Musa Pam is a Stroke Survivor who went on a combined Stroke Recovery and Sports journey and rediscovered his love of golf despite being able to swing with only one arm.

Socials:
LinkedIn
Myfitnesspal
Highlights:
01:15 It’s the best and worst thing that happened
04:00 North-American One-Armed Golfer Association
08:10 Strokes are like snowflakes
13:57 F.A.S.T (Face, Arm, Speech, Time)
18:50 Patent Foramen Ovale
31:50 Home modification
42:00 B.M.R Basal Metabolic Rate
54:15 Find your strength
Transcript:
Musa Pam 0:00
But the true absolute actual cause of the stroke was that I had a PFO a PFO is a patent foramen ovale, which is essentially, in simple terms, a hole in the heart. We’re all born with a hole in the heart. In 90% of the population, that whole is close. And in about 10% of the population, it remains open. So in my case, it was open for as long as I had been living up to age 41. And then I never knew that I had that whole. And the way that you find out, unfortunately, we have the whole is when you have when you develop a clot somewhere.
Intro 0:45
This is recovery after stroke with Bill Gasiamis helping you go from where you are to where you’d rather be
Bill 0:51
Musa welcome to the program.
Musa 0:55
Thank you, Bill, thank you so much for having me. This is a fantastic opportunity, the chat with a fellow stroke survivor.
Bill 1:03
Yeah. It would have been better if we just fellow something else, human beings. But we are fellow stroke survivors. So you know, we’ll just run with it, man. It’s no big deal, is it?
It’s the best and worst thing that happened

Musa Pam 1:14
It’s absolutely no big deal. As I tell people, it’s the best thing that happened to me, it’s the worst thing that happened to me. But I like the part where I say it’s the best thing that happened to me because it really gave me an opportunity to hit the reset button at the time that it happened. And it’s opened me up to so many opportunities to meet people and to help people to educate people in the volunteer opportunities that I have that I take advantage of. And I wouldn’t give it up for anything else.
Bill 1:49
You on your Instagram feed you call yourself the one golf champ. And that just blew me away when I read that. So I thought I’d get in touch and I wanted to find out. Tell me a little bit about what happened to you.
Musa Pam 2:08
Yes, so I’ve had it for probably since about 1995. So I’d say it’s probably been about 24 years since I’ve had this passion for golf. I never thought that I would become so enamored with golf, but I started playing golf, just after I finished college here in the US. And I’ve been playing I wasn’t a very good golf, I’ve never been a very good golfer. And I was just hack hacking as a golfer. And so fast forward to 2012 when I had the unfortunate circumstance of being afflicted with a stroke, and here I was then was left with a residual disability with limited use of my left side because I had an ischemic stroke that affected the right side of my body, the right side of the body tends to result in the left-sided weakness in opposite side weakness in my case, right side, right side stroke, left side weakness.
North-American One-Armed Golfer Association

Musa Pam 04:00
And so I was limited in the ability to use my left, my left side my my left arm to play golf. And so for about two years after my stroke, my stroke happened in 2012. For about two years after that, I was just after all the rehab and what have you, I was left with this dilemma. I wanted to play golf again. But you know, how do you play golf when you’re only left with the ability to use one hand or one arm? So I did some research on the internet and I discovered this organization in the US called the North North American one on Golf Association of NOAGA for short
Bill 4:06
As if there is an organization that exists like that. Unbelievable.
Musa Pam 4:10
There absolutely is in the UK. In the UK, there’s an organization called the Royal, Royal Society for one-armed golfers. I believe that that’s the equivalent organization in the US in the UK. And so I discovered that this was an organization for golfers who have to have to play golf with one arm for whatever reason it is, in most cases, it’s an amputation, due to an accident or what have you. In other cases, it’s people like me who’ve had strokes. In other cases, people have cerebral palsy, and in some cases, people were just simply born with one arm. And they discovered golf as a result of either being exposed to it by their parents or by their loved ones or by friends or they just were simply naturally born athletes who decided that golf was something they wanted to explore.
And so this organization came together. And I discovered them on the Internet. And I found out the year I discovered it, I found out that they were coming to Rhode Island, which is a neighboring state, to where I live in Massachusetts, they were coming to Rhode Island for our tournament, and I decided to join them and it absolutely blew my mind. It changed my life because I then found are actually people out there who are playing golf with one arm. In the subsequent, the following year in 2017, my division called the Sanders division, we had a tournament in Michigan, which is about 1400 miles from where I live. We had a tournament for a week and in my division, I won the championship that year, I was just beside myself thinking two years ago, I didn’t know where to go to play golf with one arm. And here I am standing with a championship trophy in my division. You couldn’t write that script if you tried.
Bill 6:06
I was gonna, I was going to start by saying what I say to a friend of mine who’s a double amputee below, above the knee Yeah, double amputee above the knee who’s a golfer. And what I say to him is mate golf is a great way to ruin a really good walk. And
Musa Pam 6:28
it was so funny.
Bill 6:31
And the and I’m starting to consider my comment more seriously now because of finding so many people who are saying to me, that’s actually an amazing way to rediscover yourself and to overcome challenges and to you know, integrate into sport again, you know, which, which I think is great.
Musa Pam 6:57
Yeah, absolutely. It’s, it’s, you know, for normies, that’s what we call in the stroke community. In the one on golf community, we call no means people who play golf normally, with two arms and two legs. So for normies. When I was normal, we would say that a great day at a great day on golf. Have a great day. A bad sorry, start over a bad day on the golf course, absolutely beats a good day at work any day.
Bill 7:30
Well, that. Absolutely. It’s true, that must be true. I’m going to have to look into golf and Okay, we’ll do that maybe in the near future. But in the meantime, what I wanted to understand was what happened to you leading up to the stroke. So it was an ischemic stroke? What did you notice?
Strokes are like snowflakes
Musa Pam 7:51
Yes, um, there’s a group I belong to on Facebook called the, the young stroke survivors and it’s not really, for young people, per se, from a demographic standpoint, it’s just, it’s just a moniker that applies to anybody. And one of the models of that group that I noticed was that strokes are like snowflakes, right? strokes are like snowflakes, no two strokes are the same.
My family background, I grew up in Nigeria Bill, um, and my first exposure to stroke, or whatever a stroke might be, was that it afflicted my father in 1989. He was 54 years old.
And he was he, he, he had a stroke, and he did not survive the stroke. So 48 hours after his stroke, really, he was no longer with us. Unfortunately, for me, I never got to see him during those 48 hours by the time I arrived at the hospital way was he had passed on. But what I recall from family members was that during the course of those 48 hours, when he was unable to speak,
And to this day, I’m not sure if he had an ischemic stroke or if he had a hemorrhagic stroke, as we all know, a hemorrhagic stroke is much more devastating than an ischemic stroke, which might have had aphasia along with it as well, because he, in phases, you know, is the type of stroke that affects one’s up one’s ability to, to speak, and, and in some cases to reason as well. So, he would simply, if you can see it on the on-screen, he would rub one side of his body, when people would come to see him, like my mother or my, my, my siblings, and he indicated that he was unable to move that side. So that was my first exposure to stroke.
And so because I was about 17 ah 18 years old at the time, you know, I felt like, you know, being a teen and my dad was 54. That was something that happened to old people. And so the day of my stroke, I woke up in the morning, it was, my late brother Iacobu’s, what would have been his 40?
It was 2012. So yeah, Iacoubu would have been, would have been 45. That day, he was four years older than me. So, you know, went through my normal routine, and I said a prayer for him. And, you know, remember him was going to work, during the course of my work that day, had a couple of meetings, and one of them didn’t go particularly well. But you know, what day at work goes perfectly well for people? So I had occasion to have a difficult conversation with a colleague of mine about something that happened related to someone I worked with, that wasn’t very happy with the way that that person was treated.
Also in New England, here in Massachusetts, which is part of these six states called New England, and in the northeastern part of the United States, it had snowed that day, that was one of the first days where it had snowed. And there’s probably about half of half an inch of snow on the ground. So I went to work and came back, on my way back, I was driving and, you know, I felt a little bit of my nerves twitching and my left arm and I thought, you know what, I’ve had that happen from time to time when my nerves would twitch with twitch, and I would say, yeah, whatever, you know. I got home and on my way home, I stopped at the health center very close to my house, because I’d been trying to get an appointment with a with my physician who would, who would become my primary care physician, my primary care provider, and I’ve been going back and forth with this manager at the hospital. And she happened to not be in the office at the time I stopped by.
So I looked over at the stadium because it’s very adjacent to the stadium where if you’ve ever heard the of the New England Patriots, of football, that’s where they play at patriot place. So I looked over and I posted something on Facebook saying, Hey, you know, this is a big weekend because we’re playing the American football champion, American Football Conference Championships that weekend. And I couldn’t wait to get home I stopped by a got a 12-pack of beer for the weekend or whatever. And I got home. And I saw the snow on the ground. And I thought oh, you know, I don’t want to leave this snow, so they wouldn’t freeze. I started to just shovel it a little bit and I lost my balance, Bill.
And when I lost my balance while I was on the step I thought oh, clumsy me you lost your balance be careful. And I walked into the house after I shoveled the snow and walked in the house and I started going up the stairs as I was going up the stairs. I found my left foot was hitting the steps. As I was going up the stairs. There are 14 steps from my ground floor to the second floor. And I thought that was really unusual. And when I went when I walk through a door in my office, which I’m sitting in right now, I walked through the doorway, and my left shoulder hit the door jamb the doorway, and I thought that’s really odd. And I came into the office sat down and I thought my left foot hitting the steps. My muscles were twitching while I was driving my left shoulder just hit the door jamb. You know what I’m going to sit down and guess what I googled.
Bill 13:44
stroke
F.A.S.T (Face, Arm, Speech, Time)
Musa Pam 13:44
stroke symptoms, and I google stroke symptoms. And I got this gobbledygook. This all kinds of research papers at this professor and that thing, what I didn’t find was what we call FAST today. There was nothing that screamed out at me saying FAST. Look at yourself in the mirror. The F in Fast stands for face see the one side of your face is drooping. Or the A lifts your arms if one arm is lower than the other or S tries to speak. If you see that you’re slurring your speech, and then the T in fast is time. Do things quickly take action at any one of those three things is an effect call 911. In our case, in your case, it might be 999
Bill 14:37
000 in Australia, three zeros.
Musa Pam 14:42
Yeah, absolutely. So call for help immediately. So when I didn’t see anything that really caused the alarm, I took a couple of ibuprofen tablets for headache or pain and decided I wasn’t going to finish the bottle of Heineken I’d start on and I just decided I’d take a nap. And I took a nap. And would you believe that in my honest belief, I think that my dad woke me up, my dad woke me up? Because I woke up in cold sweats thinking to myself, Oh, my goodness, I don’t know what’s going on. But I am losing sensation in my left side. So whatever it is, you know, data is what we call them dada, I know you woke me up, let me get up and take care of whatever this is. So as I got out of bed, tried to take one step and crumpled to the floor like a sack of potatoes. And I thought to myself, Oh my goodness, something terrible is going on here. And I reach for my phone and I called 911 told the person on the other line, I think I’m having a stroke.
Subsequent to that I made another phone call, which I would not, I would not advise anyone and my brother lives in a different state than I do. And I thought he was my closest living relative. And I thought I would just inform him that I was having a stroke. Well, that didn’t really help matters too much. Because here he is absolutely helpless. He’s six hours away from me. I told him that, you know, I’m upstairs, I don’t think I can get downstairs. You need to help me call the fire department in my town and let them know that they need to break the door down. Well, I come to find out later on that you know what, when they show up, and you’ve called for service, and there’s no one at the door, they’re going to break the door down anyway, which is what they did. But he was absolutely you know, he was beside himself with despair.
He didn’t know, you know how to how to help. He was helpless. Because he was so far away. He happened to call the fire department and they told him exactly that. Listen, we’re going to show up. And if there’s no answer at the door, we’re going to look, we’re going to break the door down we’re going to go in. And so they came in with a walking structure upstairs, basically put me in it and it’s essentially a stretcher that allows them to lift me up in a walk in a standing sort of sitting position. And they walked me down the stairs with it and took me to the hospital and I was examined. It was determined initially that it seemed as though I was having a TIA which is a Transient Ischemic Attack Because when I first presented, it looked like I was starting to move my extremities on the left side, about an hour later I couldn’t move any of the extremities. So the TIA essentially turned it into an ischemic, ischemic attack and I was full, full-on having a stroke and not able to move in, I was brought into the cardiac unit and then subsequently into rehab.
Bill 18:03
So the ischemic stroke occurred from what do they know? Was it something that, a blood clot that was created at the start, at the heart? Or was it something else?
Musa Pam 18:12
Very, very good question. In my case, and I want to be honest and open here I mentioned the beer. So you know, I wasn’t an alcoholic, but I didn’t enjoy one or two Heineken’s here and there and, maybe a glass of wine from time to time. The other thing that I had, I had some risk factors. So the other risk factor was that I was a smoker. The third risk factor was that I had I was probably I was overweight, if you look at the scale, given my height, and the BMI, the BMI scale.
Musa Pam had a Patent Foramen Ovale
Musa Pam 18:50
I was overweight, but I was not obese. But the true absolute actual cause of the stroke was that I had a PFO. A PFO is a patent foramen ovale, which is essentially in simple terms, a hole in the heart. We’re all born with a hole in the heart. In 90% of the population, that hole closes, and in about 10% of the population, it remains open. So in my case, it was open for as long as I had been living up to age 41. And then I never knew that I had that whole. And the way that you find out unfortunately we have the whole is when you have when you develop a clot somewhere.
So in my case, a clot had developed somewhere probably in my leg, probably some of the part of my body, and that clot traveled, and instead of going through the lungs and getting cleansed in the lung and filtered and pumped and that and that blood pumped through my body to serve various functions. Unfortunately, that clot then bypasses the lungs and traveled straight to my brain to the rear part of my brain called the basal ganglia where the location was that was identified as the location of my stroke. And that’s what caused the left side, the right side stroke.
Bill 20:17
So that’s um, Okay, I’m going to say it’s more, sounds like more dramatic because now not only are you dealing with the stroke, but you’re also dealing with a heart condition. So did you have to have heart surgery? Straight away? Or how did they resolve that?
Musa Pam 20:38
Another fantastic question. Here in the US, there are various approaches to the PFO and dealing with it. I mentioned the New England Patriots, which is a major, a major sports organization. But there’s a player who played for the Patriots called Tedy Bruschi. And at age 37, this is before my stroke, which have been about two years before my stroke Tedy was afflicted with a stroke. And the general consensus was how come and how does someone who’s so fit who’s an athlete develop, have a stroke at age 37.
And at the time, it was discovered that he had a hole in the heart. And so when mine happened, things just started, you know, clicking together. In Tedy’s case, he had surgery to close the hole in his heart. In my case, I asked for a second opinion from Massachusetts, General Hospital vascular surgeon. When I had that consult, it was discovered, both of us did and he reported to me that about a third of the population that had a hoe in the heart had surgery, about a third of the population had some some sort of some sort of therapy some sort of blood thinner therapy.
So whether it was in my case, Plavix, or Clopidogrel, which is the scientific name for Plavix, or some other people might be on Fragment or some other blood thinners, the other third had nothing. And guess what, it turns out that there was no discernible scientific proof that any one of those populations resolved permanently or resolve the situation with the hole in the heart. And the results were inconclusive in all three of those cases. So in my case, I decided, well, if there’s no scientific evidence that surgery resolves the situation, then I might as well stay with the Plavix. In just stay on blood thinners?
Bill 22:57
Yeah, okay. I suppose at that time, it’s a really good decision because you’re trying to heal the brain. So another surgery and all the stuff that can possibly happen during surgery and all the risk factors to surgery could make the brain injury worse. How long were you in rehabilitation after you were admitted, and they discovered the cause of your blood clot?
Musa Pam 23:28
Right, so I should add that it was it wasn’t simple, it wasn’t easy to find my find that PFO at first. So when I presented in the emergency department, I was sent to the cardiac unit at Morwood Hospital, very close to where I live. And over the course of the next 48 hours, they began to do several, several tests to rule out various things. I had an MRI and a CAT scan, and I had an ultrasound, but none of them showed anything luckily, I had a very good neurosurgeon who was attending at the time by the name of Salvatore Napoli who’s still my neurosurgeon this day.
And he ordered what’s called a Trans Esophageal Echo Cardiograph. So TEE it’s essentially a scan, where a tube is passed through your mouth down your throat into your heart. And that was the definitive test that showed from the TEE that I had a hole in the heart. and subsequent to that, then, you know, he was able to then look at various other things to deal with. But that TEE was the definitive diagnostic exam that discovered the PFO.
And so you’re right, thinking about surgery and all of the various complications that could come about, you know, I had to weigh all those factors. And for me, I felt like it was a no-brainer, if you know, no, no pun intended right? Now, it was a no-brainer that, you know, if surgery didn’t prove that that was the definitive, best remedy for this, then why why why try to do anything to have invasive surgery, why not just stay with the medication?
Bill 25:36
And then you have to recover from the impact of the stroke, right? So your left side is not working. And you’re in the hospital for how long?
Musa Pam 25:48
I was in the hospital for a total of 33 days. So three days in the acute care hospital in the US. That the acute care hospital is your run-of-the-mill hospital, General Hospital, community, hospital, etc. And then I was taken to what I insisted, I insisted I would be taken to the Spaulding Rehabilitation Hospital in Boston, about 30 miles from where I live. Initially, there were no beds available. And I was offered another rehab hospital and, I insisted on being taken to Spaulding, I was offered to go to Braintree rehab, which is a little bit closer, I insisted on going to Spaulding. I’m glad I did because Spaulding changed my life because the model at Spaulding is to find your strengths. Luckily a bed opened up at Spaulding. I was taken to Spaulding Hospital within three days and there I began, I began an intense regimen of rehabilitation.
Three types of rehabilitation, I’m not sure what it’s like in Australia Bill, but the three major components of rehabilitation for stroke patients at Spaulding are physical rehabilitation, occupational therapy, and speech therapy. So so PT, OT, and ST as the other three acronyms, physical therapy, occupational therapy, and speech therapy.
And speech therapy really dealt with not just speech, but swallowing as well. Because one of the things we find out as stroke, stroke survivors is that because of the weakness on the left side if you’re not taught very carefully how to swallow, you could chew on your tongue and swallow the wrong way. Chew on your lips, bite your tongue, those sorts of things. So speech therapy, really in ——–, not just speech and how to speak, but also being able to eat well.
Bill 27:51
Yeah, I’ve done a couple of episodes on. I’ve done an episode with a lady called Tracy Bode who’s a speech therapist here in Australia. And she’s the one that first told me about speech therapy not being just about people speaking again, in Australia, the rehabilitation is similar in that you go through everything that you need, I needed to learn how to walk again, and use my left arm again, I didn’t need speech therapy, because I didn’t have any issues with my speech, or my tongue, any of that stuff I didn’t have.
I had motor neuron challenges. So it was more about being able to use my left arm and left leg and get the sensation back that my left leg, for example, was on the ground so that my brain could recognize that it was there. So very different kind of rehabilitation, there was occupied occupational therapy, but I didn’t know that I was doing that at the time. And I was getting frustrated because they were making me make my own breakfast using my left arm.
And I was thinking of how why are they doing this, like, can’t they get somebody to bring us breakfast, you know, why do I have to make it? So what I realized later, a little while after I asked was what we want, we want to make sure when you get home, you’re able to cook and feed yourself and do the simple things, you know, make a tea or whatever it was on your own and that you wouldn’t drop it or burn yourself or not be able to use your left arm.
Okay, so I thought all right. So they didn’t make it explicit, that that’s what was happening. And that’s why I was making my own breakfast. But they were supervising us while we were doing that, we would make breakfast we would eat and then we would wash up. So that’s how we did occupational therapy was a little bit ah It was really good. It helped me get the confidence so that when I went home, my wife was at work, and my children were at school, I could be home alone, and I wouldn’t have any challenges. Tell me. Are you a family man?
Musa Pam 30:07
No. One of my challenges was independent living because I’ve always thrived on independent living. And so that was a very important component of what it, what was taken into account in my discharge planning. Fortunately for me, my brother came down from Maryland and spent quite a bit of time with me visiting me in the hospital during the course of the 30 days that I was in the hospital. And as discharge planning began, you know, there are two options in the US you could be discharged to home, which was what I was fortunate to have had. And there’s discharged to some other facility.
So a lower-than-acute rehabilitation facility would be a skilled nursing facility. And they are called SNFs for short so SNFs, skilled nursing facility, that’s a that’s other rehabilitation hospital where it doesn’t necessarily have all of the level of complexity and staffing that in that an acute care hospital and acute care Rehabilitation Hospital has. But that’s still you’re still supervised in many cases and in helping to be to become independent. So that occupational therapy at Spaulding really helped me in many cases because part of what we had were sessions on, really being able to cook in the kitchen make you’re way around, and try to think about what your home layout was.
Home modification for Musa Pam
Musa Pam 31:50
Whether you had steps in my case I talked about the steps going up so so I had to have handrails installed in my house. On the right side going down I had handrails the on the right side going up and not coming down. So I had something to hold on to going into the house I had to have the steps modified because that’s all I had with just steps going up with no handrails, so I had the steps modified with it with the ability to hold on to handrails going in I had my shower and tub and bathroom modified so I had a shower bar and grab bars to be able to hold on to basically things and then we laid out the house and made sure that all of my quarter that I had around the house was was was cleaned up and I had ample room to be able to move around to walk with my quad cane.
And this brings me to something one of my went into Spaulding I was wheeled into a small day and a stretcher. And it was really determined Bill, this was something that was absolutely adamant about that I wanted to walk out Spaulding after 30 days, when I was discharged, I was fortunate one of the fortunate few to be able to walk out with a quad cane a cane with the four little legs at the base. So we call that a quad cane. And shortly after that, maybe about two or three months after, after spending some time I had, I was fortunate to have an in-home visiting nurse and in-home physical therapist, and in-home occupational therapist who visited about two or three times a week for about three or four weeks until I transitioned to an outpatient, an outpatient rehabilitation center here, very close within the stadium complex next, near where I live.
So I was I did that for about nine months, nine to 12 months or so until I was able to transition from a quad cane to just a single straight cane. We were working on strengthening my left side strengthening my body. You know, I was doing various exercises, and then I decided that you know what those exercises, I could bring them to my local gym. So I would go to my gymnasium, and do the walking on the treadmill doing the strength exercises to really strengthen my my left side as much as possible.
And I had one of the most amazing therapists he’s not he wasn’t a therapist at the time, he was a physical therapy aid. Tyler McCarthy, who happened to love golf as well. So during the course of our therapy, he found out I love gold and during the tail end, as we’re approaching the end, he and I actually went out on the golf course and played golf together. And you know, I think I shot 72 or something like that I posted on Instagram and Facebook. But I was absolutely excited because I was finally able to play golf again. And I couldn’t wait for what the future could hold.
Bill 34:53
I’ll take out we’ll have that discussion and a little bit I’ll definitely ask you about your golf game. Tell me about, so did you experience fatigue or any of those challenges that a lot of stroke survivors talk about where, you know, fatigue doesn’t, gets in the way and the energy levels are, you know, are drained and it’s difficult for them to get up and be as active by the sound of it, you’re very active. To be as active as you did you have any of those challenges on top of you and not being able to walk or use your left side properly.
Musa Pam 35:33
You know, I am fortunate and blessed that I did not have fatigue as an obstacle in the course of my recovery. I’m really thankful for that. Because as I visit, with other stroke survivors, I volunteer at Spaulding now I go there about once a month or so and I visit with patients as part of the pier visitor program. You know, like we talked about fatigue. And I really am thankful that during the course of my recovery, fatigue really wasn’t an issue.
I mean, The only thing I remember relative to fatigue is that as I contrast to this day, seven years after my stroke, I think about the times I was in the hospital where I would wake up at, you know, seven o’clock in the morning, and by 5 pm I’d be in bed and so literally, I was sleeping for you know, 12 to 14 hours. And I I didn’t think like there was enough time to sleep because I was tired when I woke up. But after discharge, I think that you know that as the energy levels came back and as my strength came back, any fatigue any residual fatigue, I think for me disappeared and dissipated very quickly.
Bill 36:47
Yeah,
Musa Pam 36:48
So I’m unfortunate.
Bill 36:49
Yeah, that’s a great bonus and a great benefit. I had a massive struggle with fatigue early on as well and then dissipated and got a lot better. And then after, because I had my bleed, the first blade in February 2012. And then I had surgery in November 2014. And then in November 2014, there was no fatigue, although there was initially, you know, in rehabilitation, there was fatigue, there wasn’t the ongoing fatigue that people talk about.
And it was just the brain healing after it’s been touched by you know, a surgeon and, you know, the skull getting, you know, put back on and all that usual stuff, you know, overcoming the anesthetic, and all that type of thing. But one thing I realized was that food really affected me and created fatigue, more in the sense of, you know, what you hear about a lot of brain injury people talk about is high carbohydrate foods tended to create fatigue afterward, similar to when we talk about a food coma.
When we’ve been you know, healthy and just overeating, similar kind of feeling when we’re carbohydrates. Tell me did you change your diet? What changed after the stroke? You’re a smoker beforehand, you drink a little bit? Nothing major, like sounds very similar to me. I definitely stopped smoking and drinking initially. What about you?
Musa Pam 38:20
Yeah, so the funny story I tell about smoking was that Dr. Napoli, the attending neurosurgeon at the hospital at Norwood Hospital, the day of my stroke, while examining me said, you know, the million questions, they ask you what, you know, What year is it? Who’s the president, etc? And at some point, he said, Do you smoke? And I said, Yes. And he said, You’ve had your last cigarette, and I said, Okay, make me better. And I haven’t had a cigarette since and seven, almost seven and a half years. So that was the situation with smoking.
As far as diet goes. The interesting thing about diet was while I was in the hospital, and I think it was probably more of an experiment than anything else on the part of the, medical providers, I would look at my tray when it arrived. And, you know, I you know, there would be this land stuff on my, on my tray of no salt, and this and that. And eventually, maybe after about three days, I mustered up the courage to ask a nurse or someone, you know, what is up with my diet? And they said, Oh, you’re on a cardiac diet.
So no salt? No, no, this No, that, and the other thing. I said, Okay, so I went along with it. And eventually, one of the days I was examined by a physician, I said, You know what, I’m on this cardiac diet, what’s going on with this diet? And how long am I going to be on it? And they said, Well, you know, I could take you off of the diet because you really don’t need to be on a cardiac diet. I think we have things under control all right now in the hospital, I can take you off the cardiac time. And I chose I said, You know what, hold on, hold off on that for now. Because I you know, I kind of, I kind of liked the idea of understanding what, what the right portion sizes are what a low sodium diet should consist of, and what a high you know, sort of vegetable high vibe fiber diet, I said, I’ll stick with it.
And I really did throughout the course of the hospital. Now we had what we call sausage Saturdays was able to have a sausage, and I really enjoyed it. But I didn’t really I wasn’t really much of a breakfast person, Bill. So it wasn’t something where I, you know, I was going to bring that home. But in the hospital on seven, three meals, I was having breakfast, lunch, and dinner, which is very unusual for me. But what I did was I had a lot of time in the hospital to do research on a number of things.
A very, very dear friend of mine, who was who had been in the military served in Iraq and came back and unfortunately was a victim of an idea attack and his Humvee and, and none of his fellow soldiers survived. He was the sole survivor of this attack. So when I met Brian in New York, Brian was his fiance was working in a bar in New York, where I was visiting, and we happen to talk to each other was it was if you’ve ever heard of New Year’s Eve in Times Square in New York,
Bill 41:27
I’ll be there.
Musa Pam 41:27
It’s a big deal. Yes, he was waiting for Briana. So he was away from Times Square. And I came to find out that he doesn’t really do well around fireworks and explosions as you can very well imagine.
Bill 41:41
Wow.
B.M.R Basal Metabolic Rate – Musa Pam
Musa Pam 41:42
Well, Brian and I were talking and at the time, he had just come back. So he was dabbling in various things to do for work, he is working in a jewelry store, and he really didn’t like it. So starting today, who’s starting to take classes to become a personal trainer? And during the course of those classes, were talking and he talked to him, and he taught me this term called the BMR or the basal metabolic rate, which is really how much you burn calories when you have a sedentary lifestyle.
What is your basal rate? If you don’t absolutely do anything at all, how much how many calories do you burn? And the math is really simple. If you know what that number is for yourself, then whatever you burn over and above that number can result in weight loss. And I told him, I wanted to lose weight. This was before my stroke, mind you. So under about November, December of 2011, we were talking about these things and I started losing weight, I think I’d actually lost about five or 10 pounds before the stroke. and subsequent to the stroke.
Now, the numbers have changed a little bit because of you know, different things related to work recently in the last year. But at my peak, I’d lost 80 pounds. Simply by watching my dog consume fewer calories than then, I burned. And understanding that I knew my BMR or rate was was my BMR was 1600. So if I, if I burn 1600 calories by doing absolutely nothing, then that meant that if I were to consume less than that, and if I would have burned more than that, then I would have the equivalent weight loss of 3500 calories a week equals a pound of weight loss. So that’s 500 calories, fewer per day, times seven is 3500 calories.
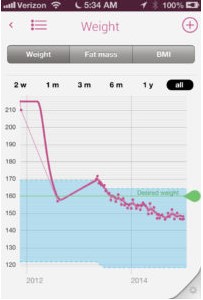
So going by that formula. I just started watching myself in the gym watching what I eat, watching the calories making sure I was burning calories. I wear a Fitbit, which is a personal fitness tracker. I wrote an article on LinkedIn about this, I have three, three tools that I use, if you can see it’s hard to see against my red sleeve. But this is my Fitbit, the pink tracker here, I use the Fitbit, use my fitness pal to track the meals I use. Yeah, I use a Withings scale, which in 2013 had just come out at the Consumer Electronics Show in Las Vegas was a brand new product, it was an electronic scale those a smart body analyzer as well.
So it told you body fat percentage, and it connected all those three connected to each other. So what I consumed I recorded in My Fitness Pal, and what I burned on the Fitbit reported to My Fitness Pal, so I had, I knew what my bonus calories to consume were for on any given day. And at the end of the day, I weighed myself on the scale. And if I wasn’t losing the wait, definitely the scale would would would show it. And the pounds were just coming down like you wouldn’t believe it, I went from 215 pounds to 140 pounds at 130 135 pounds was my was ah, I’d say 133. So eighty-two pounds total was my highest pounds lost right now I’m probably back to about 150 or so
Bill 45:27
Your wardrobe can handle any more weight fluctuations.
Musa Pam 45:33
That is correct, my highest. My largest size suit was 46. And when I started losing weight, I went down to 44. And my dry cleaner who also happens to double as my clothing adjuster, he’s got a seamstress the world works for him, really was having a hard time keeping up because I went from 44 to 42, we take it in some more, I buy some new suits, and went from 42 to 40. Buy some more new suits, take them in, and went down to 38. And I said that’s it, we’re staying at 38 whatever it is, I’m not getting any more new suits. So. So that’s where we ended up but I feel good.
The body feels good being at that weight. And even as I said the weight has crept up a little bit over over the last year. Because of you know, I’m not going to the gym as much because this little thing called work gets in the way. But it’s quite all right. I do try to I try to get at least 5000 steps a day on my Fitbit. Most days on that I’m on between 7500, 5000, and 7500, but I try to average 10,000 a week, 10,000 10,000 a day. So 7000o a week.
Bill 47:04
Yeah, that’s okay, that’s good. They’re all good numbers tell me. Actually, you know what great minds think alike. I think you’ve got a great mind. Because when I was in the hospital in 2012, it’s exactly what I started doing researching how I can lose weight and do all those types of things. And I found my fitness pal. And I learned exactly what you learned about calories in versus calories out. And for somebody who’s not very early on in the weight loss program, or process, it’s really good to just do that, because it helps you count the calories. Now My Fitness Pal for anyone listening and watching is free. I’ll have the link on the post after I upload the audio and the video. So people can go and find it.
It has a amazing little section that if you have it on your smartphone, you could take a photo of the barcode of the food that you’re eating, and it’ll tell you how many calories that portion is. It allows you to put in your age, your weight, how much weight you want to lose per week, etc. If you’re in the UK or Australia, you can do it in kilograms. If you’re in the US, you can do it in pounds. And it’s completely free, you don’t have to pay for it, which is really amazing. And I worked out that my metabolic calorie burn was around 2000 calories a day. So if I ate 2000 if I ate 1800 calories a day, and then I got up and walked
and did my exercise and did the things that are normally doing that would burn between 500 and 700 hundred calories a day, which meant I would be in a negative calorie consumption place. And as a result, the weight would come up and I did exactly that.
And I had the same problem with clothes I started off with all my big clothes becoming too big, then I went and bought mid-size clothes, they became too big. then I bought my smallest-weight clothes. And now I’m back to my midweight clothes. So the only thing I can say to you about weight loss is it can get expensive if your wardrobe has to keep getting updated. But just use the belt for a little bit longer and get somebody to decrease the size of the waist and your parents for a bit longer before you make the decision to buy that next ah next smaller size of pants or shirt or suit.
Musa Pam 49:42
Yeah, absolutely. And I’d say you know, most manufacturers have enough material to be able to take in and take out up to one or two inches on pants and suits and things like that. So so you shouldn’t have to worry too much about that. But one more point real quick on My Fitness Pal. And, you know, I’m not a paid endorser, the article I wrote on LinkedIn and I’d love to share it with you at some point because you know, interesting enough, I wrote the article at the point where I got on a scale and it said 66.6 pounds lost was mine was what my My Fitness Pal reported. And I kind of made a play on it with a joke because it was 666 and I said I’d lost I just lost the devil. Right? So it’s really true. I’m not a paid endorsement, but I absolutely believe and I would advocate for any one of those three products any day, the Fitbit, My Fitness Pal, and the whitening scale because those are three, three tools that I used to aid me in the journey because if you’re not seeing it, you wouldn’t believe it in terms of the weight loss.
And then with My Fitness Pal, I talked about my dad’s story happening in Nigeria. And obviously, if it’s not evident, I grew up in Nigeria. And there were ethnic foods that I grew up eating in Nigeria and My Fitness Pal has data on the most traditional ethnic African and Nigerian foods you can imagine with absolute accurate nutrition counts for carbohydrates and fat content and protein content. If just like any other database it built a crowdsource information from various sources. And I think it’s it’s the better everyone’s the better for it.
Bill 51:41
Yeah,
Musa Pam 51:41
so absolutely recommended
Bill 51:43
Great tool, I’m not a paid endorsement either, but it works. It’s worked for me for seven years it works for my wife works for lots of people that I know and so anyhow, enough about My Fitness Pal. This is not a My Fitness Pal ad now I want to know about your golf.
Musa Pam 51:56
Yes.
Bill 51:57
Now
Musa Pam 51:58
golf.
Bill 51:59
You wake up in the morning, and one day, you realize, oh my gosh, I can get back to Golf. But you’re getting back to Golf with a different, a different version of your golf game, because now you’re swinging with one arm instead of two tell me about the transition to that and how you had to overcome, you know, the old golf style to this to take up this new golf style. What was that? Like?
Musa Pam 52:27
Yes, so I’d say that this is this should apply to anyone with any sport or any passion that they have. In my case, it was golf, but you name it, people are out there doing it, whether it’s playing basketball with one arm, skiing with one arm or bobsledding or skating, or doing gymnastics. For goodness sake, I saw someone actually lifting about 300 pounds of weight with one arm the other day online. So anyone can do anything with one arm with whatever limitation they have. So in my case, I discovered this organization as I told you, so the ability to crowdsource the ability to be in a community of like, likely situated folks was immensely important to me, where I could see people who would, who are going through it.
There was a gentleman who was a veteran who tried to commit suicide actually shot himself in the head with a pistol and missed the most vital organs. But it left him with similar symptoms as someone who would have suffered a stroke with only the use of one, one side of his body. There was a gentleman whose arm was who’s on had to be amputated because it was, it was caught up by a crocodile while he was a crocodile hunting in the Amazon forest.
Finding your strength – Musa Pam

Musa Pam 54:15
There are folks as I mentioned, who’re born with one arm, people with industrial accidents and motor vehicle accidents, etc. Anyway, so being in that community was very helpful as a motivator for one to tell you that you could put your mind to it. Think back to the motto I mentioned about Spaulding Rehabilitation Hospital in Boston, find your strength, all of those people helped you find your strength. And the motto of NAOAGA, the North American One-Armed Golfer Associate Association is never quit.
So whenever you put your mind to something you say to yourself, I’m not going to be able to do this, just, think about the motto never quit. And it never fails. You think about that model, you can do anything and accomplish anything. So being amongst those people helped when I saw that, it was something that was possible. And then came back home. And went back to Spaulding, Spaulding has an adaptive sports program, which I’m sure is available in any community around the world with maybe associated with healthcare organizations or rehab organizations, but adaptive sports programs help you do anything within yourself to be able to play sports, the sports that you love with the disability that you may have.
And BITS is another acronym. Back in the swing B I Ts was a program that was being taught by a PGA Tour teaching professional who specialized in working with adaptive athletes. And I attended a few sessions over that summer, where he was going through the fundamentals of the golf swing when you only have to use one arm went over the fundamentals went over the basic swing. And I thought I got it. I went back to my home course and started working on my one-arm swing and went back to went back to our next tournament the next year.
Bill 55:54
How exciting is it when you went back? And first stood on the golf course and the club. And you know, you realize well, like it’s gone down the course?
Musa Pam 56:08
Yeah, it was I’d recommend that it happened in a controlled environment. And luckily for me, I mentioned Tyler McCarthy, who’s now a DPT, the way DPT is a Doctor of Physical Therapy. So he’s gone from in the seven years since my stroke. He’s gone from a physical therapy assistant, someone who was in college at the time to where he’s actually earned his doctorate degree in physical therapy today, but I credit him with the opportunity for me to as we were talking about my passions, we discovered that we had a shared passion around golf.
He told me that he was he’s a phenomenal golfer got a beautiful swing, we decided that we would go out on the golf course after working inside of the rehab center setting as part of the rehabilitation program at Mass General at Patriot Listen, for Spaulding was there there was a controlled environment where they had golf clubs where you could swing on a mat inside of the cage in a controlled setting on them. We went from there to the golf course and of course, I stumbled a bit I had a lot of missteps mishaps Miss swings, but just being out there for the first time was an unbelievable feeling to be able to reconnect with your passion bill.
Bill 57:24
Did you wear the crazy golf pants that you see some people were around the world with checkers and different colors and all that kind of stuff?
Musa Pam 57:33
You must have been sneaking around my Facebook and Instagram pages Absolutely. Loudmouth Golf is a manufacturer again not a paid endorser. Another one is the John Daly pants as in he actually thinks he was an endorser of loudmouth golf but the very loud very bright golf pants absolutely love that if you see any my if you see any of my pictures playing golf or being around the golf course, you’ll probably see a very bright color or two or three or four more
Bill 58:07
I’ll be sure to add some of those photos to the post when I finally edit it and get it up on the website. And I think I think that’s the beauty about golf is that it seems such a serious and you know you’re not allowed to speak if you’re in the crowd you know, you have to whisper if you’re a commentator you know that kind of stuff but you can wear the craziest pants that anyone has ever seen. And everyone thinks Yeah, that’s normal, no problem.
Musa Pam 58:34
Absolutely no problem at all. At some of my now granted the American golf players are some of my favorites of all time, but I’ve really I really grew up, really appreciate a lot of Australian golfers.
Top amongst them was Greg Norman. And I got to follow Aaron Baddeley. And I Adam Scott and Stuart Appleby, Robert Allenby, Geoff Ogilvy a number of Australian golfers who were just phenomenal golfers I’ve followed over the course of, of, of my golf, my golf career. And I would be remiss if I didn’t put a plug-in here. I didn’t have to even mentioned to him that I was a stroke survivor. But two years after my stroke, I was fortunate to have met Tiger Woods and I’ve got a picture of him to prove it and show for it
Bill 59:32
Yeah, isn’t it amazing golf, I know, he went through a few personal issues. But when you watch the guy play golf, the things that he was able to achieve are just unbelievable. So to be inspired by somebody like that is a really good thing. It’s great when you can look up to other people. So that’s what I recommend for stroke survivors, you know, look up to somebody who you think is an amazing person and somebody that you’d like to mimic. And if you don’t like to mimic, you know, everything about them just mimic their desire to play a good game, or their desire to, you know, be better at this sport or their chosen, you know, passion or whatever that is.
And in Australia that definitely is a community of golfers who played and are disabled in some way, whether they’re amputees or suffered another injury, like like you mentioned, and I’m sure there are many, many around the world. So just get googling guys, whoever’s listening, who wants to be involved in something like that. And if you’re not into golf, if you’re not a keen golfer, then there are other communities that Paralympic communities, for example, local communities that allow for, you know, wheelchair, wheelchair basketball, wheelchair tennis, you know, all sorts of amazing things to get people out there and get active and amongst others people in the community,
Musa, I’m really keen to follow your, you know, golf career, and keep up to date with what it is that you’re doing. As we wrap up this interview, I just wanted to ask about work. How long was it before you got back to work? And how did you find that transition? into getting back to work?
Musa Pam 1:01:30
Great question, Bill. And this is one of the questions that I mentioned when I volunteer at Spaulding rehab hospital as a way of giving back and ending up paying forward it. And if I were to leave a message with folks here tonight, it’s to try and find that opportunity tonight for me this morning for you and Australia, right? Is to find that opportunity to pay it forward. If you can, to help tell the story tell, educate someone helps uplift someone. So when I do it, as a volunteer, I do it as part of a group of peer visitors, where we go in and we visit with patients and help them by telling our story to them and hoping that in some way that it might inspire one or two or three of them to, to, to look at us and say you know what? recovery as possible, and that we’re able to, we’re able to do things that that we put our minds to, but absolutely taking, taking the opportunity to learn as much as possible. Taking the opportunity to give back. I think it is important. It is vitally important.
Bill 1:02:43
How was it? How was it that you got back to work? Were you able to have enough time off work to heal and recover and then transition back into your job? What was that like?
Musa Pam 1:02:55
Yeah, so I was fortunate that I had the flexibility to be able to work from home for a period of time, I had enough sick days, built up with my company at the time. So I had about 51 sick days available that I could use. So for the first two months or so, I was able to use those sick days, 30 days in the hospital and about 30 days at home. And then I began to work from home. and slowly transition. So the reason I started talking about what we do and Spaulding as volunteers is we put together what we call the list of most commonly asked questions by stroke patients that we visit stroke survivors, one of the first questions is how do you get back to work?
- How do you get back to driving?
- How do you deal with relationships with close loved ones?
- How do you manage depression?
- How do you manage anxiety?
- How do you deal with stress and all of those types of things?
So going back to work was what is one of those very common questions that were asked and that we deal with. And in my case, I was fortunate, that I had the opportunity to have a flexible work arrangement where I could work from home. And then when I began to drive, I was able to drive to the various locations I had, I had a job that required me to drive to a number of different locations on a daily basis. But I was fortunate to be able to transition. So my stroke was in January by July, actually, by May, I was driving. And by June and July, I was visiting my accounts already. So within six months, I was back into driving, doing the one-arm thing driving, driving like a road warrior.
Bill 1:04:43
Awesome. But it’s really a pleasure to get to know you over the internet here for an hour. Today, I really do appreciate you getting in touch, I really appreciate you sharing your story, and making it possible for other people to hear, you know what’s possible for them. And I really love that you’re passionate about your golf and that you’ve read discovered golf and you went back to it and it was, you know, something that helped you in your healing and help you overcome your, you know, your challenges and the things that stroke patients go through.
And I am really, really happy that I hear when people feel the need to support others in the community that are going through something similar and have been through before us. Because saying somebody like you standing there, after, you know, they’ve experienced potentially what’s the worst day in their life, you know, looking up out of a bit, I think immediately offers hope to say, oh, okay, he was where I am. And now he’s there. It was X amount of years ago, but that’s actually where I could be. And I think that’s one of the most important things in our community to do is support each other, isn’t it?
Musa Pam 1:05:56
Absolutely it is. Every time I celebrate what I call us stroke-a-versary are stroke averse, re is the anniversary of our stroke, I think about the blessings that I certainly have been fortunate to have been to have experienced and encountered since that stroke happened. And it always helps me renew my commitment to give back and on my behalf, I’d be remiss if I didn’t thank you for what you’re doing and what you’ve done to really help elevate the opportunities there are for stroke survivors to live meaningful and prideful and important and engaging lives whatever people want to do, they can put their minds to it and they can do it because they’re hearing from you and they hearing stories about other people they channeling through your podcast. So I really appreciate everything that you do build not just your Podcasts, but all of the literature, everything that you’ve done around stroke for survival. So thank you.
Thank you, Musa.
Intro 1:07:07
Discover how to support your recovery after a stroke. Go to recoveryafterstroke.com






