was tough. You know, just very just panic attacks every single day, you know? seizures, the epilepsy. That was, I’d say a seizure is almost scarier than the stroke was. There’s a level of like, aloofness that comes with the stroke, where you’re not, you know your brain is not working 100%. So you’re not aware of what’s going on in a seizure, like, oh, I, I get an aura where I sense it’s coming. And that’s terrifying. And then the initial, you know, electricity that’s going through your brain that you’re still conscious for, is terrifying. And then the idea of having a seizure, and in the wrong timing, you know, swimming or driving is terrifying. So, that just led to a lot of anxiety, which went along with depression. And then like, what am I going to do? Like, the job I used to work was driving, and I couldn’t drive, I didn’t drive for five years. So what am I going to do with my life? Am I ever going to make money again? Am I just going to be disabled my whole life, that whole just mental health? And identity? Who am I? What can I do in this world still, that was the hardest part of the stroke. And I think it took me a whole, I’d say five years, to just get over the mental aspect of it and to feel like, okay, I’m still myself, I’ve evolved, there’s a new version of me. And but I’m okay with it, I love this new version of me and I have, if I don’t accomplish another thing in my life, I’m still happy to just be here. And, you know, I kind of had to let go of the timelines that you create in your mind. And like, this is all the things that I’m going to do in my life. And like, so this is my idea of success, I had to reach a point where I had to let all of that go. Because it was giving me so much anxiety because it just wasn’t realistic anymore with the stroke. But I you know, that I’ll probably end up surpassing all those original ideas, that I considered were successful with the new direction that I picked. And my new goals, I’ll be, I assume I’ll be even happier. So just that mental hurdle, and redefining myself is just so difficult.
AVM recovery and career path evolution
Bill 1:13:31
I love what you said about you’ll probably surpass all your previous ideas of what success looked like. And that’s so true, man because I’ve done that. And I’m continuing to do that. You know, I might not be a novelist or a literary master. But, you know, the guy before stroke. Did you buy the book? Yeah. Yeah, the guy before the stroke doesn’t write this book like that guy.
Bill 1:14:05
He doesn’t have any clue what it’s like to write a book, you know, and to have a four-year project because there’s a four-year project but mitigated done was the stroke brain, and my inability to understand how to put words together on a page and then make a cohesive and then turn it into something useful. That wasn’t that didn’t happen.
Bill 1:14:31
I had goals and ideas and thoughts of what success was, and it was all around money, how much money I was gonna make how big my house was going to be whether it had a pool, and what brand of car I had, and all that junk, you know, and being able to get over that. And then being able to focus on what I loved, and do the things that I desired rather than the things that my head was telling me to do.
Bill 1:14:58
It was kind of like a real relief. The stroke led to that as it gave me the chance to do these things that I never would have been, and would have allowed myself to do before because I had preconceived ideas of who wrote books and who read books. And I wasn’t that guy, I didn’t identify as that guy. And it’s so cool that you said that, I love it because you will, you’ll surpass all your goals. I know my nice as a result of, I’m going to take some credit for this as a result of what happened to me.
Bill 1:15:39
She’s gone into speech therapy. Awesome. Her granddad also had a stroke. And in her first week, I think it was in her first week of work experience when she finished her degree. And then she had to do a placement or whatever it’s called. She’s gone in, and there’s a kid who has been in speech therapy for five years. He’s five or six years old by now. And he hasn’t progressed too far. And she says to the mum, has anyone ever done a mouth check? Have they ever checked the child’s mouth to see what’s going on inside his mouth?
Bill 1:16:18
And she said, No. Why? And she said, Well, sometimes, you know what, just check the mouth to make sure that everything is correctly abnormality. Yeah. And she said, Can I check his mouth, she goes, Yeah, checks the child’s mouth. And immediately notices notices, an abnormality in the child’s mouth.
Bill 1:16:39
So everybody is trying to work to support this kid, and not giving the kid all of the tools, and then also judging that kid on his lack of ability to improve and questioning his intelligence and a questioning all these things. They all missed the very first step in assessment, which is to open the child’s mouth and have a look inside. Yeah. And she has been able to do that, for the first time she’s ever come across a live patient with her first opportunity.
Chet Ciconne 1:17:22
Sad that that opportunity was there but great that she got to be the one. Yeah, unfortunately, nobody thought of that for five, or six years. But awesome for her to, you know, do the right thing.
Bill 1:17:35
It’s credit for her all credit to her, but I’m taking some of that credit, too. You know, we’ve spoken about her career, was spoken about all these things, she interacts with me a lot about aphasia and other things related to stroke, and that we have this great thing. And I never wouldn’t have been an adult would have been able to hold a conversation like that. With a human that was working in that space. If I hadn’t been through what I’d been through, I knew how to paint a wall and make your house look good.
Bill 1:18:04
But that kind of gets old, you know, like, who cares, your house has got a painted wall on it. And it was painted before it was just a different color. And it was I didn’t achieve much it just changed the color in your house. That was kind of that’s kind of how it’s grown for me, like how I’ve evolved and become this version of myself that I cannot recognize. So I look forward to finding out where your path ends, where it ends, or where it goes.
Bill 1:18:33
Because it’s not going to end in just the next thing that you do. It’s going to make a massive difference and your insight as a stroke survivor, when you’re working with people with aphasia or another speech disorder, that’s going to just make you such a better therapist. Because, yeah, so acknowledge.
Chet Ciconne 1:18:55
Ultimately, I just, it’s like, you know, what I was doing before was like, went to college and had no idea what I wanted to do. And I was like, well, I’ll pick engineering because that’ll get you a job. And that’ll make it not a waste of time. But I had no connection to it, or like, I didn’t enjoy it, like, you know, sure it was a job that paid. But then, you know, I have a stroke.
Chet Ciconne 1:19:20
And I’m interested to use to speech therapy, and I’m interested in it. And I’m very interested in just brain injuries and the community. And I’m like realizing, Oh, this is a career path where like, you know, maybe I don’t make as much money even though it pays well. But you know, my old goals of the engineering where I didn’t care about it, I was just in it because it made money like oh, now I’m like able to make money and do stuff that I find fascinating.
Chet Ciconne 1:19:47
And that will be rewarding like I can help someone else on the journey that I went through. I can interact with them, like very early on in that journey, or maybe later depending on you know, where we meet, and Who knows, I could have that one little thing like your cousin did? Oh, did you think about this? Have you, you know, have you thought about how you sleep or what you’re eating, you know, all the things that I had to learn to feel normal again?
Chet Ciconne 1:20:14
I can give them one little nugget of information that might revamp the recovery process. So that’s definitely why I think stroke is the best thing that happened to me because I feel like it gave me an actual purpose. In, my career, I feel like as a man, you know, the purpose and the way you make money, or whatever is so important to your happiness. And the fact that I was just kind of mailing it in and just doing whatever because it would pay me I’m so much happier to be on a path where I feel like I’m doing something that I care about, and can also pay me.
Bill 1:20:56
In the book in the acknowledgments, there’s an acknowledgment, you read it at the end, it’s to Louise Gilbert, a friend of mine. And before she was a friend of mine, she was a coach. So I was a life coach. So I decided that very early on in my recovery, I was gonna get life coaching, counseling, like everything, I threw everything at this. And she, of everyone who knows me, and Louise knows that I could say this about her, quite comfortably.
Bill 1:21:29
And she, the bitch made me stop drinking sodas. If I didn’t stop drinking sodas, she would not work with me. And I’m like, what do you mean, I’m coming here to get your services I’m paying you. That should be, that’s when we’re not. You know, there shouldn’t be anymore. She goes. If you don’t stop drinking sodas, I can’t work with you. That’s it. And I’m like, What are you talking about woman?
Bill 1:21:59
You know, anyhow, I just kind of said, All right, I didn’t believe that I was going to stop. I told her I would, but I didn’t believe I would. And I was just going to go back to session one, and we’re going to get kick it off from there. But sure enough, that thing that she said to me made me stop drinking sodas. And that was after my brain surgery. Sorry. And that was after the second bleed.
Bill 1:22:27
And that one decision to stop drinking sodas then made it possible for me to take all the other changes and apply them to my nutrition. Stop. Stop smoking, stop drinking, stop eating sugar, stop drinking caffeine, stop eating dairy to an extent. Because I’m great. I have to eat cheese a bit. And that was what snowballed into me improving my health and well-being while I was healthier 37 than I had been, you know, for decades.
Bill 1:23:07
And when I look back at the the key moments in my recovery, that was one of the key moments, just that what you said that one little decision that seemed ridiculously unnecessary. That snowballed and became this other thing where now, if somebody says to me, let’s go to dinner, and there’s pasta on the menu, I won’t eat pasta. I don’t know when the last time was that I ate pasta because it puts me into a food coma almost immediately. I can’t cope with it.
Chet Ciconne 1:23:44
A food coma for a stroke survivor is a completely different feeling, like the level of brain fog. Yeah, and just like you’re useless for hours until you digest this stuff you’re mentally just you’re there but you’re not wiped out. Yes, yeah.
Lessons Chet Ciconne learned from the stroke
Bill 1:24:04
So I love that. Your next question is what a stroke taught you
Chet Ciconne 1:24:17
so much, means so much I spent so. So long, unable to work. Just trying to figure out my seizure meds and trying to figure out my health and the general trend of stroke broke my sleep. It broke my ability to enjoy food. It broke my confidence it broke some friendships, relationships, you know, you find out who’s there even if you’re not available all that Um, and so I had to figure all of those things out. And for the most part, you know, by yourself, you have to, people can tell you certain things.
Chet Ciconne 1:25:12
And, for me, at least I know that like, no matter how many times somebody tells me something, it might even be the right thing. I’m not going to learn it until I learn it the hard way, myself. And so just all of those things like, how to eat in a way that I can still function properly. poststroke what I need to sleep I’ve learned who my real friends are, and the people and the relationships that are important to me, who I am, and what I want to do with my life.
Chet Ciconne 1:25:48
Stroke taught me, you know, it’s changed my career direction. Just so much there’s I can, I can hardly name things I’ve learned that stroke didn’t teach me like, honestly, the things I like as an adult in. And like the most meaningful things in life to me, I feel like all came from a stroke. Like, my life completely changed. And I feel like so much of it is for the better. So that’s a tough question to answer.
A message from Chet Ciconne

Bill 1:26:21
You answered it. Well, thank you, man. And then finally, what do you want to tell other people who are very early on in this journey? And listening to this podcast? Maybe it’s the first one they’ve listened to in the curious, what do you want to tell them?
Chet Ciconne 1:26:37
Yeah, if you’re in the recovery process. Figure out what works for you, it’s not going to be the same for everybody. That’s, that’s the main thing. All of these brain injuries are so different. And it’s great. Which I’m sure you’ve seen, like, interviewed so many people now. And you see similarities and the doctor sees similarities. And it’s like, oh, you have a right side things, you’re going to experience this or Oh, it’s the left side bleed or strokes. You’ll experience this. But it’s not always the same.
Chet Ciconne 1:27:11
And so you just got to figure out what works for you what worked with the big main thing that worked for me, I’d say two things. hydration. I put, I put it number one, it’s very close. It’s close between one and two. But I’d say hydration like I wake up and I drink 40 ounces of water. First thing in the morning, before I do anything else. I also have to take seizure medication, so they owe any medication. Hydration is important. But I feel like my recovery started to turn around when I started to drink more water. I don’t know. Can’t explain why, but uh, give it a try.
Bill 1:27:59
Are we 80% or 90% water?
Chet Ciconne 1:28:01
Something like that who knows, I’ve forgotten it plenty of times. But we’re, you know, your brain needs a lot of water to function. If you’re struggling at all, and you don’t drink a lot of water. Or you drink a lot of soda, replace the soda with water, and do whatever you can. Try drinking more water, and see if that helps you. The second thing is sleep. Like you have to figure out your sleep.
Chet Ciconne 1:28:27
If you’re struggling with your sleep at all. Your recovery is going to slow down so much so try different things. What worked for me was you know, I was very sensitive to everything like sound. temperature, the temperature still. I don’t enjoy the heat. I used to love the heat. I used to be a beach person. I love summertime, I could go to the beach. It’s 100 degrees.
Chet Ciconne 1:28:54
Who cares? I can’t do that anymore. I have you know a personal fan. I keep one of these on me in the summertime. So this is part of the advice, right? Like the pizza thing. Find a little mocha or a little pocket fan that you can keep with you. And you’re too hot you know, deal with it. Figure it out, get cooler but yes, sleep is temperature the thing and you need a fan because you’re too hot, which was my problem.
Chet Ciconne 1:29:25
I could not sleep I was too hot. I had to turn off every light I had to put a sticker over every little blinking light on any device in the room. I wore an eye mask what else did I do oh sound was annoying for me every little sound you know you go to a restaurant I used to be able to focus on just the person talking to me. Not the case anymore. I hear every conversation I hear every fork hitting every plate everywhere in the whole building.
Chet Ciconne 1:29:58
So I had to buy a noise machine, I bought a noise machine and I researched you know, white noise like the staticky noise from the TV. So there’s white noise, there’s brown noise, there’s pink noise. And we have different stages of sleep. When we go to sleep, there’s the deep sleep cycle, which is very important, and then there’s the REM sleep, the sleep cycle where you’re dreaming.
Chet Ciconne 1:30:21
And that’s kind of where your brain cleanses itself and where you remember things and learn things that you learn throughout the day. So apparently, I might have this switched out, but pink noise and brown noise, I think brown noise is probably deep sleep and pink noise is maybe REM sleep. But, uh, those noise, those noise frequencies while you sleep can help promote those different sleep states.
Chet Ciconne 1:30:50
And I found that pink noise on a noise machine when I sleep gave me the best sleep. And so once I cut out these little light distractions, and once I cut out noise distractions, and once I got the temperature, I have a, I had a mattress topper that is filled with water, and circulates water at any temperature that I want it. So in the summertime, I set it to like 50 degrees in the wintertime if I’m too cold, which is very rare.
Chet Ciconne 1:31:19
But if I’m too cold in the winter, I’ll put it up to like 80 degrees. But that keeps me at a comfortable temperature the entire night, I have a sound machine which is blocking out all the distractive noise, and I have all the lights figured out in my room. I don’t use bright lights, I use warmer lights, my my lights are remote-controlled, and I can change the color of my lights.
Chet Ciconne 1:31:42
So those are the two things that I think help the most with me figuring out my sleep, which is complicated. Like I said, there are a lot of aspects to it. And then water. I don’t already I don’t drink I’m not a big drinker. But uh, I would just focus on hydration and sleep. If you’re struggling at all, in your recovery, focus on those two things first. And I think that’s a great base. And it’s going to help you with everything else. But it’s hard to learn new things if you’re not sleeping, right? And it’s hard to function if you’re not hydrated.
Bill 1:32:17
Hard to solve problems, hard to get tasks done the following day. And it’s cumulative every day that you don’t get good sleep, it impacts the next day and so on. So you want to sort that out. There’s a chapter in the book about sleep and it talks up there yet. Yeah, talks about the stuff that you spoke about a lot about that stuff. And it’s a book designed to kind of give people just a small insight into the important things that help and then hopefully they get curious about one of those, and then go down that journey.
Bill 1:32:53
But sleep was one of the things that I got curious about. But I’ve got to say, I didn’t go to the path of getting a floating water bid in. I love the way your engineering brain has taken this to the next level. That sounds fantastic. And if you can share, not if you can, I’ll make you share, share the link to that product, and then I’ll put it in the show notes. And if anyone’s interested they can.
Chet Ciconne 1:33:23
It’s very, it’s very pricey. So I’ll give you a couple of options. I also there’s a blanket that I love, which is just it’s like a fabric that was designed by NASA that absorb heat. And so it feels cold when you put it on. It’s like it has silver in it or something right? And so that’s a much cheaper alternative. I’ll give you both because the water thing is like 1000 books, you know, I now understand not everybody has that.
Chet Ciconne 1:33:49
Especially a stroke survivor, maybe you’re not working as much as you used to whatever it is. So if you can afford the high-end, go for it. Otherwise also gives you this little cheaper blanket option. But when I travel, I’ll take that blanket with me because I don’t want to lug around a whole mattress topper and a little box with water in it.
Bill 1:34:08
Okay, all right. I hear. Well Chet, thank you so much for being on the podcast. Appreciate it.
Chet Ciconne 1:34:16
Thanks for having me, Bill. Great. I don’t get to talk to survivors. Like you know, I message people on Instagram all the time or whatever, but have a conversation with them. It’s awesome.
Bill 1:34:27
Yeah, me too. I didn’t get to talk to stroke survivors either. So now I’ve got 290 stroke survivors I’ve spoken to.
Chet Ciconne 1:34:33
Yeah, I got a lot to catch up to you, maybe I’ll get there with my new career so.
Bill 1:34:43
Absolutely love. Thanks again.
Chet Ciconne 1:34:45
Thank you.
Bill 1:34:46
Well, thanks again for joining us on today’s episode to get a copy of my book about stroke recovery from Amazon Go to recoveryafterstroke.com/book, and there you’ll find all the Amazon links To learn more about my guests, including links to their social media, and to download a transcript of the entire interview, go to recoveryafterstroke.com/episodes.
Bill 1:35:11
Thank you to everyone who has already left a review. For the podcast. It means the world to me. Podcasts live and thrive because of reviews. And when you leave a review, you are helping other people who are just like you, and in need of this type of content to find it easier. And that’s making a massive difference in their stroke recovery. If you haven’t left a review and would like to, the best way to do it is to go to your favorite podcast app and leave a five-star review.
Bill 1:35:44
You can do that on Spotify and iTunes, and a few words about what the show means to you. If you’re watching on YouTube comment below the video. Like the episode. To get notifications of future episodes, subscribe to the show, and hit the notification spell. If you’re a stroke survivor with a story to share about your experience. Come and join me on the show. The interviews are not scripted, you do not have to plan for them.
Bill 1:36:11
All you need to do is be a stroke survivor who wants to share their story in the hope that it will help someone else going through something similar. If you’re a researcher who wants to share the findings of a recent study, where you’re looking to recruit people into studies, you may also wish to reach up and be a guest on my show. If you have a commercial product that you would like to promote, that is related to supporting stroke survivors to recover.
Bill 1:36:36
There is also a path for you to join me on a sponsored episode of the show. Go to recoveryafterstroke.com/contact Fill out the form explaining briefly which category you belong to. And I will respond with more details about how we can connect via Zoom. Thanks again for being here and listening. I deeply appreciate you see you on the next episode.
Intro 1:36:59
Importantly, we present many podcasts designed to give you an insight and understanding into the experiences of other individuals’ opinions and treatment protocols discussed during any podcast are the individual’s own experience and we do not necessarily share the same opinion nor do we recommend any treatment protocol discussed.
Intro 1:37:16
All content on this website at any linked blog, podcast, or video material controlled by this website or content is created and produced for informational purposes only and is largely based on the personal experience of Bill Gasiamis, the content is intended to complement your medical treatment and support healing.
Intro 1:37:33
It is not intended to be a substitute for professional medical advice and should not be relied on as health advice. The information is general and may not be suitable for your personal injuries, circumstances, or health objectives. Do not use our content as a standalone resource to diagnose treat, cure, or prevent any disease for therapeutic purposes or as a substitute for the advice of a health professional.
Intro 1:37:54
Never delay seeking advice or disregard the advice of a medical professional your doctor or your rehabilitation program based on our content. If you have any questions or concerns about your health or medical condition, please seek guidance from a doctor or other medical professional if you are experiencing a health emergency or think you might be called 000 if in Australia or your local emergency number immediately for emergency assistance or go to the nearest hospital emergency department.
Intro 1:38:18
Medical information changes constantly. While we aim to provide current quality information in our content. We did not provide any guarantees and assume no legal liability or responsibility for the accuracy, currency, or completeness of the content. If you choose to rely on any information within our content, you do so solely at your own risk. We are careful with the links we provide however third-party links from our website are followed at your own risk and we are not responsible for any information you find there.







