Occupational therapy lecture at Australian Catholic University
Since 2015 I have been invited to speak at the Australian Catholic University to the third-year students during their occupational therapy lecture.
To find out about recovery after stroke membership go here.
Social Media: https://www.facebook.com/recoveryafterstroke/
YouTube: https://www.youtube.com/user/BillGasiamis
Highlights:
A change in gait
Too busy to go to the hospital
Another stroke is happening again
Losing my memory
The left side of my body is burning up
Surgery is the only option
When stool softeners begin to work
Damaged sensory neurons
Going home for Christmas
A stroke patient’s biggest fear
Transcription:
This is recovery after a stroke with Bill Gasiamis helping you go from where you are to where you’d rather be.

Bill 0:01
Thanks, everyone. Thanks for coming and hanging around to hear this second part of the presentation, it’s always good to present in a room where there are people in it.
My name is Bill. And at the age of 37, I woke up one day. And I had this strange numb sensation on my big left toe. And it wasn’t anything that you would really pay attention to, or think anything of until a couple of days later, when it started to spread from the little toe to the rest of the toes, and kind of started to work its way up towards the ankle. And by about the second day or third day, it got to the ankle and I went for a run at the gym. And as I was running, I noticed that my foot wasn’t landing properly on the treadmill.
And I really had to look at them and pay attention to where it was that I was putting my foot which was a little bit weird. It didn’t stop me from achieving my five-minute kilometer goal, which was something that I was trying to get to for a little while. But it was a really bizarre kind of sensation. And even though that was happening, I just put it into it being a muscle or something that I’ve done that was out of the ordinary because when I go to work as a, at my property maintenance business, we often leave things that are heavy, and I’m forever consulting my chiropractor to get me fixed and get me back on my feet. And, you know, give me work again.
As the days progress we have now gone through the weekend and on Monday I woke up in the morning to go to work the numbness had spread and id started to notice that had moved towards somewhere near my knee. And although it was there, the numbness was there, it didn’t really stop me again, from walking or doing anything that I normally do using our ladders and all the types of things that I did every day. And I’ve got to the point where as the days progress, it started to continue to move up my left side, and my wife for the first time about three or four days after I initially notice the numbness said, Why are you walking funny?
A change in gait is a symptom of having a stroke.
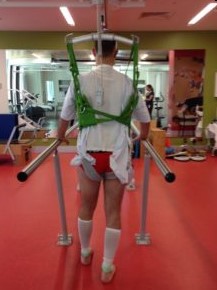
Now, I didn’t know what that meant, I thought funny meant that I was doing some kind of a ape-man movement or dragging my leg or looking really strange. But it wasn’t it was quite subtle. It was enough for her to notice that my gait was off somewhere somehow. But it wasn’t enough for me to notice. And I couldn’t comprehend what she was saying. So I just brushed it off and told her to leave me alone I have got stuff to do I’m busy.
So as the days progress we got to the end of the week. And I started to feel a little bit insecure about it now. Because the numbness had spread started to go around my hip and I thought maybe I should do something about it, I’ve got some work coming up I don’t want to miss out on my jobs if this thing starts to hurt, I might be on my back and I’m not up for that.
So I contacted my chiropractor and I made an appointment. And I went and had it checked out and he said, Look there’s some inflammation going on potentially, I can’t really see anything and it’s at that point where if things do flare up, give me a call. And I’ll get back to having somebody see you and work out what it is. And we’ll get you back on your feet. But see how you go.
So there was enough for me, there was nothing really going on. And I didn’t have any pain. I had done stuff like that before. Um gone to work you know, feeling strange, and having issues with my back or my arm or my leg. And as the week continue to progress, it got to the point where by now it was an extremely different feeling I was walking differently and my wife was still on the back about why I haven’t done anything about it, and why I’m still walking funny, and she kept arguing with me and said look go see a doctor go and do something about it.
And eventually, I thought on a Friday, now seven days after I noticed the initial numbness in my toe and by now my entire left side had pretty much gone to sleep I thought I’d ring my chiropractor again and make another appointment. But I’ll do it at the end of the day. Because I’ve got a lot of work to do and once I go, once I go at the end of the day to see my chiropractor, you know, it won’t interfere with any of the jobs will get paid, clients will be happy and all that kind of stuff. It was set up the next day, which was a Saturday and we had a whole heap of work to do and it was going to be fine.
So that’s what I did. We went into the chiropractor’s room and he started to check me out he noticed the numbness, and immediately he said the numbers is not being caused by anything that you’ve done to your back when I saw you a few days ago, there were no issues there’s still no issues with inflammation or anything like that. So I would suggest that what you do, is you go and see a doctor but don’t go to the GP go to the hospital.
I said Why would I do that. He didn’t want to scare me and say there’s probably something going on in your brain. He just said it’s not your back. So you need to go and say somebody and you need to go now
I said I can’t because if I go to the hospital, what’s going to happen is I’ll get caught in the medical system and I won’t be able to get out of there until Monday. By the time the doctors turn up, they do x-rays I get seen and all that kind of stuff as I won’t be able to go to work on Saturday. And he said look, what you’ve got to do is you’ve got to go to the hospital and don’t go anywhere else. In fact, go straight there.
And I said well, alright, leave it at that. I’ll go when I went home. When I got home my wife said to me what did the chiropractor say? And I said to her look, you know, he said whatever’s happening in my back is most likely not caused by an injury that I’ve created or done to myself, he said it’s something else and that I should go to the hospital.
And she said why didn’t you go to the hospital? I said well because we got a busy busy day tomorrow. I’ve got work to do. You know, we’ve got 15 guys who are going to be there Saturday. They’re all relying on me on managing this project. You know, we got to cut a hole in the wall. We’re going to get things in and out of this hole, we’re got to fix the wall. We’re going to paint this hole, we got to do all these things, and like how am I going to get it done If I’m in the hospital? It’s not going to happen. It’s impossible!
Too busy to go to the hospital
So my wife being a little bit smarter than me said look, why don’t I know it takes you to the hospital, they’ll check you out, they’ll tell you there’s nothing wrong. And you can go to work tomorrow. And I thought that was a great idea.
So that’s exactly what we did. And I’ve turned up to the hospital. And I walked into the Austin and went to emergency and went to triage and when I got to triage the lovely nurses asked me why I was in hospital. And I explained to them that there wasn’t really anything going wrong, too bad, but I just couldn’t feel my left side.
And then the red carpet treatment. I got the initial you know little tests to check the blood pressure and all that kind of stuff and then I was straight into what seemed like moments into CT. They did a CT scan and it took a little while before somebody came and found me. By that time I’d sent the wife away, I sent her home to be with the kids.
And it was at around 9, 10 o’clock in the evening, they told me that the CT revealed that there was a shadow on the brain. And they didn’t know what it was, why it was there. And what specifically it might be, what had caused it.
So we waiting for the tests further tests to be done and the results to come back and for a doctor to speak to me. But in fact, I wasn’t going to go to work the next day on Saturday. My wife had tricked me. I was extremely mad.
I woke up in the morning on Saturday and I rang my client and said to him, look, I can’t be there, you guys are going to handle it on your own. Everyone else is going to turn up so that’s no problem. Somebody else is just going to take the reins and get the job done. They managed to get the job done, I got paid and the hospital stay was extended for another seven days.
So I was in the hospital for an entire week where they did all those tests that Liana was talking about before MRA’s and MRIs and all those types of things, I had every single one of the tests that you could possibly imagine.
And what they discovered was that the cause of the bleed was an AVM arteriovenous malformation, which had bled and was more micro bleeding for the entire duration of time from when I noticed the bleed or from when I noticed the numbers that first day right through until the final day that I was released from the hospital.
So now the neurological symptoms started to go away. Because I was being treated with dexamethasone, it’s an anti inflammatory steroid it is extremely powerful. And it made me feel really good, except for all the symptoms that I experienced.
Which was hallucinations at night, like bugs crawling under my skin, an inability to stop eating, I put on eight kilos in the space of two weeks. And it was really shocking the things that I had to go through to get to resolve this situation that was going on in my head. And at the same time, I was told not only do you know that I’ve got to deal with this other thing that is going on and I don’t understand what’s happening. I have to always so go home and do nothing for the next six weeks
That meant no driving, no working no going to the gym, nothing strenuous nothing at all. So it’s exactly what I tried to do. I went home. And for the majority of the time I was behaving myself and I didn’t drive and I’m doing didn’t do any of the things that I was asked not to do.
But I did decide around the six-week mark to call my mates and my co-workers and asked them to come and pick me up and take me to work. And that was because I was bored out of my brain after six weeks I had done all the dusting you could possibly do at home folding the jocks you know the socks all that kind of stuff for my wife or she was at work.
And I thought our guys spend some time at work. And I’ll just go and watch the guys work. They’ll love that.
That’s what I did. I got picked up and I went to work. And I grabbed the chair. And I put it in the middle of the room with our painting quite a large wall that they are repairing. And while I was doing that, I
started to notice that I was feeling a little bit weird again. And my left side kind of started to go to sleep again. And I couldn’t rouse myself from that state and the rooms started to spin and I started to feel nauseous and I didn’t know what to do.
So I didn’t want to bother the guys because they were painting so I just waited for them to finish and I told them to look guys let’s get going. And you know, when you’re finished, you know you probably need to take me home because I’m not feeling well. But there’s no rush. You know, just do what you gotta do.
Another stroke is happening again.

Well, around midday, they had finished and it was time to take me home. It was a Friday evening afternoon. And we were working in the central business district in Melbourne. And we had to drive home to Preston in the northern suburbs, which was about 12 kilometers away.
And on the way past we drove and stopped outside of the royal exhibition gardens where they do the Flower Show and where they do the flower show there are massive amazing trees I said to the guy look pull over because I’ve got to actually throw up so when and threw up outside the car, thankfully for him on a tree. And it was exactly across the road from St Vincent’s Hospital.
So we got back in the car. And we kept driving. And we went to Preston and for some reason, there was bumper-to-bumper traffic this particular day, and I could not get him to get home any sooner. It took us about two hours to do 12 kilometers it was the craziest event. And the driving was just mental that day. So on the way there and as we nearly got home or my wife. and I said to her Christine, you need to be ready so that when I get home, you can take me to Austin because I’m feeling quite unwell, said Okay, no problem. We got home. And at around 3:30, we started to head towards the Austin hospital. And we were talking in the car and we got to emergency and she needed to take the car park it. So she left me an emergency. And it was going to take her a few moments to park the car and come back and see me
in that time of approximately 50 to 100 meters to triage and I introduced myself at the triage window. And that’s about all I could do. I couldn’t finish telling them my name. I couldn’t tell them what I was doing they didn’t know anything that was happening. And all I remember is after trying to create some kind of a conversation I ended up waking up sometime later. I’m not sure how long and there was a strange lady at the end of my bed
Have guests who it was?
Losing my memory after stroke.

The lady said to me do you know who I am, I said no
it was my wife
so I couldn’t recognize her and I didn’t know what I was doing. I was throwing up and I couldn’t I couldn’t do anything to help myself. And I just remember people running around frantic trying to get me sorted or fixed or something
a little while later I woke up and the result that came back was that there was an additional bleed. And now the blood in the brain went from being about the size of a 10-cent piece to about the size of a golf ball. And now the recovery process started to become a little more dramatic and a little more serious. And I couldn’t remember who had visited me I was having trouble making sentences,
I was having trouble typing an email and finishing a sentence I didn’t know I couldn’t drive. And I was extremely forgetful. And there were so many things that I didn’t wasn’t able to do that I didn’t experience the first time around.
As the next few months progressed, I went through the process of noticing that things were starting to come back slightly. So the doctor’s initial response was let’s not do anything. Let’s just monitor this. And let’s see if it bleeds again, it is unlikely to play the third time because these things very rarely bleed a second time they normally sort themselves out. And as I was going through that process of getting better and noticing that things were coming on. In fact, the MRI showed that the
bleed was starting to decrease in size and the blood clot was getting dissolved or going away naturally. So it was really good. And I went on this way. And I started to feel really great. And for the first time in almost three years is after the initial episode. I decided one day to go for a bike ride. And it was the first time that I had exercised or done anything strenuous. And the bike ride was amazing. It was November 2014, the bike ride was perfect I felt amazing I was fit.
The left side of my body is burning up
And the next morning had an appointment to go and see a client in the city. And on the way in. I noticed that I was feeling this burning sensation like I’ve been sunburnt but only on half my body on the left side
and didn’t know what it was quite bizarre. So we put out the car and pulled over to kind of walk around the car. Because that’s what you do. When you feel something on half of your body. Just in case you’re wondering. You know the car you walk around the car and when you get to the other side and jump back in the car. It goes away and it did for about five seconds. And then it went back
and then it was kind of like okay, well this is not right. I think maybe I’m having another episode and by now I had moved all my paperwork to the Royal Melbourne Hospital. So I decided to from where I was parked call my client said look.
I’m going to cancel the appointment because I can’t get them feeling a little bit on well it didn’t occur to me to look up at the corner where I was parked and get the name of the street and culture to zero to kind of get me a photo drive from Spring Street which was maybe four or five kilometers away into the Royal Melbourne and the hospital I got there somehow and I don’t know why or how so can physically remember getting there on it we’re just not there and when I got there I found you wouldn’t believe this is a miracle, I found the park right in front of the building the only one I parked the car there all day and I didn’t get a ticket.
I don’t know what happened. A miracle. And while the car was parked you know nicely doing its thing not getting booked I went inside to triage and I said to the nurses you need to get me in on having a hemorrhagic stroke.
And they looked at me like sorry, what’s your name?, and I said, look there’s no time for that, I’m having a stroke you need to get me in right now. and they said first you have to give us your name. And we have to go through a couple of things before we can get you in. I said, my name is Bill Gasiamis. I’ve been here before I’m experiencing a stroke you got, you got to get me in. And by now what drugs do you reckon the thought I was on?
Initially, they were a little bit standoffish. They put my details in the computer, they got my history up. And in fact, I realized this guy might be telling the truth. And they got me into again, the red carpet treatment, straight through into a CT scanner.
And normally when you go into a CT scanner or a room where there are MRIs, there are only a few people there’s one or two people who’re just doing their thing monitoring everything. This time the room seemed to be full of people that want to come and save you this crazy guy was talking about how he was experiencing a stroke and he is standing, you know, at triage. And sure enough, I was right and I proved them wrong.
Surgery is the only option.
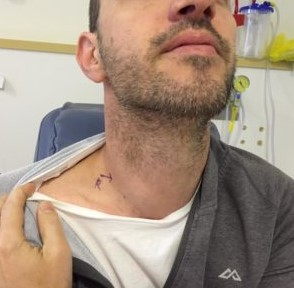
And a little while later I was admitted to the hospital and my neurosurgeon came and saw me and said, this time we’ve got to go in, we cannot muck around anymore, you are at greater risk of something terrible happening to you and you become seriously unwell then you are if we do nothing then you are if we do something and try and resolve this matter.
So in November 2014, I had surgery to remove the faulty blood vessel in my brain that kept leaking and cause these neurological conditions and these problems and this health risk was quite a dramatic time. And what I want to do is as I talk about what happened after the surgery and the role that occupational therapists played in my recovery, and physiotherapists
while I was in rehab recovering I want to talk about some stats that you guys might have heard, and you might have even touched on today. And those that are a little bit crazy because you guys are not going to be at work. So one in six people experience a stroke in a lifetime. That’s a lot of people. In 2017, there were another 56,000 people that were impacted by stroke. In Australia.
There are in 2017, there were 475,000 people in Australia living with the aftermath of a stroke. So quite a massive number of people dealing with the side effects or the impacts that are caused by either a blood clot or brain hemorrhage.
30% of stroke survivors of working age, I was 37, I was just in the prime of my working age, I had the mortgage I had, you know, two kids school fees with the whole shebang. And all of a sudden my wife became the main breadwinner on a part-time job three days a week,
65% of stroke survivors suffer a disability that impedes their ability to carry out daily living after stroke.
So
I’ve just spoken about the stroke community and there are so many other communities of people that get injured in need of the services of occupational therapy and rehabilitation.
So when I woke up from surgery,
I’m in, recovery, and my doctors and nurses came to see me and they fussed around me and my family and friends came in, it was great because I was awake.
And one of the first questions they asked me was, have you been to the loo? Have you done, you know, moved your bowls and done all that stuff? And I said, Look, I haven’t. And they decided, OK, it’s time to get you up and walking. And, you know, let’s go for a walk and see if we can get you out of it. And let’s see where you’re at.
There was no real assessment or anything like that was just day dot, you know, Ground Zero got out of bed, and the nurse who came to get me out was a very thin petite lady was about this talk compared to me, and she said just put your arm on my shoulder, and then I’ll help you. And we’ll go for a bit of a walk. And I did that. And I didn’t know that my leg didn’t work at that time. So I put my I came out this side of the bed I put my leg, my left leg out first, and within about three seconds I as bang straight on the ground
screaming, wondering why the hell is my leg not working. And why did they let me fall on the ground? And my head is, you know, freshly stitched up and, you know, fragile and it was just a disaster.
Somehow, they got me up and back into bed and realized that I’m not actually able to walk my surgeon came and visited and booked me in for a month of rehabilitation at the Royal Melbourne rehabilitation center, which is out in Parkville.
and waiting to get there. It took around two days before I was able to actually be there. And then another two or three days while I was waiting to actually start the rehab. And I couldn’t understand why they were taking so long to get me into rehab. And to get me on my feet and doing exercises. What I didn’t realize was without going through a process of assessment.
What else I didn’t realize while we were going through their process of assessment, there were a lot of rules and regulations that they have to follow to ensure the patient’s safety, and may not fall over again, hurting myself and injuring myself. And it reminds me of an incident that occurred while I was in rehab. So I was in bed and I wasn’t allowed to walk anywhere or do anything on my own.
And they had a wheelchair for me, and family and friends will come and push me around in this wheelchair. But it was one particular time of the day there was nobody there to visit me. The other patient was in bed sleeping or something in our shared room in our where there were two patients who needed to go to the loo. And I press the button for the nurse to come.
And I was waiting patiently. And then what seemed like you know, too long later, she hadn’t come here and pressed the button and I still waited and nothing but what was happening was it was day two of the effect of laxatives that didn’t work on day one.
When stool softeners begin to work.
So what had happened was day one they gave me some laxatives that didn’t work day two they thought well up the ante a little bit a give you a little more. And when they started working, I couldn’t get anyone to help me out of bed to go to the bathroom.
So I dragged myself out of the bed felt pretty much into the wheelchair and start to push myself towards the bathroom. And I go to the bathroom door. And as I drag that open, I noticed that inside the bathroom, the toilet is kind of elevated. Like it’s weird, it’s a little bit higher than the toilet at home, it was going to be a bit of a struggle to get up there.
Nonetheless, I was going to try and go to the door the nurses walk in and said, What are you doing I said, Well, can I’m trying to get to the toilet I have been ringing the bell and you guys haven’t been coming, I really gotta go, you know, the laxatives you gave me two days ago, twice. They’re really working now. And guys, you know, help me out get me on here.
And they were still kind of trying to be careful about getting me on there and making sure that I was going to be okay because they had no method to approach because I hadn’t been told what my issues were they just knew that I couldn’t feel my left leg, they didn’t know why and how I was going to be supported to get back on my feet. Because the reports hadn’t been completed by all the assessing doctors to get me on my feet in a way that was going to be safe.
So the story continues to unfold. Now with me finally getting the two nurses to get me onto the loo. And now they won’t leave the room.
And I said, “Okay, you can go now” and well “No we can’t we have got to stay here because we’re afraid that you’re going to fall and hurt yourself,” I said, “I promise like I am not going to go anywhere. I’m going to sit here and I’m gonna do what I gotta do”. “You guys have to leave the room please I’m busting off gotta go”.
And they won’t leave. And it felt like I was arguing with them forever to get out of the room so I can do my business in private because I was wondering like in that time, when I do finally let go and everything happens, what are we going to talk about?
I convinced them to get out of the room. And just as they did nature took its cause and everything ended happily It was amazing and fantastic, I cleaned up myself. And then the nurses came and got me back into the wheelchair and got me back into bed. Now what seemed like approximately three, approximately four days later, after my initial being in rehab initially and getting there, we started to do some exercises that were going to be safe for me to get back onto my feet.
So I had to get back home, I had to get back to work, I had to get back to paying the mortgage, dropping the kids off, and pick them picking them up from school. There are all the things that I had to do that I couldn’t do. And I didn’t know what would happen if I couldn’t get back to doing those things.
And what I realized was that when I was being impatient and complaining about why I’m not at rehab the doctors that were saying to me on a regular basis, almost two or three times a day, or assisting me. And they were asking me to see if I could move my arm, move my leg feel these feel that, they would get me up and see if I could balance do all the things that I needed to do to get home.
Because when I got home, my wife wasn’t going to be able to be at home with me 24 hours a day, seven days we should go to work. We couldn’t stop her from going to work. And although family and friends would close by they couldn’t be with me all the time. So it had to be safe enough for me to go up and down the two steps to go into my front door. And I had to be safe enough for me to get to the loo, make a cup of tea and a sandwich while I was waiting for somebody to come home and help me out. So it was quite a process that they needed to go through to determine the best way forward for me.
Now a couple of the things that they worked out that was going to be really good for me were to do exercises to get me recalibrating the use of my arm so that I could get it working so that I could pick up a knife or fork can use it accurately without making everything fall on me. So they assessed me initially as not being able to pick up my fork and bring food to my mouth, or hold a cup and bring it to my mouth.
Damaged sensory neurons due to stroke
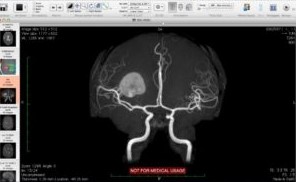
They also realized that I wasn’t going to be able to tell the difference because of the sensory neurons. damage to tell the difference between when something is too hot for me to be picking it up with my left hand, it would kind of register but a little bit too late. And I’ll probably be burned by them.
The left side is colder than my right side. And that continues to this day. I didn’t realize exactly what was happening yesterday, we had a really hot day in Melbourne, one of many that we had the last few days, and I was perspiring on my left side only.
I just noticed that yesterday. That was quite bizarre. And then you do this and be smooth on this. And then they get really sticky on this side and clammy in my hand. So there were really strange things were happening and the doctors who are assessing me and the nurses who are helping me out were constantly asking me about how I feeling what I’m noticing what I can do and what I can’t do. And it felt like I didn’t have the strength in my leg to actually keep me upright.
But I actually had I had the strength in my leg. What I didn’t have was the proprioception to notice where my leg was in the world. So my leg would go down, and my brain wouldn’t register that it was down. And it would try to counterbalance me on this slide with these muscles. And I would end up falling over. One of the best exercises that I did was in the swimming pool. Because for the first time, I didn’t feel scared like I was going to fall over while I was trying to walk. And I was trying to get movement happening in both my arm and my leg. So that was really, really good.
And one of the weirdest things that I experienced after the assessment was, remember how I said that they needed to make sure that I was going to be able to eat and you know, fend for myself while I was at home for those few hours was at the beginning. They took us to breakfast in a breakfast room. And we had to make our own breakfast. I thought that was so weird like, why am I making my breakfast what they’re supposed to be like bringing me that stuff and helping me recover and you know, get better?
And it turned out what they wanted us to do and see us do is you know, go to the fridge, get the milk out, go to the kettle make a coffee make a tea make whatever it was that you know, we enjoy eating in the morning, sit down and eat it. And then they made us wash the dishes as well. And it was just crazy. But what they were doing was getting me used to working with this new version of myself. And also at the same time assessing whether or not I was meeting the goals and objectives that we all had. And whether or not I was able to safely go back home when it wasn’t going to be anyone around.
Going home for Christmas
So it took around a month and Chris and just a couple of days just before Christmas in December of 2014 I went home and I went home and enjoy Christmas at home with my family. And then after that, I went into a process of rehabilitation at home where I was being visited by an out by occupational therapist that would come to my house and watch me walk up the stairs or watch me do all the things that I was being trained to do but at home, which was really comforting because now we had that next level of attention and assessment.
So it went really well, we’re able to really feel comfortable about using you know my home and getting into the shower and out of the shower safely. And then rehabilitation continued to occur as an outpatient. At one of the rehabilitation hospitals, in the northern suburbs in Bundoora where again that were assessing me because some of my goals changed now that I was up on my feet and back to work kind of, you know, part-time. I also wanted to get back to running. So one of the things that I felt was going to be really beneficial was I could run. And it wasn’t to be fit and you know, the five-minute mile or whatever it is these days, it was just to be able to get across the road if I needed to cross the road. And there was a car coming so I could run off the road safely.
So I was assessed in a way that was really good. We got me running recorded on a video. And then I was able to compare my running from the beginning of that rehabilitation to the end Got to the point where about nine months after I had been let out of a let out away from the hospital, I was able to nicely sack my occupational therapists and tell them that I was done and you guys have helped me out and now it’s up to me to do the rest.
But if it wasn’t for that initial care support, nurturing, love, compassion, amazing, you know, assistance, I don’t think I could have taken that next step and felt confident about being able to go home and live a relatively normal life with the deficits that I experienced.
One of the biggest challenges with stroke is when the deficit isn’t visible when you can’t see the deficit is that people judge you differently. In this case, I didn’t feel like I was judged differently. I felt like the people that were assessing me even though I didn’t look like I was affected by a stroke really did an amazing job in supporting me to get back on my feet back to my family back to work and back to a relatively productive life.
So that being said, you guys are doing amazing work going into the field that you’re going to, you’re going to make a massive difference in the lives of people on a daily basis. And I know that stroke patients can’t thank you, guys, enough when we don’t have the tools and the resources available to us to do the things that we want to do. So in advance of you guys going out into the field and doing that. Thank you for what you’re doing and all the best with your studies and please. Feel free to ask any questions.
Liana 36:41
Thank you so much, Bill. Always so entertaining and heartfelt. So as I said, Bill is happy to take any questions. So maybe I could start here in Melbourne does anyone have any questions here for Bill
Student 36:54
The first time you went to triage and you were talking to the nurse and you couldn’t speak properly as you mentioned when you woke up again did you have further problems with your speech?
Liana 37:05
Yeah, I’m just going to repeat the question for those in other states. So the question was when Bill went to triage and he wasn’t able to speak and communicate properly when he woke up, did you continue to have those problems?
Bill 37:19
I was able to speak as per normal I did have additional issues though I didn’t recognize my wife Initially, I couldn’t remember when people had come to visit me.
So I was really upset at a few people because apparently they didn’t come but they did. Yeah, and fatigue was a massive issue. Actually, I’d become extremely fatigued after that. It was the first real sign that I had experienced a massive neurological problem. I couldn’t, I couldn’t go to I couldn’t get out of the car and do a five-minute walk without becoming exhausted.
I remember having a massive argument with my wife because she parked in the wrong car, car spot one time which was three cars over from the one that I wanted her to park at because I couldn’t explain to me that I actually don’t think I can make it from that one to the door o the building that we’re going into, I became extremely aggressive and I couldn’t control my emotions I became extremely emotional crying at the drop of a hat, like, you know, a kitty cat tripping over something or whatever.
I noticed that I couldn’t comprehend what people were saying. So complex conversations, we’re just not registering I couldn’t understand. I couldn’t read and not because I actually couldn’t understand the words I actually didn’t have the brain energy to process that stuff. It was extremely tiring for me to read, man, I couldn’t do anything like it’s just really gone. It was not the same person that walk into that hospital or just prior to walking into the hospital completely different.
It took I reckon it took a good nine months before I started to feel comfortable that I was able to hold a conversation together with somebody. And I only realized that I was doing that because one of the only amazing things that I did was I went and saw a psychologist initially.
Probably the week after I was released from hospital and as I kept seeing her over the months that passed, she kept saying to me, wow you’re talking completely differently now. Do you notice how much better you are at finishing sentences and having a conversation? And that was the first time that I realized that I was actually able to have a conversation.
I used to forget appointments were terrible. So outpatient rehab was three times a week and for different one was arms one was legs for these different things. And it was over different days, different times of the day. I missed half of them. Like I didn’t know which one was coming next didn’t matter what they put it in the calendar something wasn’t computing to put the dots together of time. So time was warped and things were really weird and bizarre. There were some more questions in the back and then we will come down to the front
Student 40:25
in consideration of your whole recovery process whether it be at the start when things were being assessed or later on through your rehab what would you feel would be important for therapists whether it would be us as future therapists or others to be aware of when we are treating you what considerations do you think we will need.
Bill 40:48
Awesome. So the question was with regards to therapists when they’re assisting patients, what are some of the things that I think would be great for the patient, the therapist to consider when supporting us.
A stroke patient’s biggest fear.
So my biggest fear was falling over again. And one of the things that I needed people to understand and to consider was that although I was very keen to get on my face was very afraid of falling over and hurting myself and I didn’t know how much they took that into consideration, which of course they did, but I didn’t know that so it’d be great to have felt like that was verbalized to me.
Like we are here to look after you and make sure you don’t fall over, tell us what is it that you need to do or we need to do for you so that you can feel safe when we do this exercise or these exercises.
One of the other things that would have been amazing was to be told what was happening in those first three or four days, I didn’t get to see the occupational therapist or the physios but nobody was really telling me what was happening. So I’m the kind of guy I just need to know exactly good or bad. I just need to know everything.
So if I was told that what we doing is assessing you at the moment. And then at the end of that assessment in two, three, or four days, so long as you are going to start your exercises that would have been much better for me. Now in saying that though I don’t know if they actually told me that they may have. But I don’t know if I remember that.
So repetitive conversations are really important. And even more important when family and friends are around. I think conversations if you can have them with family and friends even better, because then they can remind me all the time.
So there were some of the things and then I was asked at one point which was amazing. I was asked what I would prefer to do and what kind of exercise I prefer to do. And that was great because that took away the concern that I might have had about what was coming and whether it was going to be difficult or not.
So as soon as the opportunity came I said like is there a swimming pool? And they said yes that’s a great get me into that. So that was amazing.
Liana 43:20
Yeah, I’ll just give the other states a chance to ask a question if there were there questions at all in Sydney. No? I don’t think there are any questions in Brisbane. Just one from Brisbane Um Bill there was a question about before the stroke where you were a smoker, but an AVM is different to an Ischemic stroke. So the question really is did you have to change any aspects of your lifestyle after this event?
Bill 43:55
Yeah, that’s a good question. Yes, I was a smoker. I was a smoker and a drinker but not an excessive drinker. I was stress head I worked too many hours I was perfect, I was creating the perfect storm for this weakened blood vessel to you know, just let go.
And I didn’t have high blood pressure, high cholesterol, and that stuff looking at me, you would have thought that I was in very good health, but I had noticed that I was getting these strange headaches about 18 months prior to the hospitalization.
The first hospitalization and whatever was causing those headaches by the time I went to the hospital they weren’t able to show proof so it was inconclusive but I have a feeling that it had to do with a high-stress high blood pressure episode that was you know brought on by myself and I say that because the time that I noticed that massive headache occur I was at the Collingwood St Kilda drawn Grand Final and I was screaming like a maniac. And when I went home, the headache didn’t go away for the whole week. So I missed the replay. And as a result, didn’t get to see Collingwood win the grand final.
So my headaches and my stress episodes kind of occurred when I was doing you know, what I would call like being just a real hothead and, you know, smoking and not looking after myself in certain instances of the week or the day or whenever it was
I don’t smoke by the way anymore, and I hardly drink I had one drink on the weekend for the first time. in about three months. I was completely drunk my wife was wrapped because she said I was a cheap date
Were there any other questions?
That’s alright. Any more questions from Interstate?
Liana 46:00
Probably have time for one more question. If there’s not any for me to start. I think that was another one in Melbourne.
Student 46:09
You pretty much answered it I was just going to say, upcoming to your episode. You talked about a little bit of numbness, but were there any other symptoms at all, like headaches that you mentioned? Was there pain at all?
Bill 46:16
the question was was there any other symptoms or anything that gave me any clues as I was leading to that first episode, there weren’t and that headache happened it happened in almost more than a year before this first hospital episode, the numbness before I noticed the numbers. And I can’t say that even if there was something that I really paid attention to, I don’t think I was paying attention to anything. I was just trying to get through my work.
So nothing that I could really hold on to and really sort of say that, you know, there were some warning signs because even that thing that happened and when I was at the footy, it wasn’t a warning sign that there was something more sinister around the corner or not, for me.
Anyway, the doctors when I went to the hospital did check to see whether I was bleeding in the brain. They did a lumbar puncture, and it came back negative, so they just put it down to, you know, one of those things and it went away and that was it.
Thanks, everybody. Really appreciate it.
Liana 47:36
I just want to thank Bill. Again, I think you can all probably realize now what a remarkable individual he is and what a remarkable recovery he’s had. So I just want you to join me in thanking him once again. Thanks, everyone and I hope you enjoyed the classes this week.
Discover how to support your recovery after a stroke. Go to recoveryafterstroke.com







