Beating Locked-In Syndrome
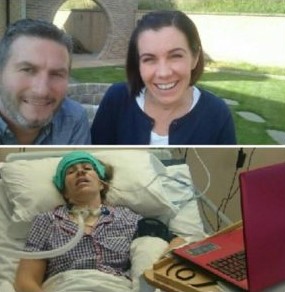
Clodah Dunlop is a police officer that experienced a brain stem stroke in 2015 and woke to find herself locked-in an unresponsive body with no means of communication other than the ability to blink.
Highlights:
01:25 Clodah before the stroke
10:32 My heart stopped
16:49 I was being held prisoner by my own body
22:07 Coming out of locked-in syndrome
27:27 Using blinks to communicate
29:42 Importance of humor in recovery
42:51 Caseworker’s bad bedside manners
Transcript:
Clodah Dunlop 0:00
It was really difficult for the first two and a half weeks all I could do was blink because my partner discovered which is very unusual for locked-in syndrome and on the first day that I was there he asked me Clodah you still there and I knew I can’t miss this chance and he said blink once if you’re there so I close my eyes and counted to three amateurs I can’t flow over my eyelids I need to get this right and so I blinked gas so he established straight on that I could answer yes and no we created a system with blinks. One blinks for yes two for no three for I love you and four for your a moron.
Bill 0:45
That’s great.
Intro 0:49
This is recovery after stroke with Bill Gasiamis helping you go from where you are to where you’d rather be.
Bill 0:58
Well, as I said, it’s really I really appreciate the opportunity to chat with you. I’ve had a little bit of a look to see some of your stuff on, you know, on the internet on Facebook, etc. And it’s a really inspiring story. And, of course, my story is similar but no, not as dramatic. Can you tell me a little bit about what you were doing before you had the stroke?
Clodah Dunlop before the stroke

Clodah Dunlop 1:25
And back in April 2015, almost three years ago today, I was a FET active frontline police officer serving Northern Ireland and then a particularly difficult area. I was a frontline police officer. I love life, and I love fitness back in April 2015. My biggest challenge then was whether Could I get a seven-minute mile down to a six-minute mile and if I could, I would join an elite department and police service in Northern Ireland fitness was my everything.
Bill 2:05
Wow. So you wanted to go for the six-minute mile?
Clodah Dunlop 2:11
Yeah, that ever had gone down to a seven-minute mile and if I had reached the six-minute mile I could apply for an elite department. The police service in Northern Ireland was a bit like I, I felt it myself was a bit of a G.I Jane.
Bill 2:31
So how long were you working in the police service?
Clodah Dunlop 2:35
And at that time I was working with a service, for eight years,
Bill 2:41
Eight years so you were fairly established you knew your job well, you were pretty on top of things and everything was going normal. What was your personal life like?
Clodah Dunlop 2:51
Life was pretty much perfect at that time. I had been through a divorce. But I met my partner Adrian and we were together for two years before I took my stroke. We had bought a new house together, we had traveled rowing Southern Africa together.
Clodah Dunlop 3:11
And just prior to me taking my stroke, we’d gone to South Africa travel up to Namibia, across to Botswana, Zambia, and then Zimbabwe back down to South Africa and home. And we’re camped all around that, life had felt perfect, and it almost felt life is almost too perfect back in 2015.
Bill 3:36
Yeah, I can relate a little bit to what you’re saying about that. You look back I do at least and everything was kind of going pretty well. Although I was a bit of a winge. I was complaining about certain things, but normal stuff life stuff.
Bill 3:51
And sometimes I look back at those times you think well, what would I give for everything to be the way that it was back in the Yeah, before anything went what I call wrong, but I know what you’re saying. And did you have anything that you thought was something that could lead to you being unwell did you notice anything in your body that was giving you a sign or a warning that you had potentially something life-threatening? about to happen?
Clodah Dunlop 4:25
Absolutely not lives really fit really healthy. So where my Walkman Terms of Care award I’d wondered what had happened and when someone told me I’d had a stroke, I couldn’t understand why I had no one. And as a result of the minor collision, I suffered whiplash and my neck and my stroke came from a weakness in the artery and the left side of my neck. The quote traveled up toward my brain before becoming lodged in the brainstem parts. My brain began today on TV lucky enough to have surgery, and dial the clock removed.
Bill 5:05
Okay, you cut out there a little bit. So just before you cut out, I think you’re about to tell me you’re involved in a collision. Is that what
Clodah Dunlop 5:16
I am I was full and bold in the minor collision at work. As a result of the minor collision, I sustained whiplash on my neck. And for approximately six months, I’d have a small pain in my neck and went to physiotherapy at taking painkillers. But the pain was so minor. It didn’t cause me alarm or distress. I was just constantly aware that it was there. But when I say that it was the entree of my neck wickman what was causing the pain?
Bill 5:51
So the minor pain that you experienced was from the whiplash would you say? Or was it something else that was carrying that you are Now aware of that you weren’t aware of at the time,
Clodah Dunlop 6:02
and the minor pm was from the whiplash, but the whiplash had caused the vertebral artery of my neck to start to weaken. So the pm was actually coming from it, but I had thought it was just my new work life. And so it didn’t cause me the alarm, just minor discomfort.
Bill 6:24
Yeah. So then your clock traveled up into the brainstem and got lodged there, and that’s where the stroke occurred.
Clodah Dunlop 6:32
Yep, four bays for several days prior to taking the Stoke spurge of the cloth release in Mowbray, and that cause me to feel like I was going to collapse. But it wasn’t until the major plot release that I took the massive stroke. And I’d always thought that when the spurge least I had confused that with I was just feeling tired.
Bill 7:03
Yeah, so you just confused this feeling tired. Did you notice any numbness or tingling or any different sensations in your body at all?
Clodah Dunlop 7:12
No, I had when I was first released, I collapsed and bought them then I came around within four or five minutes, which isn’t as normal. So we had I’ve noticed since learned that they were many strokes, but that very often younger people have mini strokes sorry and older people, and the symptoms can disappear. Yeah, that was unfortunate off the top of what happened, so I dismissed it. What was going on in my body is tiredness.
Bill 7:48
Yeah, often the mini-stroke. So the sign that there’s a bigger stroke. Around the corner and symptoms go away and people have never had experiences with stroke. So they just ignore it and don’t really pay attention to it. I ignore the symptoms of what was causing numbness in my left side for seven days. How long? How long did you go before the initial mini-stroke and then the biggest stroke?
Clodah Dunlop 8:18
Well, I had an initial stroke at work on a Thursday night. And I’m because I collapsed at work and they were a little bit alarmed. It was on the night shift. And as soon as the police officer had been put into an ambulance, taking my costs to the hospital with blue lights and sirens, so my uniform, but we all dismissed others just tiredness because it was a night shift. But then, on the Monday, following Thursday, I took a massive stroke. But in between I had only really tired most I had nowhere They’re physical symptoms of stroke.
Bill 9:04
And were you at home or where were you when you experience the large stroke?
Clodah Dunlop 9:10
When well I probably had a mini stroke before I took a larger stroke at home on Easter Monday 2015 my sister visited my house. And as I go up from the back door of the highest ladder and a mini-stroke Comes on me and I collapse in front of her which alarmed her. It was unusual for me to collapse she called an ambulance but by the time man loves arrived, I was completely back to normal.
Clodah Dunlop 9:40
But I went to the and department and as the wizard named me my condition started to deteriorate began when I was offered, medical staff. They thought that it may be fatigue. And just as they were discharging me I took a massive stroke and they didn’t know what it was that was coming. fused with how they take prescription drugs because of my job was I stressed? And so for quite a few hours, I was putting in just a coma. But it wasn’t several hours there that they realized I had taken the loss of brain stem stroke.
Bill 10:18
Yeah, wow that’s quite dramatic. I mean, I imagine that your sister would have some long-lasting trauma because of what she experienced. When you took ill.
Clodah Dunlop’s heart stopped
Clodah Dunlop 10:32
Said it was the worst day of her life. We fail when I was named when I took the final stroke that I died, and that there was a brief few moments and when my heart had stopped, she hit my face and scream my name, and I feel I had the whole white light experience that I was happy and peaceful today but She hit my face scream my name.
Clodah Dunlop 11:03
Doctors work worked on me and they brought me back to what I can only describe as. An absolute nightmare. I never thought that I would say it’s peaceful to die or I was happy to but at that time, at that moment, I was more than happy to die.
Bill 11:20
Yeah, I’ve had a friend of mine who experienced altitude sickness one time when he was overseas, in Annapurna near Katmandu. And he said that as he was going through the lack of oxygen to the body into the brain, and people that he was around, he was happy and telling them look, you know, it’s a good day to die.
Bill 11:42
It’s okay, you know, no problem. I’ll be fine. You guys just Look after yourselves. And it was really traumatizing to the people that were with him. But at the time, he felt really comfortable. And he said he felt just almost euphoric.
Clodah Dunlop 11:58
I always felt there’s a real irony at the moment too because in Northern Ireland, the peace service they are still a terrorist threat. So that every day before I went to work, I would check on my car to check if there wasn’t a bomb. I said it was, you know, I wanted to live, I didn’t want to die. But then I took a stroke and the bomb, ironically was in my own head.
Bill 12:25
Yeah, well, we often also, forget about the impact that our illness has on our loved ones. Of course, at the time, we were really unaware at least I was unaware of exactly how serious my condition was. But I had a feeling that my family was really concerned about the extent of what it was that was happening, especially to my brain. I couldn’t really focus on myself too much because I wasn’t in the space to be able to comprehend almost what had happened but they could really comprehend What the doctors were telling them and walking and we take it for granted that the family goes through a really tough time.
Clodah Dunlop 13:06
I think I will put a locked-in center and it was very different because I couldn’t move a muscle from the top of my fears to the tip of my toes and my feet were all but warm I was able to move my eyes and so I could see a year everything. I’m I can see my parents, my sister, my partner, anxious and distressed at the end of my bed.
Clodah Dunlop 13:16
I could hear medical staff, tell them that I would never be the same person again. It was like I would be vegetative. And I will see them crying. But I couldn’t reassure them I couldn’t speak I could move for days and intensive care. I was able to observe everything that was going on around me, but I couldn’t communicate.
Bill 14:02
Wow so In that time, were you aware least of what had happened to you and how they spoke about what had happened to you in front of your family while you were present?
Clodah Dunlop 14:17
And nurses told me when I woke in the intensive care, I was going to just coma for one day. So on the second day when I woke the nurse and me that I’d had a massive stroke, and that I was in intensive care, and, and it wasn’t diagnosed with locked-in syndrome for a couple of weeks, well, for there were a few more days.
Clodah Dunlop 14:41
And so people were talking around my bed, but there wasn’t much detail about my condition. And I find that made me very anxious because I knew it had a stroke. I couldn’t understand that I was young, fit and healthy. wanted to ask all the questions as to why has this happened. And then I was puzzled and frightened by that.
Clodah Dunlop 15:08
I’d had a stroke, but all I knew of stroke was affected one side and not the other. And here it was I in both sides affected. But I couldn’t move even like, I couldn’t move my tongue and my mouth and I was confused as to what a stroke is. So it was a very terrifying time lying there unable to move and being able to communicate to ask questions about my condition.
Bill 15:39
Yeah. Did you have moments where you were sleeping and moments where you were awake? Or were you just constantly in this sort of awakened state without being able to move? But what was that like? Were you going through a cycle of sleepy and tiredness and awake and alert how was that going?
Clodah Dunlop 16:02
I was largely awake my whole time in intensive care. When I woke, I realized I couldn’t move, I couldn’t communicate. I was more helpless than a newborn baby. In my head. I was still Clodah. Still, the girl was preoccupied with life. Certainly, you worried about my roaming times? Could I get my mind time reduced? But externally, I couldn’t kick out when I was in pain and quiet when I needed help.
Bill 16:35
So you still experienced pain. And you experienced all the challenges that most people will experience after stroke, except you had no ability to communicate that whatsoever.
Clodah Dunlop was being held prisoner by her own body
Clodah Dunlop 16:49
I couldn’t move effectively. I was being held prisoner by my own body.
Bill 16:55
Well, I can’t imagine what that’s like. And I know that a lot of people have experienced some dramatic Symptoms as a result of stroke and I understand about locked-in syndrome. Does it feel like it’s a dream? Or does it feel real? How did it feel for you? Were you in any sort of state of awareness of this is actually you, your body’s actually not moving your conscious or did it feel like a bit of a dream a haze, or a nightmare?
Clodah Dunlop 17:25
And it felt very real, but it was a living nightmare. And for my walk, they were, I always said people effectively, I was a quadriplegic, but I had the same mental like that I had the day before. And, it was terrifying. I could only describe it. I was a bit of an adrenaline junkie.
Clodah Dunlop 17:52
And I loved skydiving and Northern Ireland. I’ve been to many public worker situations. I was got recruited for the public order team and I took petrol bombs and missiles but there is nothing more terrifying than being held a prisoner by my own body unable to communicate.
Bill 18:13
Well, I smile but it’s a nervous smile because I hear you say stuff like I took petrol bombs that’s really foreign to me or anyone who hasn’t taken a petrol bombs and yet locked-in syndrome was worse.
Clodah Dunlop 18:29
Yeah a lot more terrifying just to be able to communicate to indicate to me what around you your simple needs or simple wants or desires and nights I was much too hot, but I couldn’t indicate to me one around me that I was hot I want to define or compress and became alarming to I had male nurses Give me my night, the bed bath and as a female I felt so vulnerable at work, I dealt with victims of sexual assaults.
Clodah Dunlop 19:06
And they’ve been very good. They were aware that there are male nurses bathing my naked body. And I got a notion in my head or I got frightened that if someone touch me or sexually assaulted me, I couldn’t cry out. I couldn’t scream for help. But also I couldn’t tell anybody what had happened. And I became so aware of the highly abominable I was.
Bill 19:33
Yeah, well, just imagining what that would have been like is very difficult for me. I had the pleasure of needing to just convince my nurses to stay out of the toilet when I needed to go to the toilet after surgery. You know and that was really devastating and challenging, and they wanted to show me and bathe me and I just couldn’t move my left side.
Bill 19:58
So I had, I have a had the ability to use my right side was just my left side. And that felt really disconcerting and that felt really uncomfortable. And I’m just in my mind I’m playing over what would have been like to multiply that by two times and being your situation and it’s Yeah, it’s something that we wouldn’t want to wish on anybody really, is it?
Clodah Dunlop 20:23
No, it is terrifying when I became frightened to this very aware of how helpless my body was. I was like a rag doll and the medical staff would have to turn me and became terrified even by those terms. I was frightened that I would fall off the bed to the floor and which is bizarre. I don’t prepare plans and thought hadn’t frightened me but a simple full bed. I realized I could really hurt myself here and it terrified me.
Bill 21:00
I fell out of bed the first day after surgery. So I had a very big scar on my head, you know the stitches and all the stuff that was going on and I couldn’t walk, I couldn’t feel my left side. The nurse tried to help me go to the toilet and she came to my she came to one of my sides and she put her arm around me but she was half my size. She was very short and petite. And she could not hold my weight and I was a dead weight and as soon as I got out of the bed I fell to the ground and that was actually terrifying.
Bill 21:24
I screamed and I just feared my head getting hurt, my brain getting damaged. And it was damaged enough and I didn’t want it to be even more damaged so I can relate to your concern about getting dropped and not being able to support yourself and not having made the decision to jump out of a plane it’s just your on a bed and somebody else drops you, that’s a little bit different.
Clodah Dunlop 21:55
But terrifying.
Bill 21:59
How did you slowly come out of locked-in syndrome and regain your body?
Clodah Dunlop came out of locked-in syndrome
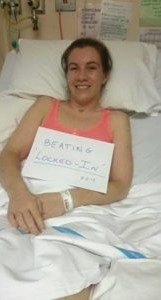
Clodah Dunlop 22:07
And I will say I thought about my life at work, I had 24 hours in the day and when you’re awake and you can’t move, that’s quite a long period of time to full, sort of thought about my life at work and how police officers run to travel model away from it. And work we’d learned by the fight or flight response from fears of the threat to your survival. And I knew that someday I had two choices.
Clodah Dunlop 22:36
And definitely, the flight wasn’t in me so I chose to fight and but it took a lot long time before how do you show people that you’re willing to fight if all you can do is communicate by blinking your eyelids? And so was two and a half weeks into a locked-in syndrome that I was issued by Nelly Tomic, I guess spell board.
Clodah Dunlop 23:00
Every speech and language therapist and I would spell out the article three caution that we issue on the arrest people to the nurses however spell articles I’d have the European and human rights to show that I had the same intellect but they are nice didn’t recognize that you can be as determined as you want you can spell like what you want but physically I need to just show everybody how determined I was.
Clodah Dunlop 23:28
And I really got that opportunity after three weeks for my got neuro physio, I would be willing to my bed to neuro physio Ward will be hoisted from my bed onto a plane and I will be put into a seated position with five physiotherapist support and every bed of my body and putting my head on there we will put me into the stand and hoping that my brain will engage with my body and my muscles.
Clodah Dunlop 24:01
But it was during this time that I could show how determined I was I would stand for fives for I will do the name was that I would stand for 30 seconds my partner would be there he was asked to ask me was okay so when he asked me was I okay I would always blink yes and but they are my body will be consumed by a fee into my will pass so again we will try to stand Nick and he would ask me was I okay and I will blink Yes.
Clodah Dunlop 24:35
And I became known for the patient to be determined to the last two would stand until the feet and this became my daily routine standing by LinkedIn was a machine on till I will pass out or until I nearly or pass out. And then we’re present we dive again and we will begin again the process of Making me stand well it was the own point I could show that I had like this body for I was still the same girl as I was before the stroke and still the same girl wanted together Sam and the mind don’t do a six-minute mine.
Bill 25:19
Yeah. Hey is it frustrating when before you got your board where you could blink words etc? Or some It was blinking words that are pointing to words
Clodah Dunlop 25:32
And electronic I guess spell board. Basically, it was a board with ends inserted coveted in the middle, and around the board were six colored squares. And contained within those squares were colored ladders. And I would look at the ladder that I wanted to blank out our blank give it the latter would pass Be colored blue, and the green square. So far I would look led to the green square servery Library wanted, I had to blink twice, it was like predictive text. And the user on the other side would only see the colored squares that I was looking at, and on their side would hit the color that they saw me looking at or indicate.
Bill 26:26
So it was a combination of two people, yourself and others supporting the rest of the process.
Clodah Dunlop 26:32
Yeah, it was tedious and difficult often for the other person, but as the patient using it, it was also frustrating. And conversations were never fast like this. And I had to spell everything out. And very often, you assume that everyone has good language skills-based services. discovered that many of the nurses couldn’t understand flamboyant language and I learned that communication has to be short and derived flamboyant language doesn’t work.
Bill 27:15
How before you receive that board was it frustrating when they weren’t asking you the right questions for example where they would tell you to blink and do some things but, I don’t know what to ask them?
Using blinks to communicate
Clodah Dunlop 27:27
It was really difficult for the first two and a half weeks more I could do was blink because my partner discovered which is very unusual for locked-in syndrome on the first day that I was there. He asked me Clodah you are still there and I knew I can’t miss this chance.
Clodah Dunlop 27:46
And he said blink once if you’re there. So I close my eyes and counted to three. I can’t (inaudible) my eyelids I need to get this right. And so I blinked my eyes at him. So he established fairly that I could answer yes and no we created a system of blinks, 1 blink for yes 2 for no 3 for I love you, and 4 for you’re a moron.
Bill 28:13
That’s great.
Clodah Dunlop 28:16
It was great he had established that I could communicate and that I was there, but many people didn’t understand that if they asked me open questions, how do you respond with blinks?
Clodah Dunlop 28:30
Do they say what is wrong with you? How do you answer what is wrong, when all you can do is blink yes, no, and tell them you’re a moron, which is quite useful because my own had them when they’d say what is wrong, I would blink them four times.
Bill 28:52
That absolutely loves it. Absolutely love it. I imagined that made it just a little bit easier in your city. situation to be able to tell someone there are more on
Clodah Dunlop 29:03
you know really did and there’s a news me to some of the nurses working on the new task closed questions like are you MP and are you comfortable? I am on when they would enter the ward and see me like four times they understood that I ever said you’re a moron and it and use them to it as allied needs become more human to them. And I think for people to understand the person you are, you have to be able to communicate in some way even if it’s not through a spoken word.
Importance of humor in Clodah Dunlop’s Recovery

Bill 29:42
Yeah, and a sense of humor during such a dramatic time in someone’s life is really important. Don’t matter how bad things a sense of humor is really important.
Clodah Dunlop 29:52
To know I find humor was really important to reassure my family and friends that I was still close. And that I was still there. I remember my best friend came to visit me within three weeks after I had had my national stroke. And she brought her husband and I could see that he was terrified. He was feel nervous.
Clodah Dunlop 30:19
And I knew that he didn’t recognize this quote a lion with the track iOS to me and then n g tube and completely lifeless. And my partner gave him the spell board and told him how to use it. And I could see his terror, so I thought I’m gonna make him realize it was still Clodah. We can still have fun. And I spelled though, to him It is cold, Chris. Hi, Chris. I’ve shipped it myself.
Clodah Dunlop 30:52
You read this spell board then he was like, I think I’ve put this down wrong. And I spelled out Chris, you’re a moron. I have shit myself. And my partner laughed at him. And he was like, Yeah, she had a shit herself.
Clodah Dunlop 31:11
And everybody laughed. And my best friend and she was like, quiz. You’re agreeing to create diarrhea people, but it was admitted the situation calm and relaxed him. We realized she was still in there. She’s still cheeky. She’s still got our humor on it. admit him more comfortably.
Bill 31:35
Yeah. Well, that is amazing. I love it. I love your approach. It’s just really what some situation is because it’s very dramatic, to have a conversation with somebody and to tell them that if defecated in your pants, in any other way, like how do you have that conversation with somebody, but the fact that you’re able to take him off guard and to tell him why he’s a moron at the end. do all the things that you did like makes even that situation which is quite severe and serious.
Bill 32:07
It just makes it better and easier. And I felt that I was also trying to come and allay the concerns of everybody else around me. I was quite calm myself in what I had to overcome like yours very determined, I knew that I was going to get better. I was looking for solutions. I didn’t want to know about the problems. But I had to do a lot of work to keep everyone else around me calm so that when I turned up here, I wasn’t dealing with their stress and anxiety. Is that something that you relate to?
Clodah Dunlop 32:34
Yeah. And it is because I realized very early on that low that in my head, I still felt like I was close. And that I would get better. I could see the anxiousness on the faces of people of my family and friends who visited and so I was in the hospital for seven and a half months. So during that time, I put a very restricted business going on.
Clodah Dunlop 33:03
And it was just my mother, father, my sister, my close friends, and my partner, I realized how distressed people came, became when they visited me and they couldn’t communicate with me and I had to keep a way to protect myself almost because I knew my condition and I almost not accepted it, but I felt like I want to get better. And I but I don’t need to deal with their emotional distress. I have enough to cope with myself to keep myself strong.
Bill 33:40
Yeah, and I love it. It’s a situation where people don’t know how to behave, I think the best thing they can do is do nothing. Just coming off of their love. Give a hug, give a kiss, and get out just so that you know you can Yeah so that you attended and you offered your support and live with that because I used to have I come from a great Family and the great families are very dramatic.
Bill 34:03
So when something goes wrong even in you know, when a child you know, just cut their head open a little bit 25 people have to become aware of it. And you have to, you know, make all this fast and all this scene. So imagine when something is a lot more serious, they all at the same time, when they came, they all turn up in the hospital room.
Clodah Dunlop 34:21
And I prefer when I enter rehabilitation after six weeks, and I really restricted my business and especially with my family, and I felt like rehabilitation was my day job. So definitely after and visitors and that was for my rehabilitation. So I only permitted visitors during the evening period, but again, that was almost as lever me something. It would be my mother’s love of making clothes.
Clodah Dunlop 34:52
My sister, I always got my sister to help with personal care mothers, and as a female when you’ve noticed Your arms, simple things like I’m worried about my boys still do concern us. So my sister comes to pluck my eyebrows and fix my hair and shave my legs and butt and my partner. And we had really become very determined that from very early on that we wouldn’t wait for life to begin.
Clodah Dunlop 35:25
When I recovered. We would live life to the full when I recovered. So it was very strange for doctors and nurses. When I was in rehabilitation. My sister would arrive for the evening and fix my hair and pluck my bros. And my mother would bring me a dress, and the next evening I would get my partner to come on leave a voice in Belfast, to a restaurant or a bar and he would often catch up by food and spoon-feed me and I’m sure people in the restaurant world confused by a girl with her hair and makeup Donna dress and their partner spin feeding her was, I’m sure right. So really for people,
Bill 36:11
They would have thought he was the perfect gentleman.
Clodah Dunlop 36:14
to her. I know that we took a spa break about a year after my illness. And at that point, I could sound myself, but I would have needed a lot of physical support to do it. And my partner Maya did destroy the pole and if he had let go out of the dry diver sank, so he gave me a lot of there was a lot of physical support.
Clodah Dunlop 36:41
And later on that evening, a couple of purchases in the bar in the hotel and they said, we thought you were really being really sickeningly romantic in the pool. And then it wasn’t until you provide that we saw your partner car your opinion into a wheelchair, we felt so terrible. But they were so impressed by how gentle and how caring he was.
Bill 37:08
Yeah, it’s easy for people to judge when they don’t, they don’t understand what other people are doing. And it makes sense. I wasn’t the same, I probably did the same, especially when people would walk slowly in front of me, I became a slow Walker, or walk well now, but in the beginning, I was a slow Walker.
Bill 37:26
And I used to almost push people over to get past them in a queue or, you know, going into a store or something like that. And then I quickly realized, you know, that, okay, there’s probably a lot more going on for people that we are completely unaware of, that makes them walk slowly, and be a burden to somebody like me who was completely physically fit and totally unaware of, you know, physical disability.
Clodah Dunlop 37:55
And I think that one thing I’ve learned from this journey is that I’m a lot more Patient lies person. Um, I realized that everybody’s on a journey in life, everybody is doing the best they can. And everybody has challenges. Everybody’s challenge, I would say, is important. Emma’s big to them as the next person challenge.
Clodah Dunlop 38:20
And I would often say, my mother would worry that she is making up her mind to don’t more Oh my if she cuts her finger, but I say that’s challenging and the moment when my partner, Dr. Soul, the milk and there’s no mo for breakfast, I find that challenging. those challenges are all relative to the moment. Yeah,
Bill 38:44
Yeah, I understand your training as a police officer would have made you resilient in your job, you would have had to have a level of resilience to put up with the things that you put up with on a daily basis. How do you feel that the work that you did and the resilience that you had to have for your work helped you get through your experience with stroke?
Clodah Dunlop 39:09
I think of work we are very big into personal responsibility and being resilient Am I know that I’m personally responsible for myself, there is no one else who can make me better. I need to remain resilient. And I can’t let this get me dying. And so every day I would work with all the different therapists speech and language therapists, physios and occupational therapists, and again, medical staff.
Clodah Dunlop 39:40
And I have to say that some of them I perhaps wouldn’t have chosen to be friends with before the stroke. But I realized that we were all on the same team. We’re all trying to make me better, but I personally needed to want to get better. So I had to work with them. Every Day. Yeah, um, I would say it’s personal responsibility is a huge thing.
Bill 40:09
Yeah, your responsibility.
Clodah Dunlop 40:11
Yeah, there was no one else.
Bill 40:14
Yeah. And I often talk about that. And I tell people as well that we have the ability to respond. And that’s what our responsibility is, our ability to respond. And regardless of how challenged we are by the impact that the particular stroke we’ve experienced, has created or caused. There is, no one wants you to recover more than you hopefully. And if you don’t want it, people are going to go well, I’m just going to help the next person who wants more.
Clodah Dunlop 40:44
Yeah, I know I agree with you. It is you have to want it. And I was told, you’ll never walk. You’ll never talk. But in my head, I had thought if I get something just to move, I will work out it. And psychologists in the hospital thought that I was much too positive as a person. But I had said that and I don’t fear failure. I will work at this and I’m not setting a time limit on success and I will be the best that I can be. But I still feel that I will be the best I can be whatever that is, I do except the parts of my brain are dead. And I will have long-term disabilities. But I still will fight every day to be the best I can be.
Bill 41:38
Yeah. What have you got to say to doctors who say things like you’ll never walk and never talk again? Have you had an opportunity to tell them what you think of their comments?
Clodah Dunlop 41:48
And yes, I have it I would always tell them I don’t get people no hope. You don’t have to get them So you don’t have to say, Yes, she will return just normally we’ll talk a new Rome again, for the thing, don’t eradicate the hope. I had some wonderful physiotherapists who were quite the opposite. They would never tell me you won’t walk and you won’t talk.
Clodah Dunlop 42:16
And I would spell out to them that I will roam again. And they would tell me to focus on each day as a key him and they were like, You’re like a BB? First, you need to learn to set their stand there and take steps. And we’ll see. And I think their approach was very correct. They never took away my hope. But it was set small goals every day. I’m just learning to take things step by step until I achieve your big goal.
Caseworker’s bad bedside manners
Bill 42:51
Your psychologist said that you’re far too positive for somebody in your situation. That psychologist shouldn’t be a psychologist. Surely they should be something else.
Clodah Dunlop 43:02
And it was my first family meeting in rehab. There were real concerns about. And before I had my first meeting and rehabilitation, I was spoken to by my caseworker. And he had said what are your goals for just the first time meeting, and I spelled out to him to walk to the hospital walking and talking, not perfectly but just enough to work on.
Clodah Dunlop 43:33
And he looked at me with real pity, and he said, has no one explained locked-in syndrome to you? And I he, it started to expand my condition. I let him finish because obviously, I couldn’t interrupt them. I couldn’t move or couldn’t talk.
Clodah Dunlop 43:50
But then I spelled it out to him. I will leave here walking and talking not perfectly and again, he looked at me and said, but you have locked-in syndrome and I spelled out to him. And you’re full of bullshit. And you have obviously never had to work really hard at something in your life. And I will show you. And I think yes, I understood my condition.
Clodah Dunlop 44:23
But I always felt that should I never talk that I would always continue the work habits. And I was always big into it. And I’d always felt like I will return to work even if I never move unable to talk again. Because as long as I can communicate and have the same intellect, I can still live a full life.
Clodah Dunlop 44:49
And yes, I would be confined to a wheelchair but just because you’ve done baldies doesn’t mean that you’re going to have a less or less I think there was a perception not because I was going to be paralyzed, that I would have a lesser life. But I would very much disagree with that.
Bill 45:12
Yeah, I had previously before this interview, I’ve interviewed David Rowland. He’s the author of a book called How I rescued my brain. And he is a psychologist by proficient and he experienced a stroke. Yeah. And now the book is written, is being used as a tool to educate other health professionals about how to go about speaking to people and treating people amongst other things that have experienced stroke, especially since they’ve never experienced that and they don’t know what it’s like.
Bill 45:49
So, I said to him, it was great that I met him and that he went through all of the air. I never wished that he would experience a stroke. But as colleges to experience a stroke, he’s got a lot of value to offer to the rest of his peers about how to go about treating human beings that have experienced a stroke. And I love what you did. I love the fact that you had a conversation with your doctors.
Bill 46:18
I didn’t have a conversation with my doctors, but I did sack my doctors. So my doctors, the first batch, I didn’t enjoy the way they were talking about me at the edge of my bed with other people, and they weren’t including me in the conversation. And I just said I’ve had enough with you people. I’m out of here, took my paperwork, and I went to another hospital.
Bill 46:40
And I met with another surgeon and another doctor and I said this is the way that I want you guys to work with me and treat me are you getting any problems with that? And they said no, that’s how we work. No problems with that. And basically, then the conversation was free flowing and like you I needed information.
Bill 46:57
I wanted to know what had happened where it happened. why it happened. How can I? What can I do to make sure that it doesn’t happen again? Even if it’s a physical thing that’s gone wrong? What can I do to try and make the situation better? I don’t want to be told that it’s too dangerous. We can’t operate. We can’t do this. We can’t do that. You’re just taking away all my spirit. So yeah, I love the way that you set the record straight me to doctors
Clodah Dunlop 47:26
I had a therapist pressure me. And I think I was much my physiotherapist the head physiotherapist said that and it’s live the first month for my dander rehabilitation, that everybody was terrified of this patient who couldn’t move a good talk. But yeah, it could spell light and be really bossy. And I would challenge therapists that they were 10 minutes late. And if they wanted to visit the mystery therapy early was valid? Absolutely not. I need I was supposed to get more beats discipline. And they made sure that I got Nora Beach. But I had money. I had three occupational therapists quit on me. Their timekeeping wasn’t very good.
Bill 48:19
Wow, that is amazing. That says a lot about them. As opposed to you, I need to in Episode 10 of the podcast, I interviewed a lady of Scottish heritage, she’s fiery, and she experienced a stroke and the physical therapist that came to her house was talking about her hand that was not working correctly at the time, she was talking about her hand as being the bad hand.
Bill 48:45
And my friend Claire said, hang on a second. That’s not how you talk about my hand. It’s not the bad hand. It’s just a hand that needs therapy that needs to get better. Yeah, please don’t talk about my hand in that way. And that therapist never came back
Clodah Dunlop 49:03
I think a loss I guess I often say it’s like the police service I think the more life experience you have the better your job and again and I find the older therapists had much more patient experience and so we’re a lot more understanding and against just very experienced just a little better at their job, bro.
Bill 49:35
Yeah. So you got out of the hospital around seven months after the stroke after you were locked in. Yeah, how soon before you got out of the hospital Were you able to speak how soon after being locked-in digital speech came you back?
Clodah Dunlop 49:54
And so it was very like the process of my speech just returned, I had dysphasia and dysarthria. So all my muscles and my throat had stopped working all the muscles in my cheeks and lips tongue and all completely stopped working.
Clodah Dunlop 50:15
So Edwards has been a very it was very lengthy people says to strengthen my swallow, and I would spend hours drinking fruit smoothies and my partner would spend hours and putting a motel I spin into my mind covered Metallica strike, get my tongue to respond. And I spend hours and hours strengthening my muscles.
Clodah Dunlop 50:46
So when I returned home, my speech was very average. And I knew what I wanted to say I didn’t have this Vizier But I couldn’t. The mic was perhaps too weak to form the levers. And my direction was bad. I couldn’t do some signings. But I can do to work a lot. Even my colleagues now three years later, wouldn’t notice that since I’ve returned to work, my speech has improved. It’s not completely back to normal. But it does still continue to improve three years later.
Bill 51:32
Yeah, I watched one of the interviews that was on Facebook. And you have improved a lot since then. And I think that interview was a couple of years ago on one of the chat shows, so yeah, constantly improving and that’s one thing that people need to know is that recovery happens slowly and it’s important to get some video footage of yourself if you can so that you can look back in six months or in 12 months and compare yourself to feel good about the progress that you’ve made? Because often we don’t notice how we’re progressing, but other people do. Notice how we’re progressing.
Clodah Dunlop 52:08
Yeah. And I find it interesting. I have a window cleaner. And he comes every six weeks. And every six weeks, Swami comes. Even three years later, he still notices physical improvements. And I enjoy it. He’s like a measure. And if he doesn’t comment on seeing an improvement, my mom was disappointed.
Bill 52:35
Well, make sure that you tell him to tell you about the Yeah. How young you’ve gone back to work now. Yeah, back with the police force.
Clodah Dunlop 52:47
Yeah, I’m back in the police service of Northern Ireland. And I am no longer in the public order team in the riot squad. And with my decibel days that job bulls just not suitable Leia’s walking need isn’t appropriate and the frontline policing I ever AM. Back in February this year I saw the Nashville police investigator exam, which is to be a detective. So I pass that exam and I’m now doing a detective role and really enjoyed the best to get frauds. Burghley is involved in more serious offenses such as murder and attempted murder. And it’s challenging but very rewarding.
Bill 53:40
Yeah, congratulations well done. I imagine that that’s also helping your mind and your body to recover and you’re finding your limits. And you’re also starting to get beyond your limits as far as what you’re able to achieve on a daily basis and do on a daily basis.
Clodah Dunlop 53:59
Absolutely. When I returned to work 18 months after I had my stroke, I had wanted to return to full-time Mars but Occupational Health and Welfare at work had told me that I had to have a fee returned, starving with three hours a day, for three days a week and I was very opposed to that.
Clodah Dunlop 54:19
And it was explained to me that everybody who had maleness and was returning to work with BP had his bike because the police service of North Island wanted along with the person for the return to be successful. I find that I was able to increase my hours on my days, but it was challenging and I did suffer from fatigue. But now I am back full time and I find that I can manage my tiredness so they do have my finger the fee is returned and has definitely helped a very successful return my fatigue levels are more Much much slower nine.
Bill 55:02
Yeah, that’s amazing.
Clodah Dunlop 55:03
I personally have gotten stronger.
Bill 55:06
Yeah, that’s amazing. I really, I love your spirit. I love your fight. If you were if I was in Northern Ireland and something bad happened to me I would love for you to be on my team trying to find the person and bring them to justice. You know to support me. I just love the way you go about your work and the way you’ve gone about your recovery. How long? How long has it been? You are back to driving.
Clodah Dunlop 55:35
I returned to driving 18 months after taking my stroke. I’m very proud of the fact that I returned to work, walking, talking, and driving. I was not perfect and but I was able to do all I have adopted many comforts around. It has I can only drive with one hand my Right say this so affected and I have a hunger drill for my left hand I drive an automatic they accelerate is my on my left-hand side and so it has taken a bit of retraining my brain will do that but I very much enjoy driving my vehicle adult surprised people will make it in and realize that it is acted. It was mentally challenging, but I enjoy it.
Bill 56:32
Yeah. Well, that’s brilliant. I just I’m so pleased that I got to find your post somewhere on Facebook and to reach out to you I think it was Instagram actually. And to reach out to you and get a response always makes me smile. I love it when people respond and interviewing people like you is just just makes my recovery a lot easier and a lot better. So you’re doing a massive thing. Thank you so much for reaching out On the
Clodah Dunlop 57:00
Well, I mean, likewise, people, people would say to me, you’re very inspiring. And I will say, I am so inspired by the author’s stroke survivors that I meet them when I hear their stories. And so, I think, for me and my recovery, I particularly enjoy him from all the survivors. When I was in rehabilitation, an elderly woman came to see me, and she said to me, she was 80 years of age.
Clodah Dunlop 57:29
I left the world and thought, Why is she visiting me, she sought me my story in big media, the press, and she told me Pluto, my name’s he is all when I was, I think, 32 and a young mother. I have a brain stem stroke. And for almost three years, I couldn’t talk I couldn’t walk. And I looked at this glamorous elderly woman who walked into my ward both welcome and welcome.
Clodah Dunlop 58:00
She told me you will get there. Don’t change too much about your home. Because if you change things by the whole meal maker self more disabled, and vs all your challenges, and if you do that you will overcome them. And she’s always story a bite. She was in a wheelchair, and her two-year-old daughter had slipped in a paddling pool and started crying she was in a wheelchair only able to move on able to talk, so she couldn’t run to help her daughter and she couldn’t call for help.
Clodah Dunlop 58:39
She just sat there watching as a toddler, frightened. But thankfully her partner cave or husband came along and sold the child and rescued the child. And for me, it was it’s a mono-marginal story. First of all, the actual story of yourself having to watch 10 Drawing, but this one was standing by my bedside at 80 years of age, glamorous and talking sore technically and I was at, it gives me massive hope that yes, I will get there.
Clodah Dunlop 59:16
And she also told me that when her daughter was 4 that she and her daughter attended speech and language therapy together. Because childhood never learned to talk. And he iZl and her husband when they were at home, his little one couldn’t talk. So her husband and heard never calm, had never had a conversation. So their daughter hadn’t learned at all. So she and her daughter learn to talk together.
Bill 59:45
Wow. This is a thing you know, this isn’t a person who doctors could learn so much from you know, if they follow the the story of somebody who was at who had a stroke. Probably 30 3050 years ago, it was much harder to recover from.
Clodah Dunlop 1:00:07
And she told me she was discharged from hospital after five weeks. And at that time, she couldn’t move a single muscle like me from the top of her face to the toes and her feet, and couldn’t talk. And she was left in the care of her husband. And he also had a two-year-old and a four-year-old son. So, and nine North and Ireland, we would have care packages.
Clodah Dunlop 1:00:35
If someone was to be sent home from the hospital my condition and I would have someone come in and assess the family four times a day. But 515 years ago, there was no such thing. So our husband relied on her family, his family, and himself to deal with the personal care and to help her recover.
Bill 1:00:57
Yeah, well, so we have a completely different situation these days, no doubt that syndrome stroke, any serious illness is difficult for people to deal with. But we’re dealing with it in the email time and the resources are more plentiful. Even though there’s never enough, we still have more resources. Yeah. And this lady is the perfect example of, you know, how you can, with enough time, and enough effort and enough focus and attention to your well-being and your own responsibility to recover.
Bill 1:01:34
You can really make a massive impact on life and live a full life and get to it and beyond. And that’s what we want to do want to offer hope to people who are listening and who might be going through something just as serious now. So, again, thank you for your time. I really appreciate it.
Clodah Dunlop 1:01:52
No, thank you, Bill. I feel like I need to interview you and I’m here you’re in your story. By all means interested
Bill 1:01:59
Anytime. I’m available, make yourself whenever you’ve got time, you know, just reach out. I’ll be happy to help you. I want to keep in contact, and I want to keep following inspirational people and you’re one of those people. So anytime.
Clodah Dunlop 1:02:12
Just quickly, what age did you have your stroke and what happened?
Bill 1:02:16
Yeah, so I was 37. And what had happened was I noticed some numbness in my left toe in my big toe on my left foot. Yeah, and that was it. And I noticed that on a Friday, I have a property maintenance business that I that I’ve been running and that means that the next two days I had work to do Friday and Saturday.
Bill 1:02:39
We needed to you know, fix ceilings and paint walls and all that type of stuff. And we had deadlines, so there was no way that I was going to attend to, a numb sensation. big toe, you meant nothing. But then the numbness spread from the toe to the entire left side of the body over the next seven days. Yeah, I know I ignored the symptoms for pretty much seven days.
Bill 1:03:04
My wife noticed me walking funny after the third day or fourth day, she said to me, you’re walking funny. And I said, Oh, you’re crazy. Leave me alone and go to work to do. I’m busy. Yeah, I went to the chiropractor because I thought I’d done something to my back. And my chiropractor said Whatever has happened to your body is not happening in your back. It’s happening elsewhere, you need to go to the hospital immediately.
Bill 1:03:28
And when I got to the hospital seven days after the first symptom, they noticed that there was a bleed on the brain on the right-hand side. And it was caused by a defective blood vessel that I had been born with, and just took 37 years to blade to Lake it was a very small lake, and it bled slowly. But as the amount of blood started to increase in the brain, it started to impact more and more of my left side.
Bill 1:03:57
And then, six weeks later, I had another massive bleed. And at that point in time, I didn’t recognize my wife, I didn’t know my name. I didn’t know what was going on. And that took me around about. It took me around about six months to start to recover and get my memory back and speak properly, get back to work, and do all those types of things.
Bill 1:04:21
And then almost three years after the first incident, so in February 2012, was the first incident the third incident was in November 2014. It happened again, and then I had surgery in November 2014. To remove the faulty blood vessel and when I woke up from surgery, I couldn’t feel my left side and I had to learn how to walk again and use my arm again.
Bill 1:04:49
And I got back to sort of being at home just before Christmas of 2014 and then It’s been an ongoing, continual gradual like you recovery to some kind of normal work life, some kind of normal timeline, dealing with fatigue, and also a whole bunch of other issues. And something that really impacted my health and recently in the last two years was I had thyroid surgery.
Bill 1:05:21
And the general anesthetic that I took, actually really affected the damage that I received on the brain from the surgery and it made it worse. And I noticed that when I woke up numbness on the left side of my right side was more emphasized, and I couldn’t feel as much as I could previously. And now I was dealing with, you know, similar but worse sensations on my left and on my left side. So that’s my story short, briefly.
Clodah Dunlop 1:05:58
Wow, you’ve been through the wars. Though
Bill 1:06:00
Yeah, we have we all have, you know, stroke patients. And I get comfort in knowing that other people are doing well in their recovery, and they’re having ups and downs, but it just sounds like now a lot of the ups and downs of becoming part of average, basic life, you know, it’s our it’s just another up and down. Yeah, but we just notice it a little bit more.
Bill 1:06:26
And we have to take care of our response after that because when I have a down, you know, could last two days and I’m not very nice to be around. I’m not useful. I’m not productive, and that frustrates me. So if I take care of myself during those downtimes, I decrease the downtime and increase the uptime. So I’m learning about how to help myself as much as everyone else has to learn about you know, how to get through their own struck.
Clodah Dunlop 1:06:56
And I find that diet really affects Me and my fatigue and mood I am my partner he has children from his previous marriage and if they come down and we order Domino’s Pizza pego pizza monster carbs I fatigue really affects me but if I eat a very clean diet eat lots of vegetables and protein but largely I’m perfectly okay.
Bill 1:07:29
Yeah, I was the same. I dial down my diet and the fibroid surgery made my metabolism slow a little bit and made me hypothyroid. Which means that carbs affect me even worse now. Yeah, so absolutely notice that stopping the carbs really brought my brain back to life and clean, healthy veggies and protein and you know nice oils clean healthy oil.
Bill 1:07:56
Brought me back to life and and now the fight droid surgery just made any kind of car very difficult for my body to process and immediately my brain starts to go to sort of slow down and shut down. And it starts to process things a lot slower. And I start to respond differently.
Bill 1:08:16
So part of the work that I’m doing is I wanted to bring these types of stories to people, but at the same time or through the recovery after stroke com website creates a community where we can bring people together, and I could train them and they can come in in a community and talk about what’s working for them and what’s not working.
Bill 1:08:36
And we can all support each other in a recovery that seems to be going to going to be long, you know, for the rest of our lives, long-term recovery and care of our bodies and care of ourselves so that we can have a very productive life despite what it is that we experienced. So that’s what I’m motivated to do now. And I figured if I’m teaching other people How to take care of the brain and recover after a stroke. Then I have to walk the walk and talk talk.
Clodah Dunlop 1:09:07
Otherwise, I can’t do it.
Bill 1:09:09
It keeps me honest.
Clodah Dunlop 1:09:14
It’s been so nice to talk to you
Bill 1:09:16
And to you. I hope to talk to you again, I will follow you and I’ll keep in touch with your social media.
Bill 1:09:27
I just really appreciate your time. Thank you so so much
Clodah Dunlop 1:09:30
No, thank you. It’s been really nice talking to you.
Intro 1:09:36
Discover how to support your recovery after stroke. Go to recoveryafterstroke.com






