Neale Mahon experienced an ischemic stroke nearly 30 years after radiation treatment to deal with a brain stem tumor.
Socials:
https://facebook.com/neale.mahon
Strokefitinc.com
Highlights:
00:45 Introduction
02:15 What happened to Neale Mahon
11:27 They can make mistakes too
13:43 Brain Stem Tumor & Stroke Recovery
24:13 Mortality
31:36 Covid vaccine having a risk of blood clots
40:46 Stroke recovery timeline
52:03 Being afraid is something to be afraid of
57:20 The biggest disconnect
1:03:56 Future plans for Neale Mahon
Transcription:
Neale 0:01
Yeah, you know, I think fear can be a very powerful thing. You know, being afraid is something to be afraid of.
Bill 0:18
Oh, man, hang on a sec say that again.
Neale 0:23
Being afraid is something to be afraid of.
Bill 0:27
That’s deep man that is real deep.
Intro 0:33
This is the recovery after stroke podcast, with Bill Gasiamis, helping you navigate recovery after stroke.
Introduction

Bill 0:45
Bill from recoveryafterstroke.com This is Episode 140. And my guest today is Neale Mahon. Neale is no stranger to health challenges born with a cleft lip and palate, dealing with a brainstem tumor as a young child, and an ischemic stroke in his 30s has given this middle child some lessons in resilience.
Bill 1:07
Now, just before we get started, if you enjoy the recovery after stroke podcast, and you think that others should hear the amazing stories of these excellent stroke survivors, please tell others about the podcast and share it on your favorite social media app.
Bill 1:23
Also, leave the recovery after stroke podcast, a five star review on iTunes, or your favorite podcast app. And if you’re watching on YouTube, click the thumbs up button and subscribe to get notified of new episodes. Thanks so much for listening. And now it’s on with the show. Neale Mahon Welcome to the podcast.
Neale 1:45
Thank you Bill it’s an honor to be here with you today. And an honor to have people listening to what I have to say.
Bill 1:54
Yeah, it’s great to have you here. Thanks for reaching out, I really appreciate it when somebody reaches out and asks to be on the podcast. That’s exactly what it’s about. That’s exactly what it’s for. It’s about stroke survivors sharing their stories. So tell me a little bit about what happened to you.
What happened to Neale Mahon

Neale 2:15
Well, I’ve got an interesting medical history, to say the least. But specifically for my stroke happened back in May 21. of 2018. Actually, three days before my 31st birthday, and so now I’m 34.
Neale 2:40
So I was on my way driving to a just a normal kind of doctor checkup. And while I was driving, I put my arm out the window, really nice day in May. And my arm went numb. But I figured you know, it’s done that before because I usually pinch a nerve when it’s at a weird angle.
Neale 3:08
So I just figured I pinched a nerve. Well, it didn’t go back to normal. Until like a half hour later, an hour later. I noticed it was still numb and I had just gotten into my doctor’s appointment.
Neale 3:26
And I got up on the exam table. And my left leg went numb, literally that second. And I was like, you know, that’s really weird. And I told the, whoever the doctor was checking me out. I was like, Hey, you know, weird in my arm and leg feel numb. You know, what could be going on there.
Neale 3:50
And to me, I was like, Oh, it’s just really weird. It’s probably I pinched nerve again. You know, they did all the checkups on me blood pressure was great heart rate was great. I knew I didn’t have high cholesterol or anything like that. So there’s really no marker to give anybody an idea what was going on.
Neale 4:15
But I noticed after I got off, the table and started to walk out. I was kind of disoriented, and I have been to this doctor, this is my family doctor. So like I know my way around the building. And I was disoriented in the lobby. And I was like, well, that’s weird I started to walk outside.
Neale 4:39
And then I realized I was veering towards the left. So as I was walking, I was walking straight in my head, but I was actually walking to the left. And then I ended up kind of walking off the sidewalk. I didn’t hurt myself or anything. I just walked into the grass.
Neale 4:57
And then I said you know that’s really weird. That should’ve sent me off right away, first of all, but it didn’t. I said, well what the, you know, if I can jog to my car well then I guess I can drive home. If I can jog to my car, I guess we can drive home.
Neale 5:19
So I jogged to my car and I make it. I don’t know how pretty it was or not pretty, but I felt like I was okay. So I said, I’m gonna get in my car, go home. And I figured I was just really dehydrated, you probably heard that a ton of times.
Neale 5:38
I went home, I chugged a big 32 ounce glass of water. And I was just still tired. So I was like, I’m gonna lay down for a nap. Right before I layed down for my nap, I texted my wife who was at work, I said, Hey, you know, say a prayer for me. I’m not feeling too hot, or you know, not feeling very well.
Neale 6:03
You know, I layed down for my nap. And about 45 minutes later, I woke up from that nap. And I felt world’s worse. I was dizzy, I was really disoriented. But in my own home. That didn’t make sense. And so I called my wife I said, I don’t know what’s going on.
Neale 6:28
And, she works at the hospital. So everybody was like, Oh, my God, he’s having a stroke or something heart attack, or, you know, we didn’t really know what was going on at that moment.
Neale 6:40
But she knew that I needed to be, you know, at an emergency room. And luckily, my niece, who I credit was saving my life was living with me she was living in our house at the time. And so I called her and they’re like, Hey, can you drive me to the hospital? I don’t know what’s going on.
Neale 7:00
And she drove me to the hospital. The crazy thing is I went back I had her drive me back to the not the ER, but had her drive back to the family doctor. The wrong place, the place I didn’t need to go. Like they couldn’t do anything for me.
Neale 7:25
So on the way there. I just, you know, I realized that I really go downhill kind of quickly. And I called an ambulance and had the ambulance meet us at the family doctor to rush me to the ER, which is right down the street from my house.
Bill 7:47
I’m listening to you. And it reminds me of me. I just met you but I’m gonna be completely totally blunt. I did the same stupid things that you did. Thinking that I was doing the right thing. But that’s what stroke does. Like it messes with you in so many ways, and it makes you make decisions that you would not normally make.
Bill 8:17
At this time. When you’re feeling these strange symptoms. Your head is going no no it’s okay. It’s not that it’s nothing serious. It’s probably something else. I’ll tell you what I did, just so you know that I’m not lying.
Bill 8:32
For a week. I ignore the numbness in my left side for a week. I had numbness in my foot, it spread to the entire left side of my body. I was arguing with my wife with my doctor with my chiropractor about why I shouldn’t go to the hospital.
Bill 8:54
One other time because I had three blades one other time. The numbness came back as sunburn on my left side, and my way of fixing it was to get out of my car and walk around the car and if I walked around the car and it went away, then I was good. So I got back in the car and then it happened again.
Bill 9:20
I drove myself to the hospital. I mean, everything you say are the same crazy things that I did and tried to convince myself that something else was happening and it wasn’t serious. And it wasn’t life-threatening. And one other time. I was being driven home feeling sick being driven home.
Bill 9:43
We stopped outside of the hospital where I threw up and we got back in the car so I can drive to the hospital near my house. I didn’t drive somebody was driving me but he was an hour away from the house. hospital I was outside of when I was throwing up.
Neale 10:05
That’s crazy.
Bill 10:06
That’s crazy. That’s the same stuff that you did. And then you go to the hospital and then what happened then? like you’re at the hospital and then what?
Neale 10:17
So, you know, in the ambulance on the way the hospital, they were like, you know, asking me all these questions, and I felt cool. And awesome because I could answer them. I was like, ooh, a challenge. Yay. I like challenges.
Neale 10:31
Like, what’s your date of birth? I’m like, ring ring, you know, I said everything real quick. And they’re like, well, we think you’re having a stroke. But we don’t know, if you’re having the stroke, we can’t really tell what’s going on. because number one, that when I had my stroke, I was 31 years old.
Neale 10:51
So they don’t see a lot of 31-year-old stroke survivors or stroke patients in general. But, but so they take you to the nearest emergency room, which is actually a stroke-certified hospital.
Neale 11:08
And then they continue to do the stroke protocol here in the US, on me, you know, the MRI, CAT scan, blah, blah, blah. And they come back and they go, we’re pretty confident you’re not having a stroke.
They can make mistakes too
Neale 11:27
In that, you know, I’ll never ever ever forget that. Yeah, I sat in that hospital for eight hours in the ER with nothing, no. intervention, no, nothing. For eight hours until I got sent to the Cleveland Clinic. And in that eight hours, I went from having strength in my arm and my leg, slowly going away.
Neale 11:58
I could feel it, like slowly getting harder to open and close my hand. My strength was leaving me. And I was like, Oh, here we go. You know, I still didn’t know what was going on. You know, we all have so much faith in doctors and medicine and hospitals that we forget that they’re also you know, they’re human, they can make mistakes, too.
Neale 12:26
So I got to transport to the Cleveland Clinic. Thank God that, you know, I arrived there probably at midnight that night, or at one in the morning. And within five minutes, they told me to stick my tongue out. They said, stick it straight out and they went all the way to the affected side. And they’re like, you’re having a stroke.
Neale 12:49
And then, by that time, I was way over the timeframe for any type of unconventional you know, TPA, or anything like that.
Bill 13:03
Too long, too long and past.
Neale 13:06
And I mean, thank God I was breathing, actually.
Bill 13:10
So, you know, now you’ve been diagnosed, you’re in the hospital, they know you’re having a stroke. Did your condition deteriorate? What happened then?
Neale 13:21
I mean, it got to a by the time I got to the Cleveland Clinic, I couldn’t move anything on my left side, not my toes. My fingers couldn’t move a thing. Probably couldn’t move, I think for about three or four days.
Bill 13:35
And your stroke was an ischemic stroke caused by a blood clot. Do they know what caused the blood clot?
Brain Stem Tumor & Stroke Recovery
Neale 13:43
Yeah, so I was born with a brain tumor, called the Ganglioglioma, which is a brainstem tumor, and back in early 90s, I went through about three years of chemo and radiation. And it turns out that they believe that the radiation that I did back in the day caused by blood vessels in the back of my neck to atherosclerosis. And, that’s what caused the stroke.
Bill 14:12
Was it a dissection or was a part of the blood vessel actually, what caused the clot? Did a piece of your blood vessel come off?
Neale 14:23
No, I don’t think anything came off.
Bill 14:29
It sounds like it might be a dissection. It sounds like something has changed in the inside of the blood vessel. Which makes the blood flow slightly differently, and as a result, just creates a little blood clot just because of the pressure that’s there, and might throw it off somewhere.
Neale 14:49
That makes sense.
Bill 14:51
Wow man so you’re not new to all of this kind of stuff. So this brain tumor. Do you recall what kind of challenges you were facing back then as a child?
Neale 15:05
Nothing really. So I’m lucky in that aspect. I guess when they found it. I was kind of dragging my left leg, I believe it was my brain tumor I guess is slightly left sided or I’m not 100% sure. But basically I, you know, for 30 something years, I had a completely normal life.
Neale 15:35
I didn’t really have anything because we found it early enough and they shrunk the tumor. They couldn’t go in because it’s in my brainstem, they couldn’t go in and get it out. They can only shrink it with chemo radiation.
Bill 15:48
Was your wife there when you found out that you had a stroke? Or were you alone?
Neale 15:53
My wife was there. She met me at the first hospital. So and then, you know, my mom met me there. And you know, my family met me at the other hospital.
Bill 16:05
How did they take it? I know it’s an obvious question right?
Neale 16:15
Like absolute angels and professionals. I mean, you know, my mom, my family has been, you know, I’m the middle child, I have all the so called problems.
Bill 16:30
Of a middle child.
Neale 16:32
Yeah, I got screwed with all the problems.
Bill 16:39
I’m sorry to hear that, man.
Neale 16:41
No, that’s all right. That’s right. They’re all good. Not really, but uh, you know, and I was also you can’t really tell in this picture but I was also born with a cleft lip palate. And so, you know, I’ve gone through what, like, 25 surgeries throughout my entire life to correct that. And, and the tumor, and now I had a stroke. It’s like, jeez anything else to throw at me?
Bill 17:09
Enough already enough?
Neale 17:10
Yeah. But they were amazing, you know, I really couldn’t have done, I wouldn’t be where I am without my family, for sure.
Bill 17:20
You know, your history of medical situations, conditions, whatever you want to call them, does that help you when somebody says to you, you’ve also had a stroke, Neale, like, does it help you with your mindset? Or does it help you with how you’re going to move forward and overcome things?
Bill 17:39
What goes through your mind when now you’ve had a stroke? Like, I know, what goes through your mind is well, I know, part of it might be I don’t want to be in the situation or stroke’s no good, or what I have to do to recover? But is this some of your history that helps you now?
Neale 17:58
Are you speaking of like the mental aspect of that?
Bill 18:03
Yeah, your approach to life and your approach to overcoming? Like, how do you move forward?
Neale 18:11
I mean, I completely understand that because now I’ve had a stroke, you know, strokes, not only affect you physically affect your emotions, and very much.
Intro 18:22
If you’ve had a stroke, and you’re in recovery, you’ll know what a scary and confusing time it can be, you’re likely to have a lot of questions going through your mind. Like, how long will it take to recover? Will I actually recover? What things should I avoid? In case I make matters worse, doctors will explain things.
Intro 18:41
But obviously, you’ve never had a stroke before, you probably don’t know what questions to ask. If this is you, you may be missing out on doing things that could help speed up your recovery. If you’re finding yourself in that situation. Stop worrying, and head to recoveryafterstroke.com where you can download a guide that will help you.
Intro 19:02
It’s called the seven questions to ask your doctor about your stroke. These seven questions are the ones Bill wished he’d asked when he was recovering from a stroke, they’ll not only help you better understand your condition, they’ll help you take a more active role in your recovery. head to the website now, recoveryafterstroke.com and download the guide. It’s free.
Neale 19:25
Something I’ve had to deal with now but I haven’t really ever had to deal with it. I’m kind of a full throttle guy, you know, the gas pedal is either down or it’s you know, the brake time.
Neale 19:39
So I always have approached life as like, you know, tomorrow’s tomorrow, just try to be a good person and then if you think you’re being a good person, try to be a better person. And, try to bless those around you with what you can. But you got to bless yourself too. So you got to take care of your own person too.
Bill 20:09
When you’re having a terrible day, how do you be nice to other people? But how? You know, how is it possible to focus on others when you’re having a really bad day? Or is that the time to go? Hang on a sec.
Neale 20:22
I always I understand, what you’re saying I always feel like, you know, it could be worse. You know, I got enough, checkboxes, they have a lot more problems.
Bill 20:35
How long did it take you to get back on your feet, your stroke affected your entire left side. So what happened after your hospitalization and your clot was sorted?
Neale 20:47
So I was in acute therapy for eight weeks at the hospital, so I didn’t leave the hospital for two months, or two and a half months, or whatever it actually was. Thank God for the Cleveland Clinic and their therapists over there, because they’re number two in the planet for a good reason.
Neale 21:09
Because they’re really good at what they do. And I still go to therapy once a month over at the clinic. And I have my own home program that I work on all the time. So if not every day, every other day.
Bill 21:28
Yeah. And how long has it been since the stroke?
Neale 21:32
And it’ll be three years. On the 21st. of May.
Bill 21:40
Sounds like your your approach, has been kind of created from that early days, probably the brain tumor in that you had a brain tumor, you probably did, you might accurate when I say you thought every day after the brain tumor was sorted, that is a blessing and therefore, just keep moving forward, just keep going, just get stuff done, just achieve what you want to achieve live a happy life, just be nice to people.
Bill 22:12
Is it fair to say that that approach was the one that you use previously, and now it’s worked for you then and it’s going to continue to support your recovery moving forward?
Neale 22:25
I would agree with that. You know, I definitely would agree with that. I think, I don’t know, if you’ve seen my website or anything, you know, one thing I have on there is my, my be 100 you know, 100%, mental 100% physical, and 100% diet and nutrition, after you have a stroke, all of those things are affected.
Neale 22:51
You know, your diet, your, your mental state, your physical state. And so I choose every day to be 100% and all those you know, if I’m going to do it, I’m going to do it 100% not 70% 30% 20% and sure I’m not perfect. Nobody is, you know, I’m not the best at diet. I wish I was better. But, you know, everything comes with practice.
Bill 23:26
Yeah. And you strive I believe in striving for the 100%. And if you get 75% that’s better than 60% yeah?
Neale 23:37
You know, talking to Kent. Kent, who was one of the people on your podcast, I was talking to him yesterday, I said the only thing I can guarantee anyone is if you don’t do anything, you have a chance of zero recovery. It’s not just gonna come back if you sit on the couch and don’t do nothing.
Bill 23:57
Yeah, Kent Bragg Episode 138. And yeah, he’s a pretty cool dude.
Neale 24:09
Yeah he’s from Ohio too, so he lives like an hour and a half away from me, apparently.
Mortality for Neale Mahon

Bill 24:13
Ah, wow. Okay, that’s great. Isn’t it amazing? A guy from the other side of the planet in Australia, Connected to a dude from my Ohio, man. That’s awesome. So your wife. How has she dealt with all of this? How have you noticed her going through this process with you? Has it been difficult for her? Have you guys discussed serious issues like mortality and all that kind of stuff? Because they’re the kind of conversations I had, you know.
Neale 24:49
Yeah, it’s really funny that you say that because three weeks before I had my stroke, we started our will. And guess what we finished it in the hospital. After my stroke, when I can barely move my left side, I called up the attorney I said, Hey, I’m in the hospital, can you come meet me and he could. I was just like, Man it was bad you know, that’s what it’s for.
Bill 25:22
You guys are hardcore. Doing that in hospital that is hardcore, let me tell you. I completed it about I reckon maybe two years later, or a year later, something like that. But I did definitely complete it very rapidly. I was 37 years old at the time. So I did complete it rapidly as well and made sure that it was done, because I felt relief when I did it. Did you feel some kind of relief?
Neale 25:53
Yeah, I felt like, you know, okay, you know, I don’t have to. It felt like, I don’t have this mental power on like, what if, what if, what if, what if, I kind of have answer for that. You know, now my mental power is how can I best rehab? You know, and then how can I work and make money and you know, I don’t want to be less of a husband to my wife.
Neale 26:21
You know, and I’m sure anyone who has a stroke that has a spouse really feels that way, you know. And there’s also things that I just can’t help her with, you know, that are so mundane. And what just trigger all my neuropathy and just, I just can’t do it, because I’m a grouch. When that happens.
Bill 26:44
What are some of those things because I relate to that I relate to being a grouch when I can’t do things, and what are some of the things that trigger you.
Neale 26:54
One of the things that triggered the pain are like holding, so like, fine movements, too much of that will cause me to not sleep at all that next day or, I’ll get like two hours of sleep, and be a terrible human being the next day. But that’s really the big one. And carrying anything that weighs more than a couple pounds.
Neale 27:23
You know, I really, we were lucky to have Greyhound dogs full grown greyhounds, so I was really worried after I had my stroke, that we’d have to get rid of them because they like to lean on you. And they’re tall. So they kind of hit you right above the knee sometimes, you know, and I’m like, Well, I just need to be like flipped right above the knee when I came home, like fall over.
Neale 27:53
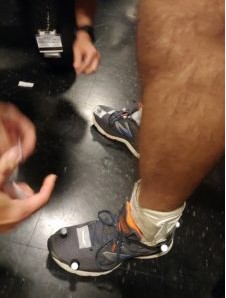
So but I’m able to really do a lot. And there’s been some breakthroughs in medical technology that I’ve really, really been a fan of, like the XTERN AFO, which is a new like exoskeleton AFO that goes on the outside of the shoe. And it’s really allowed me to just step everything up. You know, I’ve only had it for a week and I tell you it saved my life.
Bill 28:24
Yeah, maybe when we’re done, maybe you can send me the link. And I’ll include that link to that product in the show notes. So if anyone who’s listening is curious about this particular AFO where they might be able to find a little bit more information about it.
Neale 28:41
Actually, yeah, I have a bunch of that. I don’t know if you’ve ever met Martin Jackson. He apparently is a Australian, like a championship shot putter in Australia.
Bill 29:03
Well, here we go. Now the person from Ohio is gonna tell an Australian about another Australian. That’s classic.
Neale 29:11
Well, I just wanted to prepare that for you know, information on how to get the brace in Australia.
Bill 29:19
So tell me about Marty, is Marty a Paralympic athlete?
Neale 29:24
You’re probably reading it. Yeah.
Bill 29:26
Yeah. Okay. So he’s a world champion. shot putter and he uses an AFO, and there’s an image here of him with his AFO winding up, ready to launch a shot.
Neale 29:47
Yeah it’s pretty cool. And that’s the exact one that I have. Okay. It goes on the outside of the shoe. So all you need is your shoe size.
Bill 29:57
That’s brilliant good to know, I wonder if it’s widely known. Do you think it’s widely known that this new version of AFO is available?
Neale 30:06
No not really no sadly, no, it should be and I’m working on that.
Bill 30:13
Was it expensive to get?
Neale 30:16
It was 950 bucks I think. So a little bit of money but not like buying a car.
Bill 30:27
So you know about Marty? What happened to Marty? Did Marty have a stroke as well?
Neale 30:30
I have no idea. I just met Marty three days ago.
Bill 30:34
You met him online?
Neale 30:35
Yeah, I met him on the turbo med foot drop group, which is turbo med makes the brakes. So it’s a Facebook group about people with foot drop.
Bill 30:47
Wow. You know, Marty, probably lives an hour away from me. An hour and a half away.
Neale 30:56
Yeah. He said he lives in Ocean Grove. Victoria.
Bill 30:59
Oh man that’s about an hour and a half from me.
Neale 31:02
I don’t know. I’m sorry. I’ve been to New Zealand, but I haven’t been to Australia.
Bill 31:08
You’re missing out. You better get here at some point when COVID and all that junk lifts. You got to get here, man.
Neale 31:13
Yeah, I will. Absolutely.
Bill 31:15
Now let me ask you a question about COVID. Because it’s really controversial, what’s happening at the moment with the vaccines. And I’m not, I’m not one to tell people what to do, whether they should have a vaccine or not. And I’m not an anti-vaxxer, or a vaxxer, or any of those kinds of things.
Covid vaccine and risk of blood clotting
Bill 31:36
But you’ve had a stroke, right, and somebody says, your stroke was caused by a clot and all that kind of stuff. And now they’re talking about a vaccine, the AstraZeneca vaccine in Australia has been recommended for people above 50. Because for people below 50, it’s causing blood clots.
Bill 31:56
What makes this what goes through your mind when you hear that, because I’ll tell you, firstly, I’ll tell you what goes through my mind, I’m, I’ve had a stroke already. And I don’t want to have another one. And I’m not going to do anything that’s going to put me at risk of potentially having another stroke.
Bill 32:12
So AstraZeneca is off the table. For me, there’s no chance I’m getting an AstraZeneca vaccine in any way, shape, or form whatsoever. And that’s even making me reconsider my, you know, my desire to get any other vaccine for COVID. So I’m a little bit concerned and nervous about it.
Bill 32:32
And I’m going to delay getting vaccinated as long as possible, because it seems like, in the end, we’re not going to really have a choice if we want to travel or if you want to go to certain places. We won’t be allowed to go if we don’t get proof that we’ve been vaccinated. How do you feel about this situation that we find ourselves in as a stroke survivor?
Neale 32:56
Oh, exactly the way you feel, you know, I’ve got the Pfizer one. So got one already.
Bill 33:11
Okay, tell us about it was that a long ago?
Neale 33:15
We have like a week or two ago, I have faith in the medical community but not undying faith in the medical community. There are some things that are kind of out of my control. And if Astra Zeneca was the only one to get, I would absolutely not get it. You know, or because they would come in my thought it would be they would come out with rules that say, Hey, if you had a stroke before, obviously, you can’t get the vaccine.
Neale 33:54
You know, because obviously, we can’t put you at risk for a stroke, when a stroke could kill you faster than COVID-19 work. And I’m not a medical person either. I’m either here nor there, but I’m not stupid at all. Just go do whatever sombody tells you to go do.
Bill 34:15
Yeah. With the vaccine that you did get. Did you experience any side effects any of that stuff that they talked about?
Neale 34:22
Nothing? Nope.
Bill 34:23
And is there a second one that you have to get? Do you have to get a top-up or something?
Neale 34:27
Apparently, in a couple weeks, going on vacation with my wife. So we’re just going a couple of states down so I need to reschedule the time. But I’m supposed to get one more but I’m like, you know, do I have to? It’s not like it’s been you know, my only fear is exactly what you know, everybody else fear is, is that it’s not not been tested enough thoroughly enough. You know, What if, in the what if for stroke survivor is a whole different ballgame for somebody who doesn’t have problems.
Bill 35:10
Yeah, we’ve already been there we know what stroke and problems are like.
Neale 35:15
I mean, honestly, my brain can only take so much beating after a while, you know, your brain can only take it so many times till it’s done.
Bill 35:25
Yeah, I agree with you, man. I know, it’s a big conversation. And I don’t hear a lot of people having in the stroke communities that I’m involved in, and not that. Not that I’ve instigated that conversation or not, but it seems like people are just laying low and trying not to have those type of concepts. They seem to be controversial conversations to have, and I’m not sure why.
Bill 35:48
But I know that I haven’t met a lot of stroke survivors that are keen on on having a vaccine and, and I completely get it, I completely understand. So now, are you easing back into work? Where are you at with all the stuff that was put on hold? Because you’re in hospital? Eight weeks in rehab? How long did it take you before you started to get back into? Let’s call it quote unquote, you know, back to normal or normal life or whatever.
Neale 36:22
I’m real far away. Still, I am real far away from normal life. We’re in you know, I’m so easing back into it. You know, I can’t, I can’t honestly say I’m 100% aiming for sure. You know, I give it 100% effort. But my 100% now is like 40 to 50% what it used to be. And then we are stroke survivors, you know, maybe have to like figure out how to live like that, for now. Have to be, we have to be okay, with it.
Neale 37:06
Just Okay, knowing that tomorrow, it’s going to be similar to it was yesterday. The one thing I hate is the word the new normal. You know, I hate that all the time in the stroke community, and all the time outside of the stroke community anyways, now COVID going on the new normal.
Neale 37:25
If yesterday was the same as today, then sure why that. But, but my days are never the same. I you know, one reason I still go to therapy, or one of the important reasons I still go to therapy, I get that statistical readout of how I am doing, how my physicality doing what, you know, if I feel stronger, that doesn’t mean I am stronger. Unless I get a readout of how strong my grip is. I don’t know how strong it really is. or weak, you know?
Bill 38:07
I love what you said about the whole, my 100% now is about 45%. I mean, that’s a beautiful way to describe what stroke survivors go through that is exactly it that’s they’re words that I’ve been lacking for many, many years. My 100% now is 45%. Or, I remember people asking me, how am I and I would say I’m always 90% or 95% back to normal, I would say.
Bill 38:37
But I was nowhere near 95% back to normal. I was nowhere near it. But I didn’t have words to describe where I was at. So I like what you said my new 100% is about 45% of my old 100% that’s created clear to people that there’s something that we’re still trying to gain back that we’re still trying to achieve.
Neale 39:02
I can’t run I can’t lift things to carry. I can’t, you know, can’t walk up and down the stairs without using the handrails. There’s a lot of things I can’t do. And all of those things that I can’t do, I used to be able to do it like 100 miles an hour. And the one thing that upsets me is that some people talk about being 100% back to normal or 90% back to normal.
Neale 39:35
And I think they’re really giving themselves a you know, a shot in the foot when they say that because they’re saying, some people are saying that, hey, this is my new 100% and you can’t think like that. Because you If you think like that, then you won’t get any better.
Bill 40:07
What hear what you’re saying so what you’re saying is, you got to set your sights higher, and, try and get further along than where you are now?
Neale 40:17
Yeah, I mean, I can’t tell you how many times I’ve been to therapy, and they said, Well, you might not get much more bad. I keep coming back, my levels keep getting better, and better and better. And then sometime I hit the dreaded plateau. And when I hit a plateau. It’s, really frustrating. But I know that I just got to keep working. If I stop working, I won’t get better.
Stroke recovery timeline

Bill 40:46
Out of curiosity, did you put a timeline on your recovery, some stroke survivors do the whole and I get why they do it. Kind of frustrates them later, when they haven’t achieved that they kind of give themselves off, in six months, I’ll be back on my feet, or in 12 months, I’ll be back on this or in 16 months, I’ll be doing this.
Bill 41:05
And what is interesting to me is that they’ve I don’t know how they come up with it. Like, I don’t know how they come up with this number that they’re going to use to once they get there, they’ll be better. And what seems to keep happening for people like that is that they get to that number, they’re not better, and it upsets them more than anything, and then they kind of take a little spiral downwards.
Bill 41:32
And to get them out of that. It’s really difficult when they set these goals that they don’t achieve. They get really disappointed. And I don’t know how they come up with these figures. But they start they’ve got to start somewhere. So I suppose that’s how they they start. Did you ever do that? Did you ever put timelines on your recovery?
Neale 41:52
I had a, I would say I definitely had a theoretical timeline. But you know, I went from not being able to lock and use my hand to go, okay. If I all of a sudden, I can move my hand now and have a grip now and walk then there’s progress. And I can’t be upset about progress.
Bill 42:14
Right. So you focus on the small wins. And, keep working towards the big wins.
Neale 42:23
You know, I may have dropped foot for the rest of my life. You know, sadly, that may be the case. But that’s not gonna let me be upset about it, you know, doesn’t mean I stop trying, because the only thing I’m guaranteed is to have dropped but for the rest of my life, if I stopped trying.
Bill 42:49
On Instagram, it’s interesting that you just sent that on Instagram. People who are listening can follow me at recovery after stroke. Is my Instagram. I just my last post was how do you cope with knowing that you are going to have deficits for the rest of your life? That question, just went nuts. You went nuts. And people asked so many responded. heaps. I’m curious about that for you. Like how do you cope knowing that you’re going to have deficits the rest of your life?
Neale 43:25
Well who’s to say I am, that’s my answer to that you know. Am I dead yet? You know, I’m not it’s not the end of my life yet. So I’ll let you know when I get there.
Bill 43:38
Okay, good. All right. Hopefully in about 50 years. We can both have that conversation.
Neale 43:44
Yeah. On some island in the Caribbean.
Bill 43:49
I’m happy to be there. I will, definitely be there. No problem. Tell me about did you do any emotional counseling or psychological counseling or anything like that? Did you seek out talking therapies for support?
Neale 44:05
Yeah, I absolutely. Did. You know, I I find psychology can be helpful. You know, I am I am bullheaded. So that’s just the way I am. You know, I think that has aided me in my recovery, and also done the exact opposite sometimes, you know, I mean, I just hit my head. Like a week ago, I hit my head harder than I have ever hit my head. And I was laying on the ground going, you idiot.
Neale 44:42
I said a lot of other words to myself besides that, but, but I got overly confident about what I was doing. And I knew I shouldn’t have done it. Right before I did it. I did all this could end up real bad, right before I did it. And all I did was I was breaking a stick a big stick at my sister’s house.
Neale 45:05
I was just breaking this stick, I put it in a frame by the tree and I pulled off. It shot me backwards and I ended up blasting my head on the grass, luckily. But I hit my bashed my head off the grass. I told my therapist, he’s like, man, don’t do that anymore.
Bill 45:26
I’m gonna agree with you’re therapist man I’ll tell you what though, I’ve become a little less. I’m not sure what the word is. But maybe I’ve got less awareness about where my head is in the world like something’s missing. Because I’ll tell you what, I’ve smashed my head since the stroke. And since brain surgery because I’ve had surgery now there’s a plate on the side. I’ve smashed my head so many times.
Bill 45:52
And it hurts so much more. Because I associate people touching my head and doing things to my head and impact on my head I associated is a really bad thing, which it is but, but since the surgery in 2014. Like I reckon I do way more. I just don’t seem to pay attention or have enough awareness or vision of what’s above my head? Like, it seems like, I’m not I’m missing something. I don’t know what it is.
Neale 46:27
Yeah, well, you might want to get tested. Correct. That may be like spacial awareness, or, or proximity awareness? Like how close my hand is? That kind of stuff? I think, you know, one technological, interesting thing that has come about is like a virtual reality, and kind of training for that visti role. I don’t know the words like that risky role training, or retraining your brain, how to determine how far and how close objects are.
Neale 47:08
I think that’s a really, really interesting technology. I’m lucky enough myself to have a quite interesting setup that I put in my basement with a virtual reality system, some workout stuff, and I, I, I love now riding a stationary bike, because that’s the number one way I can really get some intense cardio with.
Bill 47:38
Yeah. Do you ever worry about? What if another stroke? Is that issue that you have with the blood vessel that has atherosclerosis? Is that issue resolved? Or what is the approach that the medical team is using to support that not causing another clot?
Neale 48:03
Yeah, it is resolved. And then it took me a while to come to terms with their not so good answer and how to resolve the problem. Basically, like take aspirin and take a take a lift or take, you know, get your LDL down and I’m like, it already is down. Like what’s the what’s the problem?
Neale 48:25
You know, my mindset is always if it ain’t broke, don’t fix it. But it took me for a while to accept that those would be good alternatives. And, you know, like you were just saying, the psychology aspect, I did see a psychologist for a couple sessions, you know, having just really scared about having another stroke and it really, really messed my whole day.
Neale 48:54
After I just had a MRI, which is a, you know, the arteries? And they came back and said, Hey, it looks good. But now it’s like, Oh, here we go again. But we think you have an aneurysm I was like what? Anything else? Any other things you wanna tell me?
Bill 49:29
Was it confirmed?
Neale 49:30
No. My surgeon looked at it said no that’s not an aneurysm. That’s just the weird way to look at the picture or whatever. And so I you know, and I was a mess after that. I was like, oh, gee, here we go. Yeah, it takes. It literally takes 100% of my effort to just put stuff like that aside, you know.
Neale 50:00
I have my life, I have my faith. I have my friends, I have my family, you know? If Now is the time, then let it be, you know, I got no power in that. I don’t do drugs, you know, you know, I’m trying to keep myself fit as best I can, you know, try to eat healthy. Yeah, I try to do what I can do.
Bill 50:28
Yeah, you keep on top of the things that you can influence and you can help out with and you can do and the things that you can’t, you can’t end, there’s power in giving up on trying to control things that I out of our control, we can’t control what’s going to happen.
Bill 50:44
So there’s a real for me, when I’m able to do that I get a real what’s the word, I get a real kind of a burden ease. As you know, the shoulders get lighter, there’s less I have to worry about when I don’t have to worry about the things that I can’t control is perhaps I’ve learned to deal with the fear.
Bill 51:11
And I’m not fearful of dying anymore. And one of the reasons I’m not fearful of dying is because I’ve put things in place. I’ve told my children, I love them all the time. My wife, my parents, my family, the people that I run with, I’m trying to make better, I put my will in place so that if I do get hit by a bolt of lightning, then everything that needs to be in place for them.
Bill 51:40
My last wishes are known, and it’s all sorted. So I’ve done a lot of things. To prepare me for something that I hope doesn’t happen for another 50 years. But in the event that it does, of course, that’s all been sorted. So they’ll be okay. And, and now I can let go of the fear of that.
Being afraid is something to be afraid of
Neale 52:03
Yeah, you know, I think fear can be a very powerful thing. You know, being afraid is something to be afraid of.
Bill 52:20
Oh, man, hang on a sec say that again.
Neale 52:25
Being afraid, is something to be afraid of.
Bill 52:30
That’s deep man that is real deep.
Neale 52:35
Came straight from Ohio to Australia.
Bill 52:38
It’s so true, though. I mean, talk about a real meta version of paying attention to being afraid. Because we know what being afraid of things does, he puts us in a cycle that’s not good, right? So if, if you’re afraid of being afraid, then hopefully you won’t get to be afraid.
Bill 52:59
And therefore, you won’t go into these cycles of stuff that happens that causes problems in your mind, in your body, in your emotions, in your relationships. Yeah, if we can put that aside, then I think the best way to put it aside also is that is that you have to put things in place and work things out and sort things out and actually tackle the hard stuff like the wheel because I know that can be confronting for a lot of people, but it is hard.
Bill 53:31
If you do that. It does it lifts some kind of a burden from the shoulders. For me, it was so freeing that I had done that it just felt great. So that fear has gone and I like what you’re saying how does your faith help you in your recovery as well? Because it seems to me from what we’ve said already, that you are somebody that has faith in something other than what’s going on, on this planet.
Neale 54:03
I’m a Catholic. But you know, I truly believe that. And I heard this from my pastor rather like a month ago. You know, there is no faith without works. You can’t have faith and then not act on your faith. Rehab, there’s no progress without work. You can’t progress without working at it but work, you have to just kind of make money. You know, money doesn’t grow on trees, I’m sure you heared that before.
Bill 54:42
I like what you’re, saying and in recovery, what I find is with the people that I’m coaching and supporting on their stroke recovery, the people who are the most active, get the most results and I’m not talking about physical results or they get results.
Bill 54:59
They just feel better, they feel different, they change, they adjust, they come to terms with things, they find new ways to be themselves, they find new ways to find what they’re passionate about. They learn new skills, the more they focus on the solutions to their problems, the more solutions they find. And I find the people that put less effort into their recovery, they get less results. That’s pretty straightforward, isn’t it?
Neale 55:31
Yeah. I think we got to stop telling people that, you know, you can only go so far, you know, don’t think that you’re gonna get much more back. For me, it’s like a challenge. I go watch me. But for someone else, it’s not that much of a challenge, like, Oh, okay.
Neale 55:58
And, oh, okay to that answer is, you know, terrible, depressing. It’s all the, it’s all the bad stuff. And to make your situation worse, that’s all you got to say to somebody is, you know, well, you know, that, after the first couple months, if you can’t move your leg, you’re probably not going to be able to move it. You know, good luck living 30 years without moving your leg.
Bill 56:25
And they still do that a lot. Even in Australia, a lot of stroke survivors say that, that the doctors still do that. And I have met people who have taken that information from the doctors as gospel, and they lived by it, and then they’ve got no results. And thankfully, I’ve met a lot of people that have said, screw that I’m not listening to you.
Bill 56:47
I’m not taking what you’re saying, as the truth, I’m going to do what I can, and most of them get better results than the doctor expected. And that is great. And why doctors do that? I don’t know, I don’t get it. And if we could get them to stop doing it would be fantastic. I don’t think that we can they judge everybody based on statistics. And then they apply those statistics to everybody. And that’s real harsh.
The biggest disconnect
Neale 57:20
You know, for me, I think there’s a big Avenue. I think that and this is why I created my website and my business is to stroke fit Incorporated. You know, I think that the biggest disconnect is in between when you come home from the hospital.
Neale 57:42
And when you’re home, and how do you rehab if you can’t go to therapy, or even if you do go to therapy, because the therapist gives you stuff to do, but he’s not there with you doing it in your house. And everybody’s got different tools available or different challenges available to do those things.
Neale 58:04
It’s not cut and dry. It’s not like here, this 80 year old guy gets the same thing as you get. I’m like, Why are you giving me the same thing? If it’s hard for me to do that. It sure is hard for that guy to do. You know? It’s just, there’s so much non-medical speaking like therapies or like, things that you can do.
Neale 58:29
There’s so many different things you can do out there that are just available that the doctors aren’t going to tell you about because they’re not FDA certified. Or you know, government certified or okay by the hospital. The bosses you know, everybody’s boss in therapy world.
Neale 58:49
Your last your last. Let me look it up here real quick. Last lady that just talked on your show. Forgot her name. Karen Moorman. Yeah, Karen, and Karen has an Instagram and I looked at Karen’s Instagram, and I saw that she was using a Bosu ball upside down. It was awesome for your hips and everything like that.
Neale 59:24
I got a Bosu ball downstairs. And I’ve had it for about two and a half years. It wasn’t pumped up probably for a year and a half. But I can’t really use it because my ankles not really secure. But in this brace that I’m wearing, it is secure. And so I did exactly what Karen just did.
Neale 59:45
I flipped the ball upside down and did standing squats but in order to like get myself onto the ball safely and kind of stand there. I had a pair of TRX bands. I was, suspension trainers, and I was hanging on I need something to hang on while I’m sitting there. So go down, do a squat, come up, go down do a squat, you know, and then kind of see if I can let go and watch my body work, you know.
Bill 1:00:17
So when you’re describing that ball you’re talking about, it’s a circle and underneath it is a half a, half moon ball, that’s blow up, and you’re supposed to stand on the platform. And then it’s supposed to give you it moves as you move as your weight shifts, and you’re supposed to get a tighter core, and it’s supposed to help balance.
Bill 1:00:51
And Karen is on Instagram, her Instagram handle is @stroke_sur_vivor, and I’ll put the link on the show notes there. So people can find that, but also, Karen was on episode 139. And we spoke about her stroke journey and the stuff that she was doing, that I really loved.
Bill 1:01:23
You know, she had a couple of really good quotes as well, she spoke about being perfectly imperfect, and she’s getting creative as well, just like you’re talking about, you know, doing the things that she can within her own home within her limits, to continue rehabilitation and continue getting better at home in a way that’s really safe and comfortable for her to do.
Neale 1:01:50
Yeah, I’m also a big proponent on like, doing as many research studies as you can, you know, because a lot of the the universities like Melbourne University and Cleveland State here, they have a lot of, you know, federal grant money or whatever it is to do research projects.
Neale 1:02:12
They, they need stroke survivors to do that. And, you know, on my website, in the Cleveland area, I have a registry that the Cleveland Clinic actually made up a registry to put everybody down. So that when the college professors or whatnot, are ready to do a research study, they have a pool of people that fit certain categories that they already know who to call, you know, they don’t have to like, seek them out. Because the more work they got to do. The more work anybody’s got to do the worse.
Bill 1:02:53
Yeah. And it’s kind of an opportunity to get some free support for access some services they could not otherwise get.
Neale 1:03:05
What I’m throwing is like, three months of free therapy, I’ll take it.
Bill 1:03:10
That’s great. That’s great, man. That’s awesome. I love your out of the box, kind of thinking on how to get access to things that some people would not get free. Definitely, universities are always looking for people to support them in their programs and in their research and in their work. So yeah, if it’s convenient, it’s a no brainer. It’s perfect.
Neale 1:03:40
Yeah. And it’s usually like a more unconventional therapy. Or a newer therapy.
Bill 1:03:47
Yes.
Neale 1:03:47
Because, you know, they’re not going to just do the same old job that you’ve been doing. You know, for 50 years.
Future plans for Neale Mahon
Bill 1:03:56
Yeah, yeah, it’s cutting edge. It’s most recent. What’s the as we come to wrap this up? What’s on the horizon for you? What are you hoping to achieve over the next few years as your recovery continues?
Neale 1:04:15
You know, get my get that stroke fit business up and running and providing people the tools and the help they need to really make themselves better and set them up for progress in their life. For me, personally, I still have to run. I still, I’m desperate to be able to run and jog and swim.
Neale 1:04:41
can’t do any of that because I have too much spasticity going on. Too many limiting factors at the moment that I keep trying to power through. And I’ve been I’ve been seeing amazing progress, but it’s just I always I’m almost there, I’m almost there. I’m almost there, you know. And being almost there kind of motivates me also in another way and meeting people like you, learning about podcasts like this.
Bill 1:05:16
The great things to info I am, very, very early on in the podcast, I interviewed a stroke survivor, somebody who had a stroke when they were a child, probably eight years old. And in her early 40s, she has foot drop. And she uses an afo. And in early 40s, she decided that she was going to hire a trainer to get back to running to be able to run again.
Bill 1:05:47
So a long, long time had passed, and she hadn’t been able to fulfill that goal. So she decided that she was going to do it. And she was on episode 28. Donna can peasy. And an episode 28. She talks about how to get back to running after stroke. And she talks about how she was challenged to run a marathon, not just a few kilometres that she was initially wanting to do.
Bill 1:06:18
So in the beginning, she thought, I’m going to go and learn how to do four or five kilometers. And her trainer said to her, no, we need to run a marathon. So she went quickly from being somebody who was just trying to get back into running to becoming somebody who was going to run a marathon. And she ran a marathon, I think back in 2012, or 13, or something like that.
Bill 1:06:43
And it’s a really inspiring story, because it’s what she did, she got back to running after the stroke. But it took her quite a long time. And she fell, and she struggled and she had injuries. And she suffered pain and all these things. But they slowly but surely, they overcame all these little obstacles and all these hurdles and all these problems. And she ended up running a full marathon man. It was slow, but she did it.
Neale 1:07:11
Yeah. My main goal, goal wise is, but by the time I’m 40 I want to do an Ironman for a little bit, but the half Ironman, so it’s not gonna be 30 there’s no way I can do the whole 30. My cousin is an Ironman. So and he is my age too.
Bill 1:07:34
Well done on that. Man. I hope you do get that I couldn’t think of anything worse not before the stroke, that after the stroke, there’s no chance I’ll be doing anything that takes 40 kilometers. And there’s no chance I’ll be doing anything that is a full marathon a full Ironman no chance in the world.
Bill 1:07:50
I don’t enjoy challenging myself like that I never have you know, and I’m inspired by all the stroke survivors who have done those types of things after stroke. Absolutely you guys are amazing. And I take my hat off. I’m never ever gonna do it.
Neale 1:08:08
Well, I’ll get a hat made for you at the end of the line. And maybe I’ll come down in Australia.
Bill 1:08:20
You can do it in Australia. Man, I will be cheering for you at the finish line. There’s no problem whatsoever. I look forward to it. I want to thank you for reaching out. I really appreciate it when people contact me and say, can I be on the podcast? I love meeting new people. I love sharing stroke stories.
Bill 1:08:39
And I just like your approach, man, I think your approach is one that people need to hear about. And I like that you’ve also made it a little bit about other people. It’s not just about you, this recovery that you’re on, is trying to somehow incorporate other people and support them.
Bill 1:08:56
And a lot of stroke survivors do that. And I don’t understand why I did the same thing. I don’t understand why. But that’s what we need, isn’t it? We need to support each other because nobody else gets us. No one really understands what we’re going through.
Neale 1:09:11
That’s absolutely correct.
Bill 1:09:13
Neale, thanks so much for being on the podcast.
Neale 1:09:16
Thank you Bill.
Intro 1:09:21
Discover how to heal your brain after stroke go to recoveryafterstroke.com. Importantly, we present many podcasts designed to give you an insight and understanding into the experiences of other individuals.
Intro 1:09:38
The opinions and treatment protocols discussed during any podcast are the individual’s own experience and we do not necessarily share the same opinion nor do we recommend any treatment protocol discussed all content on this website and any linked blog, podcast or video material controlled this website or content is created and produced for informational purposes only and is largely based on the personal experience of Bill Gasiamis.
Intro 1:10:00
The content is intended to complement your medical treatment and support healing. It is not intended to be a substitute for professional medical advice and should not be relied on as health advice. The information is general and may not be suitable for your personal injuries, circumstances or health objectives.
Intro 1:10:16
Do not use our content as a standalone resource to diagnose, treat, cure or prevent any disease for therapeutic purposes or as a substitute for the advice of a health professional. Never delay seeking advice or disregard the advice of a medical professional your doctor or your rehabilitation program based on our content if you have any questions or concerns about your health or medical condition, please seek guidance from a doctor or other medical professional.
Intro 1:10:39
If you are experiencing a health emergency or think you might be call 000 if in Australia or your local emergency number immediately for emergency assistance or go to the nearest hospital emergency department medical information changes constantly. While we aim to provide current quality information in our content.
Intro 1:10:55
We did not provide any guarantees and assume no legal liability or responsibility for the accuracy, currency or completeness of the content. If you choose to rely on any information within our content, you do so solely at your own risk. We are careful with links we provide. However third-party links from our website are followed at your own risk and we are not responsible for any information you find there.







