Peter Cass lived with Atrial Fibrillation which caused a stroke at age 60. In our interview, we discuss his journey and how his recovery is coming along 5 years on.
Highlights:
01:27 Introduction
02:20 Stroke And Atrial Fibrillation
08:07 Prescription Medication Caused The Stroke
14:49 Peter Cass’s Post-Stroke Deficits
23:47 Vision Problems After The Stroke
30:05 Stress-Related AF Instances
40:55 Post-traumatic Stress Disorder
48:35 The Emotional Recovery
56:14 Restoring the Gut Walls Could Help Save Brain Function After Stroke
1:04:20 Recovery Rate
1:12:09 Rest Management
Transcription:
Peter Cass 0:00
This neuropsychologist, she said, Has anybody ever talked to you about post-traumatic stress disorder? And I looked at her like are you crazy? I’m not a Vietnam War vet. I wasn’t in Afghanistan, having to deal with IEDs the whole time. She said, when you have a stroke when you have a heart attack when you have something like that, it’s a trauma it’s a significant trauma, and you need to do things in a therapy that also helps you cope with that trauma.
Intro 0:38
This is the recovery after stroke podcast, with Bill Gasiamis, helping you navigate recovery after stroke.
Bill Gasiamis 0:50
Hello, and welcome to episode 226 of the recovery after stroke podcast to learn more about my guests, including their links to social media and other pages and to download a full transcript of the entire interview, please go to recoveryafterstroke.com/episodes.
Bill Gasiamis 1:08
If you’d like to support this podcast, the best way to do it is to leave a five-star review and a few words about what the show means to you on iTunes, and Spotify. If you’re watching on YouTube, comment below the video, like the episode and to get notifications of future episodes, subscribe to the show on the platform of your choice.
Introduction – Peter Cass

Bill Gasiamis 1:27
My guest today is Peter Cass, who had a stroke that was linked to atrial fibrillation. Five years down the road to recovery, Peter has had to overcome much and is getting help with anxiety as well as emotional recovery from stroke. Peter Cass, welcome to the podcast.
Peter Cass 1:46
Thank you very much Bill. Nice to be here in virtual world, so to speak.
Bill Gasiamis 1:51
Nice to have you here all the way from Switzerland. What time is it there now?
Peter Cass 2:00
It is just after nine o’clock in the morning.
Bill Gasiamis 2:04
Okay. And here, it’s 7pm on Thursday. And that’s quite a time difference.
Peter Cass 2:12
Certainly is, it’s a lot of fun when we do projects in Australia.
Bill Gasiamis 2:16
Tell me a little bit about what happened to you.
Stroke And Atrial Fibrillation
Peter Cass 2:20
What happened to me was, it’s the beginning of 2017, I was diagnosed as having atrial fibrillation. And as you know, if you have that, your chance of having a stroke is increased by fivefold, I think something like that. So I was given some regular medication.
Peter Cass 2:43
And in March 2017 on a Monday lunchtime, I just started to feel really bad. And noticed that my atrial fibrillation was bad and my heartbeat was all over the place. So I drove home, excuse myself, and thought that the rest would sort that out.
Peter Cass 3:08
The following day, on a Tuesday, I spoke to my GP. And he then spoke to the cardiologist, the local hospital department that was dealing with me. And he said, there’s a possibility that we can give you what’s called a pill in the pocket, which is a medication that will you know, break the cycle with your AF and bring you back to normal.
Peter Cass 3:37
So he said, Okay, come in tomorrow, and we’ll sort that medication out for you. So I went in, in the morning, took the pills home with me and took the pills. But I was still kind of you know, working from home, so in the afternoon of the Wednesday I was actually hosting a web conference and suddenly I’m looking at the screen and I can’t see the cursor when my mouse cursor is moving to the right when I was presenting.
Peter Cass 4:07
And my first reaction being an IT person was thinking oh, the driver’s messed up or something doesn’t work. So I didn’t really you know, think about it. And then the meeting finished and I really noticed that I couldn’t see so well without of my right eye.
Peter Cass 4:26
So I sat down, had a rest and I thought to myself this is interesting because I know these tablets that I was given and taken strong. So I just took it easy really. mate of mine was coming around to watch the Champions League. So I decided that beer wasn’t on the menu for me that night if I was feeling a bit dizzy.
Peter Cass 4:53
And when he came around, I got him to read the instruction of the leaflet that comes with the drugs which is printed so small, it’s hard to read, and I really couldn’t read it. Though my eyesight is pretty good. So he read it, and he saw that it said, you could have as a side effect blurred vision, and you could also have slurred speech.
Peter Cass 5:19
So I didn’t think too much about it. The next day, I called the doctor and I said, now I’m having these problems. Do you think it could be the side effects of the medication or something else? And he said, that sounds like the side effects of the medication. And he said, then on the following day, if you’re not feeling better, then come to the office, I won’t be there but someone else could look at you.
Peter Cass 5:46
And my wife at lunchtime said to me, you know, your speech is slurred sometimes. And I speak two languages. Obviously, mother tongue is English, but I’m also speaking German. And with her, I speak English and her English is very good. And I thought, yeah, this is interesting. I’m really looking forward to going to the doctor the following day, which I did.
Peter Cass 6:15
And I was seen straightaway, saw another doctor who did some tests with me, you know, the typical stroke, things like balance and that kind of thing. Right! You’re going to hospital now to emergency I think you’ve had a stroke. And of course, in my mind, I’m thinking stroke, you know, half the body on fire, terrible pain, all these other things, because that’s my kind of layman’s knowledge at that point of what a stroke is like.
Peter Cass 6:43
So I’m thinking, how can I? I can’t have had a stroke, that cannot be that I had a stroke. So I went to the hospital. And I had a scan. And then the neurologist showed me the damage on the pictures. And indeed, I had had a stroke, probably on the Wednesday after I took those tablets.
Bill Gasiamis 7:10
Wow. So how old were you at the time?
Peter Cass 7:15
How old was I? I’m 65 now, so I would have been 60.
Bill Gasiamis 7:22
Are you doing in your mind after that amount of days elapsed when you finally found out? Are you kicking yourself? How are you responding to the fact that you waited so long to do something about it? You’re giving yourself a hard time. How does that go?
Peter Cass 7:41
I think I was giving the doctors a hard time. The first opportunity, of course, I said to myself, well, I should have insisted on going to the doctor earlier, as soon as I had those symptoms, but, you know, you tend to trust healthcare professionals. And I thought, if he says this is a possible side effect, and then it probably was.
Prescription Medication Caused The Stroke
Peter Cass 8:07
And of course, actually, I met the cardiologist some months later. And he knew when I walked through the door, I was going to ask him, I said, could the medication you gave me has caused the stroke? And his answer was in German, of course, but it’s basically, Mr. Cass, you were very unlucky because on very rare occasions, this drug can actually cause problems and loosen up, let’s say an embolism that you have in your heart. So I would say the likelihood, which is positive and negative, was that the medication caused the stroke, but I would never get that from the hospital or from the cardiologist.
Bill Gasiamis 9:01
In hindsight, do you wish that they had said that and you think that would have made a difference in your decision to take the medication? If they’d made you aware of that potential risk?
Peter Cass 9:15
It would have been a consideration. I mean, if I believe what I’ve read afterwards about that drug, it is a very, very rare occurrence, you know, less than one in 1000. So everything is a gamble, when it comes to it, especially with medical treatment and with medication as you know.
Peter Cass 9:34
I tried to keep myself informed. I’m probably a pain in the rear end for doctors because I have worked for pharmaceutical companies years ago. So I consider myself to have quite a good knowledge level. But yeah, maybe I’d have havening I’d have thought about it. But I guess at that point in time a stroke was a million miles away from my thoughts, you know, it wasn’t really something that I could consider would happen.
Bill Gasiamis 10:06
Had you ever known anybody to have had a stroke?
Peter Cass 10:11
Actually, no. And of course, the funny thing is, well not funny,but in the last five years, you start to network with people, actually, a very good friend of mine has had a very, very bad stroke. So I thank myself, I’m grateful every day, of course, that I didn’t have anything serious.
Peter Cass 10:35
However, on the other hand, what I feel is that, you know, a lot of people who have long lasting physical problems as a result of having a stroke. You know, it’s much more serious. But when you have one of these silent strokes, the problem is no one understands it.
Peter Cass 10:54
Because, you know, when I called at work and said, You know, I’ve had a stroke, and it was like, can you walk? You know, and when people came and visited me in hospital, I’d go and walk to the coffee area with them. And I think they found it hard to believe I’ve had a stroke.
Peter Cass 11:09
And to be honest, in the beginning, before I understood more about it, I found it very difficult to believe that I’ve had a stroke, because I’m in hospital in the stroke unit, you know, wired-up, monitored and everything. And besides a few problems with my heart and my blood pressure, I didn’t feel you know, bad.
Peter Cass 11:29
I felt like a fraud, if that makes any sense, you sort of thinking, well, you know, it has, this really happened. And, of course, the evidence was there that it had happened. And then I started to notice what the problems were at least in short-term.
Bill Gasiamis 11:44
Yeah, well, I can completely relate to that part. So my first incident was a bleed in the brain. And it took seven days for me to go to the hospital. And I was walking differently. And my wife noticed that and she told me about it, and I ignored it. And my chiropractor told me and I ignored it. But when I finally went there, and they gave me some medication to decrease the inflammation in the head, I was up and about and walking normally. And you couldn’t tell I was in my football gear.
Peter Cass 12:20
When you say football, which kind of football? Because you have so many different types.
Bill Gasiamis 12:25
Round the ball. And of course, I wasn’t in boots or anything, but just shorts and a T-shirt and running shoes. And then people would come to visit me and I would be down with them in the cafeteria. And I’d be walking all over the hospital telling them what they’re doing to me and all that.
Bill Gasiamis 12:48
And people you could tell they couldn’t compute it, because there was no visible signs. And I was being told constantly stay in your bed, Do not wander around the hospital, by the nurses, the doctors, they kept looking for me, they kept trying to bring me back. But I just didn’t feel like I needed to be there.
Bill Gasiamis 13:06
And I didn’t realize how serious it was until six weeks later, when I was supposed to go to the follow up appointment a day before I had another bleed, which was a little more catastrophic, a little more dramatic, where it was at the point where I didn’t know who my wife was, I didn’t know my name.
Bill Gasiamis 13:25
So I had a long winded recovery from that portion of the bleed. And the other thing with me was they never called it a stroke, because it was an arteriovenous malformation, which is technically a tumor, which is inside your head, which bled, it’s technically not an ischemic stroke, and it’s not an exact hemorrhagic stroke.
Bill Gasiamis 13:52
So for many years, they actually didn’t call it a strike. And I wasn’t traded by the stroke department, if you like or wasn’t in the stroke ward. And, I couldn’t relate to anybody because I didn’t know where I fit in. I had all the neurological symptoms that stroke people had, I had fatigue, I had all these things, the first time I realized that, I could say that I had a stroke for lack of a better label.
Bill Gasiamis 14:22
Was when I when I read it on the Stroke Foundation. Australian Stroke Foundation page, that I had a brain hemorrhage and they classify that as a hemorrhagic stroke. So when you’re saying you felt like a fraud. I felt like I was explaining myself to people who weren’t believing me who downplayed the seriousness of it. And I couldn’t convince them otherwise.
Peter Cass’s Post-Stroke Deficits
Bill Gasiamis 14:49
And it was a really challenging thing to bring people on board so they can understand what neurological problems I was facing cognitively, emotionally, mentally, a whole gamut of issues, right? But I couldn’t get people on board. So what were you left with? When you were discharged from hospital? How long did it take to get discharged?
Peter Cass 15:20
Well, I was in hospital for six days. Of course, I’ve mentioned the vision problem. But within two or three days, I was still using my iPad, I was using my phone, sending texts and things straight away. But the right half vision on my right side, it was like someone just cut the screen about 20%. And that last 20%, I remember watching football.
Peter Cass 15:49
And whenever the ball got played, from the left to the right, I was having to turn my head to follow the ball. You know, it’s normally you sit in front of the TV. And so there was definitely a vision problem. What I began to realize forever soon after, and I didn’t hear about aphasia for probably two years after my stroke, was that I was writing sentences, in text or whatever, missing out words using the wrong words.
Peter Cass 16:21
And that became very apparent. And also, I was struggling sometimes to read. I’ll give you an example, I was probably two days in, I was reading the BBC News on my phone. And I came across a word, which I didn’t understand. And that word was M A, R, C, E, L. Marcel. It’s a person’s name, a very common name here in Switzerland, actually.
Peter Cass 16:48
And I found myself reading M A, R, C, E, L, what does that mean? M A, R. C, E, L, about the third time, Marcel. And then I realized I had problems with certain words, let’s say where the pattern is, you know, when we read, we don’t really look at every letter. So through, thought, trough words with similar patterns, I was having to think consciously about the context of that word, if I was reading something and which word it was.
Peter Cass 17:27
Which is completely stupid when you think about it, but then I realized that, you know, the linguistic center of my brain had been affected, and it still is today. So if I write an email, I will check it more than I used to, I think anybody who doesn’t check what they write is an idiot sorry. So you should check it at least once.
Bill Gasiamis 17:50
Thank you.
Peter Cass 17:52
But, you know, I found myself checking it three times, when I look back at some of the texts I sent, which I still got WhatsApps on my phone. When I was in hospital, I’m surprised at how few errors there were actually, but missing out a word completely.
Peter Cass 18:08
And if I may, I’ll give you a bizarre example. Later, when I was back at work. We had decided to give me less responsibility in the business and to hire a successor because I’m just about now going to retire fully. And we had a meeting with our I’m in it, and we do software projects, we implement software throughout our companies.
Peter Cass 18:37
And I had to introduce the guy who was taking over my department. And his name is Maxim. And I introduced him as Sasha. Now, I know two Sashas, they don’t look anything like him. Totally bizarre, where the hell does that come from? And people looked at me like, really weird, you know, are you drunk or what’s going on?
Peter Cass 19:05
And then we had a good laugh. And actually very kindly, he adopted Sasha as his nickname. So we know him in the company that people that work closely to him refer to him as Sasha. But it was just bizarre things like that. And that still happens, I will use the wrong word. And have no clue. So I left the hospital with a vision problem and an awareness that I had these linguistic problems.
Peter Cass 19:39
All the tests I had, I passed quite well in mathematics, and you know, on screen testing and eye coordination, everything was pretty good. But I left hospital after six days with still a vision problem. And with this linguistic problem, and vision got better After two or three weeks, but the linguistic problem is still there, from time to time, Fred Oh, sorry. It’s Bill.
Bill Gasiamis 20:11
Yeah, I understand, I got left with. I struggle with wear, where, and ware? Yeah. And sometimes I can spend way too long on trying to work out when to use which word. And then other times, I won’t spend any time on it. And I’ll completely get it wrong. And I’ve done that a fair few times on Instagram where I ask questions of people. And I’ll use the wrong (where), and then I’ll post it. And then my wife will notice it after I’ve posted it. But 10 people have responded to my question. And then I can’t take it down I’ve got to leave it there.
Peter Cass 20:48
Yeah, sure. And I think the other thing is that in today’s world, especially with AutoCorrect, which probably you should switch off because the AutoCorrect, I wrote someone the other day and didn’t notice, in a WhatsApp, I basically wrote a sentence that was pretty much nonsense, or didn’t understand, and I wasn’t careful enough, checking it.
Peter Cass 21:17
So then there are some things also long-term, which could possibly be a result of having a stroke, where no one’s really willing to sort of nail it down and say, that’s absolutely because you had a stroke. And that is when I go walking. Or when I went walking originally, and the back of where I used to live was very nice hills and woods, go up there. And I started to be more breathless.
Peter Cass 21:49
And then they did an angiogram. And I think the cardiologist in my hospital had to go somewhere else for the angiogram, for whatever reason, the cardiologist in my hospital, thought that, you know, he’s going to find clogged arteries, and that we’re going to put a stent in or something straightaway, actually, it turned out that I was in quite good shape, much to my surprise and amazement for someone who’s overweight.
Peter Cass 22:15
At that time, still middle aged. But they didn’t really find anything wrong. And the cardiologist at that hospital, said to me, he’d had a number of stroke patients who had similar experiences, where he believed it was to do with the dilation of the capillary arteries in the lungs, and they needed some help.
Peter Cass 22:39
So that you didn’t get breathless, and I’ve had medication since then. And sometimes, for no apparent reason, this kind of, you know, challenging breathing, pops up. But my rehab lady really showed me some deep breathing exercises that helped me get more oxygen, even when I’m walking around, you know.
Bill Gasiamis 23:05
So, a result of the stroke, it’s impacted your ability to take a proper breath. Is it a neurological issue?
Peter Cass 23:16
I think that no one knows. And I wouldn’t say that I know better than the doctors. If you ask one cardiologist he would say basically, that’s rubbish that that could have impacted that. And asked him the other cardiologists was the guy who suggested it to me. And I found that there’s a lot of research, interestingly, there’s research in Australia about it, to try and measure the correlation between these kinds of breathing difficulties afterwards for people who’ve had strokes.
Vision Problems After The Stroke And Atrial Fibrillation
Peter Cass 23:47
So, again, you know, and I think I mentioned to you once we were chatting, I recently had my prescription changed on my right eye. And I’ve always felt that since the stroke, I didn’t see so well in the right, which was the one that was affected immediately. And actually, the strange thing is when the opticians measured it or the eye doctor measured it didn’t find really anything wrong until recently, when they said yeah, there is a weakness there. And we have to change prescription.
Bill Gasiamis 24:21
Yeah, I know that it we can’t blame everything to the stroke and it might not be related. The interesting thing though, is that well, the heart is part of the autonomic nervous system in that it beats kind of independently of us. It doesn’t really need us to be it beats on its own, however, you know, communicates with the rest of the body and then there’s a part in the brain that creates communication between the brain and the heart and that kind of says, you know, okay, we’re beating and do that and if that part of the brain is damaged or is not there anymore.
Bill Gasiamis 24:59
Then the heart stops. And that’s, you know how, for some people, you know, brain challenges, whether they are ischemic or hemorrhagic strokes can cause the heart to stop. So, to me, it kind of makes sense that there is a plausibility to your condition that it might be related, but at the same time, we don’t know, maybe it doesn’t matter if we know or don’t know.
Peter Cass 25:26
This is exactly what the cardiologist said, you know, all these things be linked together, and you could have an impact. And we just like, I will never know whether the medication really caused the stroke or not, I will probably never know about the other things.
Bill Gasiamis 25:45
One of the things about medication I know with a lot of my female guests I’ve had on the show, or who have been taking the pill, the, you know, for a few a few times, you know, for medical reasons, yes, some of the ladies are taking it for, you know, birth control reasons. And, often, and they’ve had a stroke, for example, and then often, they later learned that the birth control medication can potentially put women at greater risk of ischemic stroke. And all of them will go back to their doctors, if they ask the question, you know, the doctor says, look, it’s a risk, you know, it’s a very low risk and all that. But again, they just rule out the possibility that it was that or definitely that, or something else. We’re talking about young women who are having ischemic stroke.
Peter Cass 26:46
And let’s be honest, if if you read every leaflet that comes with every drug that you’ve ever taken, you’ll never take anything, and you know that there is going to be a risk of side effects. And it’s not like the nasty drug companies are making things to make you ill or have strokes. It’s just a fact that everybody’s different. And like you said, we’re totally interrelated. All these systems in the body. And, taking medication or a combination of medications can cause problems.
Bill Gasiamis 27:24
So what was the hardest part of this stroke journey for you to experience?
Peter Cass 27:32
I think, the thing we’ve already talked about the fact that other people don’t understand that there can be strokes that are less dramatic, that was difficult for people to understand. And like you’ve mentioned, you know, you have to explain to people what it is, and you have the feeling that they don’t treat you the same as they probably would, if half of your body was paralyzed.
Peter Cass 27:59
So we’ve discussed that, I would say the other thing is, you know, like the anxiety, because, you know, it could happen again, I can remember the first time I went home, I had great difficulty in going to sleep, because I thought I would just would never wake up again. And that anxiety stays with you.
Peter Cass 28:24
Tried to address that to a certain extent, by having some therapy and learning to do yoga nidra to on a regular basis to you know, help you relax and whatever. I think fatigue is is one thing, and also probably coping with stress. I gave up some responsibilities was, which was exactly the right thing to do.
Peter Cass 28:50
I have still a lot of responsibility. But, you know, I found I couldn’t deal with stress. And it’s interesting that since the stroke, I’ve had three instances with bad instances with atrial fibrillation, where I’ve had to have a cardioversion, which is they put you out, put a defibrillator on special one and give you a shock, kick everything back.
Peter Cass 29:16
And the first time I had that done, of course, I was terrified when I had experienced it and had it repeated, you know, I was comfortable with it. But you know, those instances could happen. And you know, when those instances do happen, that then possibly it would, you know, create the right circumstances or conditions to have another stroke.
Peter Cass 29:42
And the interesting thing is those three instances, they have always been kind of stress-related. One was the day that we moved apartment. Another one was on a very rough flight from the UK back to Zurich. Really bad turbulence and I was sick, had some sort of fluid type thing.
Stress Related AF Instances
Peter Cass 30:05
And so mostly the the AF instances were related to stress. So I haven’t had one now in three years, but they adjusted my medication. But again, you know, these things are all linked. So you’re thinking, if you have one of these instances, you’re thinking, you know, now I’m prime territory for a stroke again.
Peter Cass 30:27
So of course, that’s very worrying. But I’d summarize in fatigue, coping with stress. And these long term linguistic limitations or instances, I think, it’d be very helpful to talk to other people in support groups and read other people’s experiences.
Peter Cass 30:52
Because that helps you also understand, you know, you’re not alone. And there’s lots 1000s Millions of people around the world who have same experiences. But yeah, I think I’ve also changed certain things in the way I behave. Probably kind of quite a while I think I’m probably quite a direct person, and also a chatty person tend to talk too much. But I, I would say I don’t suffer fools gladly.
Peter Cass 31:22
If I see a situation in a conversation in a business or in a meeting, and I see that someone is stressing me out, because we’re discussing something for the 50th time, then I tend to be less tolerant, and just say, Come on, look, we’ve discussed this enough, let’s make a decision. Let’s move forward. And I think my threshold, if I’m allowed to say, my bullshit threshold has changed, it’s a lot lower than it used to be.
Intro 31:50
If you’ve had a stroke, and you’re in recovery, you’ll know what a scary and confusing time it can be, you’re likely to have a lot of questions going through your mind, like, how long will it take to recover? Will I actually recover? What things should I avoid? In case I make matters worse, doctors will explain things. But obviously, you’ve never had a stroke before, you probably don’t know what questions to ask.
Intro 32:15
If this is you, you may be missing out on doing things that could help speed up your recovery. If you’re finding yourself in that situation, stop worrying, and head to recoveryafterstroke.com where you can download a guide that will help you it’s called seven questions to ask your doctor about your stroke.
Intro 32:34
These seven questions are the ones Bill wished he’d asked when he was recovering from a stroke, they’ll not only help you better understand your condition, they’ll help you take a more active role in your recovery, head to the website. Now, recoveryafterstroke.com and download the guide. It’s free.
Peter Cass 32:54
You could say that I’m less patient, perhaps. But I just realized every minute that I live is valuable. And going round and round in circles in a business context is not valuable. Let’s get on with it. And let’s make decisions. And yeah, so that’s affected me a little bit. I think in the way I conduct meetings, because I have to conduct a lot of meetings.
Bill Gasiamis 33:21
What kind of level is your role?
Peter Cass 33:28
Well, when I gave up some responsibilities, the responsibility I gave up was people management. So I’m a program manager, I have several teams working for me. But they’re not people that work for me, in a line relationship, people from different teams.
Peter Cass 33:47
So I’m coordinating those projects, and guiding people see something going off track, and also have net responsibility. We have steering committees with members of our board. So yeah, but I don’t know whether that’s also getting older and closer to retirement that you tend to say things that you perhaps wouldn’t say in front of board members 10 years or 15 years ago when you wanted to keep your job with the company.
Bill Gasiamis 34:21
Get some feedback from the doctors see what they think maybe it’s linked maybe it’s not linked to stroke.
Peter Cass 34:25
Yeah exactly. But I think it’s just you want to get on with things and you want to keep things straightforward, and focus. And, of course, you have to do that because you’ve had a stroke. I don’t know whether you’ve found that you have to focus more. When you do something. You know, your attention span can be a problem. Your mind can come wander so you want to try and because of that you try and keep everybody else focused and I don’t think that’s necessarily a bad thing.
Bill Gasiamis 34:59
It’s definitely all about resources and energy and the lack thereof. And the there’s not an infinite amount of it. And I get short towards the end of the day, because towards the end of the day, I’m running low on energy. And it’s very different to what it was before my bleeds.
Bill Gasiamis 35:20
Until then I could go on and on and on. And after that I couldn’t, I had a Alea wall that I would hit. And when I hit it, it was just lights out. So if I needed to get stuff done, and you’re fluffing around, in and getting in my way to get that stuff done, before I hit the wall, then I didn’t want you to be in my way, I did want to hurry you along, I wanted you out of my way.
Bill Gasiamis 35:46
And I wanted to get to my destination so that when I did hit the wall, I could sit down, rest, recuperate, and get ready for the next day. So a lot of other stroke survivors report that they don’t suffer fools as much as they would have previously.
Bill Gasiamis 36:06
And they also report that whole Well, perhaps that lack of patience, but I think it’s more fine tuned than being impatient. I think it’s them being totally aware of the fact that they’re running out of resources, and you’re, and that interaction is chewing up valuable resource, and I need to keep moving.
Bill Gasiamis 36:31
And I think the more we get better at talking to other people about our stroke and telling them what happened to us and how we’re different compared to them, or how it’s changed. I think we could get away with decreasing the amount of time it takes to get to the next part of the conversation. And people, most people will come on board, and they’ll appreciate that. But if you’re also coming across differently, and people are experiencing differently that might set other people off to think oh Peter’s being a bit of an ass.
Peter Cass 37:06
Yes, absolutely.
Bill Gasiamis 37:07
Did you get any of that pushback? Did people misinterpret your lack of well, time with them as you having changed as a result of your stroke?
Peter Cass 37:24
I think that, you know, incidents that I can remember very clearly was that of course, I’m talking in two languages. So if I’m talking in German, maybe I have more of a struggle to find a word. But I have people finishing sentences for me. And that just really annoyed me and pissed me off to be honest.
Peter Cass 37:47
And I remember saying once to quite senior people, hey, please just give me a few more seconds to think and process. Don’t finish off my sentences. But I know that the bad habit I had before the stroke was sometimes finishing off other people’s sentences, not people who have had strokes.
Peter Cass 38:08
So yeah, I think fundamentally, you’re not changed. And I have to say, this may sound weird, but there are some benefits. Because I found when I had the stroke and was going through recovery, I learned from the professionals that I was working with, but also from studying and reading much more about the way that the mind works.
Peter Cass 38:36
And that was a curious thing. But we never really we take it for granted. And suddenly you start to think more about mind, and emotions and that kind of thing, and how that’s all connected. I don’t know whether other people experience it.
Peter Cass 38:55
But right after the stroke, I found that my dreams, I was very often dreaming about my late childhood formative years. You know, they talk about when you die your life flashes past before you. And it was almost like when you have some kind of trauma, that you have a similar thing and you dream about when you were younger.
Peter Cass 39:17
And I think one thing is very important was when I think during the pandemic, I said to my doctor, I said, look, I’ve had no assessment. I’ve had no follow up. I had nine months of going to a rehab place. We’re lucky to have a very good one close to us. People come from all over the world. 7:30 on a Monday morning, I went there on my way to work, spent an hour with my therapist.
Peter Cass 39:45
She was excellent. And suddenly at the end of the year, it’s like okay, now with health insurances. you’ve recovered. I don’t you don’t need that anymore. And then after a couple of years, I was asking my doctor hey, isn’t someone gonna do some kind of assessment to see what’s going on.
Peter Cass 40:06
And he sent me to a psychiatrist who the first meeting said, I can’t believe they haven’t done an assessment on you. And he sent me to a neurophysiologist. And I spent the day with her doing all these kinds of tests. And what was encouraging, because I had a kind of benchmark, you know, she said a lot of things for your age, you’re better than average.
Peter Cass 40:28
There’s a lot that’s in the zone for your age. And there are one or two things like particularly hand-eye coordination, which I’ve never been good at which scores are a bit low. But that gave me kind of a benchmarking. Because I think it’s very difficult for you yourself to judge, you know, where you are in the journey. You need something to hold up, you know, like a map and say, Okay, I’m there, and they’re in there.
Post-traumatic Stress Disorder
Peter Cass 40:55
And that was really useful. But this neuropsychologist, she said, has anybody ever talked to you about post traumatic stress disorder? And I looked at her like, Are you crazy, you know, I’m not a Vietnam war vet, I wasn’t in Afghanistan, having to deal with IEDs the whole time. And she said, when you have a stroke, when you have a heart attack, when you have something like that, it’s a trauma, it’s a significant trauma.
Peter Cass 41:26
And you need to do things in the therapy, that also helps you cope with that trauma, which is actually how I ended up doing yoga nidra, she sent me to someone to do wellness based stress reduction. And she said, people who have strokes, people who have heart attacks, people who have terrible car accidents, there are a lot more people who are traumatized than anybody realizes. And so that was actually helpful to understand that. And that certain of these behavioral things were very typical.
Bill Gasiamis 42:07
My wife would say, after the second bleed, I couldn’t finish sentences, I was vague, a lot of the time I’d start a sentence and then not even know what I was talking about. I couldn’t type an email, I couldn’t do calculations. You know, there’s so many things that I couldn’t do after the second bleed. And I had I had a counseling session with my den psychologist.
Bill Gasiamis 42:35
And she said, has anyone suggested a neuropsychologist? And I said, No, I don’t know what that is. And it was because of her that I then went and asked for an appointment for Neuro Psych. And that’s the only reason why I got one and followed up. And like you, it seemed like, it wasn’t even worth mentioning to me, it wasn’t a priority for my doctors to allocate me one or to make an appointment for one.
Bill Gasiamis 43:05
But they also didn’t feel the need to tell me. And I’m not sure why that is because I clearly struggled with a lot of things after that second bleed and for many, many months, nonetheless, I went to the neuro Psych. And it’s exactly the relief that I got, I got to learn where I was at. And then I’ve got to be able to reflect. And my counselor, my psychologist would say to me, Hey, also, do you remember, when you came in last time, you couldn’t complete a sentence or you couldn’t do this, or you didn’t do that.
Bill Gasiamis 43:38
And now you’re doing that really well. And that might be three or four sessions down. So she was doing a lot of that reminding me of how far I’d come, as well as my wife and all the other people that were around me. But yeah, how do you know, I mean, and you also got a brain that’s dealing with stroke recovery. How do you know to be your own self advocate, but you do have to be your own advocate.
Peter Cass 44:06
You can’t just sit back and say, I’m surrounded by these people, and they’re gonna take me along the journey. You have to get the map and get the compass and point your feet in the right direction. I think one of the things that I’ve learned is that it was important for me to take over control of the recovery process, and not rely on other people. Now you could say, well, that’s a weakness with the healthcare or something.
Peter Cass 44:36
Healthcare is excellent in Switzerland. But you, it’s you, it’s your brain, it’s your mind, and you need to take control and talk to the right people and do things, but you also have to listen, you know, to your partner and close friends and people like that.
Peter Cass 44:53
Don’t push yourself. I don’t know. You know, a lot of people in groups. I was saying to someone the other day you I’ve never been a sporting person, though. I love sport, football. I used to coach it. I see people who have had a stroke. And suddenly they’re doing half marathons and marathons and swimming across the English Channel, and they’re doing all these kinds of stuff.
Peter Cass 45:20
And I understand that because doing these physical things is a confirmation back to them that they’re recovering and going in the right direction. But sometimes you think you just need to rest a little bit and relax and not do so much. And that’s sometimes the message I’ve had from other people. You know, my wife says that, you don’t have to do that now, you know, you’re not feeling that great, because I had a bad virus over the summer wasn’t COVID.
Peter Cass 45:50
And after that an infection, give yourself a break, give yourself time. You know, probably with the fatigue, like you mentioned later in the day, you can’t do so much. So schedule your key activities for the times when you you know you’re at peak performance. But give yourself a break as well. And I think we want to reassure ourselves that we’ve got back to normal or as close as we can, and probably we push ourselves too far.
Bill Gasiamis 46:19
Yeah, I couldn’t agree with you more. Look, I’ve interviewed people that become ultra-marathon runners, Episode 130, I interviewed Andy Robinson. And he got into ultra-marathon running so more than 40 kilometers in one day, and just absolutely thrives on it and loves it. And it’s where he finds his meditation time, is where he, you know, uses all the skills to overcome the pain and suffering that he’s feeling in his muscles.
Bill Gasiamis 46:53
It’s helping him mentally, physically, emotionally, and all power to him. But I tell you what, I could not think of anything worse now. Maybe Andy hasn’t got some of the deficits that I’ve been left with. So you know, running is definitely difficult for me, and I don’t feel comfortable running. So all power to him. But I felt like also telling Andy like, kind of just rest up a little more.
Bill Gasiamis 47:21
Maybe it’s helping him avoid things like post-traumatic stress. So maybe that’s why Yeah, some people are doing it. Because I know movement. And exercise really does help the brain overcome. Well help with the managing of post-traumatic stress disorder.
Bill Gasiamis 47:36
You know, I interviewed Dr. John King, for episode 162. And, you know, he’s somebody who deals with post-traumatic stress disorder, not because of a stroke, because of a different life experience. But he talks about the whole process of going through an episode and all the things that help him.
Bill Gasiamis 47:59
And he didn’t know how to deal with it, he didn’t know how to get help. He didn’t know what was happening. It ruined his life, it ruined his marriage, it ruined all those things. And slowly, he’s had to take control where he could and claw back to a life that was stable, to a job to all the things that normal, quote unquote, normal in somebody’s life. But again, he didn’t come from stroke to post-traumatic stress disorder.
The Emotional Recovery

Bill Gasiamis 48:35
But he had to be his own advocate. And he knew what he needed. He also had to have the courage to go and get the help. Because if they’re an emotional recovery after stroke, a lot of people won’t go and get help. I know men are less likely to get help than women.
Bill Gasiamis 48:50
And that’s the thing that’s going to help your recovery. I spoke about it in the last episode where I did a solo episode it’s part two of my, my solo episodes, where specifically I spoke about the possibility that if you missing out on the emotional recovery from stroke, then you’re missing out, in my opinion on 1/3 of the recovery that’s required.
Bill Gasiamis 49:18
Underneath emotions, you can put spiritual, you can put all sorts of different things under that bracket. But if you’re doing the physical recovery, and you’re doing the psychological recovery, or the mental recovery, and you’re changing the way you’re thinking about your life, and you’re thinking about, you know, the negative sides, and you’re thinking about the future.
Bill Gasiamis 49:38
If you’re able to bring that around, but then you’re not doing the emotional recovery, which is heart centered work, and you’re going to be kind of behind and if you’ve never done that kind of work, because you never thought you needed to do it. Well, here’s the time where you really, really need to do it besides struggling it’s gonna take To do more than anything, and it’s going to bring all those demons that we thought we had swept under the rug, it’s going to bring everything into the surface.
Peter Cass 50:09
Yeah, because I think the physical recovery is very measurable, you know, you have metrics, it’s very visible. And I think that emotional, psychological recovery is something that’s more elusive, it’s more difficult to pin down. And I think you’re absolutely right, you need to talk to people. You know, I can think of situations where I’ve had just lost it, you know, emotionally and burst out crying and whatever.
Peter Cass 50:38
And, my wife would say, What’s the matter? And I would just say something like, I just can’t cope at the moment thinking about that. Because, you know, you have these phases where you are weaker emotionally and psychologically. And yeah okay, I haven’t had too many physical deficits that I’ve really had to concentrate on. So I’m very fortunate in that sense.
Peter Cass 51:08
So I’ve had have concentrated on the other things. But yeah, I think it’s the recovery spans a whole lot of areas in your life, doesn’t it? And, you know, there’s lots of different aspects to it. And everybody’s different. That’s the other thing. I’m sure there are people who, who just said, Okay, get on with it, I’m more or less okay and that’s it.
Peter Cass 51:36
And there are other people like me who think about things a lot, you know, and think about, where am I? And is that linked to the stroke or not. And, of course, we don’t want to make our experience a crutch, an excuse for things. But I think it’s very important that the wider community has a better understanding of brain injuries. And that’s why, you know, I’m happy to come and talk to you.
Bill Gasiamis 52:12
Yeah, I appreciate that. And hopefully, the people that know you will listen to this and get a better insight as well. And that will be really fantastic. I wanted to ask you about your friend who, you know, had a serious stroke. How are you interacting with that person now? That you’ve been on that side of stroke. And he’s been there, where are you guys at?
Peter Cass 52:40
I’m not interacting with him really at all. Because his brother is interacting with his friends and social media and emails and stuff like that. Because as a result of his stroke, and I don’t know the exact medical condition, it’s kind of his 48 is brought on like an early dementia. So he’s not only had terrible physical problems, and he was like the guy who was running half marathons while he was living in New York.
Peter Cass 53:10
I think he even ran the New York Marathon. And he’s really been hit him like a railroad train physically, mentally, or whatever. So I react with his brother. He’s a Filipino, he happened to be home visiting when he had a stroke. So at least he’s with his family, rather than in New York. So I can’t interact with him directly. And that’s, of course, frustrating.
Peter Cass 53:37
But it’s nice thing was he went on Facebook a few weeks ago and wished his mom happy birthday. And that was the first post probably in nine months or something. So I hope that I’ve helped, you know, his brother asked me a lot of questions. So I’ve tried to support his brother with some some interaction there, because he’s really in a tough space, mentally and physically, and making progress but slow.
Peter Cass 54:06
And I think he’s brother appreciated, having someone to talk to or just ask, you know, how did this work for you? How long did it take? And then, of course, I had to say, look, it’s very different. And with your brother, and it’s really a lot more serious in many ways. And you have to just stick with it and encourage him and be positive.
Peter Cass 54:33
And I think that hasn’t been easy been months since it happened. But I hope that maybe in the future he’s able to communicate more, I would love to be able to support him in and have a call with him and just really help him more. But at the moment, that’s just not possible.
Bill Gasiamis 54:50
Sounds like he’s still in the very acute stage.
Peter Cass 54:53
Yeah, absolutely.
Bill Gasiamis 54:55
He might be able to come around a little later. The fact that I’ve had a stroke, and I can answer questions for family members of other people who have had a stroke, is really an amazing thing that’s come out of stroke for me, to be able to iterate to them, something that they cannot possibly understand in any way, unless they have a stroke, which we would prefer they never ever did is something that’s amazing for me.
Bill Gasiamis 54:57
And I really get a lot out of the interactions that I have with people who are desperate, who need some light at the end of the tunnel. And that’s what the podcast is about, it’s about shedding some light and giving people the before the middle, and then the after, and then the mutch after if that’s possible.
Bill Gasiamis 55:47
So that, you know, there’s, we can, we can offer hope. And then as a result of that, I keep receiving emails from amazing friends who say, Oh, I read this article, and it’s related to stroke recovery, you know, check it out, tell me what you think. And I just received one yesterday, and one of the ones I received that it’s from an organization called technology networks.
Restoring the Gut Walls Could Help Save Brain Function After Stroke
Bill Gasiamis 56:14
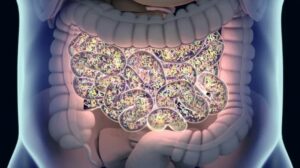
And they’ve got a subheading of neuroscience news and research. And it’s an online publication, and the article is restoring the gut wall could help save brain function after stroke. And I get encouraged, because now I hear about things and read things that are related to stroke, recovery and, and improving recovery after stroke via the gut, which is a part of stroke recovery that I’ve known about for quite some time, but there wasn’t a lot of research on.
Bill Gasiamis 56:50
So now I’ve got this group of people who know me, as soon as they come across something that’s stroke related, they share it with me immediately. And I get to increase my database of knowledge and get excited about the possibilities of this. So many people looking at stroke recovery in all these different and amazing ways. And these guys are a team of researchers at Texas a&m University School of Medicine.
Bill Gasiamis 57:22
And they’re pioneering research into the connection between stroke induced gut permeability or leakiness, and cognitive impairment. So what they’re finding is potentially that people who have a stroke also get impacted at the gut level. And many stroke survivors will report having constipation, or having some kind of an impacted bowel after stroke, and not realizing that the two are linked.
Bill Gasiamis 57:51
And then it also brings on gut permeability or leaky anus, which is exacerbated by gluten and casein which is found in milk and all sorts of other things. And now, we actually got the opportunity to support those people. Because a we have this information about a lived experience from stroke, of stroke.
Bill Gasiamis 58:18
And then we also have, I also have this beautiful network of people continuing to update me and inform me of things that I can share with other stroke survivors. So I’m going to make a link so that people can find this article, if they go to recovery after stroke.com/episodes. Find this episode. And then from there, they’ll be able to see the link and read the article. So I get that that’s the good part of stroke. And for me, stroke recovery.
Peter Cass 58:51
You reminded me of something that maybe I can share. You know, where you you have a stroke, you go into hospital, you cause you want to drink water until they know that you can swallow probably you don’t get anything? Well, during the pandemic, well, I’ve had a lot of throat problems. And during the pandemic, I went to see a specialist and he said, you know, the back of your throat where you have your vocal cords, the vocal cords are supposed to kind of fully close and they didn’t.
Peter Cass 59:29
And although at the time all the checks were done. Because that can be something that’s impacted by a stroke. And he said, well, you know, you had a stroke that could be as a result of that. So who would have ever thought that having persistent and chronic sore throats, which are related to the vocal cords could have been also a result of the stroke.
Peter Cass 59:57
So I went to like a therapist who deals with all this, you know, talking and singing speech therapists exactly, and went to her during the pandemic, which was very difficult because we’re doing all the exercises with a big screen. And then I found, for example, I can talk better, I played a guitar and sing for fun. And I found that also doing these exercises that my voice was stronger.
Peter Cass 1:00:31
So even two or three years down the line, maybe you trip up over something, and it could be related. On the other hand, you don’t want to say every time you sick every time something’s wrong, the stroke is to blame. But I think educating people like you just did you know, these problems with the gut and whatever. We don’t want to make them more hypochondriacs, but we want to make them aware that probably having a brain injury has a lot more peripheral damage than perhaps we’ve realized.
Bill Gasiamis 1:01:04
Yeah, absolutely. I mean, my brain was messed up by the blood clots that were in my head for nearly three years before brain surgery. And then it was fiddled with because of brain surgery, you know, that had to move, go into my head for about four centimeters deep, so almost to the cerebellum.
Bill Gasiamis 1:01:25
And that’ll go kind of behind my ear, and in there, on actually above my ear, and in and down and in. And they would have had to wiggle stuff and push stuff out of the way. I mean, it’s been physically it’s been handled and poked and prodded it makes sense that something that happens under conditions of surgery, that’s not at the spot of the stroke could impact, you know, the way that you experience your body afterwards.
Bill Gasiamis 1:01:57
I’ve had an eye condition, which I cannot describe, and an ophthalmologist can’t see it. But I’ve had this weird kind of flutter. In my eye that feels a bit strange. Pretty much since the brain surgery, and my entire left side is numb and I experienced it differently to my right side, it’s numb, it has pins and needles, it’s colder, it has more tension. So it’s kind of it has a little bit of spasticity, although you can’t see it anywhere.
Bill Gasiamis 1:02:32
And when my eye flutters, I just kind of put it off, I didn’t know what it was. And I couldn’t get anyone to explain it to me. And then one day only, only about five or six months ago, it occurred to me that it’s on the left side of my body where everything feels different. And if my eye feels different, that could explain it.
Bill Gasiamis 1:02:54
And there isn’t anything wrong with my vision or my eyeball, but it just makes this weird thing that I feel from time to time, especially at night. So yeah, it takes a while for things to sink in as well, sometimes that it could be related to the stroke. So I’m just I’m nearly 10 years out. I mean, I’m discovering these things all the time tomorrow. In Australia, it’s going to be Friday, it’s going to be the 25th of November.
Bill Gasiamis 1:03:27
And that is the day the anniversary of my brain surgery in 2014. So it’s been eight years, and I’m still discovering things that I’m going through. And on that note, not only am I discovering things that I’m going through that are related to the show, I’m also noticing improvements in my abilities, capabilities, my fatigue levels are decreasing, still, my energy levels are increasing still. So I want to share that as well, that eight years down after stroke surgery, more than 10 years since the first bleed, I’m noticing minor incremental changes for the positive you know.
Recovery Rate After Stroke And Atrial Fibrillation

Peter Cass 1:04:20
That’s fantastic. And I can remember at hospital the neurologist, told me one of the very frustrating things about having a stroke can be that you’re immediate recovery like my vision, I couldn’t drive straight away three weeks later, I did a test and I was able to drive.
Peter Cass 1:04:38
So right that weekend after you know when I was in the stroke unit, things began to improve. I started watching TV playing games and he said one of the frustrating things can be the rate of recovery will go from superfast. To very very slow. And that that can be frustrating.
Peter Cass 1:05:00
And you shouldn’t think as someone who’s had a stroke or brain injury, that it’s going to be like, you know the brain is rewiring itself like crazy in the first few days. And it’s not going to be like that. And I think it’s also important, like you just said, dwell on the positive as well and sort of say, you know, what is good? What can you do now that you couldn’t do maybe six months, two years ago?
Peter Cass 1:05:28
Whatever. Because of my age, you know, I’ve got the aging process going on. And that’s also a challenge, which you think, Well, you know, how much of this is just getting older, or if something pops up, you know, how much of it is to do with, with with getting older, and I think that’s, that’s also a challenge. And, yeah, of course, staying positive is, is very important. It’s not always that easy.
Peter Cass 1:05:59
I’m not a person who is really I remember years ago, when I was a salesperson in the UK, we all had to stand on the desk and say, we are the best sales person in the world. You know, it’s one of these rah rah rah all kinds of seminar events, and I just got down off the desk, and then the guy, the facilitator said, how you’re feeling.
Peter Cass 1:06:21
And I said, well, we can’t all be the best salesman in the world, you know, that’s mathematically not possible, unless we’re all equally the same. So, you do have to have a dose of reality, and be realistic. But having that positive mindset, it is also a battle to maintain that you’re going to have your good days, you’re going to have your bad days. And I think that that’s where we can gain support from the community. And people who’ve had similar experiences.
Bill Gasiamis 1:06:53
Yeah, to help bring you out of one of those difficult days, like positive mindset is not a permanent thing. Hopefully, a positive mindset is something that you do more often than not, but really recognize that it’s okay to not have a positive mindset as well, because you’re gonna go through the gamut of emotions and mindset feelings, and you got to go through it all, you got to have the ups and you’ve got to have the downs. And you got to find the balance somewhere in your own experience, because having a positive mindset all the time is not viable. It’s absolutely not doable.
Peter Cass 1:07:34
Causes you’re allowed to have a bad day as well. Sometimes you have a bad day, don’t do anything. You know, read a book, play guitar, listen to music, whatever it is, watch some crap movie. You know, give yourself a break. And you cannot maintain that level of positiveness. If it’s such a word, positivity. But you know, the whole time and if you try and persuade other people that you’re up there the whole time, come on, get real.
Bill Gasiamis 1:08:17
And that’s gonna set a false expectation. I know, there’s a lot of people that went back to work too soon that I’ve interviewed who pretended that everything was okay. And there was nothing wrong. And they really struggled to keep up appearances and pretend that everything was okay. And then only fall into a heap leader, you know, down the track.
Peter Cass 1:08:38
Yeah, I mean, I was back at work, from home 50% within two weeks, and then I guess, probably about after six weeks. it was a Monday morning, and I had my therapy. And then I agreed to meet my boss, we had a nice relaxing lunch somewhere in the shopping center.
Peter Cass 1:08:59
And then I went back in the office. And the difference I felt of being back in the office to working from home. I stayed there about two hours, and I went home. I could, and then I realized it was far too early to go back in the office. What’s nice about the home office, which we’ve all experienced during the pandemic, is that you can control things better.
Peter Cass 1:08:59
You know, at that stage, I was very vulnerable. Someone comes into your office, you have five minutes, Peter, and they’re there an hour and a half later, then you wanted to get on with something else. You were struggling to stay focused on a particular thing. What’s nice about the home office, as you can see this person is trying to call you on teams or whatever.
Peter Cass 1:09:46
And you can just ignore it and finish what you’re doing stay focused and then call that person back. Because I think that when you’ve had a brain injury, what’s very important is being organized certain patterns of doing things, they’re really helpful to you, at least I find that they’re very helpful to you. And you know, when you’re home office environment, you have much more control over that.
Peter Cass 1:10:18
Whereas, you know, you’re back in the office, and then, of course, especially because you have this invisible brain injury, then people Oh, I thought you were going to be sort of limping along or something like that. And then because people see that you appear to be normal, they interact with you normally, but you’re not ready for it, actually. And that’s, I think that’s absolutely important. You know, make these small steps going back into your work environment, don’t do it all at once.
Bill Gasiamis 1:11:00
Through just sheer ignorance, you know, I had those experiences oh you look fine. And it used to annoy me at the beginning listening to somebody say, You look fine. Well, I actually get know annoyed at that person for being ignorant about stroke and what stroke feels like, well, it’s like, come on, that I had to be okay with the fact that they were ignorant.
Bill Gasiamis 1:11:22
That’s how they were meant to be, they couldn’t possibly know what it’s like to have had a stroke. But I do love that opportunity that you had to do part of your transition back to work from home, in an environment that you could control, when you stopped for a quick rest, or when you were overwhelmed, or you can control the lighting the noise, you didn’t have to travel and therefore get fatigued in the just in the task of traveling to work and then having to try and find a way home. You know, that’s a really lovely transition back.
Rest Management – Peter Cass
Peter Cass 1:12:09
Yeah, yeah, you know, and we’re fortunate in our company, we have a quiet room, which has, you know, where you can lie down with your head slightly raised. And when I did go back in, I found that was very good. After lunch, to just be able to go there for 30 minutes, lie down, say meditate, you know, but just be quiet, not go to sleep, necessarily, but relax.
Peter Cass 1:12:36
And I found that really invigorated me to cope with the rest of the day. So I found I’ve kept that habit of having short, relaxing, breaks, or especially after lunch. And I even noticed that if I don’t have that after lunch, power, nap, meditation, break, whatever you want to call it. And whenever you want to do that I struggle then more as the day goes by.
Peter Cass 1:13:05
So I think it’s really good to do that. And I tell you, what’s, what’s great. doing that. And having that quiet time is usually where I get the best ideas and creative ideas or solving solving a problem. Suddenly, it will come to me Oh, yeah, we could do that.
Peter Cass 1:13:25
And, you know, I think we all rehearse things in our minds. We have a playbook in our minds, if something’s coming up a meeting or something like that. And those periods of quiet, especially, I think, if you’ve had a brain injury, are really valuable.
Peter Cass 1:13:43
They’re like recharging, but also, you know, you get a dose of creativity. I mean, I get my best ideas. When I wake up to go to the toilet, at three o’clock in the morning. I’ve always kind of had that. It’s weird, isn’t it? Because when you’re able to relax and you know, it’s usually then the best.
Peter Cass 1:14:03
I remember years ago, we’re reading about the Top UK businessman and he, someone said to him, in an interview said that you’re always on the golf course. He says whenever we say You know, you’re always on the golf course. He says, I have my best ideas on the golf course. If the people I’m having problems with play golf, I don’t play golf, I’ve given up trying to learn.
Peter Cass 1:14:24
He says if the people I’m having problems with play golf, we go out on the golf course and we solve those problems. So just changing the environment. And I assure you, you’re gonna say the same thing, just going for a walk in the forest, by the lake, on the beach or whatever, those things are so important.
Peter Cass 1:14:46
Or go for a walk around the factory at lunchtime outside, you know, those things are so important and anyway, but they become much more important when you’ve got a brain injury and I think by most of us have had that experience, you know, we value more, going for a walk, going for a walk, you know, looking at the woods, looking at the lake, whatever very important I think.
Bill Gasiamis 1:15:12
The benefits of exercise on the healing brain are just, I mean, I’ve written a whole chapter about it in my book. It’s just never ending when you could write forever about the benefits to the brain from exercise, and we’re talking about mild exercise, even if it’s not standing up, even from a wheelchair, you know, anything like that, really suppose the brain to recover.
Bill Gasiamis 1:15:38
With regards to what what I love is the applying kind of in my mind, I see the stagnation of being stuck in a problem. Usually, when there’s a problem. If you think about the physiology of most people, when they’re in the problem, they’re stuck, they’re scratching their head, they’re not moving, nothing is really turning over.
Bill Gasiamis 1:16:01
And then when you get them moving, and you get them actively, kind of getting out of their head, because now they have to do walking and paying attention to, you know, the path or the rocks or whatever, wherever they might be, then you’re getting out of the way of the brains getting out of the way of itself, and then allowing for things to start moving again.
Bill Gasiamis 1:16:25
And for those ideas to emerge or pop up wherever they are living, and to come into your awareness so that you can utilize them, I find that in the middle of the night, I get some ideas, etc. And you know how some people will talk about them, they’ll say they’ve got a piece of paper next to their bed, and they’ll write it down. I’ve never done that yet. So in the morning, I forget about them.
Bill Gasiamis 1:16:53
And, they’re gone. And sometimes they reemerge, they pop up. But usually I’m not cognitively awake enough to go, Okay, actually, what I need to do is go down and write it down. And sometimes, if I have gone and written it down, I’m getting, I get too excited about what I just realized. And then I can’t go back to sleep.
Peter Cass 1:17:16
Yeah, I’m a musician. And I write songs and play the guitar a lot. And after the stroke, probably only a week or so afterwards, I dreamt that I was playing with a band that I played when I was a teenager, or early 20s, probably more accurately. And I actually dreamt some words to a song. And I actually drempt a guitar riff.
Peter Cass 1:17:43
And I couldn’t be bothered to get up in the night and write that down. So I got up, it was still very present in my mind. But I was hungry. So I had my breakfast. And I of course forgot it. But what was interesting is, fortunately, it all came back to me about 10 minutes later, because I remembered enough fragments of it to do it, and then it came flooding back.
Peter Cass 1:18:08
And that developed into a song. You know, I mentioned earlier about dreaming a lot about my youth immediately after the stroke. So yeah, I think it’s creativity is very important. And whether it’s physical exercise, playing golf, playing a musical instrument, whatever it might be, those things are, of course, very, very important for the brain and also for the physical side.
Peter Cass 1:18:37
But you know, my first reaction to being told that I had a stroke was can I play the guitar or not a year before I injured my arm. And that was exactly the same reaction then. But you know, I was really concerned and I was thinking, okay, I can move I can, everything’s fine with my hands and whatever. But I was wondering, when I really start to try and play again, is something going to be limited or something I was very fortunate not to be but I think getting away from the normal environment is good.
Bill Gasiamis 1:19:11
I did an interview with Vinnie Valentino, very accomplished guitarist in the United States on episode 168. That’s a cool one. And he had an ischemic stroke. And then he struggled to get back into playing the guitar. He’s back there now. But he mentioned that he is not at his best and it doesn’t feel like he’s at his best like it was previously. But he’s managed to rediscover, you know, playing the guitar after the stroke and it was one of the things you’re worried about.
Bill Gasiamis 1:19:49
I also have a friend of mine who’s had a stroke who I met many years ago at the beginning of my journey, who actually was a guitarist and lost the ability to play guitar Because of the spasticity on, I think his left side or his right side, and then and then it took up playing the keyboard one handed. So you couldn’t really stop him from being a musician, he just evolved and adapted.
Bill Gasiamis 1:20:19
So they can still play in a band and they can still perform and write music and do all the things that he love to do he’s just doing it in a different way. Peter, thanks so much for coming onto the podcast. Mostly, thank you for reminding me that I had forgotten to get you on the podcast and to allocate time in my diary. And in my calendar. I say that because there’ll be people who reached out and want to be on the podcast, probably listening, who I forgotten to get back to or in amongst all the messages that I received, I missed out on getting back to somewhere.
Bill Gasiamis 1:21:01
So if you’re one of those people, and you’re listening, or watching, reach out, and let me know that I’ve forgotten. I’m very happy to receive your reminder. And we’ll do it. And we’ll definitely get on the podcast. In the meantime, Peter, I really appreciate your time and best of luck with your continued recovery. And thanks for choosing to be on here.
Peter Cass 1:21:25
Thank you very much. And I appreciate very much what you’re doing. You know, I stumbled across somewhere in social media, and I haven’t listened to all of your podcasts. But I certainly listened to some of them. And I think it’s very valuable. And I’m sure I’m not the only person who appreciates it. So thank you. And I would say good evening. Now I have to start working.
Bill Gasiamis 1:21:48
Yeah, enjoy. Enjoy the rest of your day. Thanks, Peter. Thanks for joining us on today’s episode, sharing the show with family and friends on social media will make it possible for people who may need this type of content to find it easier. And that may make a massive difference to someone that is on the road to recovery after their own experience with stroke. If you are a stroke survivor with a story to share about your experience, come and join me on the show.
Bill Gasiamis 1:22:12
The interviews are not scripted, you do not have to plan for them. All you need to do to qualify is be a stroke survivor or care for someone who is a stroke survivor, or you are one of the fabulous people that helped stroke survivors in their recovery. Go to recoveryafterstroke.com/contact fill out the form. And as soon as I receive your request, I will respond with more details on how you can choose a time that works for you and me to meet over zoom. Thanks again for being here and listening. I really appreciate you see you on the next episode.
Intro 1:22:44
Importantly, we present many podcasts designed to give you an insight and understanding into the experiences of other individuals opinions and treatment protocols discussed during any podcast are the individual’s own experience and we do not necessarily share the same opinion nor do we recommend any treatment protocol discussed.
Intro 1:23:01
All content on this website at any length blog, podcast or video material controlled this website or content is created and produced for informational purposes only and is largely based on the personal experience of Bill Gasiamis. The content is intended to complement your medical treatment and support healing. It is not intended to be a substitute for professional medical advice and should not be relied on as health advice.
Intro 1:23:23
The information is general and may not be suitable for your personal injuries, circumstances or health objectives. Do not use our content as a standalone resource to diagnose treat, cure or prevent any disease for therapeutic purposes or as a substitute for the advice of a health professional.
Intro 1:23:38
Never delay seeking advice or disregard the advice of a medical professional, your doctor, or your rehabilitation program based on our content if you have any questions or concerns about your health or medical condition, please seek guidance from a doctor or other medical professional.
Intro 1:23:52
If you are experiencing a health emergency or think you might be call 000 if in Australia or your local emergency number immediately for emergency assistance or go to the nearest hospital emergency department medical information changes constantly.
Intro 1:24:05
While we aim to provide current quality information and our content. We did not provide any guarantees and assume no legal liability or responsibility for the accuracy, currency or completeness of the content. If you choose to rely on any information within our content, you do so solely at your own risk. We are careful with links we provide however third-party links from our website are followed at your own risk and we are not responsible for any information you find there.







